
Fam Pract Manag. 2002;9(8):26
HIPAA privacy rule modified
The Bush administration has announced its final modifications to the Health Insurance Portability and Accountability Act (HIPAA) privacy regulations, which establish federal standards for protecting patients’ health information. Perhaps the biggest change made to the regulations is that the final, modified rule does not include the Clintonera requirement that physicians and other health care providers obtain written consent from patients before using or disclosing personal medical information for treatment or claims purposes. Instead, physicians and other providers will only need to have made a “good faith effort” to obtain written consent. Physicians will not be penalized for “incidental use or disclosure” of patient information, which means they can continue using sign-in sheets in their waiting rooms and talking to patients in semi-private rooms, for example. The HIPAA privacy rule goes into effect on April 14, 2003. For more information, go to www.hhs.gov/topics/privacy.html.
Liability crisis fuels talk of reform
Excessive litigation has caused physicians’ malpractice insurance premiums to skyrocket over the past year and is hindering patients’ access to high-quality, affordable health care, says a new report from the U.S. Department of Health and Human Services.
Physicians’ premiums increased an average of 20 percent nationally but soared 44 percent in states that have not enacted malpractice reforms, says the report, citing research from Medical Liability Monitor. The states with the highest increases were Nevada, Mississippi, Pennsylvania, North Carolina, Virginia, Florida, Ohio and Illinois.
Some physicians in the hardest hit areas have reportedly closed their doors or stopped offering high-risk services, such as obstetrics, which has left some patients struggling to find care. The report cites a recent poll of Chester County Pennsylvania physicians, which found that 65 percent of physicians were contemplating moving their practices to another state.
In an effort to curb runaway litigation and malpractice insurance costs, Congress members have introduced legislation (HR 4600 and S 2793) that would encourage speedy resolution of malpractice claims and cap non-economic damage awards at $250,000.
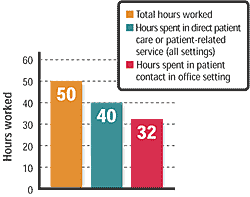
An average workweek
Family physicians spend 80 percent of their average 50-hour workweek providing direct patient care or patient-related services and spend 64 percent of their time in patient contact in the office setting, according to the results of the AAFP 2002 Practice Profile I Survey.
Home sweet home

Housecalls are making a comeback, thanks to Medicare reimbursement rates that pay up to 46 percent more than office visits, reports the Aug. 2 Wall Street Journal. The number of paid home visits shot up to 1.5 million in 2001 from 195,700 in 1996, according to the Centers for Medicare and Medicaid Services.
Simple fixes overlooked
Many simple and well accepted practices for improving patient safety were “conspicuously absent” in a recent report of best practices by the Agency for Healthcare Research and Quality (AHRQ), write safety experts Lucian Leape, MD, Don Berwick, MD, and David Bates, MD, in the July 24/31 JAMA. They argue that the AHRQ report focused too heavily on evidence-based safety practices, ignoring effective strategies that lack extensive research, such as the use of protocols and checklists to prevent errors. Waiting for “incontrovertible proof of effectiveness before recommending a practice would be a prescription for inaction,” write the authors.
$1.5 million for hospitals
Family physicians generate an average of $1,559,482 a year for affiliated hospitals, reports a survey conducted by Merritt, Hawkins & Associates, a Dallas-based physician search and consulting firm. The average for all physicians was $1,540,181, with cardiovascular surgeons generating the most ($3,134,615) and pediatricians generating the least ($690,104).
White coat phobia
The “white coat effect” is real. A study published in the Aug. 3 British Medical Journal found that blood pressure readings taken by doctors measured much higher than readings collected by others. Researchers suggest doctors would be better off basing their decisions on readings taken by nurses or by patients themselves.