
Fam Pract Manag. 2003;10(2):24-26
Medicare cuts could be postponed
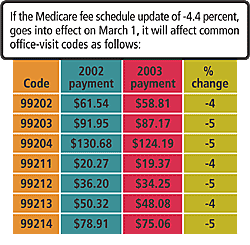
Last-minute Congressional action is likely to postpone a 4.4 percent cut in Medicare payments scheduled to take place on March 1; the 4.4 percent cut would follow a 5.4 percent decrease in 2002. The decreases are due to a flaw in the Medicare reimbursement formula, which the government has acknowledged but did not correct in 2002.
At press time, Congress was debating the appropriations bill for fiscal year 2003, which contains a provision that could freeze physician reimbursement at the 2002 level until Sept. 30. Washington insiders expressed optimism that the provision would be passed.
Should the cuts occur, physicians can find out how their practices will be affected by consulting the 2003 Medicare Physician Fee Schedule (at www.cms.gov/regulations/pfs or in the Dec. 31, 2002, Federal Register), paying particular attention to new payment rates for their most common services.
Physicians have until Feb. 28 to enroll as participating or nonparticipating physicians in Medicare.
AAFP pushes for affordable EMR system

The AAFP is pursuing development of an affordable, “open-source” electronic medical record (EMR) system. Because the EMR’s source code would be shared openly without license fees, the software could be made available to physicians for significantly less than proprietary software.
As part of the project planning process, the AAFP surveyed 5,000 family physicians regarding their feelings about EMRs. Seventy-six percent said they do not currently have an EMR in place, the most common reason being that they cannot afford it.
Bold initiatives could transform health care
The greatest potential for improving the nation’s health care system lies in 1) expanding the use of information technology, 2) increasing individuals’ access to health care coverage, 3) reforming the medical liability system, 4) improving chronic disease care and 5) enhancing the primary care setting, says a new report, Fostering Rapid Advances in Health Care: Learning From System Demonstrations, from the Institute of Medicine. The report proposes national projects to be implemented as early as 2003 that would test strategies for improvement in each of these five areas, with the goal of achieving significant progress toward reform within five years. The proposed projects were developed in response to a request from the Department of Health and Human Services.
Information technology. The health care industry lags behind most other industries in adopting information technology. Many caregivers still record patient data on paper, which makes it difficult to access, resulting in errors and inefficiencies. The IOM proposes a series of demonstration projects to develop computerized information systems and virtually eliminate paper-based processes in health care.
Health care coverage. The number of uninsured Americans now exceeds 41 million people. The IOM recommends that three to five states embark on model projects to extend health coverage to all residents, either through the provision of tax credits to offset the costs of eligible participants’ insurance premiums or through the expansion of Medicaid and the State Children’s Health Insurance Program to cover a broader range of participants.
Malpractice reform. The climbing cost and decreasing availability of malpractice insurance has limited patients’ access to care in some communities, and the fear of liability has hindered efforts to identify sources of medical errors. The IOM recommends that four or five states create patient-centered, safety-focused injury compensation systems outside of the courtroom that would provide limited but fair and timely compensation for avoidable injury.
Chronic disease management. Roughly 120 million Americans have one or more chronic conditions, many of which could have been prevented or delayed, yet health care practices generally are focused on acute, episodic problems. The committee proposes that 10 to 12 projects be undertaken to develop care programs for chronic conditions and community-wide prevention and health promotion strategies.
Primary care enhancement. The majority of patients enter the health care system and receive most of their care in the primary care setting, making it central to a well-functioning health care system. The IOM recommends that 40 federally supported community health centers undertake a project to reinvent and substantially enhance primary care, building on existing innovations, such as patient self-management, and more systematic approaches to care.
Acknowledging that “the current health care environment often confounds efforts to redesign health care,” the IOM has called on government and third-party payers to remove barriers to innovation by making essential payment and regulatory changes in tandem with the demonstration projects.
Non-MDs don’t reduce MD demand
Between 1987 and 1997, the proportion of patients who visited a nonphysician provider increased from 30.6 percent to 36.1 percent although visits to physicians remained stable, reports a study from the Jan. 9 New England Journal of Medicine. Much of the nonphysicians’ increase was due to patients visiting both non-physician providers and physicians for treatment. Researchers found that nonphysician providers delivered more preventive care and less acute care in 1997 than in 1987, suggesting an increase in collaboration between nonphysician providers and physicians.
Business is booming
The managed care industry enjoyed a financial boost in the third quarter of 2002. With the help of rising premiums, 11 major insurance companies saw their earnings increase by an average of 47 percent, according to the Jan. 2 USA Today. Similar earnings are expected for 2003 with premiums predicted to climb an average of 15.4 percent. Insurers blame expensive new drugs and higher hospital fees for the increased premiums.
Employees strike back
Not only are physicians frustrated by health plans and rising costs, patients are too. Recently, more than 17,500 General Electric employees staged a two-day work stoppage to protest paying higher insurance co-payments this year. U.S. companies have experienced a 35 percent increase in health care premiums since 1999 and are passing more of these costs on to their employees. Forbes magazine predicts more GE-like skirmishes between U.S. workers and their employers as health care costs continue to rise.
What malpractice insurance crisis?
Several consumer groups are speaking out against legislation that would cap malpractice awards and thereby ease the malpractice insurance crisis. According to the groups, there is no crisis; the current jump in premiums is due simply to a downturn in the overall economy, which has caused insurers’ investment income to drop. The medical community believes growing damage awards are leading the premium increases and should be capped.
Generic drug use climbs
Name-brand drugs faced their fiercest competition in 2002, according to Express Scripts. Led by the introduction of the generic equivalents of Glucophage, Prozac and Zestril/Prinivil, the share of prescriptions filled by generic drugs reached an all-time high of 45.2 percent by the end of the third quarter. With more health plans encouraging the use of low-cost medications and several major drug patents expiring in 2003 and 2004, generic treatments should remain popular in the coming years.
Good news for Medicare
Getting older means getting better – better health care, that is. In a study by the Commonwealth Fund comparing Medicare with employer-sponsored health plans, Medicare beneficiaries over age 65 were more likely than privately insured working-age adults to rate their health insurance and physicians as “excellent.” They also reported fewer problems with medical bills and higher satisfaction with their care.
And more good news
One reason Medicare beneficiaries may be more satisfied is because their quality of care is improving. In a study published in the Jan. 15 JAMA, researchers found that, based on 22 quality measures, Medicare beneficiaries received appropriate care 73.4 percent of the time in 2000–2001, up from 69.5 percent in 1998–1999. Although the improvement is substantial, according to the authors, “there is still a very long way to go.”
Drug ads – good or bad?
A recent Food and Drug Administration poll of 500 doctors revealed both pros and cons to direct-to-consumer (DTC) drug advertisements. While 59 percent of respondents said DTC ads provide no benefits, others found the ads encouraged better discussions with patients about various drugs and treatments. Although 82 percent of physicians said their patients understood that only a physician can assess a drug’s suitability for a patient, 46 percent of physicians admitted feeling some pressure by patients to prescribe the drug in question. When patients asked their physicians for a specific brand-name drug, the physician prescribed the drug in 57 percent of cases.