
Fam Pract Manag. 2003;10(3):26
Congress averts 4.4 percent cut in Medicare reimbursement
Last month, Congress adopted the 2003 omnibus appropriations package, which included a provision to increase Medicare reimbursement to physicians by about $50 billion over 10 years. Congress’ action averted a 4.4 percent reimbursement cut scheduled for March 1. For 2003, physician payments will increase 1.6 percent.
Last year, physician reimbursement dropped 5.4 percent due to a flaw in the Medicare reimbursement formula. Physician groups had warned that if Congress did not act to correct the Medicare payment formula mistake, the number of doctors willing to treat Medicare beneficiaries would fall dramatically.
Are you over-prescribing antibiotics?
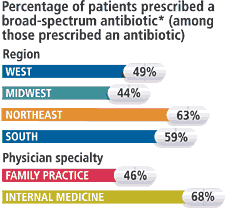
Physicians commonly prescribe broad-spectrum antibiotics for the treatment of nonpneumonic acute respiratory tract infections, even though their use is often unnecessary, concludes a study in the Feb. 12 Journal of the American Medical Association. Internists and physicians in the Northeast and South were the groups especially likely to prescribe broad-spectrum antibiotics in such cases.
HIPAA compliance at eleventh hour
April packs a double punch for practices still struggling to comply with the Health Insurance Portability and Accountability Act (HIPAA). April 14 is the deadline for complying with the HIPAA privacy regulations, and April 15 marks the date practices should begin testing the new electronic transaction standards, assuming they filed for an extension. If you’ve waited until the last minute, you’re not alone. The January issue of Health Management Technology reports that up to half of the nation’s health care payers and professionals haven’t yet started to comply or are in the earliest stages.
The best strategy for complying with the HIPAA privacy rule at this late date is to focus your efforts on the requirements that are most visible to patients. Educate staff about HIPAA, create a tracking system to record all disclosures of patient information and notify patients of their new rights. To save time, use templates of HIPAA-required forms and tailor them to your practice. (See www.aafp.org/fpm/20030200/29theh.html.)
When it comes to the transaction and code set standards, don’t attempt to implement any new electronic transactions. Instead, identify the ones you currently use, and work with your payers or clearinghouse to determine what needs to be done to make the transactions HIPAA-compliant by the October 2003 deadline.
Investing in technology to reduce errors
Nearly 60 percent of health care information technology executives say implementing technology to reduce medical errors and promote patient safety will be their top priority over the next two years, according to a survey by the Healthcare Information and Management Systems Society. Survey respondents showed high interest in computer-based physician-order-entry systems and bar-coded medication management.
Clueless on drug costs
Physicians don t know how much prescription drugs cost or how much their patients pay for them, says a study from the January Journal of General Internal Medicine. Of doctors surveyed, 72 percent confessed they were unaware of drug costs even after attending a lecture on the subject and receiving educational materials. The study s researchers encourage doctors to maintain open communication with their patients about medication expenses so that patients do not avoid filling their prescriptions due to cost.
Medicare plays favorites
Last year, Medicare overpaid an estimated $1.1 billion by reimbursing different providers at different levels for the same services, according to a report by the Department of Health and Human Services Office of Inspector General (OIG). Sixty-six percent of the out-patient services examined in the report were reimbursed at a higher rate in a hospital setting than in an ambulatory setting; the remaining 34 percent were reimbursed at a higher rate in the ambulatory setting.
Groups slow to adopt care-management processes
Organized care-management processes, such as the use of clinical guidelines and disease registries, which have proven to be effective in improving care, are not being readily adopted by physicians, according to a study in the Jan. 22/29 Journal of the American Medical Association. The study, which examined the use of 16 care-management processes in more than 1,500 medical groups, found that an average of only five processes were being used. Researchers concluded that their use could increase if medical groups were given external incentives and technological support.