
Clinical decision rules make it easy to give patients more precise estimates of their risks of complications.
Fam Pract Manag. 2004;11(10):71-72
Patients undergoing serious medical procedures deserve to be informed not only of the complications associated with the procedures but also of the likelihood of those complications. For example, a 63-year-old man presents to his family physician with typical anginal chest pain. He is about to undergo coronary artery catheterization with possible angioplasty and stent placement and would like to have a more precise idea of the risk of complications.
Years ago, estimating this patient’s risk would have been a major undertaking; however, new clinical decision rules are making this task doable even for busy family physicians.
Using clinical decision rules
Percutaneous coronary interventions, such as balloon angioplasty with or without stent placement, are an important treatment for patients with coronary artery disease. Several clinical decision rules have been developed and validated to help physicians estimate the likelihood of short-term, in-hospital complications such as death, myocardial infarction and urgent coronary artery bypass graft surgery.1,2,3,4 (To read a summary and discussion of these rules, see the Nov. 15, 2004, issue of American Family Physician.)
The decision rule developed by Singh et al (shown below) is among the newest and best-validated rules, and because it relies on only eight clinical variables, it is relatively easy to use at the bedside. The rule does not require an assessment of the complexity of the lesion (such as the A, B1, B2 or C classification by the American College of Cardiology5), and it can easily be added to a spreadsheet for use on a handheld or desktop computer. The Singh rule helps the clinician appreciate the importance of increasing age, shock, left main coronary artery lesion and renal disease as risk factors for complications from angioplasty. Patients with these risk factors may warrant more careful observation following their procedure.
SINGH RISK SCORE CALCULATOR FOR ANGIOPLASTY COMPLICATIONS
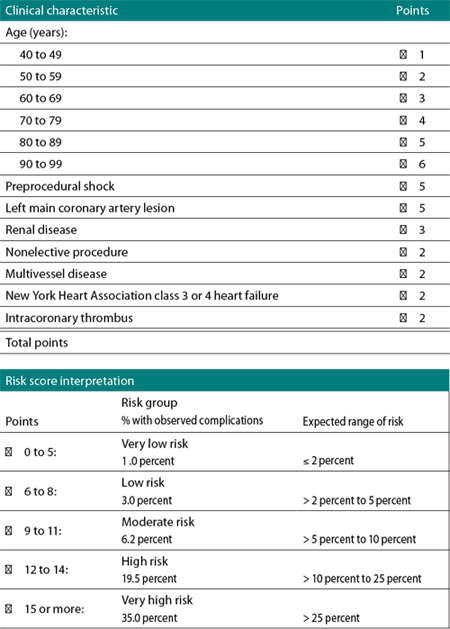
Adapted with permission from Singh M, Lennon RJ, Holmes DR, et al. Correlates of procedural complications and a simple integer risk score for percutaneous coronary intervention. J Am Coll Cardiol. 2002;40:387-393.
Applying the evidence
Let’s assume our 63-year-old patient, presented above, does not have shock, renal disease or heart failure. This gives him a baseline risk score of three points (very low risk of complications) based on age. If he has left main coronary artery lesion, his risk score increases to eight points (low risk), and if he has both left main coronary artery lesion and multivessel disease, his risk score increases to 10 points (moderate risk). Within the moderate-risk group, the expected range for risk of complications is greater than 5 percent to 10 percent, with an observed rate of procedure complications of 6.2 percent, or about 1 in 16. Given these risks, the patient would likely choose to go ahead with the procedure.
POINT-OF-CARE SERIES
This article is part of a series that offers evidence-based tools to assist family physicians in improving their decision making at the point of care. The series is produced in partnership with American Family Physician. A related article, which also includes the risk calculator for angioplasty complications, appears in the November 15, 2004, issue of AFP, pages 1966-1968.
Other articles in this series include “Making Decisions at the Point of Care: Sore Throat,” FPM, September 2003, page 68; “Diagnosing Pulmonary Embolism,” FPM, February 2004, page 61; “A Tool for Evaluating Hypertension,” FPM, March 2004, page 79; and “Acute Otitis Media in Children,” FPM, June 2004, page 52. All tools are available free online at https://www.aafp.org/fpm/toolbox.