Fam Pract Manag. 2005;12(1):25-26
MedPAC drafts recommendations to improve Medicare payments
The Medicare Payment Advisory Commission (MedPAC) has issued a set of draft recommendations that could bring about significant changes in the way physicians and hospitals are reimbursed under Medicare.
One of the key recommendations calls on Congress to establish a Medicare pay-for-performance program, which would create financial incentives for physicians, hospitals and home health agencies to provide high-quality care to Medicare beneficiaries. MedPAC’s proposal involves setting aside an initial 1 to 2 percent of current reimbursement funds and using the money to pay bonuses to those who meet certain quality measures. Measures would include clinical goals as well as process goals, such as using a patient registry to identify patients with diabetes and send care reminders.
The justification for the program is not only to improve patient care but also to redistribute payments to physicians and other providers. For example, under the current Medicare payment system, a high-quality physician is paid the same as all others. In some cases, providers that improve quality are impacted negatively.
Because Medicare is the largest purchaser of health care services, its move to a pay-for-performance system could lead the way for private-sector purchasers.
MedPAC also recommended that Congress update payments for physician services by 2.7 percent in 2006. Without such action, physician payments would decrease in 2006 due to the sustainable growth rate system for updating physician payments, which was created as part of the 1997 Balanced Budget Act.
MedPAC’s recommendations are subject to revision and will be voted on in January. Given pressure in Congress to lower spending growth in Medicare and other federal programs, adoption of the recommendations is uncertain.
Physicians get little help with Medicare questions
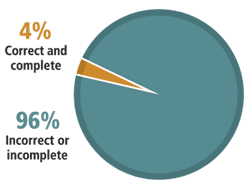
Of 300 test calls made to 34 Medicare carrier call centers, whichexist to answer physicians’ questions about the program, only 4 percent of responses were correct and complete, according to a recent study from the Government Accountability Office (GAO). Questions asked involved Medicare policy, such as billing for an office visit and procedure for the same patient on the same day.
The GAO cited several factors as contributing to the lack of correct and complete answers. Customer service representatives who answer calls must rely on fragments of information from multiple sources and are often interpreting confusing policy information. In addition, the call centers often have difficulties retaining staff.
Quality, safety revisited on anniversary of landmark IOM report
Five years ago, the Institute of Medicine released its “To Err Is Human” report, which concluded that hospital-based medical errors were the eighth leading cause of death in the United States. Despite widespread patient-safety efforts, four out of 10 U.S. residents (40 percent) believe the quality of health care has worsened in the past five years, according to survey results from the Kaiser Family Foundation, the Agency for Healthcare Research and Quality, and Harvard School of Public Health. One in six (17%) said the quality of care has gotten better, and nearly four in 10 (38%) said it has stayed the same.
The survey of 2,012 randomly selected adults nationwide found that 55 percent of respondents said they are dissatisfied with the quality of health care, up from 44 percent four years ago; 48 percent said they are concerned about the safety of medical care they and their families receive; and 34 percent said they or a family member have experienced a medical error at some time.
People with chronic health conditions were considerably more likely than others to express concerns about their quality of care and report having personal experiences with medical errors.
“This survey shows that the challenge is not just to improve patient safety but to convince the public that real progress is being made,” said Drew Altman, president of the Kaiser Family Foundation.
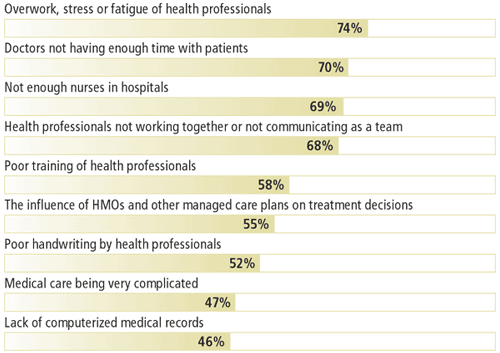
What causes medical errors?
A high percentage of patients rated the following items as “very important” causes of medical errors: