
Yes, the concept has flaws, but it may also have promise. Regardless, it’s headed your way.
Fam Pract Manag. 2006;13(7):69-74
Dr. Endsley, a family physician, is medical director for system design for the Health Services Advisory Group in Phoenix. Geof Baker is chief executive officer of Med-Vantage in San Francisco. Bernard Kershner is chairman of the board of directors for the Accreditation Association for Ambulatory Health Care’s Institute for Quality Improvement in Wilmette, Ill. Kathleen Curtin is senior vice president for client services for Med-Vantage. Author disclosure: nothing to disclose.

Pay for performance (or P4P) may seem like a distant phenomenon to many physicians - one they don’t want to concern themselves with just yet. However, in the past few years, P4P programs have proliferated. Virtually all major payers, including Medicare, are piloting P4P programs and will soon be measuring physician performance and offering financial incentives to those who meet quality targets. Although early results of P4P programs were not entirely positive, and although much debate surrounds this movement, there are no signs of a slowdown.
The March 2004 issue of Family Practice Management highlighted the early trends in P4P programs and provided guidance on how to get involved.1 This article provides an update on the trends, issues and lessons learned, including implications for family physicians.
The state of P4P programs
According to a large, national study conducted in 2005 by Med-Vantage, there are 107 active P4P program sponsors nationwide, covering more than 53 million Americans. (See “Growth of P4P programs.”) It is estimated that by 2008 there will be more than 160 P4P programs covering more than 85 million Americans.2
Although primary care physicians continue to be the key targets for P4P programs, both specialist and hospital components are growing. For instance, more than 95 percent of P4P programs include primary care physicians, whereas 52 percent also include specialists (with cardiology, orthopedics, obstetrics-gynecology and endocrinology being the most common) and a full third include hospitals. Finally, 64 percent of P4P programs now measure and reward individual physician performance, not just group performance.2
P4P programs use a variety of methods to reward physicians financially for achieving targets. Fee differentials (i.e., a percentage increase in reimbursement when quality standards are met) and bonuses are increasingly the models of choice, while withholds and grants to the practice are rapidly declining in use (see “Types of incentives”).2 The decline in withholds is particularly good news for physicians because this strategy involves taking away a portion of physicians’ regular reimbursement amounts unless targets are met. Some health plans have developed models under which they share with physicians any savings realized through their quality improvement efforts, representing an unprecedented positive alignment of physician and payer incentives.
Three quarters of all P4P programs provide report cards to participating physicians, and roughly half of these programs provide actionable information to assist the practice (such as patient education materials or patient reminders to help eliminate gaps in care). Only a third of P4P programs publicly report performance to aid in consumer choice. This is expected to grow to 50 percent by 2007 as consumers, purchasers and health plans push for greater transparency in cost and quality data.2
P4P programs focus on a range of performance measures. While clinical measures continue to be the primary focus of performance measurement, 50 percent of P4P programs now include efficiency measures (such as the number of inpatient admissions or rate of prescribing generic drugs). Use of information technologies, such as electronic health records, patient registries and electronic prescribing, are also rewarded in 42 percent of programs.2 The mix of measures is highly variable between programs, as is the weighting assigned to each measure within the performance measure set. For example, 50 percent of a bonus might be based on clinical performance, 40 percent on efficiency measures and 10 percent on use of information technology.
Over 80 percent of the measures used in P4P programs are HEDIS (Health Plan Employer Data and Information Set; http://www.ncqa.org/programs/hedis) measures from the National Committee for Quality Assurance. Internally developed measures are used in approximately 50 percent of P4P programs.2 Recently, a consortium of major specialty societies including the AAFP, the Centers for Medicare & Medicaid Services (CMS), America’s Health Insurance Plans (the trade association for health plans) and numerous employers, accrediting associations and others designated a “starter set” of 26 office-based measures for use in pay-for-performance programs. (These measures are listed in the related article.) The consortium, the Ambulatory Care Quality Alliance, views these 26 measures as the beginning of a national measure set for pay for performance and is testing these measures in pilot projects in six states (Arizona, California, Indiana, Massachusetts, Minnesota and Wisconsin).
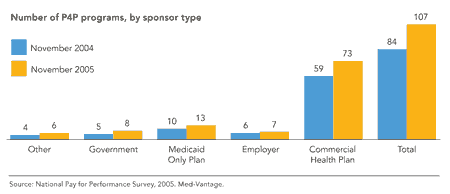
GROWTH OF P4P PROGRAMS
Between 2004 and 2005, the number of pay-for-performance programs grew from 84 to 107. The majority are sponsored by commercial health plans.
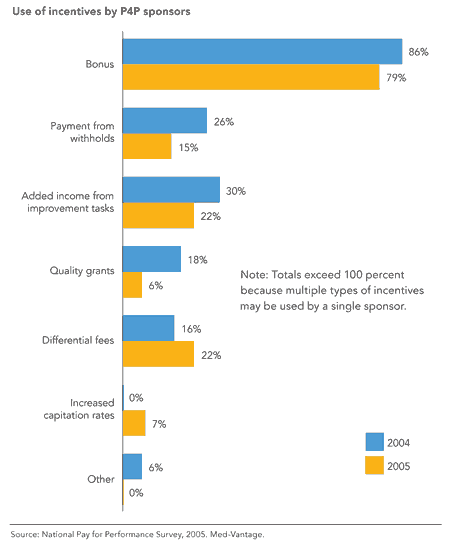
TYPES OF INCENTIVES
Pay-for-performance program sponsors offer a variety of incentives to physicians to encourage them to meet defined performance standards. Bonuses are by far the most common incentive used.
National initiatives
Today, the largest P4P programs in terms of total payments and patient volume are those sponsored by health plans. National health plans such as Aetna, Cigna, Humana and UnitedHealthcare are all experimenting with P4P pilots.
In addition, significant P4P programs are being led by coalitions, such as the following:
Bridges to Excellence (http://www.bridgestoexcellence.org) is a coalition of health plans and employers active in 16 states. It offers three P4P programs with incentives for meeting criteria related to office systems improvement (up to $50 per year for each participating patient), diabetes care (up to $80 per year for each participating patient) and cardiac care (up to $160 per year for each participating patient).
The Integrated Healthcare Association (http://www.iha.org) is a California-based coalition of six health plans representing more than 200 physician practices and more than 7 million covered lives. Through its Rewarding Results program, physicians are measured on their clinical performance, patient experience and use of information technology. Bonuses average from $5,000 to $10,000 per physician per year.
Medicare (http://www.cms.hhs.gov) is also becoming a leader in the P4P arena. CMS Administrator Mark McClellan, MD, has estimated that performance-related payments may account for up to 30 percent of Medicare payments in the next 10 years.3 Currently, two major ambulatory demonstration projects are underway, as mandated by the Medicare Modernization Act of 2003. The first project, the Medicare Care Management Performance Demonstration, is a three-year program aimed at improving care through the adoption and use of electronic health records in four states: Arkansas, California, Massachusetts and Utah. Physicians who meet or exceed performance standards in diabetes and heart disease are eligible for bonuses under the program. The second project, the Medicare Physician Group Practice Demonstration, was launched in 2005 and is aimed at measuring and rewarding performance within 10 large group practices based on 32 quality indicators.
In addition, in January 2006, CMS launched the Medicare Physician Voluntary Reporting Program (PVRP; http://www.cms.hhs.gov/PVRP/) to stimulate voluntary reporting of 16 performance measures, seven of which are applicable to family physicians. The measures are designed to be reported to CMS as G codes. CMS has made the program optional for now with the intention of giving physicians more time to implement electronic health records, which will make the reporting process much easier. It is anticipated that CMS may begin to require reporting and use the data to pay for performance beginning in 2008.
The physician perspective
Naturally, any movement that adds performance pressures to physicians and alters how they are paid will be heavily debated. Physicians have a number of legitimate concerns.
Inadequate incentive levels. A practice’s ability to afford the improvement work needed to meet P4P requirements often depends on the bonus potential and the number of eligible patients in the practice.4,5 Under single-sponsor programs, small- to medium-sized practices may not have enough eligible patients to generate significant bonuses; in fact, reimbursements may not cover the practice’s expenditures for quality improvement and data collection. Moreover, 50 percent of P4P programs offer payments that equal less than 10 percent of practice revenues.1 It has been estimated that a 10-percent bonus is the minimum needed to sustain improvements in physician practices.6
Limited focus of performance measurement. Most P4P programs focus on measuring a limited number of clinical, administrative or information technology areas. As a result, physicians may tend to invest in improving only these areas and may shift resources away from areas not being measured.
Fairness of incentive distributions. Many P4P programs require physician practices to meet specific levels of performance before they can qualify for added reimbursement. Larger and better-endowed practices are more likely to start out at or above the performance threshold than smaller practices. Thus, P4P programs may be rewarding already high-performing practices and may limit potential incentives for smaller practices that make large improvements but fail to reach the threshold.
This scenario has been borne out in a California P4P program, where participating physician groups that began at or above the baseline threshold improved the least but earned the most in bonus payments.7 Some P4P sponsors have recognized this potential inequity and have designed programs that reward physicians for their degree of improvement.
Impact on quality
Evidence on the impact that P4P programs have on quality of care is mixed at best. It is speculated that incentives totaling less than 10 percent of revenues have little impact on quality. One study found that performance on only one in three measures was significantly better in practices participating in P4P programs than in comparable control practices.7 However, some evidence suggests that at least some physicians do believe that incentive programs lead to improved care.8
Impact on health disparities. Practices with sicker or socioeconomically disadvantaged populations may have a more difficult time meeting P4P requirements. Physicians may also be tempted to limit access or close their practices to these vulnerable patient groups in order to garner financial incentives. Evidence suggests that health disparities do worsen when there is public performance reporting.9 This effect may be exacerbated when payment is at risk.
In addition to the above concerns, there are a number of issues related to the validity of performance measurement based on claims data.
Focus on quality of care.
Support the physician-patient relationship.
Use evidence-based guidelines in judging physician performance.
Involve physicians in P4P program design.
Use reliable, accurate and scientifically valid data.
Reward physicians with positive incentives (rather than withholds, for example).
Make participation voluntary.
Before enrolling in any P4P program, family physicians should make sure the program meets the above principles and should ask five key questions:
How often is the performance information delivered to physicians? You’ll want to know whether you can expect feedback annually, quarterly, etc. In general, more immediate feedback is preferable because it allows you to correct performance problems sooner.
How is the data collected and scored? You need to know whether you will be accountable for patients who have selected you as their primary provider but never set foot in your office or don’t comply with your treatment recommendations, whether performance data will be drawn from the claims you submit to the health plan, etc.
What measures will be used, what are their specifications, who developed the measures, and what evidence supports their use? Ideally, the measures would match the starter set endorsed by the Ambulatory Care Quality Alliance, as they have been thoroughly reviewed.
What is the process for data correction and appeal? The program should offer some means for reviewing and correcting the data in case it contains errors. Additionally, conducting your own performance measurement with data drawn from your patient records will make it easier to dispute data that a health plan may have produced based on a limited number of claims.
What actionable information will be provided? For example, the best programs will not simply tell physicians they need to improve their tracking of patients with diabetes but will generate a list of patients who are overdue for their diabetes checkups.
The payer perspective
Rising health care costs and pressures from purchasers to stabilize premiums are driving health plans to embrace pay for performance. The underlying business assumption is that providing incentives for targeted outcomes will lead to practice improvement in those areas, leading to increased efficiencies and ultimately cost savings.
Health plans may realize additional savings if they use performance data not only internally to motivate physicians but also publicly to motivate patients to make cost-efficient choices. Tiered provider networks are one way of doing this. Under a tiered network, patients are given incentives for selecting higher performing, more efficient practices (and avoiding lower performing, less efficient practices). Last year United Healthcare attempted such a program, offering lower co-payments to patients in certain markets if they would visit physicians who had reached certain quality markers. These physicians were designated with gold stars next to their names in the provider directory; however, some physicians were not eligible for the designation simply because of insufficient claims data. The AAFP protested the pilot program, and United has announced that it will not pursue the program for primary care. This experience illustrates the pitfalls of profiling and tiering strategies.
In addition, a systematic review suggests that the successful use of incentives is a complex endeavor.13 It depends on multiple factors such as who receives the incentive (e.g., the patient, the practice or the physician), the revenue potential, the perceived attainability of the measures, physician acceptance of the incentive or performance goal, and general characteristics of the provider, the market, the organization and the patients. Clearly, health plans trying to do pay for performance right have a complicated task ahead of them.
TELL US ABOUT YOUR PAY-FOR-PERFORMANCE EXPERIENCE
Have you participated in a pay-for-performance program? If so, we’d like to hear about your experience. What impact did your participation have on your patients’ health or your practice’s bottom line? Describe your experience, good or bad, and send it by e-mail to fpmedit@aafp.org. We may select your letter for publication, or we may contact you for more information as we prepare future articles on this subject.
A look ahead
Despite its challenges, pay for performance is here to stay. It is evolving into a more rational mechanism for rewarding quality of care.
In the coming years, P4P programs will continue to grow in number and diversity and will continue to develop based on lessons learned from early implementation efforts. Following the model of Bridges to Excellence and others, more and more health plans and employers will come together to design multisponsor programs, which will help to ensure that practices have more eligible patients and higher bonus potential. Nationally endorsed measure sets, such as the 26-measure starter set, will broaden and become widely used. Payments will increasingly be based not only on meeting thresholds but also on realizing improvements, thereby easing concerns about inequity. Risk-adjusted payments will address some of the issues of health disparities. Productive dialogue will take place between physicians and payers around the improvement of outcomes. And, finally, physicians will be rewarded for providing high-quality care.