
Fam Pract Manag. 2006;13(9):26
Physicians brace for Medicare pay cut in 2007
Although Congress still has time to act to avoid a 5.1-percent cut in physicians’ Medicare payments in 2007, hope is growing dim.
The threat of Medicare payment cuts has been an annual occurrence since 1997, when lawmakers introduced the “sustainable growth rate” formula, which limits physicians’ fees if Medicare costs outpace inflation. In most years, Congress has acted at the final hour to prevent the cuts, but this year might be the exception.
While physician groups such as the AAFP and the AMA advocate doing away with the current flawed formula and instead paying physicians based on actual costs, Centers for Medicare & Medicaid Services (CMS) officials have expressed interest in a different type of reform: a Medicare pay-for-performance program.
“To throw more money into this old system is not the right answer. We need to work together to find a better and more appropriate way to pay,” said Herb Kuhn, head of the CMS Center for Medicare Management, in the Sept. 8 Los Angeles Times.
But talk of a Medicare pay-for-performance program might seem untimely to physicians, whose immediate concern is stopping the payment cuts.
“The predicate for having a quality system is to have enough funding in the system for physicians to be able to afford to practice,” said AMA board member William A. Hazel Jr., MD, also quoted in the Times.
Without a permanent payment fix, physicians’ Medicare reimbursements could decline nearly 37 percent over the next nine years while practice costs increase 22 percent, according to government estimates.
What the surveys say
An AMA survey estimates that 45 percent of physicians will be forced to decrease or stop seeing Medicare patients if payments are cut in 2007.
In a separate survey, the Medical Group Management Association found that, if the payment cut goes forward, medical practices will face serious financial struggles: 39 percent would lay off clinical staff; 54 percent would lay off administrative or support staff; and 67 percent would modify or eliminate health benefits for employees.
In a survey of patients, the AMA found that 70 percent of the public had not heard about the planned cut in physician payments; however, when told of the cut, 86 percent expressed concern that it would harm seniors’ access to care.
Docs get raises while groups fight losses
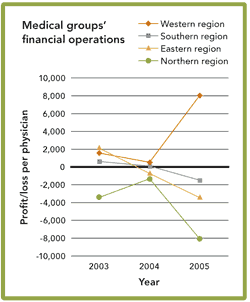
A recent survey of large group practices indicates that although compensation for most medical specialties rose last year, most medical groups operated at a financial loss.
The annual Medical Group Compensation & Financial Survey, published by the American Medical Group Association, indicated that compensation for family physicians increased 8.6 percent, from $164,209 in 2004 to $178,366 in 2005. The average overall increase among specialties was about 6 percent. Dermatologists reported the largest increase in compensation at 12 percent (from $274,014 to $306,935), while hematologists and oncologists reported the lowest increase at 3.3 percent (from $255,007 to $263,284).
The medical groups that responded to the survey indicated that they were operating at an average loss of $1,264 per physician. That number varied from region to region (see the chart).
Almost three-fourths of the 218 medical groups that responded to the survey employ at least 35 physicians. The average group size was 161 physicians. Physicians owned 48 percent of the medical groups that participated in the survey.