
Fam Pract Manag. 2007;14(4):20-23
2007 Match results: Family medicine stays flat
The number of medical school seniors who matched with a family medicine residency program remained essentially unchanged this year at 2,313 seniors. The specialty's overall match rate improved slightly (88 percent in 2007 vs. 85 percent in 2006) due to a decrease in the number of family medicine positions offered – roughly 100 fewer positions than in 2006 and more than 600 fewer than a decade ago.
Of the family medicine positions filled, 42 percent were filled by U.S. seniors, similar to the percentage in the past five years but far below the percentage 10 years ago (see graph).
The primary care components of internal medicine and pediatrics also experienced stagnant numbers this year.
“Medical students have continued to demonstrate a preference for medical subspecialties over primary care, although the preceding drop in interest in primary care has stabilized over the past few years,” says an AAFP summary of the Match results. It suggested that the income gap between primary care physicians and other specialists and increasing student-loan debt may be contributing to the low levels of student interest in primary care.
Both the AAFP and the American College of Physicians have expressed concern that without increases in the number of medical students choosing careers in primary care, the United States will not have enough physicians to care for an aging population. Additionally, a more specialized physician workforce will lead to higher costs.
“Family medicine is a critical part of the solution to providing high-quality, affordable and accessible health care to everyone,” said AAFP President Rick Kellerman, MD. “Studies clearly demonstrate that a higher ratio of primary care physicians, particularly family physicians, to population leads to better health outcomes and lower costs.”
FAMILY MEDICINE MATCH RESULTS: 10-YEAR TREND
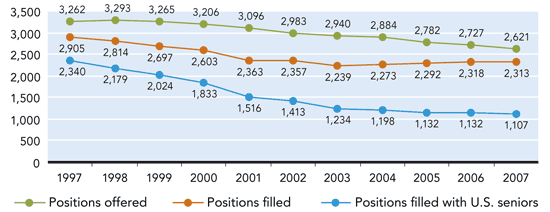
Source: AAFP summary of National Resident Matching Program data, March 15, 2007.
New CMS-1500 claim form delayed by formatting error
If you didn't make the April 1 deadline for using the new CMS-1500 claim form, don't worry. The Centers for Medicare & Medicaid services recently suspended the deadline after discovering that forms printed by the Government Printing Office are improperly formatted, causing critical information to be missed by carriers' scanning technology.
Forms printed by other vendors may also be affected, so physicians should examine any new CMS-1500 forms (version 08–05) they have purchased.
According to CMS, in the upper right-hand corner of properly formatted claim forms, there should be a quarter-inch gap between the tip of the arrow (above the word “carrier”) and the top edge of the paper. If the tip of the arrow is too close to the top edge of the paper, then the form is not printed to specifications.
CMS has directed Medicare carriers to return any claims filed on flawed CMS-1500 forms to providers. At press time, CMS was considering June 1 as the revised deadline for implementation of the new form. Medicare carriers will accept the old CMS-1500 form (version 12–90) until that date.
One of the main reasons CMS revised its claim form was to accommodate the new National Provider Identifier, which providers must begin using on May 23.
Conn. bill seeks to limit claim denials
A bill recently introduced in Connecticut could make it harder for insurers in the state to use medical necessity as the basis for denying a claim. The bill (HB 7055) would shift the burden of proof to insurers and would require them to show why a particular medical service is not medically necessary before they could deny claims for that reason.
The bill deems a service to be medically necessary if it is recommended by the treating physician or other licensed provider and meets certain other criteria.
“This legislation seeks to restore consumer control over health care decisions by creating a presumption … that a physician's diagnosis and treatment is medically necessary,” said Attorney General Richard Blumenthal in the Feb. 23 Hartford Currant.
The Connecticut Association of Health Plans opposes the bill, saying it would lead to unlimited coverage and would drive up premiums.
So many topics, so little time during office visits
An average of six topics surface in a typical primary care office visit with elderly patients, leaving a limited amount of time to discuss all of the issues fully, says a study published online Jan. 24 by Health Services Research.
Researchers videotaped 392 routine office visits involving primary care physicians and patients age 65 or older. The median visit length was 15.7 minutes, with about five minutes spent on the longest topic and 1.1 minutes spent on additional topics. Visit length varied little overall even when the contents of visits varied widely.