
Fam Pract Manag. 2007;14(7):19-23
Union barred from helping doctors negotiate with insurers
The Federation of Physicians and Dentists, an AFL-CIO-affiliated union, has been barred from helping doctors negotiate better payment rates and contract terms with health care insurers. The action is part of a settlement with the Department of Justice, which had accused the federation in 2005 of violating antitrust laws by coordinating approximately 120 obstetrician-gynecologist members in the Cincinnati area to negotiate more favorable fees in their contracts with insurers. The physicians' contract demands were allegedly accompanied by threats of contract termination.
The settlement prohibits the union from reviewing physicians' contracts with payers, communicating with physicians regarding their contracts and educating physicians about contracting or negotiating with payers.
Thomas O. Barnett, assistant attorney general in charge of the Department's Antitrust Division, said the case demonstrates their commitment to stop “illegal conduct that harms the public by increasing the prices that consumers and their employers pay for health care.”
AMA issues separate challenges to United Healthcare, retail clinics
The AMA tackled two issues at its recent annual meeting that are important to family physicians. The group's first target was insurer United Healthcare and its relatively new policy of fining doctors who use out-of-network labs. The AMA is concerned that other insurers will adopt similar policies.
The group's House of Delegates passed a resolution presented by the Michigan delegation that calls on the AMA to “oppose any penalties implemented by insurance companies against physicians when patients independently choose to obtain out-of-network services.” The resolution could lead the AMA to lobby at the federal level against the insurer's policy.
Another resolution passed at the AMA meeting in June focused on the second target: retail health clinics. The group called for state and federal investigations into the relationship between store-based retail clinics and the pharmacies that are located in the same store.
“There are clear incentives for retailers to participate in the implementation and operation of store-based health clinics, “said AMA Board Member Peter Carmel, MD. “The nation's physicians want the AMA to ensure these incentives do not compromise the basic obligation of store-based health clinics to provide patients with quality care.”
Tine Hansen-Turton, executive director of the Convenient Care Association, responded to the AMA. “We are surprised that the AMA would take the position that it has, because so many physicians and other health care professionals have accepted this new model and see it as part of the solution to our broken health care system,” Hansen-Turton said.
The AMA's call for a look into retail health clinics also includes a challenge to insurers' practice of waiving co-pays for patients who visit such clinics.
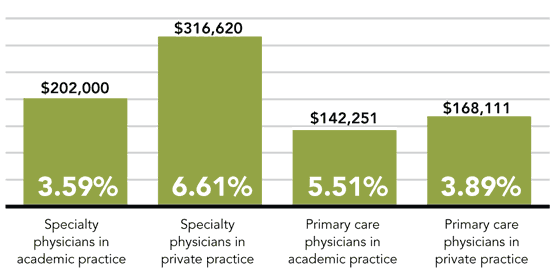
Academic practice vs. private practice
Overall compensation for primary care physicians in academic practice grew last year at a faster rate than that of primary care physicians in private practice, while the opposite was true of specialists in the two settings.
IRS OKs EHR donations from hospitals
A recent directive from the Internal Revenue Service (IRS) brought good news for physicians who work with hospitals. The IRS memo states that hospitals can donate electronic health record (EHR) software and services to medical staff physicians without violating their not-for-profit status.
“We will not treat the benefits a hospital provides to its medical staff physicians as an impermissible private benefit,” the May 11 memo stated.
The IRS decision allows hospitals to finally act on the August 2006 ruling of the Department of Health and Human Services, which made hospitals' EHR donations to staff physicians exempt from federal anti-kickback and self-referral laws. To qualify for the safe harbor rules, the EHR-related donations must be interoperable.
“For those (hospitals) who want to go forward, this clears the deck,” David C. Kibbe, MD, MBA, senior adviser to the AAFP's Center for Health Information Technology, told AAFP News Now.
Pay-For-Performance Doesn't Necessarily Improve Care, Study Says
Giving hospitals financial incentives to follow treatment guidelines may not bring about improvements in quality of care, according to a study published in the June 6 issue of the Journal of the American Medical Association.
The study included cardiac care data from 54 hospitals participating in a pay-for-performance pilot program launched in 2003 by the Centers for Medicare & Medicaid Services. While researchers found significant improvement among the 54 hospitals in areas such as prescribing aspirin at discharge following a heart attack and providing smoking-cessation counseling, they found similar improvements in 446 other hospitals without a pay-for-performance program.
Researchers noted they did not find any adverse consequences of using financial incentives, such as physicians paying undue attention to aspects of care subject to incentives to the detriment of other aspects not subject to incentives.
“The results of this study raise concerns about what magnitude of effect pay-for-performance programs should have to justify the administrative burden and potential unintended consequences of financial incentives,” researchers wrote.
Medical group goes public with its fees
HealthCare Partners, a large, private medical group in California, recently took a bold step by publicly posting its fees for 58 common services, from a flu vaccine ($15) to a well baby exam ($65-$80) to a colonoscopy ($424). The fee schedule is viewable online at http://www.healthcarepartners.com/brochures/BasicFees_Web.pdf.
The group says it is simply responding to market demands for price transparency, which aids consumers who participate in high-deductible health plans or have health savings accounts and need to better manage their health care dollars.
“Health care delivery is becoming more consumer-oriented, and posting our prices is a next logical step in its evolution,” said the group's CEO, Robert J. Margolis, MD. “People have told us they want to know how much they are paying for the health care services they need, so that they can plan and make the most informed decisions. These postings will prove extraordinarily helpful for patients who are budgeting with their annual insurance deductibles or medical savings accounts in mind.”
Health insurers are also becoming increasingly interested in price transparency. Earlier this year, Aetna expanded the number of regions in which it gives members online access to participating physicians' negotiated prices for common services. The affected regions are now Atlanta; Connecticut; south Florida; Houston; southeast Indiana; Kansas City; northern Kentucky; Las Vegas; Maine; Maryland; parts of Ohio; Oklahoma City and Tulsa, Okla.; Pittsburgh; Utah; northern Virginia; and Washington, D.C.
The Centers for Medicare & Medicaid Services has also announced plans to begin posting online the prices it pays for physicians' services.
Medicare makes last-minute changes to PQRI codes
The Centers for Medicare & Medicaid Services has issued a few last-minute changes to its coding requirements for the Physician Quality Reporting Initiative (PQRI), which began on July 1.
One change relevant to family physicians is that, when submitting a CPT II code (or “quality code”) for lipid management or blood pressure management related to diabetes, the only available modifier is now 8P, “Performance measure exclusion due to action not performed, reason not otherwise specified.” Modifier 1P, for reporting that a measure was not performed due to medical reasons, is not to be used in these cases. CMS also removed the code for the “Welcome to Medicare” physical from the diabetes measures and added codes for medical nutrition therapy.
To view all changes, visit the CMS Web site at http://www.cms.hhs.gov/PQRI/15_MeasuresCodes.asp.
The AAFP's PQRI data collection sheets have been updated and can be downloaded at https://www.aafp.org/practicemgt/pqri.
Spending study prompts call for diabetes czar
The federal government's price tag in fiscal year 2005 for treating Americans with diabetes was $79.7 billion more than it was for Americans without diabetes. That equates to about one in every eight dollars spent by the government on health care.
“We are spending as much on diabetes as we are on the entire Department of Education, but no one is leading the effort,” said Dana Haza, senior director of the National Changing Diabetes Program, a group created and funded by Novo Nordisk.
A study prepared for Haza's group found that the federal government spent $3.9 billion in fiscal year 2005 on disease prevention and health promotion. Only $0.2 billion of that was spent exclusively on diabetes. In addition, the $3.9 billion was spread out among numerous government agencies, with little coordination among them.
The National Changing Diabetes Program is calling for the creation of a national coordinator for the federal government's diabetes-related efforts.