
This special report reviews the value of family medicine, the challenges it faces, and AAFP data on the nature of family medicine practice today.
Fam Pract Manag. 2012;19(1):20-26
Brandi White is senior editor of Family Practice Management. Author disclosure: no relevant financial affiliations disclosed.

At the start of each new year, when the President of the United States delivers his State of the Union address, the standard conclusion is that the state of our union is “strong.” It's a comforting adjective; however, it doesn't always apply. For example, in 1975, President Gerald Ford concluded that the state of the union was “not good.” A year later, he upgraded it to “better … but still not good enough.” At the other extreme, President Bill Clinton declared in 2000 that the state of the union was “the strongest it has ever been.”1
How would you describe the state of family medicine? “Strong?” “Not good?” Or perhaps “the strongest it has ever been?” It's a complicated question involving multiple factors. This article will examine three important ones.
1. The value of family medicine and primary care
Primary care stepped into the spotlight in 1978 when a group of global health care leaders issued the Declaration of Alma-Ata. It was the first international pronouncement that primary care should be the central function and main focus of an effective and just health care system.
Since that time, an extensive evidence base has developed demonstrating that when patients have access to good primary care – characterized by first-contact care, person-focused care over time, comprehensiveness of care, and coordination of care2 – good things happen. Health care quality and health outcomes improve.3,4 Problems are diagnosed earlier.5–7 Self-reported health, both general and mental, improves.8 Disparities are reduced.8 Hospital admission rates and emergency room utilization rates decline.9–12 And costs go down.4,13,14 In short, the entire health care system becomes more efficient and effective.15,16
“The evidence about the value of primary care to people and to the health system is growing, and the value is strongest for the type of primary care delivered by family medicine,” said Robert L. Phillips Jr., MD, MSPH, director of the AAFP's Robert Graham Center for Policy Studies in Family Medicine and Primary Care.
But there is a caveat: “This value is at some risk as family medicine shrinks its scope of practice and comprehensiveness – an obvious trend over the last decade,” said Phillips. “This value is enhanced where family medicine is able to fulfill its broadest scope, and where it is able to deliver both personal and population health.”
Recent research has emphasized that the health care system needs more physicians who practice robust primary care in an office or clinic setting, as opposed to more physicians who are primary care in name only.17
2. Efforts to strengthen primary care
Despite the evidence of the value of primary care, it has not historically been well supported in this country. This helps explain why the United States' health care system lags behind systems of other developed nations,18 and why primary care has faced challenges attracting students of late.19 However, recent concerns about costs and quality have created a burgeoning interest in primary care. “It is remarkable that in just a couple of years, the stock of primary care has risen dramatically,” said Kevin Burke, director of government affairs for the AAFP in Washington, D.C. “Legislators in Congress who deal with health care issues profess great interest and support for primary care, and we have seen legislative proposals make this clear.”
NUMBER OF STUDENTS MATCHING WITH FAMILY MEDICINE BY YEAR
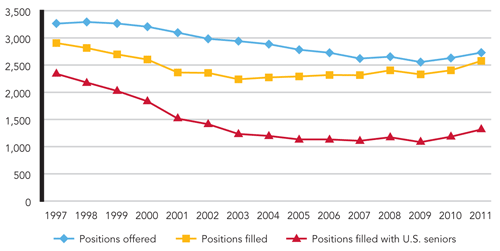
The number of U.S. seniors matching to family medicine residency positions rose by 11 percent in 2011. Family medicine offered 2,730 positions (100 more than in the previous year), and U.S. seniors filled 1,317 positions, the highest number since 2002. While this is a noteworthy increase, it is insufficient to meet the current and anticipated demand for primary care physicians in the United States.19
Source: National Resident Matching Program
For example, a recent proposal from Rep. Allyson Schwartz, D-Penn., calls for replacing the flawed sustainable growth rate formula, which threatens physicians' Medicare payments every year, with a payment system that builds in higher payment rates for primary care services offered by primary care physicians. Additionally, the “Primary Care Workforce Access Improvement Act of 2011” (HR 3667), introduced in December with bipartisan support, would provide Graduate Medical Education (GME) payments to non-hospital programs that train family physicians. This is “a major step toward GME payments for family medicine residencies, which was unthinkable a few years ago,” Burke said.
Of course, while legislative proposals are nice, what really matters is passed legislation. The best example of this is the Medicare Primary Care Incentive Payment Program mandated as part of the Affordable Care Act (ACA). Since January of last year, it has provided a 10 percent quarterly bonus to primary care physicians, as long as 60 percent of their Medicare charges are for primary care services. An estimated 80 percent of family physicians are eligible. The bad news is that the program is not permanent. It will end Jan. 1, 2016, unless legislative changes are made. Also mandated by the ACA, and also temporary, is a measure to increase Medicaid payments for primary care services in 2013 and 2014 so that they are at least equal to Medicare payments.
Another promising program, although it is just a demonstration project at this point, is the Comprehensive Primary Care Initiative launched in October by the Center for Medicare and Medicaid Innovation. This program will pay participating practices a blend of fee-for-service payments and a risk-adjusted care-coordination fee of $20 per member per month, on average. Practices will also have the potential to share in any savings resulting from the program. (See the related article.)
Dozens of other programs are rewarding primary care practices that operate under the patient-centered medical home (PCMH) model, which stresses improved access, care coordination, disease management, and quality improvement. One program of note is Maryland's Multi-Payer PCMH Program, which recently paid biannual incentives averaging $56,000 to 54 participating primary care practices in the state.20
“The intention to help primary care physicians, especially family physicians, is real,” said Burke, but he acknowledged that “the results are sometimes mixed” and there is clearly more work to be done to ensure that primary care incentives are sufficient, permanent, and more widely available.
3. Family physician income, workload, and other key metrics
Given the upheaval in the health care system, including pressures for meaningful use of health IT, the need to prepare for ICD-10, and the desire to maintain a profitable practice, what does it look like to practice family medicine today? According to AAFP data, the average family physician works 51 hours per week, 47 weeks per year, and makes $160,000 per year. He or she spends 34 of those hours providing face-to-face patient care, seeing 99 patients per week in all settings. An average of 7.4 hours each week – almost an entire workday – are spent on administrative tasks, with 2.6 of those hours spent on prior authorizations alone.21
AVERAGE HOURS SPENT PER WEEK IN PRACTICE
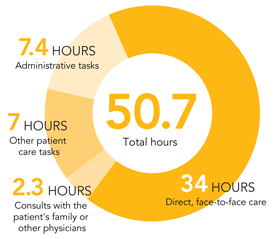
The average family physician respondent works 47 weeks per year and spends a total of 50.7 hours per week engaged in tasks related to medical practice. The majority of that time is spent in direct, face-to-face patient care. Of the 7.4 hours spent per week on administrative tasks, 2.6 hours are related to prior authorizations.
Source: AAFP 2010 Practice Profile I, April 2011
DISTRIBUTION OF FAMILY PHYSICIANS BY ANNUAL INCOME
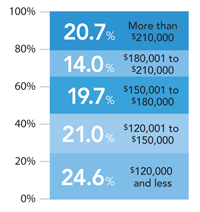
Family physicians' median net individual income from medical practice was $160,000 in 2009 (the mean was $173,710); however, income varied widely depending, presumably, on work hours, region, etc. In 1996, the median income was $124,000,23 which would be roughly $179,000 in today's dollars.
Source: AAFP 2010 Practice Profile I, April 2011
AVERAGE NUMBER OF PATIENTS SEEN PER WEEK BY SETTING
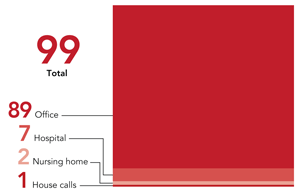
The average family physician respondent has a panel of 3,281 active patients (i.e., the number of patients seen in the last three years), with the vast majority of patients being seen in the office setting. Although hospital-based care remains an important part of practice, it has lessened over the years. For example, in 1997, family physicians saw 12 patients in the hospital each week on average,23 nearly double the current number. In addition, while 66 percent of family physicians today have hospital admission privileges, 86 percent had admission privileges in 1997.23
Source: AAFP 2010 Practice Profile I, April 2011
When asked “Who is your primary employer?” family physicians congregate around three answers: 30 percent say they are employed by a hospital or health system, 24 percent say they are their own employer (self-employed, majority practice owner, independent contractor, etc.), and 22 percent cite a physician group.22 In 1998, AAFP data found similar results: 28 percent worked in practices owned by a hospital or health system, 26 percent considered themselves the practice owner, and 25 percent were employed by a group practice.23
DISTRIBUTION OF FAMILY PHYSICIANS BY PRIMARY EMPLOYER
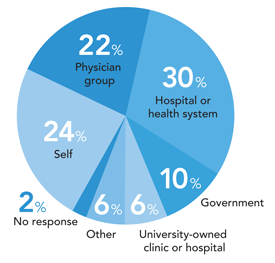
Thirty percent of family physicians consider their primary employer to be a hospital or health system. Almost a quarter consider themselves to be the primary employer (self-employed, majority practice owner, independent contractor, etc.), and 22 percent consider a physician group to be their primary employer. It's possible that some physicians in this latter category have a small ownership stake in their practices, because 35 percent of overall respondents indicated that they are the sole owner, a partial owner, or a shareholder.
Source: AAFP 2011 Member Census, Aug. 30, 2011
The vast majority of family physicians provide care for patients of all ages, manage chronic diseases, and provide urgent care, among other services, but relatively few provide obstetric care (15 percent in 2010 versus 30 percent in 1998) or intensive care (20 percent in 2010 versus 55 percent in 1998).22,23 In addition, while 66 percent of family physicians today have hospital admission privileges,21 86 percent had admission privileges in 1997.23 The most common procedures performed today are skin procedures and musculoskeletal injections. Procedures such as flexible sigmoidoscopy and vasectomy are performed less often by family physicians today than they were more than a decade ago.22,23
CLINICAL SERVICES MOST COMMONLY OFFERED BY FAMILY PHYSICIANS
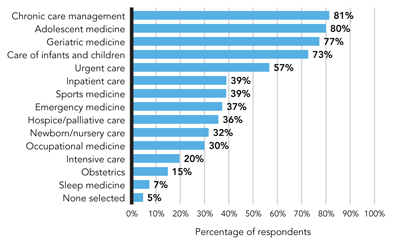
The most common services provided by family physicians surveyed include chronic care management, care to all ages (from infants to seniors), and urgent care. (Preventive care was not included in the survey.) Some services have diminished over the years. For example 15 percent provide obstetric care today versus 30 percent in 1998,23 and 20 percent provide intensive care today versus 55 percent in 1998.23
Source: AAFP 2011 Member Census, Aug. 30, 2011
PROCEDURES MOST COMMONLY PERFORMED BY FAMILY PHYSICIANS
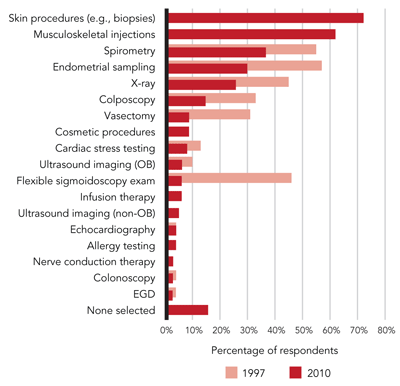
The procedures most often performed today by the family physicians surveyed are skin procedures, musculoskeletal injections, spirometry, endometrial sampling, and X-ray. Where available, 1997 data is given for comparison.
Source: AAFP 2011 Member Census, Aug. 30, 2011, and AAFP Facts About Family Practice, 1998
Although payment and reimbursement issues are of great concern to family physicians, 48 percent say they are satisfied with the financial health of their practices; 29 percent are neutral, and 20 percent are dissatisfied.24
DISTRIBUTION OF FAMILY PHYSICIANS BY SATISFACTION WITH THE FINANCIAL HEALTH OF THEIR PRACTICES
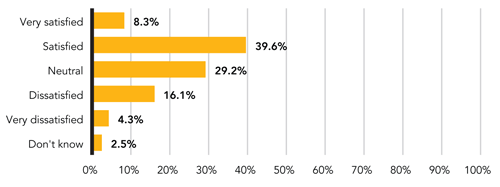
When asked, “Overall, how satisfied are you with the financial health of your practice?” 48 percent of respondents stated that they are satisfied or very satisfied, 29 percent were neutral, and 20 percent were dissatisfied or very dissatisfied.
Source: 2011 Member Satisfaction Study, July 2011
Most practices now use an electronic health record (64 percent) and some version of “open-access (same-day) scheduling” (73 percent), but only 8 percent of practices are certified by the National Committee for Quality Assurance as patient-centered medical homes.21
PRACTICE IMPROVEMENT ACTIVITY BY PERCENTAGE OF FAMILY PHYSICIANS
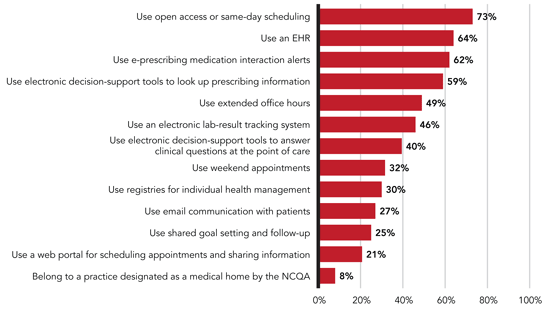
Family physicians report using a number of tools related to practice improvement, with the most common being some form of open-access scheduling (73 percent) and an EHR (64 percent). However, only 8 percent of respondents' practices have been designated as medical homes by the National Committee for Quality Assurance.
It should be noted that in the 2008 National Ambulatory Medical Care Survey, which provides a national sample, the percentage of family physicians using an EHR was lower, at 50.2 percent.
Sources: AAFP 2010 Practice Profile I, April 2011
The state of family medicine is …
F. Scott Fitzgerald wrote in The Crack-Up that, “The test of a first-rate intelligence is the ability to hold two opposed ideas in the mind at the same time, and still retain the ability to function.” This seems applicable to a discussion of the state of family medicine. On the one hand, family medicine has its challenges, including administrative hassles, a lack of support in the health care system, and threats to its comprehensiveness and scope of practice. On the other hand, family medicine has a lot going for it, including recent efforts to create primary care incentives, incomes well above the national average, and solid evidence of its value to the health care system.
One could argue, then, that the state of family medicine is best described in this way: It is at once incredibly challenging and incredibly rewarding. Family physicians all across the country and in all kinds of settings live this dynamic tension every day. And, as Fitzgerald said, that takes a first-rate intelligence.
