
A filtered display would make notes easier to read, assimilate, and use.
Fam Pract Manag. 2013;20(3):8-9
Author disclosures: no relevant financial affiliations disclosed.
Why is it so hard to read electronic health record (EHR) progress notes? A number of causes have been richly described in the literature, most commonly copy-and-paste errors. We want to focus on a cause discussed less frequently: Our notes try to meet the needs of too many stakeholders and all their foreseeable tasks.
What the auditor or malpractice defense attorney wants to see is often at odds with what the busy physician needs to see at the point of care or when reviewing the last few notes before entering the exam room for a patient visit.
Really good information design provides only the information that the user needs for the task at hand. We need our EHRs to display to users “what they need, when they need it, and nothing more.” We envision a model that would do just that, using a multilayer template that we propose EHR companies should develop for their systems.
Six layers
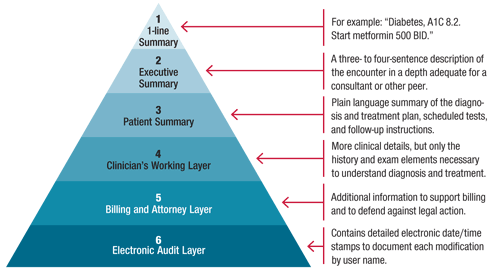
Imagine the individual document in an EHR as having six layers, as the illustration below suggests. At the deepest layer, we could see the date/time stamp showing who entered each piece of the note, a level of detail that is usually invisible to all readers.
The layer above would omit the date/time stamps but provide a comprehensive view of the details needed to support billing and defend against malpractice claims.
Because layer five has too much “visual noise” for someone trying to find information at a glance, layer four, what we call the “clinician's working layer,” would provide a more concise view. Only the important clinical details would show. Other information, such as negative review of system (ROS) elements, would be hidden.
Layer three would offer a patient summary including the diagnosis and treatment plan, scheduled tests, and follow-up plans. Translation into plain language would be required, making this the most complicated layer to build.
One layer higher would provide an executive summary. Think of this as what a referring physician would tell a subspecialist (for example, “Evaluate the persistent cough in this man with diabetes who is not taking an ACE inhibitor and is already being treated with omeprazole for GERD”).
Finally, the topmost layer would provide a one-line summary – a terse description of the entire visit.
Is it technically possible?
So how can we use technology to filter information for the type of display we have described? For one, semantic technology could be used to parse the text, find meaning, and display what is relevant. In my opinion, that is in the distant future, and we can't wait that long.
We already know how to filter some content. For example, in the ROS, negatives could be hidden, and positives could be revealed. We could also create an interactive display that would allow us to hide or reveal whole sections quickly on the fly. It could default to show layer four but enable the user to dive to layer five, for example, to see whether a prior note described a murmur. A button, slider, or accordion display would let the user filter or “show more.” The human factors principles at work here aim to reduce cognitive load,1 show information hierarchy clearly, and enable decision making by providing essential details.
Some have asked, “Why bother to do all this when it's the crazy system that needs to change?” We are sympathetic with those who say our biggest problem is the wasteful, distracting paradigm that has us counting bullet points to select codes and documenting defensively to avoid malpractice. However, we think we can improve EHR information display to achieve relief while we continue to advocate for freedom from burdensome documentation requirements.
Unfortunately, the type of multilayer EHR display we've described won't be available this year. Research into the information needs of physicians is ongoing, and software technology is evolving. When a solution arrives, we just need to make sure it doesn't add more physician work to the already onerous process of documentation. We remain hopeful.
