Patients are more likely to schedule a wellness visit if their physician recommends it, but that won't happen without staff support.

Most family physicians would agree that Medicare annual wellness visits (AWVs) are a good idea. They let physicians develop personalized preventive care plans, review and update medical histories, reconcile medication lists, identify other providers involved in the patient's care, and summarize the patient's acute care.1 As a longer visit – often an hour – the AWV lets clinicians escape the “tyranny of the urgent” and develop a proactive, coordinated care plan, which is rarely possible during short, illness-focused office visits.2
In addition, the AWV is well reimbursed. The 2017 Medicare allowances for HCPCS codes G0438 (initial AWV) and G0439 (subsequent AWV) are $173.70 and $117.71, respectively. By comparison, the rate for CPT code 99214 (level 4, established-patient office visit) is $108.74.
Despite these advantages, relatively few patients get an AWV. In 2012, following the first full year in which AWVs were available, less than 10 percent of eligible patients had one.3 Although the completion rate has surpassed 25 percent in some areas, rates in most of the country remain at approximately 10 percent or less.4 This under-use is all the more surprising given that the Centers for Medicare & Medicaid Services (CMS) waived the copay for the AWV, making the visit itself essentially free for patients.
The Department of Family and Community Medicine at the Eastern Virginia Medical School was concerned by the low rates of AWV completion. At our two residency-faculty practices, which serve a diverse urban population, only 153 of our 2,164 Medicare patients age 65 and older, or 7.1 percent, completed an AWV in 2015.
To change this, we launched a quality improvement initiative that ultimately increased patient recruitment and more than doubled our AWV completion rate.
A quick literature review: Why don't patients get AWVs?
We wanted to know why patients in general were not getting AWVs and, in late 2015, began reviewing the literature. There is not a great deal of published material, but several themes emerge. First, some patients have a negative attitude toward preventive care in general (e.g., “I got the flu shot then got the flu.”).5 Negative news coverage may also be a factor. For example, the AWV benefit was launched amid controversy over so-called “death panels,” or the belief of some critics that giving physicians incentives to discuss end-of-life care with patients was designed to limit life-sustaining treatment for older and sicker patients. Although the death panel furor has waned, it may point to a general distrust, which reduces acceptance of the AWV.6
Experience with other preventive benefits fully covered by Medicare, such as the “Welcome to Medicare” visit, indicated that eliminating out-of-pocket costs is insufficient. Most patients are simply unaware of these benefits, and most providers do not advocate their use.7
A recent, qualitative study of AWV usage revealed similar themes.8 Many patients said they had not heard of the AWV and did not understand how it differed from an annual physical or regular office visit. Some patients who had received an AWV said their needs had not been met, especially if there was no physical exam or attention to illness concerns. They were also confused when copays for services such as lab tests, immunizations, and chronic disease management were added to their “free” visit.
Physicians themselves were ambivalent; they saw value in preventive discussions, which they believed they already provided regularly, but felt obliged to provide both wellness and regular care at the AWV – which became overwhelming. They also complained of complex documentation and billing requirements.
Even with these deterrents, many patients who have had AWVs say they did so at the urging of their physician.9
Surveying our patients and providers
To assess patient and provider perceptions in our own practices, we designed two surveys for patients 65 and older with traditional, fee-for-service Medicare – one survey for patients who had had an AWV and one for patients who had not. We did not include our Medicare Advantage patients as they are mostly younger than 65 and their plans require an AWV. During the first two months of 2016, nursing staff distributed the surveys to patients to complete while waiting for their clinician and collected the surveys at checkout. Physicians completed an online survey during the same period. All responses were voluntary and anonymous.
The survey for patients who had received an AWV asked whether they did so at the suggestion of their doctor, whether the visit met all of their needs, whether there were unexpected costs, whether they would recommend the AWV to others, and how helpful specific AWV components were. The survey for patients who had not received an AWV asked whether they had heard of the AWV, whether they had heard bad press about the AWV, whether they were concerned about costs, and whether they saw various AWV components as important. Both surveys inquired about age, race, and gender, but no other demographics were requested. The survey for providers asked about the perceived value of the AWV as well as potential barriers, such as time, training, competing agendas, understanding billing requirements, and level of confidence in carrying out various AWV elements. Respondents could also provide written comments.
We did not track how many patient surveys we distributed, but we received 99 back, including 29 from patients who had had an AWV and 70 from those who had not. The mean age was 74 years; respondents were 50 percent female, 33 percent African-American, 53 percent white, and 13 percent “other.” These results did not vary by site or whether the patient had had an AWV.
Of the providers, 38 of the 64 we contacted online responded (59 percent). Approximately half were residents; the others included family physician faculty members and one physician assistant.
We learned the following:
- 90 percent of patients who had received an AWV said they did so at the recommendation of their physician,
- 61 percent of patients who had not received an AWV said they had never heard of it,
- 14 percent of providers said they saw value in the AWV but were deterred by billing and documentation complexities,
- 16 percent of providers said they were deterred by competing demands.
We found little evidence that patients in our practices devalued preventive care in general or the AWV specifically. We also found no evidence that bad press, unmet needs, or unexpected costs were deterrents.
Our survey also yielded an important and unforeseen benefit: The survey itself acted as a recruiting tool. Many respondents who had not heard of the AWV asked to have one scheduled. Several reported in the comments section that being asked to fill out the survey by an interested and enthusiastic staff member encouraged their interest.
Our solution
Following the survey, we decided in April 2016 to begin leveraging physician recommendation of the AWV with personalized recruitment of patients. A nurse care manager at one of our practices reviewed the daily schedule to identify Medicare patients eligible for a wellness visit. She would then remind the physicians to recommend that their patients get an AWV and ask the medical assistants or other nurses to introduce her to these patients so she could speak to them first-hand. She explained to patients that, for an AWV, they would not see their physician for a physical exam but, at the physician's request, would instead sit down with the care manager for a discussion of wellness and other related topics. As a result, the care manager in the first month recruited 24 patients who completed AWVs with her. This was far ahead of the usual AWV completion rate of about a dozen per month.
Given this initial success, the care manager increased her efforts to three “recruitment days” at one practice and two days at the other. She also worked with other clinic staff, such as licensed practical nurses and medical assistants, so they could recruit patients for AWVs as well. (See “Medicare annual wellness visit recruitment strategies.”)
MEDICARE ANNUAL WELLNESS VISIT RECRUITMENT STRATEGIES

| After describing the visit, try to identify what most appeals to the patient. |
| Focus on patient priority rather than clinical importance. |
| Emphasize that “Your doctor wants you to get this done. It really helps your doctor help you.” |
| Explain that the visit allows the patient and physician (or care manager) to talk longer than during a typical office visit. |
| Do not try to “sell” the visit. |
| Give the patient a health risk appraisal to bring back; this gives the patient a sense of what to expect. |
| Brainstorm potential solutions to barriers such as transportation, time, and care of other family members. |
| Be knowledgeable, caring, and passionate while not overwhelming the patient. |
In fact, the care manager's AWV caseload increased to the point that other practice nurses, including our three part-time care managers, began performing AWVs also. We did not have to hire additional staff.
According to CMS, many practice staff members can perform AWVs with a supervising physician on site, including nurses, pharmacists, dietitians, health educators, and others. Nurse practitioners and physician assistants can actually bill for the visit although medical students and residents require physician-faculty supervision.
A few practices have reported that some patients consider the dementia screening included in the AWV, which generally takes the form of a memory test, insulting or even stressful. Our care manager explains to the patient that Medicare requires a memory screen and that while the process may seem simplistic, it is a well-supported tool. So far, we have had one complaint of the test being “insulting” and another patient with low health literacy being upset by it.
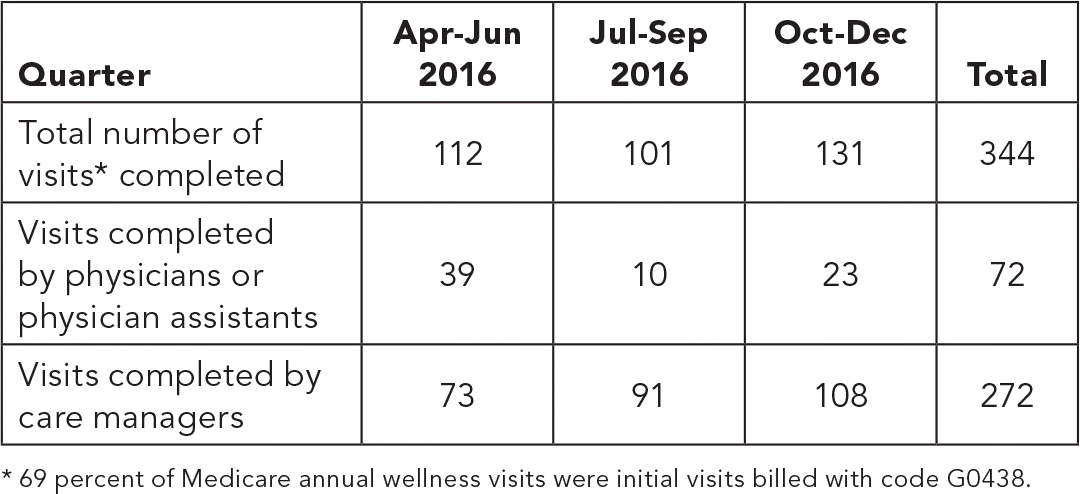
During the nine months we conducted the AWV recruitment project, we completed 344 AWVs at our two practices, compared with 153 AWVs in all of 2015. (See “Medicare annual wellness visit study results.”) Assuming that trend continues, we would complete 458 AWVs during a full year, or a 300 percent annual increase. This would increase the completion rate among our eligible population to 21 percent. Although there is clearly room for further improvement, this percentage approaches the “best” rates reported elsewhere.4
MEDICARE ANNUAL WELLNESS VISIT STUDY RESULTS
| Quarter | Apr–Jun 2016 | Jul–Sep 2016 | Oct–Dec 2016 | Total |
|---|---|---|---|---|
| Total number of visits* completed | 112 | 101 | 131 | 344 |
| Visits completed by physicians or physician assistants | 39 | 10 | 23 | 72 |
| Visits completed by care managers | 73 | 91 | 108 | 272 |
* 69 percent of Medicare annual wellness visits were initial visits billed with code G0438.
The clinical benefits of AWVs are paramount, but we must also consider financial performance. During fiscal year 2015, which ended June 30, 2015, our two practices received $26,720 in reimbursement for AWVs. Our practices factor in a 12 percent “supply cost” to any clinical encounter, reducing the profit to $23,513. During the first nine months of our project, and adjusting for the supply cost, our practices generated $38,357, on track for $51,143 for the full year. That means an annual estimated profit gain of $27,630 over 2015. Note that this figure does not include secondary revenue from immunizations, lab draws, and other billable services related to the AWV.
What we learned
Our quality improvement initiative to expand AWVs followed the “plan-do-study-act” quality improvement model. We started with a literature search that helped us design surveys that identified patient and provider attitudes and perceptions of wellness visits. Then we piloted an intervention linking physician recommendation with the personalized advocacy of our care manager, an informed and engaging champion. We studied the results of this successful pilot and acted further, engaging our staff as advocates, keeping track of eligible patients, reminding providers to suggest an AWV, and using personalized support and encouragement to encourage AWV scheduling and completion.
LEARN MORE ABOUT THE ANNUAL WELLNESS VISIT
“Medicare Annual Wellness Visit: Getting Paid for What We Do Best”
On-demand webinar sponsored by the American Academy of Family Physicians ($30 for members, $69 for non-members)
As a result, our practice culture has changed so that we discuss AWVs more often and make them easier to schedule and complete. This translated to a vastly improved completion rate (increasing from 7.1 percent to 21 percent) among eligible Medicare patients in the first year.
Still, we identified limits to the effectiveness of this initiative:
- We only recruited from patients accessing our practices, and it is likely that people who do not come to the office may be more ill and frail and more in need of AWV assessment and subsequent care. We should direct future recruitment efforts to these patients.
- Our results contain an inherent “response bias” in that patients who respond to surveys may not represent the practice population as a whole.
- A quarter of our patients who scheduled AWV appointments either canceled or did not show up, indicating additional barriers that we have not addressed.
In our model, the care manager assumed a central role not only in recruitment and staff training but also in the completion of AWVs. This has several implications. First, conducting the wellness visits helped the nurse form in-person relationships, especially with more vulnerable patients. As a result, these patients have been far more open to follow-up care management telephone calls. Second, because we let patients know ahead of time that a nurse would perform the AWV and that it did not include a physical exam – although the care manager could call in a physician to assess unanticipated acute concerns such as chest pain or febrile illnesses – we did not observe any resulting patient dissatisfaction, a phenomenon reported elsewhere. Third, revenues generated by the additional AWVs equal about a 0.4 full-time equivalent (FTE), which corresponds fairly well to the time our care manager and other nurses dedicate to AWVs, thereby paying for the effort. Fourth, this model was well received by physicians, almost all of whom appreciated relief from the complexity of the AWV and valued the nurses' perspectives.
We are a small, university-affiliated practice, so it is unknown how well our findings apply to other practice settings. However, we hope our experiences help other practices seeking to encourage wellness visits.

