
Colocating counseling and primary care services can help ensure that patients get the mental health care they need.
Fam Pract Manag. 2017;24(4):11-16
Author disclosures: Jillian Vanselow disclosed that she is the president of the company that Dr. Nelson's practice contracted with to provide the mental health services described in the article. No other relevant financial affiliations disclosed.

An estimated 43.6 million U.S. adults, or 18.1 percent of the adult population, suffer from some form of mental illness, with anxiety and depressive disorders being the two most common. In a given year, an estimated 6.6 percent of adults (15.7 million) have at least one major depressive episode, and 4.3 percent of adults (10.2 million) have a major depressive episode with severe impairment. Unfortunately, less than half of people who experienced a mental illness in the past year received mental health care.1
Primary care physicians are often the first to identify, diagnose, and initiate treatment for mental health conditions. In fact, the two most common diagnoses in our family medicine clinic are anxiety and depression, and the most common type of referral is for mental health counseling. However, we know that despite the physician's recommendation to see a counselor, few patients actually follow through with scheduling an appointment. We asked patients why, and they described multiple barriers, including financial concerns, counselor availability, scheduling conflicts, inconvenient office location, and feelings of shame. It was clear that we needed to bridge this gap between referrals and counseling in order to improve the mental health of our patients.
Thinking differently about access
We (Dr. Nelson's practice) started thinking critically about how our patients accessed counseling services and the barriers they faced. Penchansky and Thomas first argued for a more precise definition of access to health care in the early 1980s.2 Their ideas are making a deserved comeback in the field of behavioral economics, given the inherent complexity of our modern health care system. Access, they argue, is more than just the ability or willingness to enter the health care system. They describe access as a concept of “fit” between the “client,” or patient, and the system. The concept of fit is further subdivided into five specific components:
Availability is about the adequacy of the supply of health care providers and programs.
Accessibility is the relationship between the service and the patient or the patient's transportation resources, including time, distance, or cost.
Accommodation is the patient's ability to adapt to the clinic's resources, such as its appointment system, hours of operation, or phone service.
Affordability is the relationship between prices and the patient's ability to pay, including health insurance, and how the patient perceives worth and value.
Acceptability is how well the patient and the provider can work together.
We used the Penchansky and Thomas framework to consider whether reducing barriers to access would increase patients' willingness to seek treatment for anxiety and depression in primary care. (See “Barriers to access for patients seeking care for anxiety and depression.”)
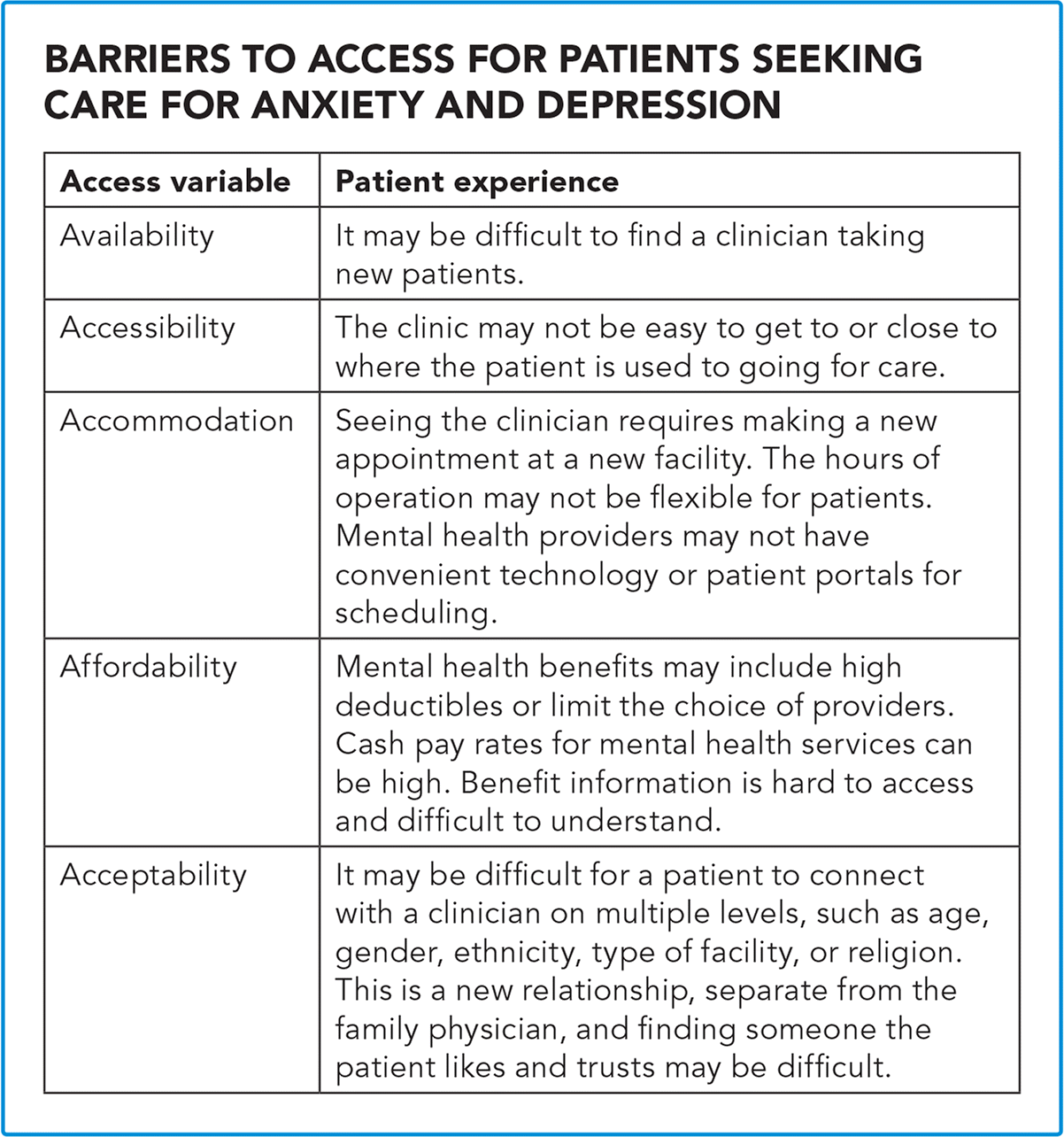
| Access variable | Patient experience |
|---|---|
| Availability | It may be difficult to find a clinician taking new patients. |
| Accessibility | The clinic may not be easy to get to or close to where the patient is used to going for care. |
| Accommodation | Seeing the clinician requires making a new appointment at a new facility. The hours of operation may not be flexible for patients. Mental health providers may not have convenient technology or patient portals for scheduling. |
| Affordability | Mental health benefits may include high deductibles or limit the choice of providers. Cash pay rates for mental health services can be high. Benefit information is hard to access and difficult to understand. |
| Acceptability | It may be difficult for a patient to connect with a clinician on multiple levels, such as age, gender, ethnicity, type of facility, or religion. This is a new relationship, separate from the family physician, and finding someone the patient likes and trusts may be difficult. |
Believing that improving access to care for depression and anxiety and engagement with a plan of care could radically change the course of a person's life, improve multiple health outcomes, save health care resources, and reduce the burden on primary care physicians, our practice decided to explore improving access to mental health care within the family medicine clinic itself.
A collaborative model
Working with a local behavioral health out-patient facility that specializes in providing individualized care for mental health and substance abuse issues, we (Dr. Nelson and Jillian Vanselow) developed a new collaborative model designed to make it easier for patients to schedule mental health services, understand their insurance benefits and coverage, and feel comfortable attending visits.
To ease the scheduling burden on patients, medical assistants at the family medicine clinic use a secure online system to notify the contracted mental health provider of the referral. The provider's scheduler calls the patient within 24 hours of the placed referral to answer questions, review insurance, and set up appointments. If the need for an appointment is urgent, physicians use HIPAA-compliant text messaging to contact the mental health provider directly.
Counseling visits are provided in the family medicine clinic in a comfortable room that is subleased to the contracted mental health provider. The counselor is seen as an extension of the family medicine clinic, and patients retain their privacy, because no one in the waiting room knows which providers the other patients are there to see – characteristics that reduce the stigma associated with seeing a mental health counselor. Providing care within the same office also allows the counselor and physicians to more easily communicate about their mutual patients. Of course the mental health counselors could also see patients in their own offices, for example, if a patient needs more intensive outpatient drug rehab therapy or other higher level care or if a patient prefers to see a counselor in a different location with a different subspecialty.
Several benefits emerged from the model, including the following:
Enhanced physician satisfaction. At the outset, we held quarterly meetings with the practice's physicians to discuss the program and get feedback. They expressed satisfaction with the new model and said they appreciated receiving frequent updates from the counselors on their patients' progress or regression either face-to-face or through secure instant messaging. This was significant as previous communication between physicians and counselors had been practically nonexistent. One physician described how she and the counselor used instant messaging to manage a patient with major depression seen in the outpatient setting on a Friday afternoon. She said that such a team approach was virtually impossible before this collaboration, and without it, “I would have had no choice but to admit that patient to an inpatient facility for treatment.”
Physicians and counselors also said they were encouraged by the progress patients made in counseling as it allowed physicians to spend more time focused on physical concerns rather than the effects of anxiety and depression. For example, before counseling, a 43-year-old patient with asthma was having such severe panic attacks that he went to the emergency room monthly, afraid he was having a heart attack. Following four counseling sessions, his anxiety had reduced to the level that his physician could assess his cardiovascular health and improve his asthma management. The patient has not returned to the emergency room in one year. A 10-year-old patient was referred to a counselor because the trauma she experienced from a choking episode resulted in chronic stomachaches and a refusal to eat anything other than soft foods. After the counselor taught the patient coping skills, which were reinforced with her parents, her abdominal pain disappeared and she returned to eating normally. Together, a physician and counselor helped a 41-year-old male patient cope with diabetes, chronic pain, and major depression while titrating his use of prescription medications, eliminating about half of them. The patient reports a decreased use of emergency room services and increased quality of life.
These success stories fueled our physicians' satisfaction with the program. They also perceived a decline in patients skipping their counseling appointments, which they attributed at least partly to reducing the stigma for patients of receiving services at a behavioral health facility.
Improved clinical outcomes. The Patient Health Questionnaire-9 (PHQ-9) and the Hospital Anxiety and Depression Scale (HADS) are standardized tools widely used in both inpatient and outpatient settings to diagnose and measure severity of depression and anxiety. (See “PHQ-9 and HADS tools.”)3,4 Using these tools, along with software we had already purchased and workflows we had already established for patient history-taking, we assessed patients for relevant diagnoses each time they visited the practice, regardless of the reason for the visit. We analyzed the results of these assessments by creating change scores (most recent score minus the first score for each of the tests), and our statistical analysis showed significant improvement over time. We believe that these results are encouraging and suggest that counseling may affect and improve scores on standardized assessments of anxiety and depression.
Low-cost approach. The collaboration created cost benefits for patients, the family medicine practice, and the contracted mental health provider. Patients saved money on additional travel costs as a result of the counseling services being colocated in the family medicine practice. They also avoided costly and frustrating “insurance surprises” because the cost of treatment was estimated and discussed up front. Patients were able to use their mental health benefits, employee assistance programs, or cash, based on individual financial resources. This attention to detail was made possible in part because the mental health provider contracted with a specific billing service that specialized in mental health services. After the counselor performed an intake visit and made a diagnosis, a care manager provided an intake assessment to the billing company, which worked diligently to receive preauthorization for individual counseling sessions. If more sessions were necessary, the case manager provided a utilization review and requested additional sessions. Patients preferred in-network benefits because they only had a copay for the service. Patients also could choose from a menu of creative payment options, including group-based therapy offered at a lower cost point or customized treatment schedules with “homework” that resulted in fewer sessions and lower costs.
For the family medicine practice, offering the services was cost-neutral. A fair market rent and management fee covered administrative costs related to the counseling rooms and staffing. The contracted mental health provider covered the cost of its professional staff, administration, billing, the electronic health record (EHR), and materials.
The main cost benefit to the mental health provider was pilot testing an innovative model for providing mental health care inside a primary care practice. This allowed the provider to test and refine processes related to the coordination of care, counselor staffing, referrals, and billing, as well as rapid cycle quality improvement processes with collaborating physicians. In addition, because the provider had already invested in customized technology and efficient billing practices, the administration costs of providing the care were low.
PHQ-9 AND HADS TOOLS
The Patient Health Questionnaire (PHQ-9) asks patients nine questions to gauge the recent severity of mental health issues (e.g., “feeling down, depressed, or hopeless”). Patients answer using a four-point scale, ranging from “not at all” to “nearly every day.” For patients who acknowledge problems, the tool also asks them to rate their ability to get along with others because of the problem. The PHQ-9 is designed to reveal minimal, mild, moderate, moderately severe, or severe depression. The PHQ-9 is available here: http://bit.ly/2ePQ4FO.
The Hospital Anxiety and Depression Scale (HADS) was developed primarily to quickly screen for anxiety and depression in inpatient settings. It includes 14 questions to answer on a four-point scale. Half of the questions provide a depression score (HADS-D) while the other questions offer an anxiety score (HADS-A). The HADS is available here: http://www.bgs.org.uk/pdfs/assessment/hads_mood.pdf.
Maximizing use. One of the main problems with offering mental health care has been patient reluctance to obtain counseling. Research suggests that fewer than 10 percent of patients referred to mental health care services actually complete the referral and seek care.5 In our case, a review of electronic orders and visit encounters during the study period suggests that 43 percent of patients referred to the contracted mental health provider by their physician attended at least one session (with an average of six visits). We believe this dramatic rise in referral rates was made possible by removing the barriers patients experienced in accessing counseling. Furthermore, regression analysis suggests that it took only five visits to see a clinically significant improvement in the PHQ-9 and HADS scores with a 95 percent confidence interval.
Lowering the barriers
In summary, we believe that adding mental health care services to the existing primary care practice gave patients with anxiety or depression improved access to care by removing many of the most significant barriers and creating a better “fit.”
Availability: The contracted mental health provider's proactive and timely outreach to patients when initiated by a physician's referral was a key improvement over the more typical process of encouraging the patient to find a suitable counselor, which could take weeks and involve multiple false starts.
Accessibility: Colocating the contracted mental health counselor in the family medicine clinic helped patients who were already familiar with the location.
Accommodation: Mental health services were offered at an existing service site where the patient could expect the same positive experience they had received previously (kind and friendly staff, the ability to schedule appointments, pay bills, and retrieve documentation through the online portal, same-day scheduling, short wait times, etc.).
Affordability: The contracted mental health provider's financial policies and willingness to investigate patient insurance plans and obtain prior authorization eliminated much of the financial guesswork for patients.
Acceptability: The process attempted to reduce the stigma of seeking mental health services and provided a warm hand-off from physician to counselor. In addition, patients were familiar with the environment and staff, and had multiple counselors to choose from.
Reducing these barriers improved patient engagement in therapy, decreased no-show rates, and demonstrated improvement on standardized measures for anxiety and depression.
Obviously, this model has its limits. Our program focused on patients belonging to a single primary care practice serving a predominately non-Hispanic, white, middle-class population. Other practices, particularly those serving patient populations that are significantly different in terms of race, ethnicity, income, or education, could encounter additional barriers, some of which could be community-specific. This could require applying the access framework differently.
Also, we collected data on counseling visits, primary care visits, and PHQ-9/HADS scores as they happened naturally, which was sporadic and at unplanned intervals. This means we were statistically unable to control for a variety of confounding variables, and our sample size was small.
Finally, this model is only as good as the contracted mental health provider with which your practice collaborates. We have provided some recommendations in “Finding the right mental health care partner.”
FINDING THE RIGHT MENTAL HEALTH CARE PARTNER
The following are key traits of a contracted provider that can help your practice improve patient access to mental health care:
Can handle increasing volume, as opposed to a scheduling backlog that would prevent the seamless flow of referrals from your practice.
Uses HIPAA-compliant communication technology such as secure texting to enhance communication with your practice.
Is well-versed in mental health care billing practices, is flexible, and can offer low-cost options to patients.
Is interested in being a true partner by being willing to accept feedback, offer solutions to problems, and grow alongside your practice.
Has a relationship with a licensed outpatient facility to refer patients to when higher levels of care are needed.
Is willing to colocate but remain a separate business entity. This takes the burden off your practice to hire, fire, and otherwise manage behavioral health professionals.
It is our hope that others will seek to replicate the program, reducing barriers and improving much needed access to mental health counseling. This has profound implications for a health care system that has been described as fragmented, forcing patients, families, and caregivers to “navigate an increasingly complex system filled with inefficiencies,” leading to higher costs, “serious complications, including medication errors, preventable hospital readmissions, and unnecessary pain and suffering.”6 Reducing the complexity patients face in obtaining care, through attention to the multiple components of access, will help enhance engagement with a variety of treatment plans.
