So you want to incorporate refugee health into your practice. Now what?
Related article from American Family Physician: "Primary Care for Refugees: Challenges and Opportunities."

The number of people displaced from their homes due to violence or the threat of violence reached more than 65 million in 2015, the highest number in recorded history.1 Of these, some 20 million can be classified as refugees – men, women, and children forced to flee their home countries due to fear of persecution based on their race, religion, nationality, political opinion, or membership in a social group. The United States has resettled approximately 3 million refugees since 1975 and admitted almost 85,000 in 2016,2 although the number for 2017 is likely to be much lower.
Refugees represent a very heterogeneous group, and yet many face similar health challenges, including lack of prior access to medical care, exposure to trauma and violence, poverty, and limited or interrupted formal education. Upon arrival, refugees may experience challenges accessing appropriate services due to language and cultural barriers and acculturation difficulties. Traditionally, health departments and community health centers have provided much of refugee health care. However, academic health centers and community-based physicians play an increasingly important role in caring for refugees.
Family physicians often already work with multicultural, underserved, and vulnerable patient populations across the United States. With our wide scope of practice, community orientation, emphasis on prevention, and ability to manage chronic diseases, family physicians are well positioned to offer essential services for refugees and respond to their ongoing physical, psychological, behavioral, and social needs.
That said, many clinicians might find the idea of caring for refugees daunting. In this article we'll address some of these concerns as we review important practice management issues related to caring for refugee populations. Having worked with refugees in a variety of settings, we'll also share some pitfalls and best practices for integrating refugee health into our own clinical and educational sites.
The resettlement process
The refugee resettlement process3 is lengthy and involved. Understanding this process and some of the obstacles refugees face can provide helpful context when caring for them.
Overseas. After fleeing their home countries, refugees undergo intensive screening and evaluation by the United Nations High Commissioner for Refugees (UNHCR). Those deemed candidates for resettlement in the United States then undergo an 18-month to 24-month rigorous vetting process by the U.S. government, including interviews with the Department of Defense, Homeland Security, and other federal agencies.
If selected for resettlement, each applicant must also undergo a predeparture medical evaluation conducted according to Centers for Disease Control and Prevention (CDC) guidelines4 by an approved physician. This examination ensures refugees do not have any conditions that could be dangerous to them or others while traveling and includes a full medical and psychological evaluation as well as screening for tuberculosis, sexually transmitted infections, and presumptive treatment for malaria and intestinal parasites.
Arrival. Once approved, refugees are matched with a U.S.-based resettlement agency, or Volag (“Voluntary Agency”), tasked with coordinating placement in the United States according to housing availability, host community readiness, required services, and employment needs. (For a listing of U.S. resettlement agencies, see http://www.wrapsnet.org/rp-agency-contacts/.) Upon arrival, Volags help arrange housing and other services for refugees. Refugees also receive assistance applying for a Social Security number, enrolling their children in school, undergoing an initial domestic medical examination, undergoing English language training, and seeking employment services. These steps must be completed within the first 30 to 90 days after arrival.
Government cash assistance and refugee medical assistance are usually discontinued after eight months because refugees are expected to be self-sufficient by that time. Minors are eligible for the Children's Health Insurance Program and Medicaid upon arrival, but after this eight-month time period, adult refugees must find their own source of health insurance, either through an employer or marketplace insurance program, similar to other legal residents of the United States.
Domestic examination. Refugees undergo a domestic medical screening examination, or “entrance exam,” preferably within 30 days of arrival. This initial health assessment is based on CDC guidelines and is overseen by state and local health departments. The assessment focuses on detecting communicable diseases that could pose public health concern and may consist of limited additional health screening. Individual physicians and practices can conduct this exam if coordinated with the state's Refugee Health Coordinator, and it is moderately reimbursable if performed within 90 days of arrival.
Six ways to care for refugees
Family physicians may interact with refugees in a variety of capacities and settings, each with its own unique challenges (see “Refugee health checklist”).
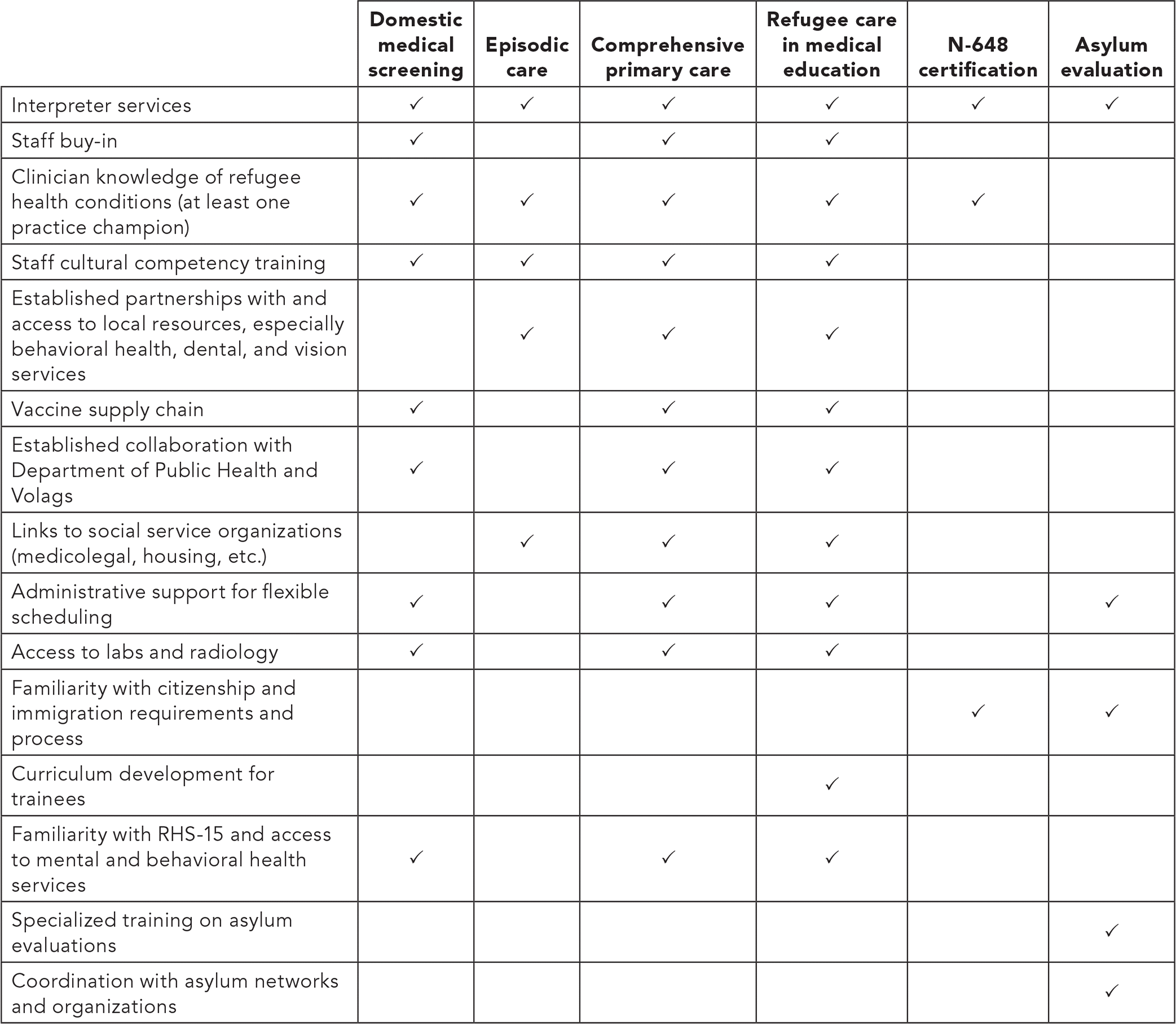
REFUGEE HEALTH CHECKLIST
This checklist summarizes the components practices should have in place when caring for refugees, depending on the type of refugee health care being provided.
| Domestic medical screening | Episodic care | Comprehensive primary care | Refugee care in medical education | N-648 certification | Asylum evaluation | |
|---|---|---|---|---|---|---|
| Interpreter services | ✓ | ✓ | ✓ | ✓ | ✓ | ✓ |
| Staff buy-in | ✓ | ✓ | ✓ | |||
| Clinician knowledge of refugee health conditions (at least one practice champion) | ✓ | ✓ | ✓ | ✓ | ✓ | |
| Staff cultural competency training | ✓ | ✓ | ✓ | ✓ | ||
| Established partnerships with and access to local resources, especially behavioral health, dental, and vision services | ✓ | ✓ | ✓ | |||
| Vaccine supply chain | ✓ | ✓ | ✓ | |||
| Established collaboration with Department of Public Health and Volags | ✓ | ✓ | ✓ | |||
| Links to social service organizations (medicolegal, housing, etc.) | ✓ | ✓ | ✓ | |||
| Administrative support for flexible scheduling | ✓ | ✓ | ✓ | ✓ | ||
| Access to labs and radiology | ✓ | ✓ | ✓ | |||
| Familiarity with citizenship and immigration requirements and process | ✓ | ✓ | ||||
| Curriculum development for trainees | ✓ | |||||
| Familiarity with RHS-15 and access to mental and behavioral health services | ✓ | ✓ | ✓ | |||
| Specialized training on asylum evaluations | ✓ | |||||
| Coordination with asylum networks and organizations | ✓ |
Domestic medical screening. As described above, all refugees are expected to have a full screening exam upon arrival. Family physicians can coordinate with local/state health departments if interested in conducting these screenings. The evaluations are typically guided by state Department of Public Health protocols and CDC guidelines4 and focus on infectious disease screening, vaccinations, and U.S. health system orientation. (A list of the CDC recommendations is available in the related article “Primary Care for Refugees: Challenges and Opportunities,” American Family Physician, July 15, 2017.) Upon completion of the exam, refugees should be referred to local primary care providers.
Another important component of the domestic screening exam is a brief mental health assessment, recommended where community mental health referral resources are available. Although most physicians are familiar with the Patient Health Questionnaire-9, they may not be familiar with the Pathways to Health Refugee Health Screener-15 (RHS-15), a 15-question screening tool validated in refugee populations and multiple languages to identify post-traumatic stress disorder as well as depression, anxiety, and adjustment disorders. Many states have adopted RHS-15 as the preferred mental health screening tool.
Episodic care. Family physicians may encounter refugees anywhere across the continuum of care. The provision of ad-hoc care (defined as not being part of a dedicated refugee health program) may not differ much from working with other underserved populations, although awareness of the unique characteristics and health status of refugees is important. Some of these characteristics include increased incidence of emotional and physical trauma, undiagnosed and untreated chronic medical conditions, lack of preventive health screenings (e.g., Pap smears and lipid screening for those at risk), potential family dysfunction due to social disruption, and difficulty navigating the health system, which can affect the ability to coordinate referrals or advocate for self or family.
Comprehensive primary care. Family physicians working in federally qualified health centers, county systems, academic settings, or other sites offering services to underserved populations could consider becoming comprehensive primary care providers for refugee populations. Effectively and efficiently delivering comprehensive primary care to refugees requires coordination and partnership with multiple community-based organizations, including local Volags and health departments.
In settings with a broad scope of practice, family physicians have the unique opportunity to care for entire refugee families. In our experience, refugees tend to come from cultures that are community and family centric, so understanding the family dynamics can provide insight and reveal barriers to care. Further, seeing an entire family at one visit cuts down on transportation costs, fragmentation of care, and no-shows.
Because refugees' health care needs can be extensive, reimbursement for these initial visits is often higher than established primary care visits. Doing this initial work, though difficult, may allow for additional funding to help support staff and other services. Staff training in cultural humility(i.e., a willingness to explore your own biases and respect other cultures) is essential, as is scheduling flexibility. Due to language and other cultural barriers, newly resettled refugees may have difficulty understanding the patient appointment process and arrive late. In one of our refugee clinics, we solved this problem by assigning a single front-office staff member to coordinate patient visits with our local Volags. Having this dedicated point person can relieve other staff of these duties and help “sell” them on the idea of working with refugees. Although this requires an investment of staff and time, the intervention can pay off by reducing no-show rates and increasing revenue in value-based health systems.
Refugee care in medical education. Linking refugee health with medical education serves dual purposes – service to the community while teaching medical students and residents to care for underserved and vulnerable populations. One benefit of this model is that educational centers are sometimes less dependent on clinical productivity measures than private practices, meaning faculty physicians can dedicate more time to working with patients while teaching learners.
Working with refugees within a residency or medical education program also fulfills Accreditation Council for Graduate Medical Education competencies. Learners develop competency in direct patient care by engaging patients with undifferentiated complaints and broadening their differential diagnoses to include imported infectious diseases. Additional skills include cross-cultural communication, working with medical interpreters, examining the role of social determinants of health, global health, and behavioral health integration. Students can even engage as community liaisons and health system navigators.5,6,7
N-648 certification. Even if physicians cannot engage directly with refugees in a clinical capacity, they can still offer their services in another way, through completion of an N-648 form for medical certification for disability exceptions. After five years, refugees are eligible to undergo a naturalization process and seek citizenship in the United States. Part of this process involves a civics examination in English. Many refugees learn English as part of their acculturation process. The N-648 form is used to establish when this is not possible due to a disability or other health barriers such as dementia, congenital or acquired cognitive delays, or other physical or psychological ailments. Any physician with a medical license can complete the N-648 form, even if they are not the patient's primary physician. The service is usually provided on a cash basis.
Asylum evaluation. Some people fleeing violence arrive in the United States without having gone through refugee processing and, therefore, have no formal refugee resettlement status or support. If these persons are unable to return to their native country for fear of persecution, they can file for political asylum in the United States. While not mandated, most immigration attorneys encourage clients filing for asylum to undergo a medical examination to document any physical evidence or sequelae of torture or ill-treatment, which can bolster the asylum claim. Of those asylum seekers who undergo medical examination, roughly 90 percent are granted asylum, compared with 37.5 percent among those who do not receive forensic medical evaluations.8 Beyond meeting the need for trained evaluators in the United States, participating in asylum evaluation programs can provide clinicians with professional and personal rewards.9
Challenges and tips
Despite the myriad ways for family physicians to become involved in refugee care, making this a reality can still be daunting. Some of the beginner mistakes we made included not dedicating enough time to preparing for the visits themselves, underestimating the skills required to work effectively with interpreters, not developing staff buy-in, and either trying to learn every single nuance particular to a certain population or completely ignoring the cultural aspect of refugee care.
Other common challenges to refugee care include the following:
- Clinical burden. Prior to their arrival in the United States, refugees often have had little to no prior medical care, and some of them may have “exotic” or unfamiliar infectious diseases. This can result in pressing health-related issues, which may be difficult to address in the standard 15-minute office visit. Scheduling frequent and regular follow-up visits can increase the therapeutic alliance and ensure thoroughness of care.
- Economic and social needs. Refugees' needs often include housing assistance, employment, insurance, and other social concerns that most practices aren't equipped to handle. Creating connections with community-based resources such as Volags, social services, and volunteer groups interested in supporting care for refugees will help foster trust between refugee patients and clinicians and may positively affect health outcomes.
- Clinic location. Private and academic clinics are often located near urban medical centers or hospital systems, not where refugees live. Transportation is consistently named one of the highest barriers to accessing care for this population. Practices should be aware of this issue and understand that it can contribute to no-shows and late arrivals.
- Financial aspects of refugee care. Familiarizing yourself with payment mechanisms for initial exams and common ICD-10 bill-able codes for continuing care are important not only in getting paid for this work but also in “marketing” refugee health to administrators or larger health systems. (See “ICD-10 codes commonly used with refugee populations.”)
ICD-10 CODES COMMONLY USED WITH REFUGEE POPULATIONS
General encounters:
- Encounter for other special examination without complaint, suspected or reported diagnosis Z01*
- Encounter for examination for administrative purposes, unspecified Z02.9
- Encounter for screening for infectious and parasitic diseases, unspecified Z11.9
- Health exam of a defined subpopulation Z01.89
- Acculturation difficulty (e.g., language barrier or cultural differences) Z60.3
- Encounter for other administrative examinations (e.g., immigration or naturalization examination) Z02.89
General findings:
- Pain, unspecified (e.g., body aches) R52
- Decreased vision, both eyes H54.2
- Screening examination for infectious and parasitic diseases Z11*
- Encounter for screening for intestinal infectious diseases Z11.0
- Encounter for screening for respiratory tuberculosis Z11.1
- Encounter for screening for other bacterial diseases Z11.2
- Encounter for screening for other protozoal diseases and helminthiases Z11.6
- Encounter for screening for other infectious and parasitic diseases Z11.8
- Encounter for screening for infectious and parasitic diseases, unspecified Z11.9
- Problems related to housing and economic circumstances, unspecified (e.g., economic circumstances, financial problems, or housing circumstance affecting care) Z59.9
- Female genital mutilation (FGM) status, unspecified N90.810
- FGM type I status N90.811
- FGM type II status N90.812
- FGM type III status N90.813
- FGM other status N90.818
Psychiatric issues:
- Problems related to certain psychosocial circumstances: exposure to disaster, war, and other hostilities Z65.5
- Reaction to severe stress, and adjustment disorders F43*
- Acute stress reaction F43.0
- Post-traumatic stress disorder F43.1
- Post-traumatic stress disorder, unspecified F43.10
- Post-traumatic stress disorder, acute F43.11
- Post-traumatic stress disorder, chronic F43.12
- Adjustment disorders F43.2*
- Adjustment disorder, unspecified F43.20
- Adjustment disorder with depressed mood F43.21
- Adjustment disorder with anxiety F43.22
- Adjustment disorder with mixed anxiety and depressed mood F43.23
- Other reactions to severe stress F43.8
- Reaction to severe stress, unspecified F43.9
Pediatric concerns:
- Routine child health examination without abnormal findings (e.g., first visit with new immigrant child) Z00.129
- Encounter for screening for infectious and parasitic diseases, unspecified Z11.9
- Acculturation difficulty (e.g., language barrier or cultural differences) Z60.3
- Delayed immunization Z28.3
- Immunization (e.g., influenza vaccine administered) Z23
- Adjustment disorder, unspecififed F43.20
- Anemia, unspecified D64.9
- Dental caries, unspecified K02.9
- Dental neglect K08.89
- Eosinophilia D72.1
- Latent tuberculosis R76.11
- Application of prophylactic fluoride varnish by a physician Z41.8
- Problems related to frightening experiences Z62.898
* Non-billable/non-specific code; select a code underneath it that describes the diagnosis with a greater level of detail.
To combat these challenges and most effectively care for this population, practices should consider developing the following resources:
- At least one clinician champion who has demonstrated skills and experience in cross-cultural care; knowledge of common refugee health conditions, risks, stressors, and barriers to care; and demonstrated experience working with interpreters,
- A welcoming physical environment with posters, artwork, and signs in multiple languages and depicting a variety of cultures,
- Referral information for torture and trauma counseling,
- Multilingual health information and other practice information available at the reception desk,
- Multilingual front-office staff or translation services,
- Multilingual voice messages,
- Experienced case workers,
- An interest in refugee health displayed clearly on the practice website and marketing materials,
- Electronic health record (EHR) prompts for refugee status, place of birth, year of arrival, and health assessment, as well as EHR support for the RHS-15,
- A process for accessing refugee exam results from the department of health, UNHCR, etc.
- Ability to schedule and offer longer appointments as necessary.
An ideal partnership
Family physicians are ideally trained and positioned to be involved in the care of refugees and asylum seekers. Although there may be challenges in incorporating care for these vulnerable populations into a busy practice, various models and resources are available to facilitate building capacity in a sustainable, coordinated, consistent, and responsive manner. Caring for refugee patients can be rewarding for both family physicians and their staff and can build deeper connections in the community.
In this time of increasing physician burn-out, we've found working with refugees has reinvigorated our clinical practice. Whether it's receiving a heartfelt expression of gratitude from a Congolese man who has never received actual medical care, holding the hand of a Burmese Rohingya woman in tears because no one had ever taken time to hear her story of fleeing violence, or providing medical care to a Syrian family grateful to have a safe place to sleep, we have reaped numerous rewards from working with refugees. Hearing our patients' stories, learning from their resilience, and helping people rebuild their lives has reintroduced a humility and joy too often missing from the clinical practice of medicine. We hope other physicians are inspired and prepared to begin caring for this population.
ADDITIONAL RESOURCES
These country-specific profiles include specific interventions for specific groups being resettled in the United States. Each profile consists of six components: priority health conditions, background, population movements, healthcare and nutrition in camps/urban settings, medical screening of U.S.-bound refugees, and general health information.
EthnoMed offers information about cultural beliefs, medical issues, and other topics relevant to the health care of U.S. immigrants, including refugees fleeing war-torn parts of the world.
Evidence-Based Preventative Care Checklist for New Immigrants and Refugees
This eLearning knowledge translation tool was designed for primary care physicians to help integrate the Canadian Immigrant Health Guidelines into practice.
Office of Refugee Resettlement
This website offers general information about refugee health.
For more resources, see the related article “Primary Care for Refugees: Challenges and Opportunities,” American Family Physician, July 15, 2017.

