
Here's how to select the measures that will maximize your success under Medicare's new Quality Payment Program.
Fam Pract Manag. 2017;24(4):5-10
Author disclosure: no relevant financial affiliations disclosed.
Family physicians in 2017 are in the first performance year of the Merit-based Incentive Payment System (MIPS), part of a new performance-based reimbursement program that will affect how much they are paid through Medicare in 2019 and beyond.
MIPS is one of two payment tracks under the Quality Payment Program (QPP), which was established when the Medicare Access and CHIP Reauthorization Act (MACRA) ended the sustainable growth rate formula of determining physician payment under Medicare.
By default, physicians will participate in the MIPS track unless they choose and qualify to participate in the second payment track as an Advanced Alternative Payment Model (APM) or meet several criteria for exclusion from the QPP, such as enrolling in Medicare for the first time this year, billing $30,000 or less per year in Medicare Part B charges, or seeing 100 or fewer Medicare Part B patients per year.
The 2017 reporting period for MIPS ends Dec. 31. The Centers for Medicare & Medicaid Services (CMS) will not require physicians to report a full year's worth of data in 2017, but they must submit some data to avoid a negative payment adjustment. Physicians should use this transition year to prepare for full participation.
MIPS adjusts physicians' Medicare Part B professional fee-for-service payments upward or downward based on how they perform in four categories: quality, cost, improvement activities, and advancing care information. Each category is scored separately, has its own measures and requirements, and is weighted for its contribution to the final score, with quality having the greatest weight at 60 percent. (See “2017 MIPS performance category breakdown.”)
2017 MIPS PERFORMANCE CATEGORY BREAKDOWN
Quality: 60 percent
Cost: 0 percent *
Improvement activities: 15 percent
Advancing care information: 25 percent
*Although the Centers for Medicare & Medicaid Services will provide feedback on how physicians perform in the cost category based on claims data, it will not affect your MIPS score in 2017. This will change in the future.
The quality category, in general, requires physicians or physician groups to report data for at least six quality measures, including one outcomes measure, if reporting using claims, registries, or an electronic health record (EHR). Note that physicians can report much less for 2017 depending on how aggressively they plan to comply with MIPS in the first year. Groups that report using a web interface (a secure Internet-based data submission option for groups of 25 or more eligible clinicians) must report data for 15 measures for the full 12 months of 2017. Groups may contract with a survey vendor to report Consumer Assessment of Healthcare Providers and Systems (CAHPS) in place of one quality measure. Groups with at least 16 clinicians and at least 200 cases will also have a readmission population measure calculated for them. (See “Maximum possible points in quality category.”)
MAXIMUM POSSIBLE POINTS IN QUALITY CATEGORY
Reporting with claims, registry, Qualified Clinical Data Registry, or EHR:
70 points: Six quality measures and one readmission measure (if applicable)
60 points: Six quality measures (if no readmission measure applies)
Reporting with CMS web interface:
120 points: Reporting all 15 measures and one readmission measure (if applicable)
110 points: Reporting all 15 measures (if no readmission measure applies)
Many quality measures apply to family medicine, so finding six to focus on should not be hard. But choose carefully. Your performance on these measures will affect your quality score, which in turn will affect your final score and your payments. This article examines several factors to consider when selecting which quality measures to report on, including how CMS uses benchmarks and decile scoring, the effects of “topped out” measures, criteria for reliable scoring, and how to earn bonus points.
Benchmarks and decile scoring
It is logical to think that you should focus on quality measures where your performance is best. However, this is not necessarily the case because your quality score is actually determined relative to a benchmark.
CMS has calculated a benchmark for each quality measure and submission method. These are based on actual performance values reported by physicians during the two years prior to the performance period or, if that data is unavailable, during the performance period itself. Performance rates are broken down into deciles, and points are assigned based on where your performance falls relative to each benchmark.
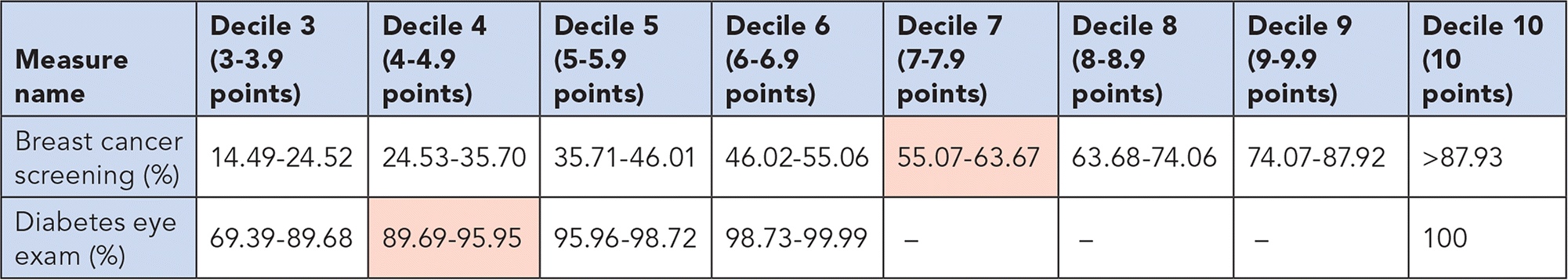
For example, assume that your performance is 60 percent for breast cancer screening and 90 percent for diabetes eye exam. (See “Example of decile benchmarks for registry reporting.”) Although your breast cancer screening performance was lower, you would receive more points for this measure (7-7.9 points) than for the diabetes eye exam measure (4-4.9 points) because your breast cancer screening rate falls into a higher decile relative to other physicians.
Spreadsheets of quality benchmarks for claims, registries, and EHRs for 2017 can be downloaded from CMS. Benchmarks for web interface submissions also are available.
Because this is a transition year, CMS has determined the lowest score for a specific quality measure will be three out of 10 points, even if performance in that measure is 0 percent.
Learn about these benchmarks to better understand how your performance on specific measures will affect your MIPS quality score and choose accordingly.
EXAMPLE OF DECILE BENCHMARKS FOR REGISTRY REPORTING
In this example, even though a physician's performance of 90 percent on diabetes eye exams is higher than his 60 percent on breast cancer screening, the physician would receive more points for breast cancer screening because his performance rate falls in a higher decile.
| Measure name | Decile 3 (3-3.9 points) | Decile 4 (4-4.9 points) | Decile 5 (5-5.9 points) | Decile 6 (6-6.9 points) | Decile 7 (7-7.9 points) | Decile 8 (8-8.9 points) | Decile 9 (9-9.9 points) | Decile 10 (10 points) |
| Breast cancer screening (%) | 14.49-24.52 | 24.53-35.70 | 35.71-46.01 | 46.02-55.06 | 55.07-63.67 | 63.68-74.06 | 74.07-87.92 | >87.93 |
| Diabetes eye exam (%) | 69.39-89.68 | 89.69-95.95 | 95.96-98.72 | 98.73-99.99 | – | – | – | 100 |
Topped out measures
For some quality measures, physicians' performance levels are so high and unvarying that CMS may determine that meaningful distinctions and improvement in performance can no longer be made. CMS will review the measures each year to identify which ones are less desirable for quality reporting and label them as “topped out.” Half of the current QPP quality measures are topped out, with several having a median score of 100 percent. If you decide to report a topped out measure, it is likely you will need a very high performance rate to score in the top decile and maximize your points. (See “Topped out 2017 MIPS measures for family medicine.”)
CMS is considering several ways to discourage physicians from reporting on topped out measures, such as removing them from the list of MIPS quality measures, awarding fewer points for them, or limiting the number of topped out measures that physicians can report on. The agency will also consider whether removing the topped out measures may decrease overall performance rates.
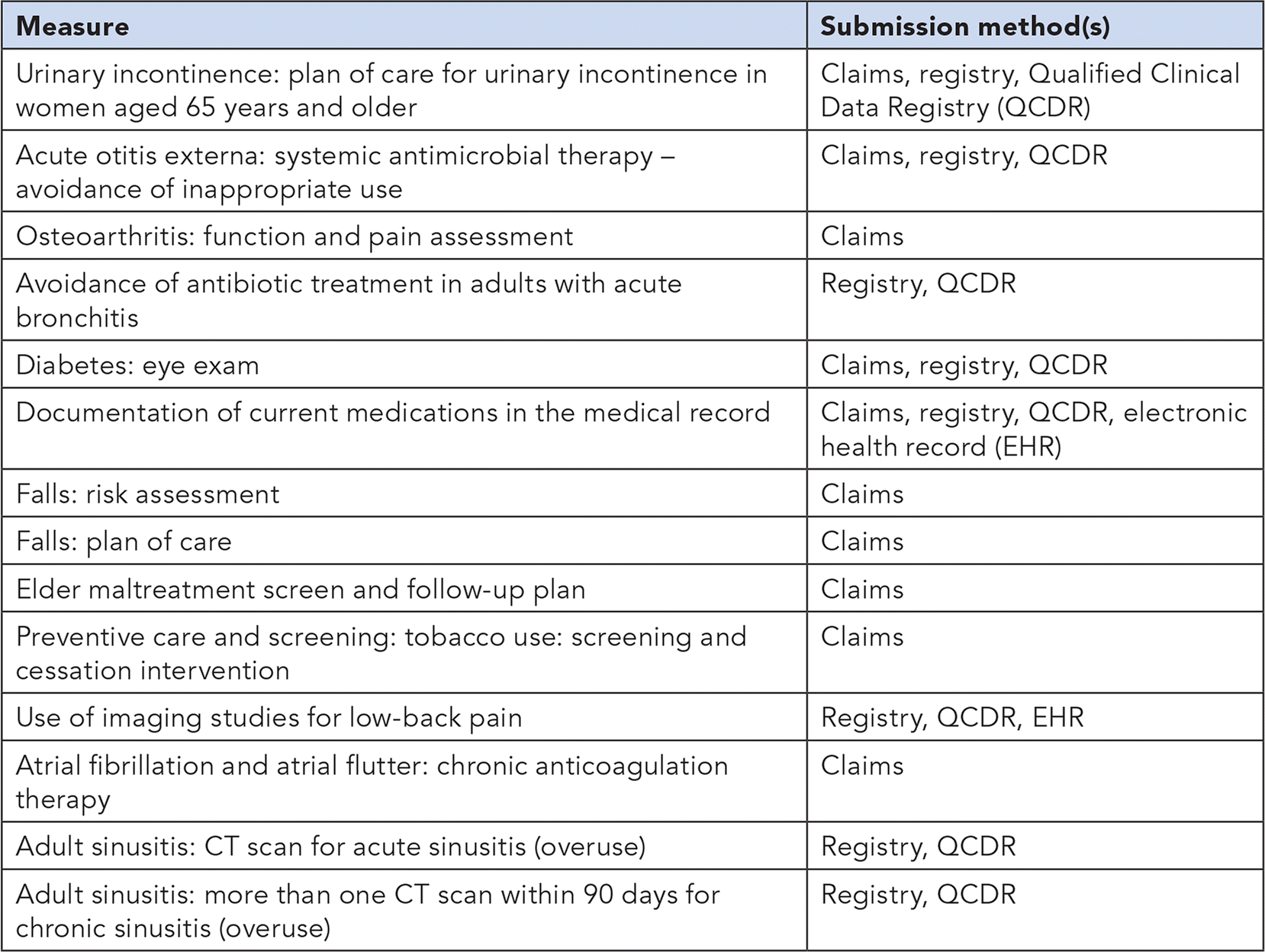
TOPPED OUT 2017 MIPS MEASURES FOR FAMILY MEDICINE
The following quality measures are considered “topped out” for certain data submission methods, meaning there may be limits on how they are scored in future years.
| Measure | Submission method(s) |
|---|---|
| Urinary incontinence: plan of care for urinary incontinence in women aged 65 years and older | Claims, registry, Qualified Clinical Data Registry (QCDR) |
| Acute otitis externa: systemic antimicrobial therapy – avoidance of inappropriate use | Claims, registry, QCDR |
| Osteoarthritis: function and pain assessment | Claims |
| Avoidance of antibiotic treatment in adults with acute bronchitis | Registry, QCDR |
| Diabetes: eye exam | Claims, registry, QCDR |
| Documentation of current medications in the medical record | Claims, registry, QCDR, electronic health record (EHR) |
| Falls: risk assessment | Claims |
| Falls: plan of care | Claims |
| Elder maltreatment screen and follow-up plan | Claims |
| Preventive care and screening: tobacco use: screening and cessation intervention | Claims |
| Use of imaging studies for low-back pain | Registry, QCDR, EHR |
| Atrial fibrillation and atrial flutter: chronic anticoagulation therapy | Claims |
| Adult sinusitis: CT scan for acute sinusitis (overuse) | Registry, QCDR |
| Adult sinusitis: more than one CT scan within 90 days for chronic sinusitis (overuse) | Registry, QCDR |
Scoring requirements
It is important to submit performance data that can be reliably scored. CMS requires that three criteria be met:
Be compared to a national benchmark. You can determine which measures have a benchmark by reviewing the CMS downloadable tables referenced earlier. For CMS to calculate a measure's national benchmark, at least 20 entities must report the measure for at least 20 cases each and meet the data completeness standard, which is explained later.
Include data for at least 20 cases. Physicians who start earlier in the performance period will have an easier time meeting the case minimum.
Meet the data completeness standard. This depends on the method of reporting. (See “MIPS data completeness standards for 2017.”) Submissions involving Qualified Clinical Data Reporting (QCDR), qualified registries, or EHRs in 2017 must report on 50 percent of all patients, regardless of payer, seen over a 90-day period. Submissions involving claims, on the other hand, must report on 50 percent of Medicare Part B patients for at least 90 days. Submissions involving web interface or CAHPS must report on a CMS-generated sample of Medicare Part B patients.
Quality measure data that meet these three criteria will be scored based on performance and receive up to 10 points. Submissions that fail to meet one or more of the criteria will still receive three points in 2017. (Note: Measures submitted through the web interface are an exception; measures that lack data completeness will receive a score of 0 while measures that do not meet the case minimum or have a benchmark will not be scored.)
In future years, CMS will revisit whether to award three points – or fewer – for submissions that do not meet these three criteria.

| Reporting method | Data completeness |
|---|---|
| Claims | 50 percent of Medicare Part B patients for the performance period (at least 90 days) |
| Qualified Clinical Data Registry, registry, electronic health record | 50 percent of patients across all payers for the performance period (at least 90 days) |
| Web interface | Sampling requirements for Medicare Part B patients |
| CAHPS for MIPS survey | Sampling requirements for Medicare Part B patients (Note: CAHPS can count as a quality measure for any MIPS reporting method.) |
Bonus points
If you report on certain high-priority measures or use end-to-end electronic reporting techniques, you can receive bonus points. In fact, you can potentially increase your quality score by up to 20 percent, which would help offset lower performance scores.
Data submitted for these measures must meet the 20-case minimum and data completeness requirements detailed earlier, and you must have a performance rate greater than 0 percent. Also, bonus points may be earned even if a measure is topped out or not scored.
High-priority measures. MIPS awards bonus points for reporting on measures involving outcomes, appropriate use, patient safety, efficiency, patient experience, and care coordination. Physicians and physician groups already must report on one outcome measure as part of the six required quality measures. For each additional outcome measure you report on, you receive two bonus points. You also receive two bonus points for reporting on patient experience measures. The other high priority measures earn one bonus point apiece.
Twenty-five measures from the family medicine specialty set are eligible for high-priority bonus points. You can identify them by using the search option on the CMS QPP website and filtering for general practice/family medicine and high priority measures.
End-to-end electronic reporting. To qualify for this bonus, a registry, QCDR, or EHR must obtain your data from Certified Electronic Health Record Technology (CEHRT) and then use automated electronic systems to aggregate, calculate, filter, and submit the data to CMS in a standard format. End-to-end reporting is available for all reporting mechanisms except claims-based submissions and is not specific to certain quality measures. Instead, it applies to any measure where the submission pathway is fully electronic after the data is initially captured in CEHRT. Any process that involves manual extraction and re-entry of data does not qualify as end-to-end electronic reporting.
Each bonus point option has a 10 percent cap. For most family physicians, this means a limit of six to seven bonus points for high-priority measures and six to seven bonus points for end-to-end electronic reporting.
Putting it all together
This article has discussed four factors to consider when selecting and reporting quality measures and how each can affect your quality category score under MIPS. Other factors must be considered as well, such as reporting method (claims, qualified registry, QCDR, EHR, web interface, or CAHPS survey) and ease of data collection, although these do not directly affect scoring. To see a comprehensive scoring example, see “Quality category scoring example.”
It is important to remember that you can report as many measures as you want, but CMS will only use the top six scores to calculate your quality score. However, any reported measure that includes at least 20 cases and meets the data completeness threshold can be reported publicly by CMS on its Physician Compare website, so this may influence whether you report extra measures.
The rules for implementing MIPS will evolve, as will physicians' strategies to optimize scores. For example, CMS intends in the future to score improvement as well as achievement but has not yet said how. Meanwhile, as physicians become more experienced with MIPS, CMS will make the process more strict – for example by eliminating the three-point minimum for reporting measures, raising the 50 percent data completeness criteria to 60 percent or higher, and increasing the performance period from 90 days to a full year. As discussed earlier, physicians may also receive fewer points for topped out measures.
To make quality improvement most helpful to your practice and your patients, you should prioritize measures that are relevant to your patient population, have the potential to affect your patients' health in substantial ways, improve the value of health care, and provide room for improvement. Once you identify these important measures, you can determine which ones are best for you to report on.
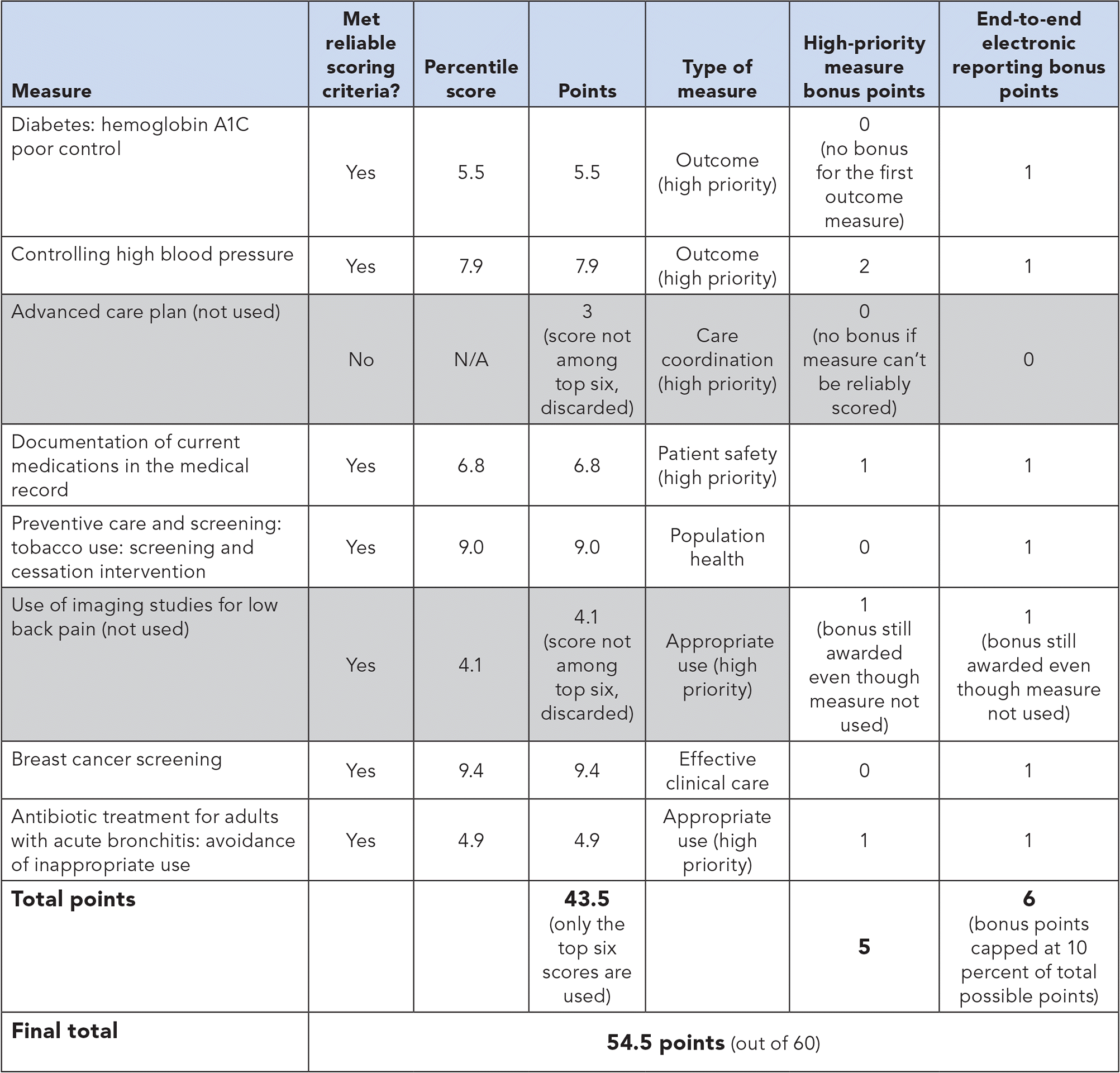
QUALITY CATEGORY SCORING EXAMPLE
The following is the quality measure scoring for a hypothetical physician who is not part of an Advanced Alternative Payment Model, who belongs to a group with 15 or fewer clinicians, and who reported measures for at least 90 days in 2017 using a qualified registry. Two of the lower-scoring measures ("advanced care plan" and "use of imaging studies for low back pain") are tossed out to reach the necessary six reported measures. Divided by the maximum potential score of 60, the physician's 54.5 points would give the physician a MIPS quality category score of 90.8 percent. In 2017, any score above 3 will avoid a negative payment adjustment.
| Measure | Met reliable scoring criteria? | Percentile score | Points | Type of measure | High-priority measure bonus points | End-to-end electronic reporting bonus points |
|---|---|---|---|---|---|---|
| Diabetes: hemoglobin A1C poor control | Yes | 5.5 | 5.5 | Outcome (high priority) | 0 (no bonus for the first outcome measure) | 1 |
| Controlling high blood pressure | Yes | 7.9 | 7.9 | Outcome (high priority) | 2 | 1 |
| Advanced care plan (not used) | No | N/A | 3 (score not among top six, discarded) | Care coordination (high priority) | 0 (no bonus if measure can't be reliably scored) | 0 |
| Documentation of current medications in the medical record | Yes | 6.8 | 6.8 | Patient safety (high priority) | 1 | 1 |
| Preventive care and screening: tobacco use: screening and cessation intervention | Yes | 9.0 | 9.0 | Population health | 0 | 1 |
| Use of imaging studies for low back pain (not used) | Yes | 4.1 | 4.1 (score not among top six, discarded) | Appropriate use (high priority) | 1 (bonus still awarded even though measure not used) | 1 (bonus still awarded even though measure not used) |
| Breast cancer screening | Yes | 9.4 | 9.4 | Effective clinical care | 0 | 1 |
| Antibiotic treatment for adults with acute bronchitis: avoidance of inappropriate use | Yes | 4.9 | 4.9 | Appropriate use (high priority) | 1 | 1 |
| Total points | 43.5 (only the top six scores are used) | 5 | 6 (bonus points capped at 10 percent of total possible points) | |||
| Final total | 54.5 points (out of 60) | |||||
RESOURCES
American Academy of Family Physicians MACRA Ready resources
Family Practice Management MACRA and Value-Based Payment articles
The Centers for Medicare & Medicaid Services Spreadsheet of quality measure benchmarks
