Taking one small step at a time, primary care practices can lead the way as the health care system begins to reward value.

Family physicians have always been the quarterbacks of our health care system. Today, they're increasingly under pressure. Across the country, our health care system is going through a transformational shift, from rewarding volume to rewarding value. This shift, which bases reimbursement on the quality of care provided rather than just the number and type of services, can feel overwhelming, but it may ultimately give family physicians new opportunities to prosper. It may also enable family physicians to finally be able to offer patients the kind of care that drew them to medicine in the first place – personal, proactive care that provides true value for patients without wasting resources.
Family physicians face some headwinds. Many still have a difficult time accessing their patients' data from outside their practices, making it difficult to measure and improve quality, and in some cases larger players in the system are actively blocking it. All too often, reporting requirements are duplicative or burdensome. Even high-performing practices are questioning whether they have what it takes to succeed in value-based care.
The paradox of primary care is that, despite these challenges, small practices have some advantages in this new world. Smaller practices have a lower average cost per patient,1 cause fewer preventable hospital admissions,2 and have lower readmission rates when compared with larger practices.3 That's because big systems often find themselves with their feet in two different canoes; they may want to reduce total costs, hospitalizations, and high-cost procedures, but their financial incentives are still aligned with the old fee-for-service system. For example, if they prevent emergency room (ER) visits or preventable admissions, they lose a major revenue stream.
This is why, as we move toward a health care system focused on quality and value, small primary care practices are in the driver's seat. Primary care doctors account for only 6 percent to 7 percent of health care spending, but they can influence up to 85 percent of downstream costs.4,5 They set the course for how patients navigate our entire health care system.
They're also motivated. A recent survey from the American Medical Group Association found that 86 percent of practices with fewer than 50 physicians say they're ready to take on risk in the next two years.6
So where can family physicians start? With simple, specific steps that other family physicians are taking today, steps open to any physician willing to take a chance on them. This article will highlight four:
- Identify high-risk patients using annual wellness visits (AWVs), the hidden gem to assessing risk and knowing which of your patients need more outreach from you and your staff.
- Manage that critical juncture when a patient leaves the hospital, also known as transitional care management (TCM).
- Gather data on your patients' outside care so you can identify major areas of ineffective – or even counterproductive – spending.
- Manage your referrals, including when you refer, to whom you refer, and what you expect when you make a referral.
Ultimately, steps like these can help family physicians succeed in a value-based system and provide better care to their patients, realize better health outcomes in their communities, and reduce costs across the system. Imagine how it would feel to spend less time checking boxes and churning out visits and more time helping the patients who need the most care. We can achieve this better health care system if we can free and empower primary care physicians, who are at the center. In this article, we share our personal experiences on this journey as a way to encourage others to take the next step.
Moving past reluctance to embrace annual wellness visits and chronic care management
I (Dr. Brull) have been a family medicine physician practicing in Plainville, Kan., for the past 15 years. My solo practice belongs to Post Rock Family Medicine, a loose association of five small practices. Until recently, we didn't have much experience with AWVs. We had looked at the criteria and requirements. We tried to imagine how they might fit into our existing visit pattern and work flow. We tried to understand what benefit we and our patients might get from another visit during the year, but we hadn't done much in the way of actually performing AWVs.
That began to change in the spring of 2015, when we joined with other local practices to form an accountable care organization (ACO). Our first goal was to perform AWVs on all of our Medicare patients. The purpose was to identify gaps in care, connect with patients who hadn't come in for a long while, and do outreach to patients who had been essentially invisible to us but were driving costs.
So off we went. We started slow and faced a host of barriers, such as “We don't have a form for that,” “There are so many requirements for this visit,” and “I'm not sure I even understand what I am supposed to be doing.” Our patients were a bit skeptical about being called in for a visit where the doctor wouldn't even be performing a physical exam. Additionally, our staff weren't sure where they were going to put all these people on the schedule; the visits took longer than the usual chronic care follow up. Preparation time could be 15 minutes to 20 minutes before the visit even started!
Despite the challenges, we trusted our partners that this was a “GT” (that's our code for “good thing”) and we pushed onward. By the fall of 2015, we had a form, an electronic health record (EHR) template, and a better understanding of the mechanics of the visit. We had patients test-pilot the visit with us, and they gave us feedback about how we could communicate the purpose and get through the process more smoothly. All of these things addressed our barriers. (See “Growth in Medicare annual wellness visits.”)
GROWTH IN MEDICARE ANNUAL WELLNESS VISITS
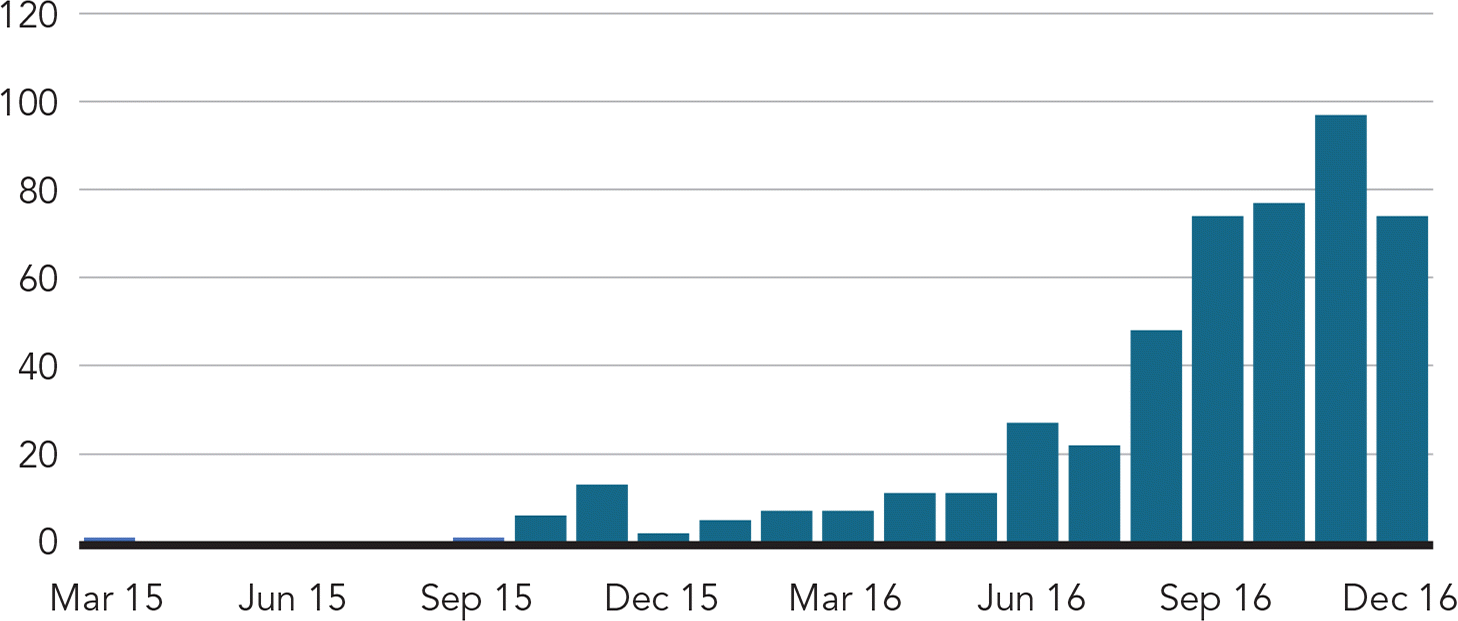
In December 2015, we took a leap of faith and hired a care manager who began doing most of the AWVs for the clinic, which has five physicians and three nurse practitioners. We calculated that the revenue generated by AWVs and other care management services would cover the cost of the care manager. Our care manager was a licensed clinical social worker who had formerly worked in a dialysis clinic with some of the most clinically complex patients. So, naturally, she began performing AWVs on high-priority patients, whereas we had started with the “easy” patients.
That's when we began to see “the why.” She quickly identified patients with significant barriers to care – barriers we wouldn't have found in the typical 15-minute office follow-up visit – such as a lack of access to electricity, healthy food, or safe housing. These social determinants of health can cause uncontrolled diabetes (if the patient has no way to refrigerate insulin), hypertension (if the patient cannot afford medications), and poor adherence to regular office visits (if the patient lacks transportation). Connecting patients with utility company programs, finding low-income housing, and helping patients complete forms and enroll in community assistance programs all became part of the care manager's follow up from these AWVs.
Before doing AWVs, we did not routinely discuss advance care planning (ACP) with our patients; it was completed only as situations arose requiring immediate attention. This often led to having conversations in the emergency room or hospital, usually during a time of significant illness – not the optimal point to start the conversation. During all AWVs, we now ask about ACP documents in a nonthreatening moment, during a routine office visit. For patients who have not considered this, we have time to answer questions and provide information. This change has led to a dramatic increase in our understanding of patients' wishes, and also some funny stories. One taciturn 86-year-old farmer who was “retired” (only working 40 hours a week) and largely healthy responded to my question with this advice: “Don't you try to start my heart back up after it stops beating; I'll come back and haunt you!” This strong sentiment on the patient's part resulted in a brief conversation and a DNR order in the chart.
Having seen the benefits to both our patients and our work, we have moved from reluctant avoidance to enthusiastic pursuit of AWVs. Our goal now is to provide an AWV to every high-priority patient each year. We want to ensure we aren't missing any patients who may have developed worrisome changes in the previous year.
A natural extension of our AWV initiative was offering a chronic care management (CCM) program to patients who need extra attention. Currently, this program serves about 100 patients. For example, one of our patients had blood pressure that was stuck around 200/110 mmHg, despite multiple adjustments to her medication. Both the patient and her provider had started to give up hope, so we enrolled her in CCM. By gaining her trust, our care manager learned that the patient often had to stop taking her medication because of the cost. She didn't want to disappoint her doctor and felt too embarrassed to tell him about the problem. With our care manager's help, she enrolled in a pharmaceutical assistance program, got access to all her medications, and came back to our office with a blood pressure of 144/78 mmHg.
Taking on referral management
I (Dr. Lilly) am a family physician who has been in the same practice, Dunbar Medical Associates, in Dunbar, W.Va., for 25 years. Our independent practice has two locations, seven physicians, and five midlevel providers (NPs and PAs), and we belong to an ACO. Over the past two years, we have aggressively taken on referral management, engaging specialists in those areas of care that represent the biggest opportunity to close care gaps, improve efficiency, and stop waste.
Referral management can seem complicated, but it starts with a simple, honest conversation. We identified key specialists in our community and brought them together for a meeting with our ACO's primary care providers. We described the changes taking shape in health care and the need for all of us to take action.
We encouraged our primary care providers to examine their referral policies, procedures, and protocols and to think about issues such as the following:
- Am I referring patients too soon or too late? Could we do more in the primary care setting, or are we trying to do too much?
- Am I referring patients to specialists who use resources wisely, or are they providing unnecessary tests and procedures?
- Am I giving specialists the information they need?
- Am I getting back from specialists the information I need?
We encouraged our specialists to think about similar issues and welcomed their feedback. Mutual input is vital to achieving our shared goals, and we believe we can help one another break out of bad habits and tendencies, or develop better ones. We trust our referral base deeply – that's why we partner with them so often – and we know it's crucial to remove any barriers that stand in the way of success.
We also stressed the importance of working collaboratively, being flexible, and communicating about shared patients even when a formal referral is not necessary. For example, less than 24 hours after we met with some of our nephrology specialists to talk about ways we could work together better, I received a call directly from one of them. It concerned a fragile patient with stage-four chronic kidney disease who also had severe diabetes and systolic congestive heart failure. Thanks to the short call, our chronic care manager helped adjust the patient's diuretic and insulin and helped monitor her weight and fluid. I saw the patient the next day. Normally, this patient would have ended up in the ER or with a costly hospital admission – possibly even a “crash” into hemodialysis – but six weeks later, no further decompensation had occurred.
Other examples of where this collaborative approach has worked well include a patient presenting to primary care with non-emergent gastrointestinal bleeding who needed to be fast-tracked for a diagnostic endoscopic procedure and a patient with atypical chest pain evaluated by his primary care physician and directed to a cardiologist for acute outpatient consultation. Ultimately, these instances of collaborative care are helping patients avoid ER visits and overnight hospital stays.
Another key to our success was giving our primary care physicians access to a population-health database that our ACO uses. This platform connects with our local hospitals, health plans, etc., to provide comprehensive, detailed information about our patients' hospitalizations, prescriptions, procedures, and specialist visits. It allowed us, for the first time, to understand our patients' patterns outside of our own practice.
Effective referral management has helped us provide better and more cost-effective care. This helps us get a handle on the spending that occurs outside our walls and bring down costs. (See “Lowering cardiology costs.”)
LOWERING CARDIOLOGY COSTS
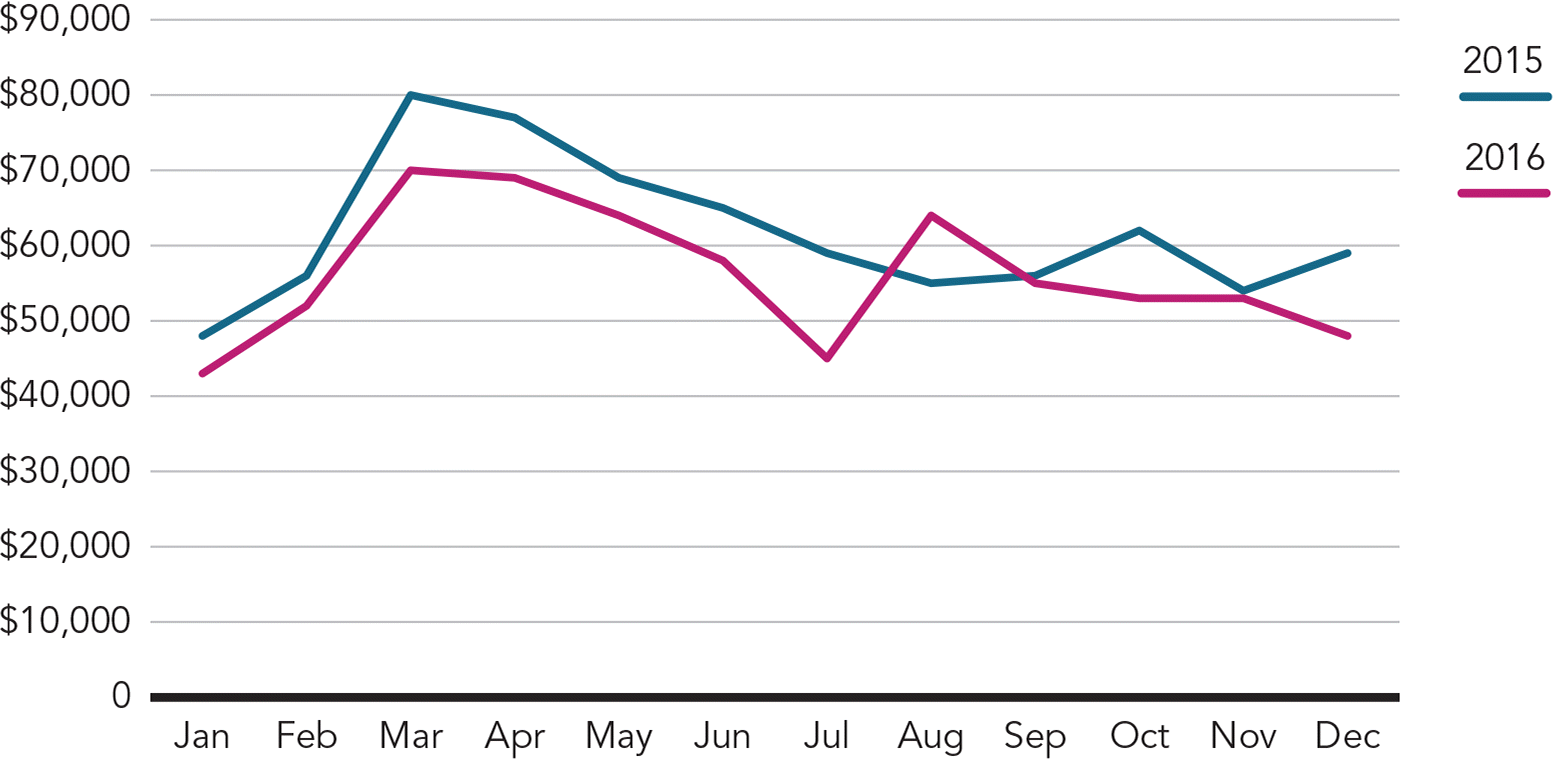
Our motto has been a quote from author and management expert Kenneth H. Blanchard: “No one of us is as smart as all of us together.”7 So we've expanded our outreach to more specialty groups and engaged skilled nursing facilities. Their progress and cooperation is helping us form a united front moving toward the common goal of patient-focused care.
Patients also play a critical role. At the end of the day, education of the patient may be the most important piece of the puzzle. The patient needs to know how the referral is generated and directed, as well as what to expect and what is expected of them. This focus on the patient's role and the patient experience helps us keep the “accountable” in “accountable care organization” so we can provide exceptional patient care both within and outside the walls of our primary care practice.
Transitioning to transitional care management
I (Dr. Navarro) have been a family physician in Delaware for more than 30 years. As the years have gone by, it has gotten more and more difficult for family physicians to maintain their independence. I have seen well-established practices consider shutting their doors because of the pressure. But this shift to value-based payment is starting to relieve some of that pressure. New tools and strategies for providing high-quality care are bringing new revenue into our practice. TCM is one example.
One of the most critical times for our patients is the post-hospitalization period. Many simple and avoidable mistakes occur during this transition because so many people are involved, handoffs don't occur or aren't clear, and everyone seems overburdened and rushed.
In the past, we had a sense that we were serving our patients well after a hospital discharge and providing timely follow-up appointments. But we couldn't articulate our process or quantify that we were doing a good job.
Today, we start planning for TCM services from as early as a few hours after admission. Through our ACO, we have access to a population-health platform that pulls in data from our local hospitals and other partners. This allows us to see when our patients are admitted, why they're admitted, and when they're discharged. It also provides us with an organized and prioritized list of patients who are in the TCM process that we can monitor daily. The information is loaded in real-time, and our patients are often amazed that we already know they have been hospitalized.
Just a short time ago, one of our patients was discharged from the hospital. We received a notification in the system and were able to bring the patient in for an appointment that very day. We talked with him about the care he needed at home and how he could avoid a potentially dangerous and costly readmission.
Information empowers us to call the patient, caregiver, or family member to plan a follow-up visit in the office and to facilitate care during the transition. At this time, we reconcile medications, arrange follow-up with other specialists, and order further testing if needed. Because of the advance notice, we can obtain medical records from the admission prior to the follow up. More importantly we can make sure our patients are not lacking anything that would put them at risk for readmission.
The obvious result from successful TCM is a reduction in our readmission rate and an increase in the coordination of care. The all-cause readmission rate for Medicare patients in our Delaware ACO has fallen from 15.3 percent in 2015 down to 12.7 percent by the end of 2016. There's something less quantifiable but even more important, though – a sense among our staff and patients that we're always in touch with our patients' needs. For these reasons, TCM has been an invaluable asset to the care of our patients.
Start small and look for bright spots
Many family physicians feel overworked and overwhelmed by the scale of changes needed in this new world of value-based health care. It's true that this transformation will not be easy for every family physician out there. Perhaps it's instructive to take a step outside of American health care for some lessons.
Jerry Sternin also found himself looking out on a new landscape in 1990. He had been tasked with opening the first office in Vietnam for the nonprofit Save the Children, and his first challenge was fighting childhood malnutrition. Talk about an overwhelming scale of changes; fighting malnutrition seemed to require entirely new systems of education, sanitation, and nothing short of an explosion in economic growth.
As Chip and Dan Heath pointed out in their book Switch, Sternin took a different approach to the challenge. He worked with mothers in local villages to survey the children, recording height and weight measurements. Sure enough, they found a number of children who weren't malnourished – despite facing the same challenges their neighbors faced. The parents of these children were taking unique, small steps that made a big difference – like serving a number of smaller meals throughout the day, actively feeding their children, and providing a mix of vital proteins and nutrients by adding in shrimp, crab, and sweet-potato greens.
Sternin and his team of intrepid mothers began to scale these changes through community cooking groups. And, sure enough, the little pebbles of change turned into a landslide. In Sternin's own village, he found that 65 percent of the kids were better nourished in just six months. In time, the program would reach 2.2 million Vietnamese people across 265 villages.
But it all started small – and it started by looking for the bright spots. As Chip and Dan Heath say, “We need to switch from archeological problem solving to bright-spot evangelizing…. These flashes of success – these bright spots – can illuminate the road map for action and spark the hope that change is possible.”8
The bright spots in value-based health care described in this article show that change is possible and provide a road map for action. Working together – across practices, hand-in-hand with knowledgeable partners employing proven tactics – family physicians can improve their use of tools like AWVs, referral management, and TCM to provide care that brings true value to patients' lives. In the short term, it means more revenue, and that's great news for the bottom line. But short-term revenue isn't the goal. The goal, the entire reason for this transition, is so we can get to a system with better outcomes for patients, smarter use of resources, and family physicians who are finally rewarded for the high-quality care they deliver.
SUGGESTED READING
The following articles provide more information on the topics discussed in this article.
ANNUAL WELLNESS VISITS
“Making Medicare Wellness Visits Work in Practice.” Cuena A. Fam Pract Manag. 2012;19(5):11–16. https://www.aafp.org/fpm/2012/0900/p11.html.
“Medicare Annual Wellness Visits Made Easier.” Hughes C. Fam Pract Manag. 2011;18(4):10–14. https://www.aafp.org/fpm/2011/0700/p10.html.
TRANSITIONAL CARE MANAGEMENT
“Transitional Care Management Services: New Codes, New Requirements.” Bloink J, Adler KG. Fam Pract Manag. 2013;20(3):12–17. https://www.aafp.org/fpm/2013/0500/p12.html.
CHRONIC CARE MANAGEMENT
“Answers to Your Questions About Chronic Care Management.” Moore KJ, Hays B. Fam Pract Manag. 2015;22(3):7–11. https://www.aafp.org/fpm/2015/0500/p7.html.
“Chronic Care Management and Other New CPT Codes.” Moore K. Fam Pract Manag. 2015;22(1):7–12. https://www.aafp.org/fpm/2015/0100/p7.html.
“Controlling Hypertension: Focusing on Why Makes How a Lot Easier.” Brull J. Fam Pract Manag. 2014;21(5):23–27. https://www.aafp.org/fpm/2014/0900/p23.html.
REFERRAL MANAGEMENT
“Optimizing Referrals and Consults With a Standardized Process.” Reichman M. Fam Pract Manag. 2007;14(10):38–42. https://www.aafp.org/fpm/2007/1100/p38.html.
“Reducing Waits and Delays in the Referral Process.” Murray M. Fam Pract Manag. 2002;9(3):39–42. https://www.aafp.org/fpm/2002/0300/p39.html.
“Simple Tools to Increase Patient Satisfaction With the Referral Process.” Jarve RK, Dool DW. Fam Pract Manag. 2011;18(6):9–14. https://www.aafp.org/fpm/2011/1100/p9.html.
ACCOUNTABLE CARE ORGANIZATIONS
“What Family Physicians Need to Know About ACOs.” Bobbitt J. Fam Pract Manag. 2011;18(5):17–22. https://www.aafp.org/fpm/2011/0900/p17.html.

