
This physician and medical assistant jump-start patient visits by teaming up and reversing some traditional roles in the exam room.
Fam Pract Manag. 2018;25(1):15-20
Author disclosures: no relevant financial affiliations disclosed.

As physicians search for more efficient ways to care for patients, a common refrain is that all medical staff must operate “at the top of our licenses.” This often involves assigning medical assistants (MAs) and nurses all tasks that do not involve the exam or medical decision-making.
However, this is not the only path to greater efficiency and can actually lengthen and complicate visits. We implemented a “team rooming” concept in which the physician (Dr. Cuenca) and MA (Lisa Perry) reverse certain roles as we begin the patient visit. This approach, combined with previsit planning, has led to more streamlined visits for patients, improved quality performance, and significantly better work-life balance at no additional cost.
KEY POINTS
Efficiency can be gained by “team rooming,” a workflow innovation in which a medical assistant conducts the initial history and obtains vitals while a physician documents relevant findings and enters orders as diagnostic and other needs emerge.
Previsit planning to identify preventive service needs and compile test results and other details boosts efficiency and quality.
Team rooming and previsit planning have saved time and improved satisfaction and quality without adding cost.
HOW OUR PROCESS WORKS
We work in an otherwise traditional multispecialty group with two physicians, two physician assistants, one medical assistant per provider, and a front office of four. We average 15 patient visits a day – mostly established patient visits with some walk-in, urgent care visits mixed in. We used to approach patient visits as most providers do now: The MA escorts the patient from the waiting area to the exam room, obtains the chief complaint, brief history, and key vitals, and inputs the information into the patient record. After rooming is complete, the physician greets the patient, obtains additional history, completes an exam and evaluation, and generates orders. The MA completes the orders, the physician finalizes the assessment and plan, and the MA prepares the exam room for the next patient. This system had its drawbacks, notably that some or all of the related documentation, referrals, and other paperwork accumulated for the physician to complete at the end of the day.
When we opened our panel to patients insured by Medi-Cal, California's version of Medicaid, in 2016, we found that these visits require additional paperwork (such as Medi-Cal “Staying Healthy Assessments”) and, on average, more complex care. Patients insured by Medi-Cal often have multiple chronic medical conditions, may not regularly seek preventive care, and often arrive for visits with a long list of items to discuss. Using our traditional visit workflow, we found we were quickly falling behind, which affected both the patients' and our own satisfaction with the care we provided. We noticed a decline in our performance on some quality measures around this same time. We realized we needed to rethink our workflow.
To speed things along, we began going into the exam room together, even reversing some of our normal roles, with the physician entering the chief complaint and initial patient history into the electronic health record (EHR) as they are obtained by the MA. This approach, combined with previsit planning and other changes, has enabled us to work faster, and it has produced other benefits as well. Here's how we do it:
Previsit planning. We begin preparing the day before the patient visit. Our clinic typically has a five-minute huddle each afternoon for the entire office staff to go over the next day's appointments and identify visits that might need to be extended, patients who might need to come in earlier to complete paperwork, records we might need to locate and review, and so on. After the meeting, between visits, the MA begins gathering information for the next day's patients.
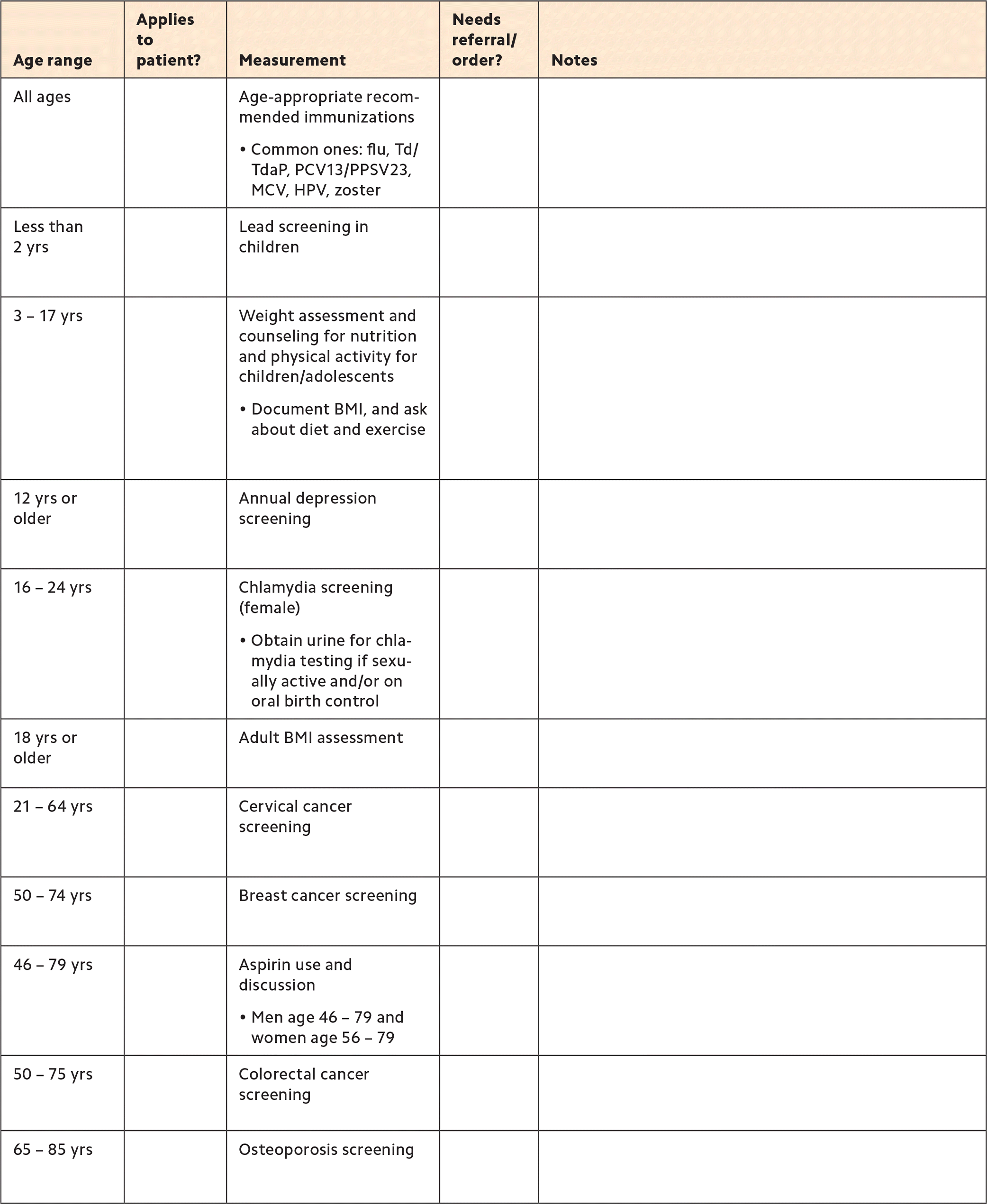
Using a paper-based, preventive care quality metrics checklist that we created (see “Previsit planning checklist”), she reviews each patient record, identifies care gaps, and compiles the results of any mammograms, pap smears, or other preventive screenings or labs provided by outside facilities. For Medicare annual wellness visits, she prepares a packet that includes a health risk assessment form and a Patient Health Questionnaire-9 (PHQ-9) depression screen. This packet is given to front-desk staff, who ask patients to complete it when they check in. The MA also reviews and performs a preliminary reconciliation of each patient's medications, if the information is available.
Meanwhile, the physician prepares for the next day's visits by reviewing prior progress notes and test results for established patients and developing a preliminary problem list and plan for each patient. He also prepares any surgical kits and other supplies, along with consent forms, that will be needed for visits that could involve procedures.
Each morning, the MA and physician have a mini-huddle focused on that day's visits. We compare notes, strategize and prepare based on the information we gathered, as well as clarify any questions raised during the previsit planning. Our workspaces are close together so that communication can occur often and frequently throughout the day.
| Age range | Applies to patient? | Measurement | Needs referral/order? | Notes |
|---|---|---|---|---|
| All ages | Age-appropriate recommended immunizations
| |||
| Less than 2 yrs | Lead screening in children | |||
| 3 – 17 yrs | Weight assessment and counseling for nutrition and physical activity for children/adolescents
| |||
| 12 yrs or older | Annual depression screening | |||
| 16 – 24 yrs | Chlamydia screening (female)
| |||
| 18 yrs or older | Adult BMI assessment | |||
| 21 – 64 yrs | Cervical cancer screening | |||
| 50 – 74 yrs | Breast cancer screening | |||
| 46 – 79 yrs | Aspirin use and discussion
| |||
| 50 – 75 yrs | Colorectal cancer screening | |||
| 65 – 85 yrs | Osteoporosis screening |
Team rooming. When a patient arrives for a visit, the front-desk staff gathers demographic information, verifies insurance, and gives him or her any forms needing completion. They also print out a one-page general intake form that the MA can use to take notes as needed during the visit. Using instant messaging, the front-desk staff alerts the MA and physician when the patient is ready to be roomed. The MA picks up the intake form, greets the patient, and escorts him or her to the exam room after measuring and noting height and weight.
When the patient and MA enter the exam room, the physician is already there, has the EHR open, and has loaded a progress note template. After greeting the patient, the physician explains that the MA will be asking some initial questions while he listens, records the information, and formulates additional questions. This greeting and explanation contribute to patients' acceptance of our approach, which has been universal.
Using the intake form and pre-visit checklist as guides, the MA then takes the initial history, reconciles medications, confirms any allergies, confirms pharmacy preference, takes vital signs, and reviews what preventive services the patient needs. The physician enters the pertinent information in the EHR in real time, securing more details from the patient as needed and entering orders for tests, referrals, or office procedures as diagnostic or preventive needs surface.
When her portion of the history-taking is complete, the MA returns to her desk and begins working on orders such as vaccine prep or labs while the physician performs the clinical exam. The MA may return to administer immunizations or facilitate any tests or procedures following the exam. The physician generally completes his assessment and plan after the exam or any on-site follow-up is completed. After discussing the plan with the patient and closing the visit, the physician typically prepares the exam room for the next patient. We use a second exam room when testing and other follow-up services cause visits to overlap.
Obviously, medical emergencies or unforeseen circumstances may sometimes prevent the physician from being in the room at the beginning of every visit. But we have found that meeting that goal, particularly with the first patient of the morning or afternoon, helps us stay on track for the rest of the day. Patients are roomed when the front-desk staff signals they are ready, even if the physician is delayed. The physician then enters the room as soon as possible during the intake process to help expedite the visit and work as a team with the MA. If the MA is delayed, other MAs in the practice are alerted that the patient has arrived so that they can escort him or her to the exam room where the physician can begin the visit.
To further heighten our efficiency, we maximize the features of our EHR, which allows us to set up procedure templates, drop-down menus, and key phrases for common conditions, such as colds or urinary tract infections. Using these is much faster than typing everything by hand.
BETTER RESULTS IN LESS TIME
Our workflow changes have produced several benefits, the biggest of which is saving time. Because the physician is typically already in the exam room when the patient enters, we essentially eliminate wait times between patient rooming and physician interaction. Finding the physician waiting in the exam room is often a big surprise and delight for patients who are used to waiting for their physician. They also appreciate that they only have to “tell their story” once, because both the MA and physician are present when they are asked about complaints and symptoms. The real-time charting also means that by the end of the visit, most of the note is complete and there is much less work waiting to be done at the end of the day or on weekends.
The MA has learned how to become a more proficient history taker and more confident with her medical knowledge, which can help expedite the physician's clinical decision making. Having two listeners means that we each may pick up on different parts of the patient's story, which can also be helpful. Our visits are also more efficient because the physician and MA can communicate immediately about next steps rather than doing it in the traditional time-delayed process.
We have not formally tracked our time savings, but on a recent day we saw 22 patients in seven hours, and notes were done by 5:15 p.m. If we had seen these patients under our old system, we would likely have been 30 minutes to an hour behind and still had hours of refills, paperwork, and patient messages to tackle after the last visit of the day. Of course our results vary from one day to the next, but we estimate after-hours work has been cut in half since starting this model.
The time savings has created capacity to work in patients who arrive late without becoming hopelessly bogged down, and it sometimes helps our ability to accommodate walk-in, urgent care visits. For same-day or add-on visits, we still do previsit planning with the MA quickly reviewing preventive measures and the physician reviewing chronic medical conditions and associated measures before the patient is roomed.
We also credit previsit planning and our visit workflow with dramatic improvements in our quality measures. For example, rates of colon cancer screening increased from 27 percent to 97 percent. (See “Quality measures.”)
Best of all, we gained quality and efficiency without having to invest in hiring scribes or care coordinators or acquiring new technology or training.
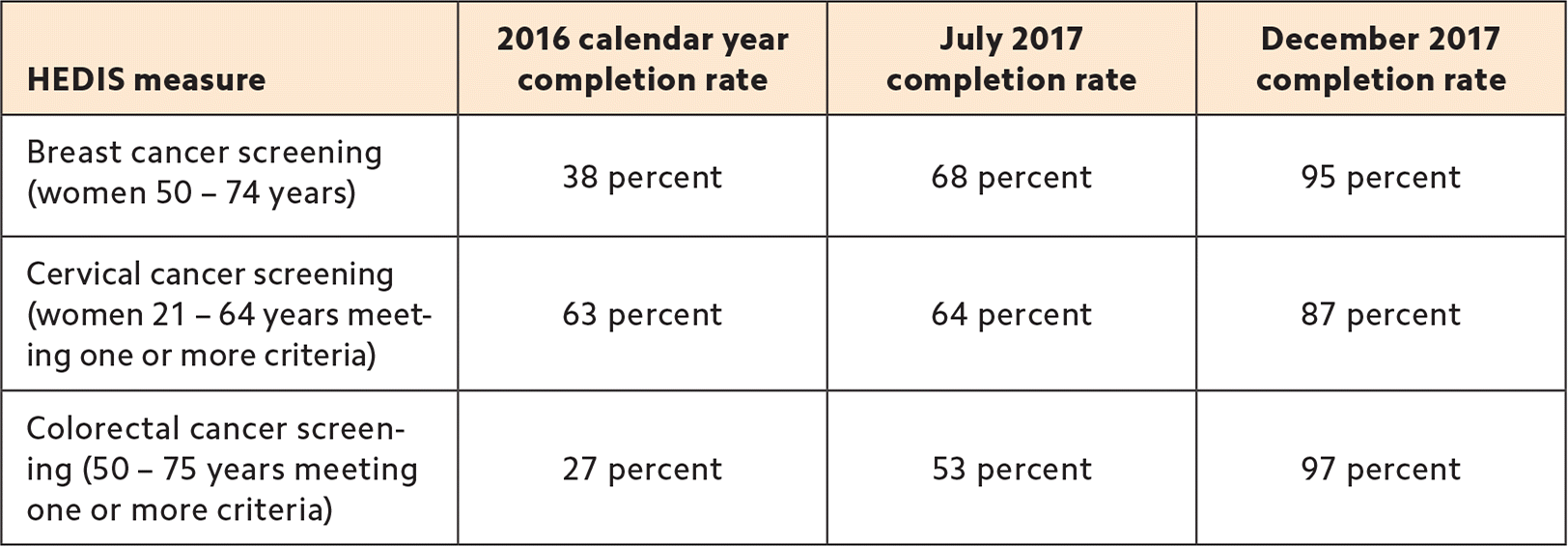
| HEDIS measure | 2016 calendar year completion rate | July 2017 completion rate | December 2017 completion rate |
|---|---|---|---|
| Breast cancer screening (women 50 – 74 years) | 38 percent | 68 percent | 95 percent |
| Cervical cancer screening (women 21 – 64 years meeting one or more criteria) | 63 percent | 64 percent | 87 percent |
| Colorectal cancer screening (50 – 75 years meeting one or more criteria) | 27 percent | 53 percent | 97 percent |
MAKING IT WORK
So far we are the only physician-MA team in our practice using this model, but we hope that others will find this of interest since there have been only positive outcomes from changing our patient rooming workflow. (See “Efficiency tips.”) The biggest challenge to making this type of arrangement successful comes down to changing your philosophy. As we said at the beginning, physicians are typically told that efficiency requires them to stick to direct patient care and to delegate so-called “busy work” to other staff. We have found it is helpful to be more flexible and to reconsider and redefine physician work.
The national health system presents challenges that demand our time and focus, including the EHR, quality and population health measures, and state insurance requirements. Meeting these challenges requires a true partnership between the physician and the MA. The MA must be fully engaged in helping the physician get the job done better and faster, and the physician must develop trust in his or her MA and be open to changing long-held, traditional ways of delivering patient care.
EFFICIENCY TIPS
For the medical assistant (MA) and front-office staff
Use the “previsit planning checklist” for preventive quality measures, and get used to doing this for every patient visit.
Print the patient's medication list ahead of time for the patient to review at check-in.
Request hospital visit notes or any outside lab reports prior to the patient's scheduled appointment.
For the physician
Review previous notes before the visit and anticipate the needs of the patient's chronic medical conditions.
Get into the mindset of team rooming.
Allow the MA to take a history under your direct supervision so he or she can learn and grow as a valuable partner in patient care.
For everyone
Make time for a daily “team huddle” so that everyone can anticipate patient needs for upcoming visits.
