Expanding the role of medical assistants to better support providers can improve not only traditional outcomes but also job satisfaction.

Burnout and job dissatisfaction pose a significant threat to primary care. Less than one-third of family and internal medicine physicians report they would choose the same specialty again,1 and one-third of health care employees report they are planning to look for another job.2
The factors contributing to burnout and dissatisfaction are many, including the use of electronic health records (EHRs), demand to see more patients, and change fatigue as practices reshape the way they deliver care consistent with the “Triple Aim” (improved population health, enhanced patient experience, and reduced cost). One study found that physicians spend only 27 percent of their time providing direct, face-to-face care to patients and almost half their time on the EHR or desk work.3 Delivering all of the appropriate preventive, chronic, and acute care to a standard primary care panel has proven to be impossible for a single physician, requiring an estimated 21.7 hours per day.4 Suboptimal access, poor outcomes, and escalating burnout, frustration, and early retirement are not surprising when providers shoulder most of this burden.
As a result of these pressures, the “Quadruple Aim,” which adds provider and staff satisfaction to the Triple Aim, has been proposed as a more sustainable approach to improving health care. To achieve the Quadruple Aim, leading primary care organizations are exploring advanced team-based strategies such as team-based documentation, previsit planning and testing, an expanded scope of practice for medical assistants (MAs) and nurses, team-based motivational interviewing and coaching, and delegation of certain elements of chronic disease care, preventive care, medication reconciliation, refills, and acute care to staff using standardized protocols. These strategies are designed not only to reduce provider burnout but also to reduce staff burnout by ensuring that they can grow professionally and engage more intimately in patient care.5 Beyond reducing burnout, delivery models that rely on a high-functioning team have become essential given rapid increases in medical information and more prevalent chronic disease.6
KEY POINTS
- When our health care system places too much burden on providers, we should not be surprised at the result: suboptimal access, poor outcomes, and escalating burnout.
- Increasing the MA-to-provider ratio to 2.5:1 and expanding the role of MAs throughout the patient visit can help practices achieve the “Quadruple Aim.”
- This team-based care model increased visit volume and patient access, improved clinical quality, and cut provider burnout in half.
THE ORIGIN OF OUR MODEL
Our organization's advanced team-based care model was inspired by the University of Utah's “Care by Design” model, which provided a financially viable Quadruple Aim strategy in a fee-for-service environment. Key components included increased MA-to-provider ratios and an expanded scope of practice for MAs, including an expanded rooming process that generates a preliminary history of present illness (HPI) and in-room documentation support (i.e., scribing). This model helped the University of Utah expand access and improve its financial performance, generating more than $5 million per month through in-network referrals and helping reverse a $21 million loss across its community clinics over five years.7
In early 2015, the University of Colorado Hospital decided to develop and pilot a similar model, the APEX (Ambulatory Process Excellence or Awesome Patient Experience) model. This article describes our experiences and early results at one of the two pilot sites, the AF Williams Family Medicine Center, an urban family medicine residency clinic with 26,000 office visits per year.
We developed our model over a series of eight rapid improvement events involving more than 120 providers and staff. Participants were tasked with deconstructing and reconstructing the original model. Improvement topics included the expanded rooming process, in-room support, post-exam workflow, and protocol development.
HOW IT WORKS
Prior to the APEX model, MAs' duties consisted mainly of escorting patients to the exam room, collecting vital signs, and executing provider orders at the end of the visit. We typically had an MA to physician ratio of less than 1:1.
Under the new team-based care model, we increased the ratio of MAs to providers to 2.5:1 and expanded the role of MAs throughout the patient visit.8 At the outset of each visit, MAs' tasks include the following:
- Elicit a comprehensive patient agenda,
- Collect or update elements of the patient's past medical, surgical, social, and family history in the EHR,
- Conduct detailed medication reconciliation, including removing expired prescriptions and marking medications due for renewal as “pending,”
- Use templates to document a basic complaint-based HPI and review of systems to begin the visit documentation for the provider (the provider later confirms key elements of the HPI with the patient to meet billing requirements),
- Use protocols to initiate certain clinical tasks, including rapid strep, urinalysis, urine HCG, A1C, and adult immunizations when indicated, prior to the provider portion of the visit,
- Review preventive care gaps (lipid and diabetes screening, mammograms, colon cancer screening, hepatitis C screening, immunizations, etc.), and either order the services based on protocols or mark them as pending for the provider to review.
The MA then stays with the provider in the exam room to provide additional documentation support such as helping to note additional HPI and physical exam findings, preparing pending orders to be signed, and writing out patient instructions.
After the provider portion of the visit, the MA completes the visit by executing orders (lab draws, immunizations, paperwork, etc.), reviewing instructions with the patient, scheduling follow-up appointments, and escorting the patient from the office. The increased number of MAs also gives providers additional support for handling inbox messages and tasks.
EARLY OUTCOMES
Our pilot program increased visit volume and improved access, particularly for new patients, while simultaneously improving the provider experience, maintaining excellent staff and patient satisfaction scores, and improving measurable clinical quality. (See “Quality, volume, and access improvements under the new model.”) The most notable outcomes were as follows:
Quality. The pilot clinic saw significant improvement in clinical quality measures such as colon cancer screening (12 percent increase from baseline), breast cancer screening (46 percent increase), hypertension control (13 percent increase), and common intermediate clinical measures for diabetes care such as foot exams (20 percent increase) and retinal exams (25 percent increase).
Provider experience. Providers reporting symptoms of burnout decreased by half, from 56 percent to 28 percent. Providers are requesting additional clinical hours, as well as showing increased willingness to initiate and participate in quality improvement activities. Provider time spent logged into the EHR after hours is also dropping. Provider experience scores have improved in all measured domains, including overall satisfaction, efficiency, documentation, patient-centered care and patient engagement, team-based care, team functioning, and inbox management. Additionally, the prospect of practicing under this model has contributed to unprecedented success in our provider recruitment efforts.
Staff experience. Staff experience scores were high across all domains prior to our pilot. We were concerned that the shift to the new model might hurt these scores, but despite the dramatic changes in our staff members' work, staff experience scores remained unchanged.
Patient experience. Our clinic's Clinician and Group Consumer Assessment of Healthcare Providers and Systems (CG-CAHPS) “top box” scores improved in key domains related to staff and provider communication, such as listening skills and providing information that addressed patient concerns, as well as in patients' overall willingness to recommend our practice to others.
Visit volume and costs. When we launched the new model, we planned to cover the costs of the additional MA staff through increased visit volume, made possible (and acceptable to providers) by the efficiencies of the new model. In time, we were able to adjust schedule templates to allow more visits. Seeing one to two additional patients per provider per half-day clinic session was sufficient to offset the additional staffing costs once we factored in downstream revenue.9 Increased visit volumes have kept per-visit staffing costs stable. Staff salary dollars per visit and paid hours per visit were unchanged from baseline after 12 months, with the exception of a modest, market-driven pay rate adjustment.
QUALITY, VOLUME, AND ACCESS IMPROVEMENTS UNDER THE NEW MODEL
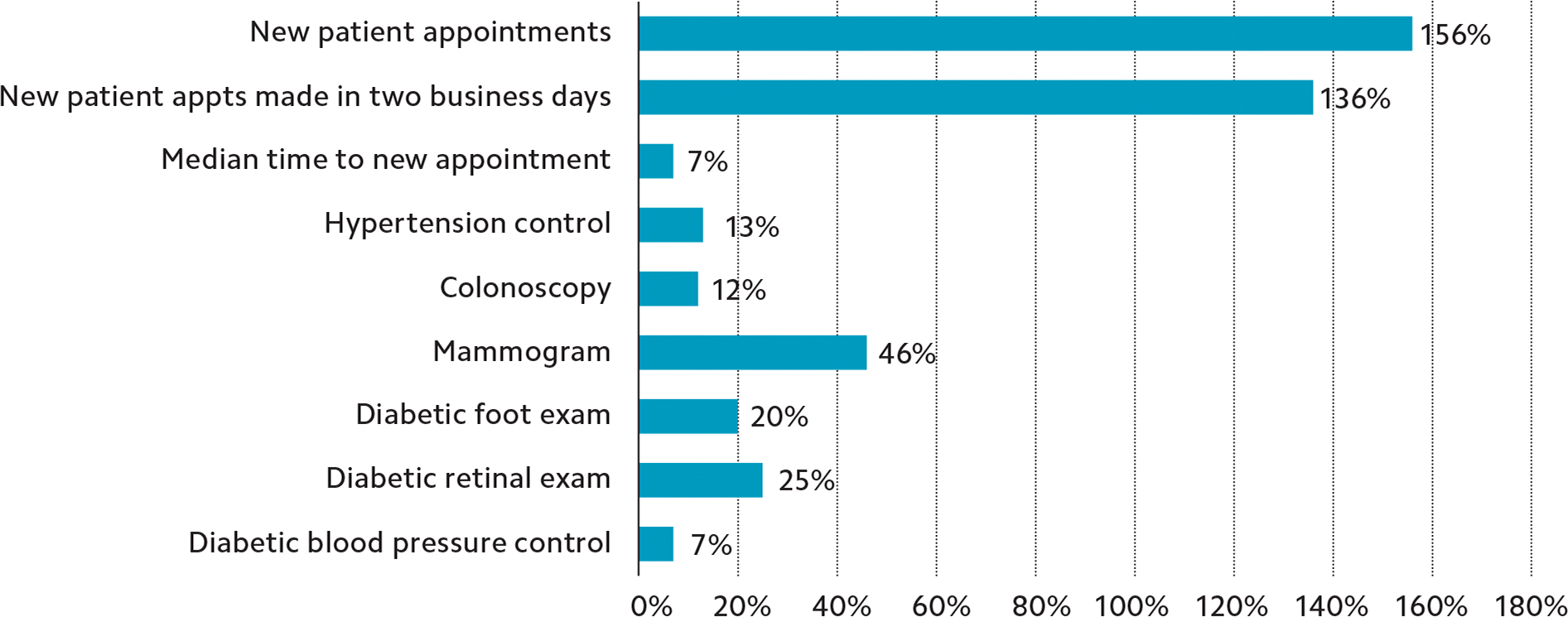
The chart compares data from six months after the go-live date with the mean of the previous six months. Note that the median time to new appointment is reported as its inverse, i.e., the 7-percent reduction in wait time is shown as a 7-percent improvement.
LESSONS LEARNED
Implementing a new care model is not easy, and along the way we learned several lessons that may help other practices:
Build the burning platform, and keep it burning. Our health system's primary care leadership advocated for this model. Our practice was chosen to be one of the pilot sites because we are a large, complex residency practice. If we could make the model work here, it would likely work in other practices. But because our providers and staff were not involved in the decision-making process, early on our clinic leadership needed to create a clinic-wide understanding of why this change would be hard but ultimately good. In our discussions with providers, we focused on the Quadruple Aim, highlighting opportunities to expand MA scope of work and provide documentation assistance. We conducted multiple “lunch and learns” for provider updates and training. For staff, clinic leadership painted the picture of how operating under this model would make our clinic special, would permit them to have a bigger role in direct patient care, and would reduce the pace of work.
Practice to make it perfect. MAs had blocked time to meet with a nurse educator who trained them on agenda setting, medication reconciliation, updating medical histories, scribing, and new protocols. They also spent time shadowing providers to observe what goes on in the exam room between the patient and provider. Prior to our go-live date, half the clinic was closed for two days for mock training with simulated patients. For the first two weeks of the new model, we gave providers 40-minute visits to allow extra time and training with the new workflows.
Go live before go live. Because the model required major workflow changes for MAs, we phased in pieces of the new model prior to go live, specifically medication reconciliation, addressing gaps in care, and recording the past medical, surgical, social, and family history. Pending orders, pre- and post-visit work, and in-room documentation were phased in at or after go live.
Have a plan B. It took much longer than expected to hire enough MAs to fully support the model. A local market disruptor began offering significantly higher MA wages, we were not offering MAs additional pay for their expanded work, and a handful of veteran MAs left because of the change in their roles and responsibilities. Lacking full staffing at launch time, we created a “partial model” that included the expanded rooming process, delegated order protocols, and post-visit work but did not include in-room documentation support. As we hired additional MAs, we were able to flex between the full and partial model based on day-to-day provider:MA staffing ratios and eventually achieved consistent use of full-model workflows eight months after going live.
In time, with the influence of advocates in the practice, the hospital system approved pay increases for MAs trained in the new model, which stabilized the size of our MA team. Additionally, given the large increase in the size of that team, we developed a lead MA position (accompanied by a pay increase) to help manage the larger team, support training, and sustain the model. We further developed a Staff Engagement Council to provide a voice for staff throughout the clinic. This group publishes a monthly newsletter to communicate successes and workflow changes to providers and staff.
Be prepared to negotiate. Hospital leadership initially wanted to increase visit volume as quickly as possible to support the costs of implementation. However, the lack of full staffing made visit-volume expansion exceptionally challenging, both operationally and in terms of morale. Clinic leadership eventually negotiated a phased-in increase in visit volume, gradually converting a proportion of 40-minute visits to 20-minute visits.
Work on communication issues (and don't call your MAs “scribes”). As a clinic providing integrated behavioral health care for more than 30 years, we thought of ourselves as team-based care experts. However, in implementing and sustaining these changes, we realized we had a lot to learn about provider-staff interaction and cultural issues affecting true team-based care. Leadership noted early communication issues between providers and MAs. For example, the MA would room the patient, elicit seven agenda items including an early refill on opiates, and relay the patient's agenda to the provider. The provider would then sigh in frustration, causing the MA to think she did her job incorrectly and then not elicit the full agenda with the next patient. Providers struggled with allowing MAs the full time needed for the expanded rooming process, feeling the urgent need to begin the visit as soon as possible. MAs had strong negative reactions to being asked to “scribe,” as that role felt demeaning. As a result, we adopted “in-room documentation” as our preferred terminology. Providers were motivated to improve these communication challenges because of the benefit of the additional staffing support. To motivate MAs, we engaged them to help with model improvements and showed gratitude for all the support they provide.
Another hurdle involved the deployment of delegated orders. For years, MAs' training and guidance focused on a very narrow definition of their scope of practice – what they were not permitted to do. Changing the predominant attitude from “Can I do that?” to “Of course I can do that!” required substantial communication, support, and reinforcement. As a result, we devoted most clinic meetings to teambuilding for six months, guided by our practice coach and behaviorist. One year after going live, the clinic even closed its doors for an afternoon teambuilding retreat at a local park.
Embed a practice coach. A key driver of our success was a full-time embedded practice coach who served as a clinic leader. This role was designed to serve as a neutral third party, unaffiliated with management or any group or faction within the practice. As a neutral advocate for the model's success, she was better able to uncover issues among staff and providers than leadership or their direct supervisors, and she was quick to develop strategies in response. For example, she hosted a lunch-time Crucial Conversations book club in response to communication deficits within the practice. Additionally, she was able to support struggling providers through direct observation, conversation, and facilitation as needed. She had the permission of the leadership team to request that clinic time be blocked in support of these interventions.
Work with the boss's boss's boss. A empting disruptive innovation as a single clinic within a large multi-hospital system carries risks as well as benefits. Although the system agreed to pilot the model, barriers to progress were often slow to move. Examples include delays in hiring due to a slow process for approving pay raises; compliance, legal, and other internal regulatory oversight of the new delegated order protocols; concerns about certain elements of shared documentation in the EHR; and lack of agreement about the proper role of residents in the model. However, once the model proved successful and the decision was made to expand it to other clinics, the system vigorously supported centralizing resources to sustain ongoing change.
Know when to pause. The initial redesign consumed everyone's attention, but as the model became routine, the clinic inevitably turned its attention to other quality improvement work. As these new efforts were occurring, audits of MA work-flow adherence indicated problems with sustaining change. At the same time, the organization was facing the arduous NCQA recertification process, and staff morale started to dip. As a result, clinic leadership put a moratorium on any additional workflow changes. This was challenging for a practice that prides itself on being a laboratory of innovation. Despite this, the temporary hold was well-received as leadership communicated the current state of low staff capacity for change and the need to protect them from burnout.
NEXT STEPS
Since launching our pilot, six additional primary care clinics have adopted the model (now named Primary Care Redesign), and we have adapted it for pilot testing in subspecialty practices as well. MA training has been removed from the individual clinics and centralized in a 40-hour training program known as MA Academy, which has reduced MA onboarding time from nine weeks to four weeks while minimizing training-related disruptions to clinic flow. As expected, new workflows are not sustained perfectly over time, but we have gradually developed tools to help maintain change, including a regular multipractice meeting, a shared data dashboard for tracking clinical processes and outcomes across practices, structured MA workflow audits, assessments of provider fidelity toward the model, and the deployment of practice coaches to the other practices.
While the model continues to evolve, we are convinced that increasing provider support with additional MAs, and increasing the MA's role during and after the clinic visit, has proven to be one of the best ways to improve access, clinical metrics, and provider and staff satisfaction.

