With too many patients taking too many unnecessary medications, deprescribing has become a required skill for primary care physicians. Here's how to go about it.
Related articles from American Family Physician: "Deprescribing Antipsychotics for Behavioral and Psychological Symptoms of Dementia and Insomnia" and "Deprescribing Is an Essential Part of Good Prescribing."

Ms. Horatio is a 76-year-old patient who has been coming to your practice for more than 10 years. She has Type 2 diabetes with stage-3 chronic renal disease and painful diabetic neuropathy of bilateral lower extremities, chronic obstructive pulmonary disease, stable coronary artery disease, and hypertension. She has seen a cardiologist, pulmonologist, and neurologist for additional care. At today's visit with you, her family physician, she has brought a brown paper bag filled with all her medications per your request. Her medications include amitriptyline, atenolol, atorvastatin, low-dose aspirin, diphenhydramine hydrochloride, clopidogrel, conjugated estrogen tablets, ferrous sulfate, glyburide, isosorbide dinitrate, lisinopril, nifedipine extended release, omeprazole, paroxetine, pregabalin, tolterodine, tiotropium inhaler, and zolpidem. Where do you begin?
WHAT IS POLYPHARMACY?
Polypharmacy is typically defined as the prescription of five or more medications. However, it also refers to the prescription of medications that do not have a specific current indication, that duplicate other medications, or that are known to be ineffective for the condition being treated. In other words, polypharmacy is the use of multiple medications that are unnecessary and have the potential to do more harm than good.
Polypharmacy is highly prevalent, especially among older adults. A 2016 study found that 36 percent of community dwelling adults age 62 to 85 were taking five or more medications.1 This is up from 31 percent in 2005. At this rate of increase, almost half of the older population could be affected by polypharmacy by 2030.
Patients at risk for polypharmacy are older than age 62, have comorbidities, have multiple prescribers or pharmacies, self-treat with over-the-counter medications, and have a history of hospitalizations.1,2,3 They also likely go to practices with poor medication tracking processes, including medication lists that are not updated or are inaccurate. Poor medication tracking processes are more prevalent than physicians might think. For example, an internal study at my previous organization found that only 19 percent of office visits to general internists included a medication review.
Polypharmacy has multiple adverse consequences. These include adverse drug events and other safety events such as falls, medication nonadherence, increased mortality, increased cost, and functional impairment. Polypharmacy often begins when a medication causes an adverse drug event, leading to additional treatment, which causes an additional reaction, and so on.4 The probability of harm increases exponentially with each medication.
All medications have potential negative consequences. For instance, delirium and worsening of dementia are common with anticholinergics, benzodiazepines, and proton-pump inhibitors; falls are more common with patients on antihypertensives, antipsychotics, benzodiazepines, and opioids; constipation is common with opioids and calcium channel blockers; and orthostasis is common with anticholinergics, antihypertensives, and sulfonylureas.
To avoid polypharmacy and the risks of medication-related harm in their patient populations, family physicians should implement effective medication management practices, including the strategy known as deprescribing. (See the related editorial, "What Needs to Change to Make Deprescribing Doable.")
KEY POINTS
- Polypharmacy is the use of multiple medications that are unnecessary and have the potential to do more harm than good.
- Patients at risk for polypharmacy are older than age 60, have comorbidities, have multiple prescribers or pharmacies, self-treat with over-the-counter medications, have a history of hospitalizations, and go to medical practices with poor medication tracking processes.
- Medication reconciliation often begins with a “brown bag” review of the patient's medications.
- To help patients buy into the deprescribing process, consider discontinuing one medication at a time or tapering medications.
THE DEPRESCRIBING PROCESS
Deprescribing is a set of interventions to identify inappropriate or unnecessary medications and discontinue them. (See “A deprescribing algorithm.”) In essence, it is backing off of care for the safety of the patient, like taking your foot off the accelerator of medical therapy. Studies have suggested that deprescribing leads to improvement in cognition, fewer falls, and improved survival.5
A DEPRESCRIBING ALGORITHM
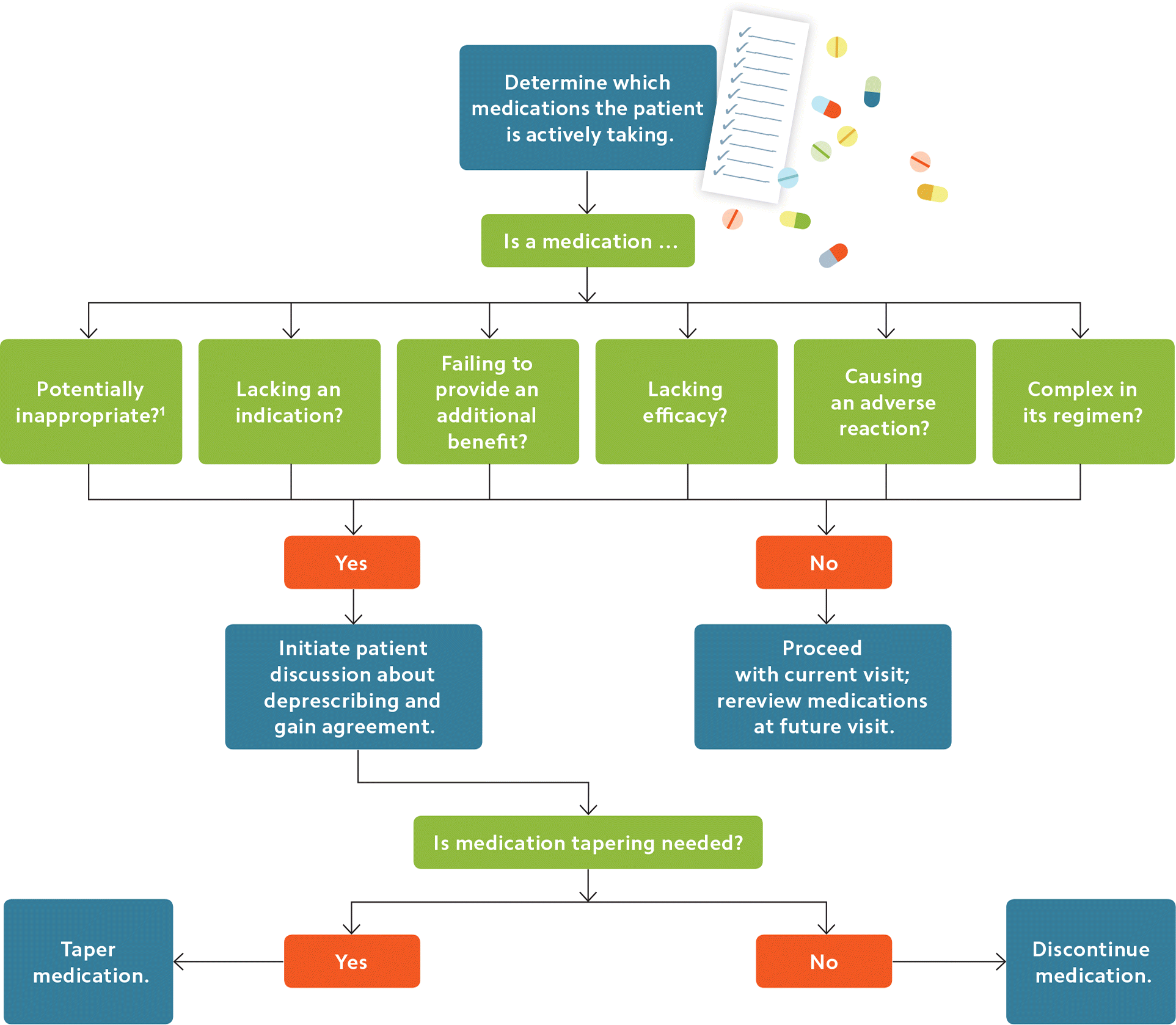
1. Consider Beers list drugs, opioids, anticholinergics, NSAIDS, etc.
1. Review all current medications. The first step in deprescribing is medication reconciliation, often centered around a “brown bag” review. Instruct the patient to bring all of his or her medications (including prescription drugs, over-the-counter medications, and supplements such as vitamins and minerals) to a visit, and have your nurse or medical assistant take a medication history. The information collected, including which medications the patient is actively taking, what regimen is being followed, and whether the patient has experienced any side effects, should be documented in the patient's medication list in the electronic health record (EHR). By the end of the visit, your nurse should be able to generate a patient “medication card,” which can empower the patient to maintain his or her own medication list going forward and share the information with his or her providers across all settings. (For additional information on medication reconciliation, see “Resources.”)
2. Identify any inappropriate, unnecessary, or harmful medications. Together with the patient, review all medications listed in the updated medication list and consider which ones are offering benefit and which are causing harm. Look for medications that are potentially inappropriate (per the Beers list, discussed below), lack efficacy, lack an indication, don't provide additional benefit, or require a long duration for effect.7 Also consider whether the patient would like to stop any medications because of negative side effects or whether any medications have complex dosing regimens that could be avoided.7 Drug classes such as anti-psychotics, statins, antihypertensives, benzodiazepines, proton-pump inhibitors, and nonsteroidal anti-inflammatory drugs/COX-2 inhibitors/acetylsalicylic acid are common targets of deprescribing.7
To aid busy physicians in deprescribing, a number of helpful tools are available:
- The Anticholinergic Burden Calculator can help you evaluate a patient's potential for serious anticholinergic effects. In the geriatric population, this is a great tool to start with, as reducing or eliminating medications with high anticholinergic burdens can often improve patients' overall function and quality of life. Start with deprescribing those medications in the highest (level 3) category.
- The Beers List from the American Geriatric Society lists medications that pose the highest risk to older patients, along with alternatives. There are numerous versions of this list, but one of the better configured lists is found here: https://bit.ly/2GQhM2Y.
- Deprescribing.org, developed by a team of physicians and pharmacists, provides deprescribing guidelines and algorithms, patient decision aids, and an up-to-date resource list of evidence and research.
- MedStopper is an online tool that allows you to enter a drug list for a specific patient and receive recommendations regarding which medications might be discontinued or switched.
3. Plan deprescribing with the patient. Many patients will resist stopping medications, especially those they have been taking for a long time. They may be concerned about their conditions worsening or about contradicting the original prescriber. To help patients buy into the deprescribing process, consider discontinuing one medication at a time or tapering medications if necessary, and assure your patients that you will monitor them for worsening conditions or withdrawal effects. Also, discuss the potential or real adverse effects of their medications; the potential benefits of deprescribing, such as reduced risk of hospitalization, cognitive or functional gains, and improved quality of life; and the minimal (if any) impact deprescribing would have on their conditions. This latter point is especially true for medications prescribed without a clear indication or with no significant clinical benefit. These benefits of deprescribing are also critical to consider in patients who are receiving palliative or end-of-life care.
4. Regularly rereview medications. Because deprescribing may require tapering of medications or may involve withdrawal symptoms, the process needs to be monitored closely. Additionally, on at least an annual basis (if not at every visit), look closely at all medications again. Many patients see multiple providers and can quickly accumulate medications across conditions. As much as you are able, actively engage your specialist colleagues in discussions of benefits and harms of new medications, as well as other options. One way to facilitate this is by using electronic or paper consultation reports that clearly list new or modified medications.
Collaborative arrangements with pharmacists may also be helpful.8 Depending on the practice setting, collaboration between pharmacists and family physicians can occur during medication history taking and medication reconciliation, drug therapy recommendation and deprescribing, or the management of adverse drug reactions. The IMPACT program in Ontario has had success with this collaborative model for some time using a variety of strategies including separate pharmacist visits, collaborative visits with the physician, and pharmacist-patient follow-up.9
RESOURCES
Medication reconciliation
- How-to Guide: Prevent Adverse Drug Events (Medication Reconciliation). Boston: Institute for Healthcare Improvement; 2011. http://www.ihi.org/resources/Pages/Tools/HowtoGuidePreventAdverseDrugEvents.aspx.
- Medications at Transitions and Clinical Handoffs (MATCH) Toolkit for Medication Reconciliation. Rockville, MD: Agency for Healthcare Research and Quality; 2012. https://www.nm.org/-/media/Northwestern/Resources/for-medical-professionals/northwestern-medicine-match-toolkit.pdf.
- Ontario Primary Care Medication Reconciliation Guide. Ontario: Institute for Safe Medication Practices Canada; 2015. https://www.ismp-canada.org/download/PrimaryCareMedRecGuide_EN.pdf.
Deprescribing
CASE STUDY CONTINUED
Before you enter the exam room to see Ms. Horatio, your nurse Lois sits with her and reviews the medications she has brought from home in a brown bag. One by one, Lois examines each medication, including the refill date. She asks Ms. Horatio if she is currently taking the medication, when her last dose was, and if she has had any bad reactions to it. For medications Ms. Horatio is not taking currently, Lois asks, “When did you stop taking this medication?” and “What was going on that made you stop taking it?” Lois records this information in the EHR. At the end of the discussion, she asks Ms. Horatio, “Are there any other medications you might be taking, such as vitamins, supplements, or over-the-counter medications?” Ms. Horatio mentions that she takes some ginseng tablets in the morning that her daughter suggested would increase her energy. Lois records that information in the EHR as well. She will later generate a “medication card” for Ms. Horatio to keep in her purse, share with other doctors at other offices or the hospital, and add to or modify when her medications are changed.
A few minutes later, when you enter the exam room, you sit with Ms. Horatio and review the updated medication list. You explain why she doesn't need to continue a number of medications, including the estrogen, iron supplements, and proton-pump inhibitor. You note that her gynecologic history and last hematogram don't indicate a need for therapy at this time and explain that her proton-pump inhibitor may be contributing to her mild cognitive impairment. You also recommend tapering and stopping the zolpidem over several weeks and, in its place, beginning a regimen for sleep hygiene. Based on the results of an anticholinergic burden analysis, you determine that Ms. Horatio has a high anticholinergic burden, and you recommend tapering and eliminating the amitriptyline and paroxetine, as well as discontinuing the diphenhydramine hydrochloride. If symptoms confirm her need for an antidepressant, you will prescribe a newer, less anticholinergic medication at that time. You make a plan to follow up with her in two weeks.
A KEY ROLE FOR FAMILY PHYSICIANS
Deprescribing is a necessary process in today's practice environment where patients often take multiple drugs prescribed by multiple physicians who are not in direct communication with one another. Primary care physicians are well positioned to manage this critical process.

