These communication skills will increase patient engagement and satisfaction without slowing you down.

The ability to communicate well is foundational to family medicine. Skillful communication helps family physicians establish relationships, solicit and share important information, and work effectively with patients, family members, and the public.1 However, when physicians are faced with the time pressures of a busy clinical work day, careful communication often gets lost in the shuffle. For example, a cross-sectional survey in the offices of 29 family physicians found that when soliciting patient concerns at the outset of a visit, physicians typically redirected patients' opening statements after a mean of 23.1 seconds.2 Once redirected, patients rarely return to their list of concerns, leading to unvoiced agenda items that are never addressed during clinic visits.2 Another study of 35 outpatient primary care visits found that some of patients' more common unvoiced agenda items include “worries about a possible diagnosis and what the future holds; patients' ideas about what is wrong; side effects; not wanting a prescription; and information relating to social context.”3 These unvoiced agenda items often lead to related problematic outcomes.3
As a physician, you want to do all you can to provide your patients with the care they want and need. Fortunately, evidence suggests that employing some relatively straightforward communication strategies can help your patients feel heard, encourage them to provide you with accurate and relevant information, and help you guide them through the complexities of the diagnostic process without derailing your schedule.
KEY POINTS
- Through skillful communication, family physicians can help patients feel heard, encourage them to provide relevant and accurate information, and ease their fears and concerns about their health.
- Evidence suggests that four communication strategies may help family physicians achieve these goals and improve patient satisfaction without significantly affecting the duration of a visit.
1. TAKE A SEAT
The simple act of sitting down can make a conversation feel less hurried, more open, and friendlier. In fact, evidence suggests that taking a seat with your patients (as opposed to standing) can improve patient satisfaction by improving patient perception of the visit. Although it is typical for physicians to sit for at least part of an office visit, hospital rounding often involves a hurried entry into the patient's room followed by a barrage of questions, updates, and plans for the day. (Indeed, most illustrations of hospital teaching involve the attending physician towering over a bed-bound patient, surrounded by a small army of students and residents, all standing!) Hospital room setups, isolation precautions, and hygiene concerns may encourage standing, but taking a minute to sit at the patient's bedside can be especially impactful.
One study of postoperative rounding by a neurosurgeon found that, when the physician sat down during hospital rounds, patients felt the visit lasted longer and rated the visit more positively than when the physician remained standing for rounds, even though the time spent at bedside did not actually change in either scenario.4 Another study among 17 internists caring for patients on an inpatient general medicine service found that when the physician sat for rounds, the visit length did not change, but patients were more likely to feel that the physician explained things clearly and listened carefully.5 (See “SORT: Key recommendations for practice.”)
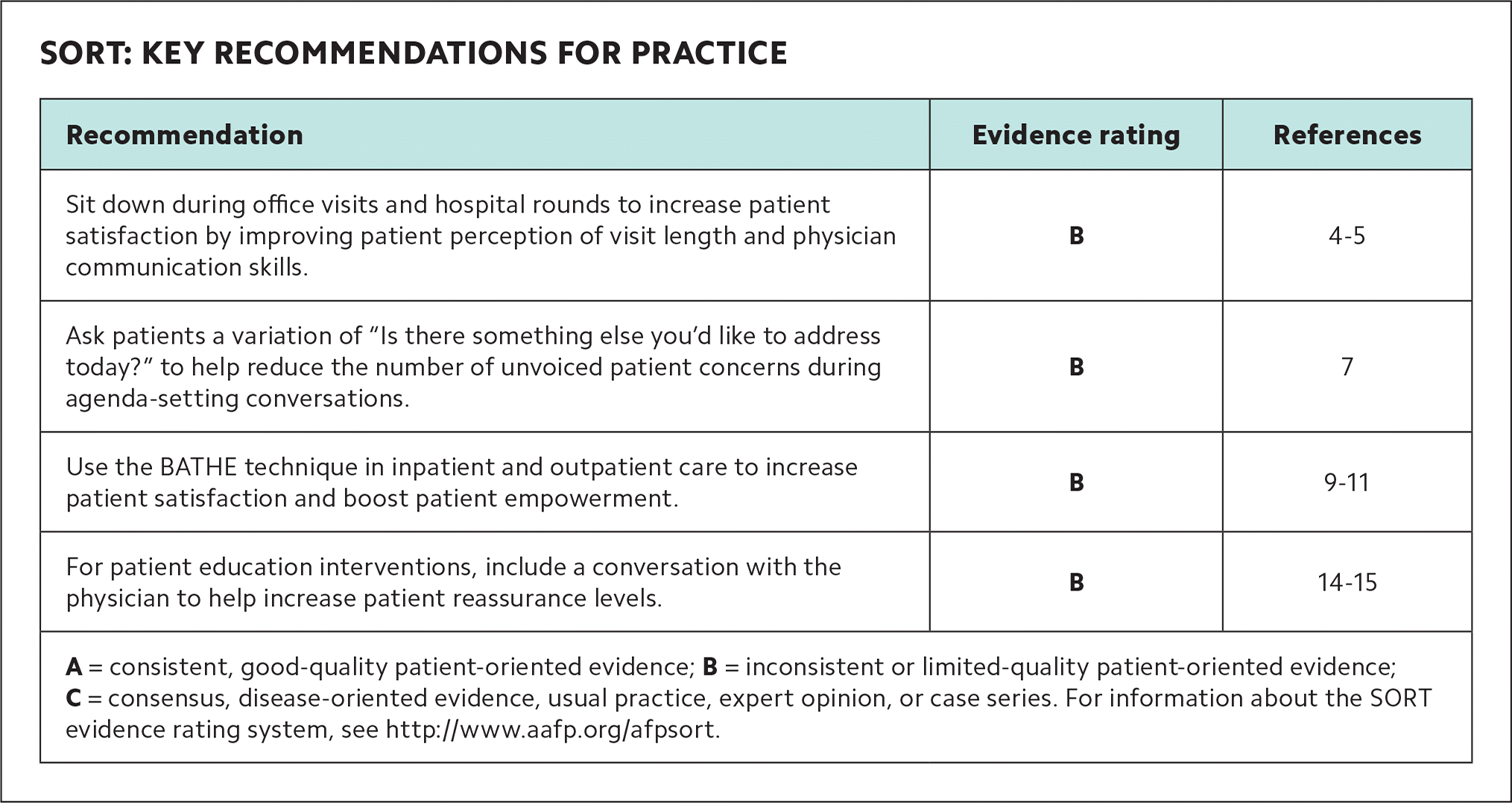
SORT: KEY RECOMMENDATIONS FOR PRACTICE
| Recommendation | Evidence rating | References |
|---|---|---|
| Sit down during office visits and hospital rounds to increase patient satisfaction by improving patient perception of visit length and physician communication skills. | B | 4–5 |
| Ask patients a variation of “Is there something else you'd like to address today?” to help reduce the number of unvoiced patient concerns during agenda-setting conversations. | B | 7 |
| Use the BATHE technique in inpatient and outpatient care to increase patient satisfaction and boost patient empowerment. | B | 9–11 |
| For patient education interventions, include a conversation with the physician to help increase patient reassurance levels. | B | 14–15 |
A = consistent, good-quality patient-oriented evidence; B = inconsistent or limited-quality patient-oriented evidence; C = consensus, disease-oriented evidence, usual practice, expert opinion, or case series. For information about the SORT evidence rating system, see http://www.aafp.org/afpsort.
2. EXPECT THERE TO BE MORE
When you're feeling pressed for time, it's natural to want to maintain some control over the office visit timeline and agenda. However, as noted above, attempting to direct or redirect the agenda can lead to unvoiced patient concerns and related problematic outcomes.
Instead, try to enter into agenda-setting conversations assuming that patients will have more to address than they are initially willing to voice.6 Evidence suggests that reflecting this mindset in how you phrase your agenda-setting questions can help patients open up. Consider it a medical version of the familiar “Would you like fries with that?” up-sell. As a physician, you're not setting out to influence patients' purchasing behaviors or encourage resource utilization, but with some simple changes to your language, you can help maximize each patient's chances of receiving the care they seek.
A group of researchers explored the linguistic polarity of the word “any” in agenda-setting questions (as in, “Is there anything else you would like to address today?”) versus the use of the word “some” (as in, “Is there something else you would like to address today?”). When physicians used “some” questions, there was a 78 percent reduction in the number of unmet patient concerns and no increase in visit length.7 So, the next time you are setting the agenda with a patient, try asking a variation of, “Is there something else you would like to address today?”
3. “BATHE” YOUR PATIENTS
The BATHE technique is a patient interview technique that consists of five components. Although BATHE was originally developed as a form of brief psychotherapy,8 the questions by their very nature provide a broader perspective of social concerns, stressors, and other life events with which a patient may be dealing. Evidence suggests that exploring these concerns, whether during inpatient rounds or during the day-to-day bustle of outpatient care, can both enhance understanding of a patient's life experience and improve patient satisfaction and empowerment.
One study of 20 consecutive outpatient visits for each of four family physicians in a shared practice found that use of the BATHE technique as a part of routine office care led to increased patient satisfaction, specifically by helping patients sense that their physician was sympathetic and concerned.9 Another study explored how adding the BATHE technique to primary care visits affected feelings of empowerment for patients with diabetes, as measured by their responses to the Diabetic Empowerment Scale. Among patients whose physician used the BATHE technique during visits, empowerment six months later was on average almost two times higher than among patients who received only standard care during their visits.10
In another study of 25 inpatients cared for by a family medicine residency service, 13 patients received the BATHE technique daily for five days or until discharge. The 12 patients in the control group received standard care. At exit, all participants completed a patient satisfaction survey. The inpatients who received the BATHE technique daily expressed higher overall satisfaction with their care, yet there was no significant difference between the groups regarding patient satisfaction with time spent during rounds.11
THE BATHE TECHNIQUE
BACKGROUND – “What is going on in your life?”
AFFECT – “How is it affecting you?”
TROUBLE – “What troubles you most about the situation?”
HANDLING – “How have you been handling this so far?”
EMPATHY – “That sounds very (scary, frustrating, sad, etc.)”
Editor’s note: For more information on this technique, consult the original source of the BATHE acronym: Stuart MR, Lieberman JA. The Fifteen Minute Hour: Efficient and Effective Patient-Centered Consultation Skills. 6th ed. Boca Raton, FL: CRC Press; 2018.
4. BE REASSURING
Physicians face the challenging task of easing patients' fears and concerns regarding their health. Often, in the face of diagnostic uncertainty, there exists a temptation to order an array of tests “just to be sure.” However, a narrative review of five randomized controlled trials (RCTs) failed to find any persistent reassurance effect from diagnostic testing.12 Another systematic review of 14 RCTs found that while diagnostic tests for symptoms with a low risk of serious illness may reduce future primary care visits, they do little to reduce patient anxiety, resolve symptoms, or provide reassurance.13
So, what is the best way to help patients sort through the meaning and implications of uncertainty surrounding their health? Evidence suggests that, for patients, having a direct conversation with a physician provides more reassurance than other forms of patient education or test results alone.
A study of 92 patients undergoing stress testing for evaluation of chest pain found that patients who received a pamphlet and had a brief discussion with their physician about the meaning of normal test results reported higher levels of reassurance than patients who only received a pamphlet or standard pre-test information.14 Similarly, a systematic review and meta-analysis of 14 RCTs and nonrandomized clinical trials examined whether patient education in primary care increases reassurance in patients with low-back pain. Patients who received written or verbal patient education reported higher levels of reassurance than patients who received standard care.15 In addition, that education was found to be significantly more effective when delivered by a physician, rather than another member of the health care team.15
It is also important to share with patients when we are certain and when we are not, and to frame our uncertainty the right way. A study with 71 parents using experimental vignettes of visits for pediatric care found parents had greater trust in the physician if diagnostic uncertainty was framed implicitly in terms of the breadth of the differential diagnosis or the most “likely” diagnoses, rather than in terms of explicit statements about being “not sure” of the diagnosis.16 Timely follow-up with results and discussion of the next steps are essential for maintaining a healthy and productive physician-patient relationship.
SIMPLE STEPS
When it comes to medical care, patients seek relationships with physicians that are characterized by trust, caring, expertise, and the right amount of autonomy.17 To promote each of these elements, it is vital to focus on excellence in clinical communication, just as you focus on excellence in medical care. By incorporating one or more of these evidence-based communication strategies, you can help bolster your relationship with your patients and improve their satisfaction with care.

