
Adding a touch of tech, a dose of education, and plenty of creature comforts to your waiting room can make it more palatable for patients.
Fam Pract Manag. 2020;27(1):14-18
Author disclosures: no relevant financial affiliations disclosed.

Waiting rooms play an important role in controlling the ebb and flow of clinical care in most medical practices. The average U.S. resident will visit an office-based physician two to three times per year, according to the Centers for Disease Control and Prevention (CDC),1 and wait an average of 18 minutes each visit.2 So it’s not surprising that the look, feel, and function of waiting areas contribute significantly to the overall patient experience.3,4 In this article we explain how to create a well-kept waiting room that increases patient satisfaction.
KEY POINTS
A clean, well-appointed waiting room makes a positive first impression on patients and builds trust and confidence.
Providing educational brochures and videos in the waiting room, along with information about resources for low-income families, can be helpful for patients.
Technology upgrades can allow patients to check themselves in, enter their own medical history electronically, and even leave the clinic and get alerts about when it’s time to return for their exam.
CREATING A COMFORTABLE AND FUNCTIONAL SPACE
Simple things like cleanliness, updated furniture, interesting decor, plants (real or artificial), and pleasing colors can contribute to the warmth and comfort of a waiting room. Each clinic will develop its own style, but there are some universal factors that make any space more functional.
Layout. An open layout with multiple seating options easily viewed at a glance can help patients select a seat based on their own preferences. For example, if there is a TV in the room, patients may wish to select the seat that will provide the best view of it, or the seat farthest from it if they don’t want to be distracted. Patients may select a seat where there are other people to chat with, or where they will have the most privacy. Waiting rooms should have enough chairs to seat not only all the patients who are usually there at peak times but also additional people who may accompany them, such as spouses, parents, or children.
There should be enough legroom in front of each chair to allow people to stretch while others pass by. This spacing also improves accessibility for those who use a wheelchair or walker. The layout should allow patients in wheelchairs to be able to sit without having to move chairs out of the way.
Seating. Chairs should have a comfortable amount of padding with a surface that is durable and easy to clean, and they should be large enough to accommodate a range of body types. Armrests improve comfort and help patients retain personal space even when the waiting room is crowded. They can also be critical for geriatric patients or patients with orthopedic issues who need armrests to lower themselves into chairs gently and push themselves upright.
Lighting. Waiting room lighting should be adequate for patients to easily read and complete paperwork. Avoid fluorescent lighting, which can be harsh and uncomfortable for patients with conditions like migraines and photophobia. Instead, choose lamps and decorative lights that create a friendly ambience. LED lighting can also be desirable, because it does not flicker or hum. Allow natural light into the waiting room if possible. Natural light and a view of the outdoors can be calming. Just keep in mind that shades may need to be closed at certain points in the day.
Ambience. Displaying works by local artists supports the community while creating a stimulating, visually rich environment. If there are offices next to the waiting room, a white noise machine can help mask conversations and preserve privacy.
WELCOMING PATIENTS AND CHECKING THEM IN
All patients should be greeted warmly when they enter the office. An indifferent or distracted greeting may give them the impression that they are “just another patient.”
Some clinics are adding technology like electronic self-serve check-in kiosks to their waiting rooms. There are many advantages to this. The kiosks can expedite check-in and cut down on wait times by providing copayment collection, language translation, and consent forms. Having patients update their medical history electronically saves staff time and often results in a more comprehensive note. Kiosks or electronic tablets can also be used to update personal information such as phone numbers or insurance coverage or engage in patient education. Patients are becoming more comfortable with self-serve kiosks as they become increasingly prevalent at other businesses such as airports, hotels, banks, and movie theaters. But there should always be a human available to help patients who need it.
Some offices have begun using a waiting room liaison or concierge to fill this role and others. This can be an existing staff member or someone hired specifically for the job. A liaison or concierge is responsible for ensuring patients are greeted warmly, answering any questions they may have, and other duties (see “Waiting room liaison responsibilities”).
WAITING ROOM LIAISON RESPONSIBILITIES
Greet patients.
Help patients complete paperwork (update personal, contact, and insurance information).
Keep waiting room organized (remove trash and arrange chairs and reading material).
Assist patients with tablets, kiosks, or other technology, if necessary.
Assist patients who have mobility issues or other disabilities, if necessary.
Your LGBTQ patients’ initial impression of your office may affect how comfortable they feel about disclosing information about their sexual orientation and gender identity. Staff members should be trained in diversity awareness to ensure that all patients feel valued and accepted. Using precise language that bears in mind the difference between “gender” and “sex” is important, as is using patients’ preferred gender-related pronouns, if known. Having at least one gender-neutral bathroom (or all gender-neutral bathrooms), displaying posters with diverse couples, and offering brochures addressing LGBTQ health concerns are other ways to make LGBTQ patients feel more welcome. Another change physicians can make is to modify medical history and other intake forms typically completed in the waiting room. Including a diversity of sexual orientations and gender identities in this paperwork will indicate that the physician is knowledgeable about LGBTQ patients’ concerns and open to discussing them.
Clinics should also take steps to ensure patients with limited English proficiency feel welcome. Cards or posters that help patients tell office staff which languages they speak are available at https://www.lep.gov/resources/resources.html. Of course, it’s also essential to select competent interpretation services and post the language services available in the waiting room, as well as develop a plan to respond to phone calls or written messages from patients with limited English proficiency.
FOSTERING HYGIENE AND HEALTH EDUCATION
The reception area should be clean and organized to reflect well on the practice. Someone from the office staff should check on the waiting room periodically to ensure patients are attended to and things are in order. Magazines should be reorganized periodically, and dirty coffee cups and other debris should be removed. Bathrooms should be checked regularly to make sure they are orderly, clean, and well-stocked. Drinking water should be accessible, and keeping food or drink with sugar in the office is a good idea too, in preparation for hypoglycemic episodes.
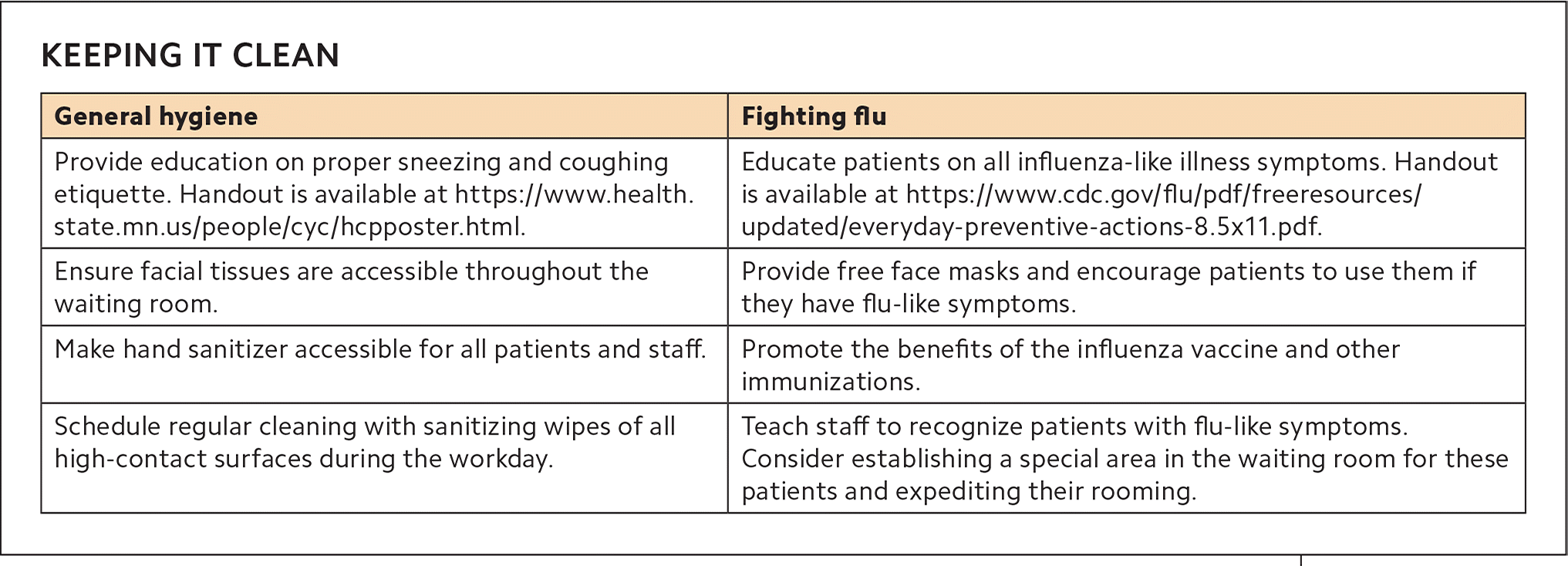
Because patients arrive at medical offices both well and sick, it is important to encourage proper hygiene in a waiting room. The CDC and some state health departments have handouts available online that can help educate patients on how to prevent the spread of disease (see “Keeping it clean”). These materials can be placed at the clinic entry points or sent to patients via email or text message before their visit.
Health education in the waiting room has an impact and has been linked to increased patient satisfaction.5 Educational posters and brochures throughout the office, including the waiting room and exam rooms, can be helpful to patients but should be screened for readability and accuracy. Educational videos can also be a source of actionable takeaways.6 Tablets preloaded with videos tailored to specific conditions can help patients with those conditions know what to ask the physician during the exam, or may even answer their questions before the exam.7
Posters and other materials from pharmaceutical companies or other vendors can give the wrong impression about a physician’s relationship with the companies, so you may want to avoid them. But exceptions can be made if the materials are evidence-based and reinforce critical and focused clinical messages.
Some clinics also provide brochures and other information about local resources and programs for low-income families. That can make the clinic feel more welcoming to those families and help them address socioeconomic issues that affect their health.8
KEEPING IT CLEAN
| General hygiene | Fighting flu |
|---|---|
| Provide education on proper sneezing and coughing etiquette. Handout is available. | Educate patients on all influenza-like illness symptoms. Handout is available. |
| Ensure facial tissues are accessible throughout the waiting room. | Provide free face masks and encourage patients to use them if they have flu-like symptoms. |
| Make hand sanitizer accessible for all patients and staff. | Promote the benefits of the influenza vaccine and other immunizations. |
| Schedule regular cleaning with sanitizing wipes of all high-contact surfaces during the workday. | Teach staff to recognize patients with flu-like symptoms. Consider establishing a special area in the waiting room for these patients and expediting their rooming. |
REDUCING BOREDOM
A physician’s schedule can be unpredictable, and sometimes a patient has to wait for an extended period. People are willing to wait about 20 minutes before becoming frustrated and feeling that time is being wasted.9 But perceived wait time is often more important than actual wait time. It is a good idea to occupy patients’ time with health screening questionnaires and other educational material, or at least give them that option. For longer waits, providing entertainment options can increase patient satisfaction by decreasing perceived wait times. Offering up-to-date reading materials featuring a wide array of topics helps. But many people now prefer to use their smart-phones to reduce boredom while waiting, so there is a growing expectation that offices have free Wi-Fi access. Patients often need to miss work for appointments, so providing a work area with multiple outlets for charging phones and laptops can also be helpful.
There is some debate over television in the waiting room. It can be entertaining, or at least distracting, but choosing programming is problematic. Political shows or news can be polarizing, and some people just aren’t interested in sports, soap operas, or daytime talk shows. Televisions or monitors are useful, however, for showing educational videos about common medical conditions.
Practices with large pediatric populations may want to dedicate a section of the waiting room to children. Age-appropriate reading materials, cartoons, and toys are mainstays in most waiting rooms. But in some offices these items are giving way to more high-tech options such as computer tablets, which can provide entertainment, education, and an interactive distraction. They can also be sanitized more easily than paper-based materials such as children’s books.
No matter how entertaining a waiting room is, some patients will probably prefer to wait for their appointment somewhere else. Smartphone and web applications such as Waitlist Me and Waitwhile allow patients to get updates on their wait times via text message and are available at varying costs (including free basic versions). Some busy restaurants use similar apps, which are especially helpful for walk-in patients whose wait times can be very difficult to predict. If the wait is long, patients are able to leave after checking in to complete errands, eat lunch, etc., and the app keeps them informed as their exam time approaches. Even without apps, patients appreciate knowing how long to expect to wait. They should be informed of any delays when they check in and given periodic updates.
The waiting room can be a place for making positive first impressions within a medical practice. A safe, clean, patient-centered waiting room fosters confidence and trust. Improving physical and environmental facets of the waiting room experience, including engaging patients with information about their own health, can increase the overall efficiency of the office while enhancing patient satisfaction.
