Simplified guidelines for coding and documenting evaluation and management office visits are coming next year. Learn how to apply the guidelines to some common visit types.
Editor's note: In its 2021 Medicare Physician Fee Schedule, CMS released new guidance regarding coding for prolonged E/M services. This article has been updated accordingly.

The American Medical Association (AMA) has established new coding and documentation guidelines for office visit/outpatient evaluation and management (E/M) services, effective Jan. 1, 2021. The changes are designed to simplify code selection and allow physicians to spend less time documenting and more time caring for patients. Physicians and other qualified health professionals (QHPs) will be able to select the level of office visit using either medical decision making (MDM) alone or total time (excluding staff time) on the date of service. In addition, the history and physical exam will be eliminated as components of code selection, and code 99201 will be deleted (code 99211 will not change). (See “E/M coding changes summary.”)
To follow up on the previous FPM article detailing these changes (see “Countdown to the E/M Coding Changes,” FPM, September/October 2020), we have applied the 2021 guidelines to some common types of family medicine visits, and we explain below how documentation using a typical SOAP (Subjective, Objective, Assessment, and Plan) note can support the chosen level of service.
In each vignette, we've arrived at a code based only on the documentation included in the note. It's possible that a more extensive note could support a higher level of service by further clarifying the physician's decision making. But we've analyzed each case through an auditor's lens and tried not to make any assumptions that aren't explicitly supported by the note.
KEY POINTS
- Starting in January, physicians and other qualified health professionals will be able to select the level of office visit using either medical decision making alone or total time (excluding staff time) on the date of service.
- Medical decision making is made up of three factors: problems addressed, data reviewed, and the patient's risk. The highest level reached by at least two out of three determines the overall level of the office visit.
- If the visit was time-consuming, but the medical decision making did not rise to a high level, the physician or qualified health professional may want to code based on total time instead.
E/M CODING CHANGES SUMMARY

| Year | Coding with medical decision making (MDM) | Coding with time | History and exam | ||
|---|---|---|---|---|---|
| 2020 | Number of diagnoses or management options | Amount and/or complexity of data to be reviewed | Risk of complications and/or morbidity or mortality | Typical time face-to-face; only when counseling and/or coordination of care dominate encounter | Key elements in selection of level of service |
| 2021 | Number and complexity of problem(s) addressed | Amount and/or complexity of data to be reviewed and analyzed | Risk of complications and/or morbidity or mortality | Total time (including non-face-to-face) on date of visit; can code any visit based on time | Only required as medically appropriate and not part of code level selection |
For more details on the new medical decision making guidelines, visit https://www.ama-assn.org/system/files/2019-06/cpt-revised-mdm-grid.pdf.
MEDICAL DECISION MAKING (MDM)
Starting in January, physicians will be able to select the level of visit using only medical decision making, with a revised MDM table. (See the table at https://www.ama-assn.org/system/files/2019-06/cpt-revised-mdm-grid.pdf.)
The four levels of MDM (straightforward, low, moderate, and high) will be maintained but will no longer be based on checkboxes or bullet points. The level of service will be determined by the number and complexity of problems addressed at the encounter, the amount and complexity of data reviewed and analyzed, and the patient's risk of complications and morbidity or mortality.
Here's what that looks like in practice:
STRAIGHTFORWARD MDM VIGNETTE
An established patient presents for evaluation of eye matting. The documentation is as follows:
Subjective: 16 y/o female presents with a 2-day history of bilateral eye irritation. She denies any fever or sick contacts. She started having a slight runny nose and cough this morning. She thinks the matting is a little better than yesterday. She wears daily disposable contacts but hasn't used them since her eyes have been bothering her. Her younger sibling has had similar symptoms for a few days.
Objective: Temperature 98.8, BP 105/60, P 58.
General: No distress. Does not appear ill.
HEENT: Mild bilateral conjunctival erythema without discharge. No tenderness over eye sockets. EOMI, PERRL.
Neck: No cervical lymph nodes palpated.
Lungs: Clear to auscultation.
Assessment: Viral conjunctivitis.
Plan: Reviewed likely viral nature of symptoms. Supportive and conservative treatment options reviewed, including eye cleaning instructions and contact lens precautions. Call the office if symptoms persist or worsen. Avoid use of contacts until symptoms resolve.
CPT code: 99212.
Explanation: Under the 2021 guidelines, straightforward MDM involves at least two of the following:
- Minimal number and complexity of problems addressed at the encounter,
- Minimal (in amount and complexity) or no data to be reviewed and analyzed,
- Minimal risk of morbidity from additional diagnostic testing or treatment.
This is the lowest level of MDM and the lowest level of service physicians are likely to report if they evaluate the patient themselves (code 99211 will still be available for visits of established patients that may not require the presence of a physician).
In this fairly common scenario, the assessment and plan make it clear that the physician addressed a single, self-limited problem (“minimal” in number and complexity, per the 2021 MDM guidelines) for which no additional data was needed or ordered, and which involved minimal risk of morbidity.
Per the 2021 CPT guidelines, “For the purposes of medical decision making, level of risk is based upon consequences of the problem(s) addressed at the encounter when appropriately treated.” In this case, there is little risk of morbidity to this patient from the viral infection diagnosed by the physician.
It's possible the physician considered prescribing an antibiotic in this case, but decided against it. Options considered but not selected can be used as an element for “risk of complications,” but they should be appropriate and documented. There is no documentation in this note to indicate the physician made that decision. The documentation provided, therefore, does not support a higher level of service using MDM. But if the physician did make that decision and the ensuing conversation with the patient was time-consuming, the physician always retains the option to choose the level of service based on time instead.
LOW LEVEL OF MDM VIGNETTE
An established patient presents for follow-up for stable fatty liver. The documentation is as follows:
Subjective: 62 y/o female presents for follow-up of nonalcoholic fatty liver. She has no other complaints today and no other chronic conditions. She denies any fever, weight gain, swelling, or skin color changes. She also denies any confusion. She continues to work at her regular job and reports no difficulties there. She denies any unusual bleeding or bruising. Energy is good. Diagnosis was made three years ago, incidentally, on an ultrasound. Condition has been stable since the initial full evaluation.
Objective: BP 124/70, P 76, Temperature 98.7, BMI 26.
General: Well-appearing. Alert and oriented x 3.
Eyes: Sclera nonicteric.
Heart: Regular rate and rhythm; trace pretibial edema.
Lungs: Clear to auscultation.
Abdomen: Soft, nontender, no ascites, liver margin not palpable.
Skin: No bruising.
Labs reviewed and analyzed: CBC normal, CMP with elevated AST (62 IU/ml) and ALT (50 IU/ml), PT/PTT normal.
Last ultrasound was 3 years ago.
Assessment: Nonalcoholic steatohepatitis, stable.
Plan: LFTs continue to be improved since initial diagnosis and 30-pound intentional weight reduction. Continue monitoring appropriate labs at 6-month intervals. Follow up in 6 months, or sooner if swelling, bruising, or confusion. Avoid alcohol. Continue weight maintenance. She is reassured her condition is stable and has no other questions or concerns, especially in light of her prior extensive education on the topic. I am arranging for hepatitis A and B vaccination. Discussed OTC medications, including vitamin E, and for now will avoid them.
CPT code: 99213
Explanation: Under the 2021 guidelines, low-level MDM involves at least two of the following:
- Low number and complexity of problems addressed at the encounter,
- Limited amount and/or complexity of data to be reviewed and analyzed,
- Low risk of morbidity from additional diagnostic testing or treatment.
In this vignette, the patient has one stable chronic illness, which is an example of an encounter for problems low in number and complexity. The risk of complications from treatment is also low. The “Objective” section indicates review of three lab tests, which qualifies as a moderate amount and/or complexity of data reviewed and analyzed. However, the level of MDM requires meeting two of the three bullets above, so the overall level remains low for this vignette.
MODERATE LEVEL OF MDM VIGNETTE
An established patient with obesity and diabetes presents with new onset right lower quadrant pain. The documentation is as follows:
Subjective: 42 y/o female presents for evaluation of 2 days of abdominal pain. She has a history of Type 2 diabetes, controlled. Pain is moderate, 6/10 currently, and 10/10 at worst. The pain is intermittent. The pain is located in the back and right lower quadrant, mostly. She denies diarrhea or vomiting but does note some nausea. She denies fever. She denies painful or frequent urination. She is sexually active with her spouse. She has had a hysterectomy due to severe dysfunctional bleeding. She has not tried any medication for relief. No position seems to affect her pain. She has not had symptoms like this before. Home glucose checks have been in the 140s fasting. Her last A1C was 6.9% two months ago. Family history: Sister with a history of kidney stones.
Objective: BP 160/95, P 110, BMI 36.1.
General: Appears to be in mild to moderate pain. Frequently repositioning on exam table.
HEENT: Moist oral mucosa.
Abdomen: Mild right-sided tenderness. No focal or rebound tenderness. Normal bowel sounds. No CVA tenderness. No suprapubic tenderness. No guarding.
UA with microscopy: 3 + blood, no LE, 50–100 RBCs, 5–10 WBCs.
CBC, CMP, CT stone study ordered stat.
Assessment: Abdominal pain – suspect renal stone. Also consider cholecystitis, gastroparesis, gastroenteritis, appendicitis, and early small bowel obstruction.
Diabetes, type 2, controlled.
Obesity – this is a risk factor for gall-bladder problems, but still favor renal stone.
Plan: Ketorolac 60 mg given in office for pain relief. Hydrocodone/APAP prescription for pain relief. Discussed at length suspicion of renal stone. Will plan lab work and pain control and await CT stone study. Urine sent to reference lab for microscopy. Drink plenty of fluids. Urine strainer provided. Call the office if worsening or persistent symptoms. Await labs/CT for next steps of treatment plan. Will follow up with her if urology referral is indicated.
CPT code: 99214
Explanation: Under the 2021 guidelines, moderate level MDM involves at least two of the following:
- Moderate number and complexity of problems addressed at the encounter,
- Moderate amount and/or complexity of data to be reviewed and analyzed,
- Moderate risk of morbidity from additional diagnostic testing or treatment.
In this vignette, the patient has one undiagnosed new problem with uncertain prognosis (abdominal pain) and two stable chronic conditions (diabetes and obesity). Either one (the new problem with uncertain prognosis or two stable chronic conditions) meets the definition of a moderate number and complexity of problems under the 2021 MDM guidelines. But they do not meet the threshold of a high number and complexity of problems, even when combined.
The physician reviews or orders a total of four tests, which again exceeds the requirements for a moderate amount and/or complexity of data, but doesn't meet the requirements for the high category.
The prescription drug management is an example of moderate risk of morbidity. One might argue that the risk of morbidity is high because renal failure could result from a major kidney stone obstruction. But even then the overall MDM would still remain moderate, because of the number and complexity of problems addressed and the amount and/or complexity of data involved.
HIGH LEVEL OF MDM VIGNETTE
An established patient with a new lung mass and probable lung cancer presents with a desire to initiate hospice services and forgo curative treatment attempts. The documentation is as follows:
Subjective: 92-year-old male presents for follow-up of hemoptysis, fatigue, and weight loss, along with review of his recent chest CT. He reports moderate mid-back pain, new since last week. Appetite is fair. He denies fever. He continues to have occasional cough with mixed blood in the produced sputum.
Objective: BP 135/80, P 95, Weight down 5 pounds from 2 weeks ago, BMI 18.5, O2 sat 94% on RA.
General: Frail-appearing elderly male. No distress or shortness of breath. Able to speak in full sentences.
HEENT: No palpable lymph nodes.
Lungs: Frequent coughing and diffuse coarse breath sounds.
Heart: Regular rate and rhythm.
Ext: No extremity swelling.
MSK: Moderate tenderness over multiple thoracic vertebrae.
CT shows large right-sided lung mass suspicious for malignancy, along with a moderate left-sided effusion. Lytic lesions seen in T6-8.
Assessment: Lung mass, suspect malignancy with bone metastasis.
Plan: After extensive review of the findings, the patient was informed of the likely poor prognosis of the suspected lung cancer. We reviewed his living will, and he reiterated that he did not desire life-prolonging measures and would prefer to allow the disease to run its natural course. He also declines additional testing for diagnosis/prognosis. A shared decision was made to initiate hospice services. Specifically, we discussed need for oxygen and pain control. He declines pain medications for now, but will let us know. He and his son who was accompanying him voiced agreement and understanding of the plan.
CPT code: 99215
Explanation: Under the 2021 guidelines, high level MDM involves at least two of the following:
- High number and complexity of problems addressed at the encounter,
- Extensive amount and/or complexity of data to be reviewed and analyzed,
- High risk of morbidity from additional diagnostic testing or treatment.
In this vignette, the patient has one acute or chronic illness or injury (suspected lung cancer) that poses a threat to life or bodily function. This is an example of a high complexity problem in the 2021 MDM guidelines. The physician reviewed one test (CT), so the amount and/or complexity of data is minimal. A decision not to resuscitate, or to de-escalate care, because of poor prognosis is an example of high risk of morbidity, and the physician has clearly documented that in the plan portion of the note. Consequently, even though the amount and/or complexity of data is minimal, the overall MDM remains high because of the problem addressed and the risk involved.
TOTAL TIME
Under the new guidelines, total time means all time (face-to-face and non-face-to-face) the physician or other QHP personally spends on the visit on the date of service. Examples include time spent reviewing labs or reports, obtaining or reviewing history, ordering tests and medications, and documenting clinical information in the EHR.
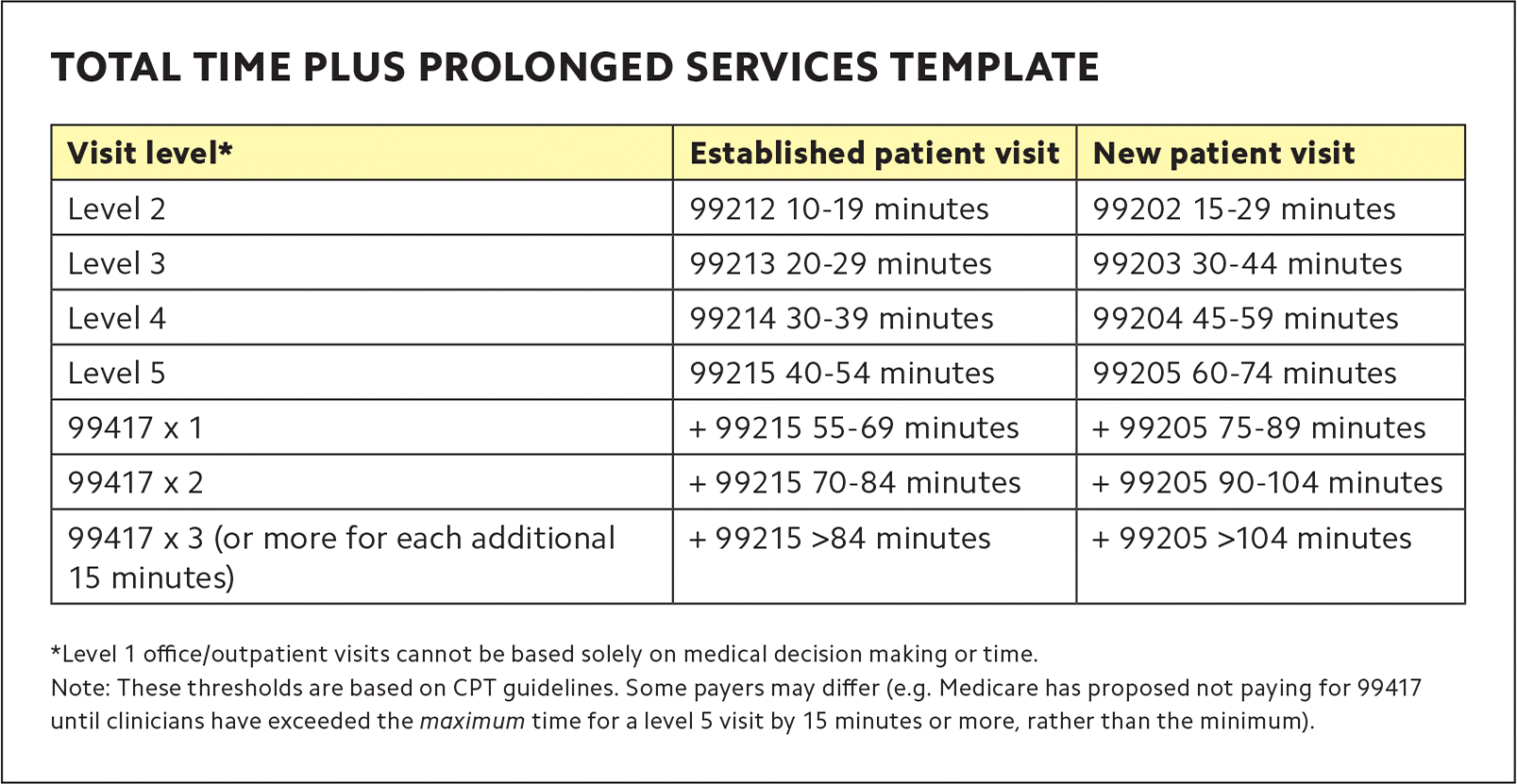
The AMA has also created a new add-on code, 99417, for prolonged services. It can be used when the total time exceeds that of a level 5 visit – 99205 or 99215. (See “Total time plus prolonged services template.”)
TOTAL TIME PLUS PROLONGED SERVICES TEMPLATE
| Visit level* | Established patient visit | New patient visit |
|---|---|---|
| Level 2 | 99212 10–19 minutes | 99202 15–29 minutes |
| Level 3 | 99213 20–29 minutes | 99203 30–44 minutes |
| Level 4 | 99214 30–39 minutes | 99204 45–59 minutes |
| Level 5 | 99215 40–54 minutes | 99205 60–74 minutes |
| 99417 x 1 | + 99215 55–69 minutes | + 99205 75–89 minutes |
| 99417 x 2 | + 99215 70–84 minutes | + 99205 90–104 minutes |
| 99417 x 3 (or more for each additional 15 minutes) | + 99215 >84 minutes | + 99205 >104 minutes |
Update: In the 2021 Medicare Physician Fee Schedule, CMS introduced prolonged services code G2212. In order to bill this code, clinicians must have exceeded the maximum time for a level 5 visit by 15 minutes or more (i.e., 69 minutes for an established patient and 89 minutes for a new patient) rather than the minimum as required by CPT for code 99417.
TIME-BASED CODING VIGNETTE
An established patient presents with a three-month history of fatigue, weight loss, and intermittent fever, and new diffuse adenopathy and splenomegaly. The documentation is as follows:
Subjective: 30-year-old healthy male with no significant PMH presents with a three-month history of fatigue, weight loss, and intermittent fever. He travels for work and has been evaluated in several urgent care centers and reassured that he likely had a viral syndrome. Fevers have been as high as 101, but usually around 100.5, typically in the afternoons. Testing for flu and acute mono has been negative. He denies high-risk sexual behavior and IV drug use. He denies any sick contacts. He has not had vomiting or diarrhea. He has not had any pain. He denies cough.
Objective: BP 125/80, P 92, BMI 27.4.
General: Well-nourished male, no distress.
HEENT: No abnormal findings.
Lungs: Clear.
Heart: No murmurs. Regular rate and rhythm.
Abdomen: Soft, non-tender, moderate splenomegaly.
Skin: Multiple petechia noted.
Lymph: Multiple cervical, axillary, and inguinal lymph nodes that are enlarged, mobile, and non-tender.
Assessment: Weight loss, lymphadenopathy, and splenomegaly
Plan: Prior to the visit, I spent 15 minutes reviewing the medical records related to his recent symptoms and various urgent care visits. We reviewed the differential at length to include infectious disease and acute myelodysplastic condition. I have ordered stat blood cultures, TB test, EBV titers, echo, and CBC. The pathologist called to report concerning findings on the CBC for likely acute leukemia. I called the patient to inform him of his results and need for additional testing. I also discussed the patient with oncology and arranged a follow-up visit for tomorrow. I spent a total of 92 minutes with record review, exam, and communication with the patient, communication with other providers, and documentation of this encounter.
CPT Codes: 99215 and 99417 x 3.
Explanation: In this instance, the physician has chosen to code based on time rather than MDM. The physician has documented 92 minutes associated with the visit on the date of service, including time not spent with the patient (e.g., time spent talking with the pathologist and time spent in documentation). According to the 2021 CPT code descriptors, 40–54 minutes of total time spent on the date of the encounter represents a 99215 for an established patient.
The 2021 CPT code set also notes that for services of 55 minutes or longer, you should use the prolonged services code, 99417, which can be reported for each 15 minutes beyond the minimum total time of the primary service (99215). The difference between the 92 minutes spent by the physician and the 40-minute minimum for 99215 is 52 minutes. There are three full 15-minute units of 99417 in those 52 minutes, so the physician may report three units of 99417 in addition to 99215. CPT 2021 instructs you to not report 99417 for any time unit less than 15 minutes, so the seven remaining minutes of prolonged service is unreportable.
Note that if this had been a new patient, the physician would only be able to report two units of 99417 in addition to 99205. Though the elements of MDM do not differ between new and established patients, the total time thresholds do. The range for a level 5 new patient is 60–74 minutes.
FINAL THOUGHTS
CPT does not dictate how physicians document their patient encounters. As illustrated above, a standard SOAP note can be used to support levels of MDM (and thus levels of service) under the 2021 guidelines.
Physicians who want to further solidify their documentation in case of an audit may choose to make the elements of MDM more explicit in their documentation. This could be particularly helpful for documenting the level of risk, which is the least clearly defined part of the MDM table and potentially most problematic because of its inherent subjectivity. Stating the level of risk and giving a rationale when possible allows a physician to articulate in the note the qualifying criteria for the submitted code. For example, going back to our vignette of moderate MDM, the physician could note in the chart, “This condition poses a threat to bodily function if not addressed, due to acute kidney injury for an obstructive stone.”
It is also worth noting that much of the note in each case is for purposes other than documenting the level of service. For instance, with history and physical exam no longer required, the subjective and objective portions of the note are recorded primarily for continuity or quality of care rather than to justify the level of service. This provides some administrative simplification. What's in the note will become more about what is needed for medical care and less about payment justification under the new guidelines. That's a plus for primary care.
We hope these examples are helpful as you prepare to implement the 2021 CPT changes. You can also visit https://www.aafp.org/emcoding for more resources and information.

