
Use this guide to up-front agenda setting to help you strike a balance between meeting complex patient needs and staying on time.
Fam Pract Manag. 2021;28(2):27-31
Author disclosures: no relevant financial affiliations disclosed. Note: No actual patient names have been used.

Mrs. Lister is a 74-year-old female who comes to you for an annual visit. She has a past medical history of Type 2 diabetes, coronary artery disease with a myocardial infarction and stent placement three years prior, hypertension, hyperlipidemia, obesity, and tobacco use. She obtained labs prior to the visit, which show an A1C of 8.9%, an increase from 8.1% six months prior. Her blood pressure is 148/91 mm Hg at today's visit, verified by repeat testing. The rooming staff informs you that a depression screen was positive — and then warns you, “Watch out! She has a list with her.”
This scenario is not unique. In family medicine, we often find ourselves with too little time to address a patient's multitude of medical concerns. The way we navigate this situation can determine whether we are timely and effective, or frustrated and late. Properly using time during a visit improves the care we give our patients and how they perceive that care.1 In situations like the one with Mrs. Lister, we want to stay on time, provide quality care, ensure that our patients feel cared for, and avoid getting burnt out in the process. We can accomplish this through effective agenda setting.
Effective agenda setting is a learned skill, and like any learned skill it takes practice to obtain mastery. When properly performed, agenda setting is rapid and unambiguous, and it facilitates clear communication of priorities between you and your patient. Here are some steps you can follow to become a master of agenda setting.
KEY POINTS
When presented with a list of concerns that are impossible to address adequately during a single visit, agenda setting can help balance patient needs and physician time constraints.
Like any learned skill, agenda setting takes practice. This article offers a simple framework and some sample language you can try using with patients.
The agenda-setting process includes eliciting all patient concerns at the start of a visit, estimating the time required, establishing priorities for the current visit, creating a plan for addressing remaining concerns at subsequent visits, and checking for understanding.
1: CREATE A COMPLETE LIST OF CONCERNS
The agenda-setting process allows you to create a plan for how time will be spent during a patient encounter. Although the agenda should be negotiated with the patient, ultimately you are responsible for finalizing it. The process of agenda setting begins by compiling a complete list of the items to be discussed.2,3 We call this the concern list, and it includes everything of interest to you or your patient.
You might start by jotting down your concerns as you review the patient's chart. Then, as you begin the visit, ask the patient about any health concerns.4 Try saying, “What health concerns would you like to make sure we talk about at some point?” This question allows you to communicate that, while everything the patient brings up may not be discussed at today's visit, you are willing to make sure the concerns are addressed either now or at some point in the future.
After you receive the initial response, prompt the patient again by asking, “What else?” Keep asking this until all concerns are written down.5 If the patient is accompanied, it may be appropriate to query the companions for their concerns too. By doing so, you may uncover essential information that could lead to important diagnoses, such as dementia or depression.
Patients often bring a list of items to discuss. This does not need to be a source of frustration. Try to view “the list” as a sign of patients who are engaged in their health care and motivated to achieve good health outcomes.
As you formulate the complete list of concerns, be explicit and precise. The list may be as short as one or two items that can easily be accomplished in a single visit. However, the list may be quite long, requiring multiple visits to fully address. Be clear about this with the patient.
If necessary, you might use an entire visit simply to generate the list of concerns and develop an appropriate plan for attending to each item on the list. This is especially true for annual wellness visits.
If you have an electronic health record (EHR), use it to your advantage. You can save time and improve overall documentation by adding each concern to the past medical history or as a diagnosis for the visit.6 If you do this during your discussion with the patient, you will have an electronic record of your concern list without having to transcribe it later.
Even with all of your preparation and questions, patients often wait until the end of the visit to raise important concerns. While there is no way to absolutely avoid this so-called “doorknob phenomenon,” effective agenda setting can help keep any last-minute concerns manageable.2
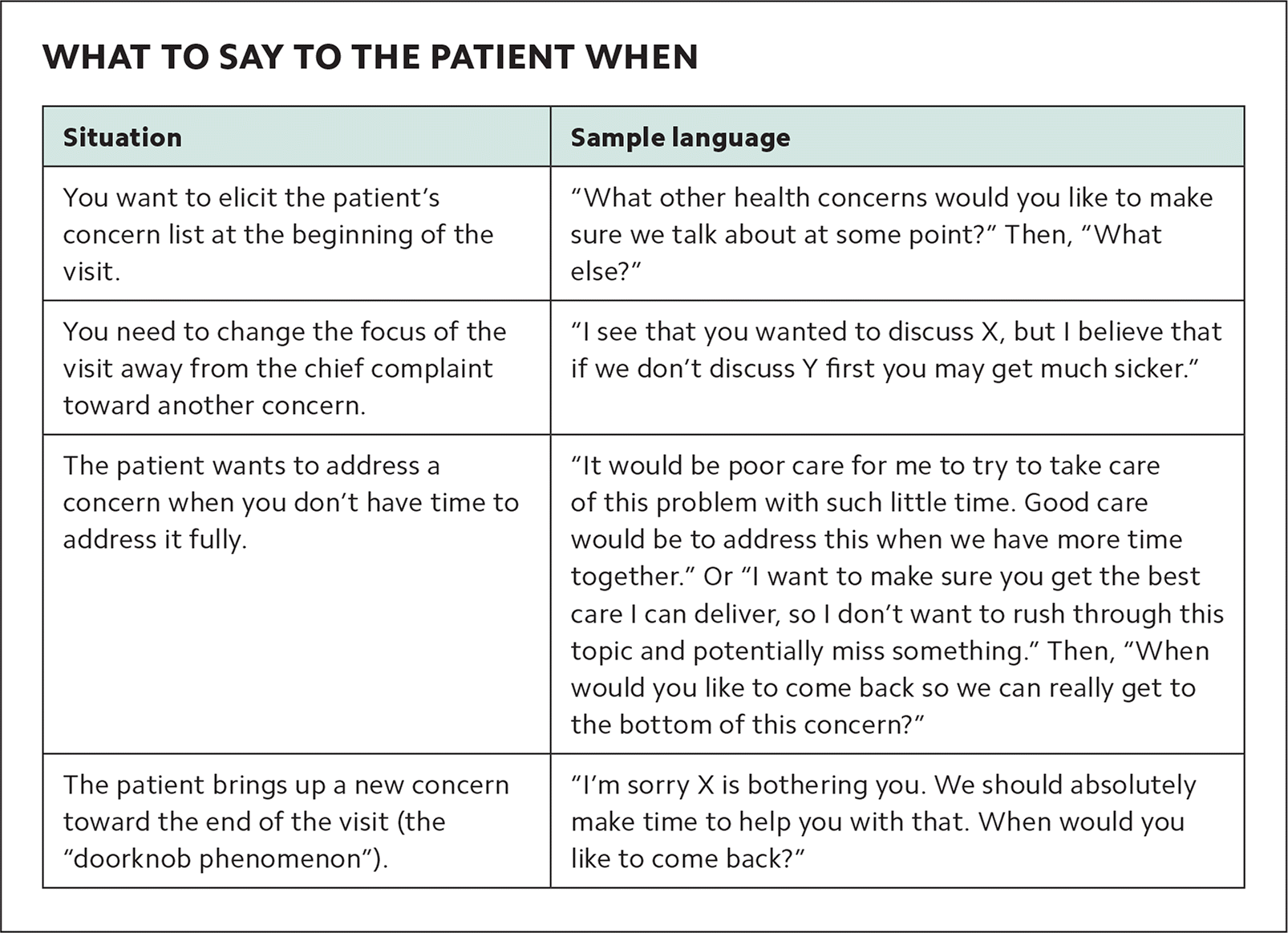
| Situation | Sample language |
|---|---|
| You want to elicit the patient's concern list at the beginning of the visit. | “What other health concerns would you like to make sure we talk about at some point?” Then, “What else?” |
| You need to change the focus of the visit away from the chief complaint toward another concern. | “I see that you wanted to discuss X, but I believe that if we don't discuss Y first you may get much sicker.” |
| The patient wants to address a concern when you don't have time to address it fully. | “It would be poor care for me to try to take care of this problem with such little time. Good care would be to address this when we have more time together.” Or “I want to make sure you get the best care I can deliver, so I don't want to rush through this topic and potentially miss something.” Then, “When would you like to come back so we can really get to the bottom of this concern?” |
| The patient brings up a new concern toward the end of the visit (the “doorknob phenomenon”). | “I'm sorry X is bothering you. We should absolutely make time to help you with that. When would you like to come back?” |
2: ESTIMATE TIME REQUIREMENTS
For each item on the concern list, quickly ask yourself: How much time will it take for me to really take care of this problem? Consider not only the time for history and exam, but also how much time you will need to review old records, communicate with specialists, enter orders into the EHR, or perform ancillary tests.
If you're not entirely sure how much time is needed, it's best to give yourself too much time. If you underestimate the time needed, you likely won't be able to give the condition the attention it deserves or will fall behind — or both. But if you overestimate the time needed, you may be able to address additional concerns during the visit or use the extra few moments to catch up on other tasks.
Once you've quickly estimated how much time you need, be realistic about how much time you have during your current visit to accomplish these tasks. If each concern requires a significant amount of time, some concerns may need to be prioritized and others addressed during subsequent visits.
3: PRIORITIZE THE LIST
If you don't have enough time to address everything on the patient's list during the current visit, take a few moments to identify which items you need to address first.3 There is no standard method for prioritizing the list of concerns. Just make sure you are focusing on what will most benefit the patient.
Concerns that are time sensitive or represent potentially life-threatening pathology take precedence. This may mean you do not have time to address the patient's primary concern. If this happens, explain to the patient why you feel it is important to focus on the other concern first. Try saying, “I see that you wanted to discuss X, but I believe that if we don't discuss Y first you may get much sicker.”
If you have additional time during the visit, next prioritize issues that are of greatest concern to the patient,7 even if it means prioritizing conditions that seem less consequential to you. With Mrs. Lister, for example, you may be concerned about her worsening diabetes, hypertension, tobacco use, and depression, but she is very worried about a lingering dry cough she has had since recovering from a mild viral illness the week prior. By prioritizing the evaluation of the cough, you communicate that her suffering matters to you. Frequently there is an opportunity to link the patient's concern to chronic disease management, such as tobacco cessation in Mrs. Lister's case.
Finally, items that take only a little time to address can be given priority. Mrs. Lister's depression may be of more concern than her mildly uncontrolled hypertension, but management of the hypertension may be as simple as telling her to take two lisinopril tablets daily instead of one, followed by a reassessment in the future.
Before you proceed with the encounter, review the prioritized list with the patient. Explain which concerns you think you are able to cover during the current visit and which ones you will need to address at a subsequent visit.
Patients frequently expect answers to all of their health concerns in a single visit, and unmet expectations can lead to dissatisfaction with the encounter. Good communication becomes critical to helping the patient reorient their expectations.7 If the patient needs more explanation about why you cannot address a certain concern during the current visit, one strategy is to say to the patient, “It would be poor care for me to try to take care of this problem with such little time. Good care would be to address this when we have more time together.”8 You can then ask, “When would you like to come back so we can really get to the bottom of this concern?” This leads us to the next step.
4: PLAN FOLLOW-UP VISITS
When you don't have time to address every item on the concern list, make plans to follow up. Plan enough time to address the concerns appropriately, and inform the patient about your expectations. This may require a single follow-up visit, multiple short visits, or a few longer visits, depending on the patient's needs and your practice environment.
It may help to invest some time at the current visit to do a brief evaluation of some of the concerns you plan to address in a future visit. This brief evaluation should be sufficient to help you determine whether any testing is warranted at the current visit, even though your full evaluation will need to be deferred until later. Doing so can save time for you and the patient. For example, if a patient complains of incontinence, you could go ahead and order a urinalysis to review during the subsequent visit.
5: CHECK FOR UNDERSTANDING
At the end of the visit, review what you have accomplished. Have the patient “teach back” to you what they have learned at the visit, what instructions they were given, and what the plan is for future visits.9 This helps the patient understand the value of the encounter, and it helps you discern whether the patient truly comprehends what was covered at the visit. Also, restate what you hope to accomplish during future visits. This can help the patient realize the importance of following through with their appointments.
TIPS TO KEEP IN MIND
While you practice these steps, there are some important things to keep in mind.
First, use your staff to help improve the patient's experience. The communication your schedulers, receptionists, assistants, and nurses provide to the patient during scheduling, check-in, and rooming should support your work and help the patient have realistic expectations about the visit agenda.
Next, remember that if you do have time to address unplanned concerns during the visit, it is often in the patient's best interest that you do so. It can help your patient avoid extra time, hassles, and costs, and providing timely care can improve quality.
Finally, remember that your best care takes time. When you rush through an evaluation, you're probably not providing your best care. If patients seem dissatisfied because not all of their concerns were addressed during a single visit, remind them that you won't accept any care for them other than your best care.
AGENDA SETTING IN ACTION
We return to our patient, Mrs. Lister, and her long list of things that she was hoping to address today. You look it over and see that it contains several concerns — too many to undertake now — and you ask what is the most important to her. She mentions her chronic shoulder pain. You make a list including her complaints, as well as her chronic medical problems. You prioritize the list to address Mrs. Lister's most pressing concern, as well as what you believe needs to be addressed first from a medical standpoint today. You explain to Mrs. Lister what you hope to accomplish today and tell her that you can definitely get to all the items on the list during future visits. Noticing that her blood pressure is elevated, you quickly adjust her medications. At the end of the conversation, she is able to teach back everything you have discussed. You plan for future follow-up visits to address the other items on her list.
You close the visit and are just getting up to leave the room when she says, “I forgot to mention that I've had problems with my feet for years. What can I do about that?” You respond by saying, “I'm sorry your feet are bothering you. We should absolutely make time to help you with that. When would you like to come back?” This shows Mrs. Lister that her concern is important, and you are not ambiguous about when you will evaluate and address it.
Effective agenda setting is a key factor in ensuring timely, quality care for patients like Mrs. Lister. Just as important, it helps you feel good about your day and stay on schedule. Your patients will appreciate the clear communication, and you will appreciate having time to give the quality care you were trained to provide.
