
Interest in home-based primary care is growing as payments increase, technology improves, and the population ages.
Fam Pract Manag. 2021;28(3):22A-22G
Author disclosures: no relevant financial affiliations disclosed.

The United States is experiencing a resurgence of home-based primary care (HBPC) after a rapid decline during the last century. Steady growth in physician house calls started with the doubling of house call payment rates in 1998 and a doubling and tripling of domiciliary payment rates in 2006. Other factors include the aging of our society; increased technology that allows X-rays, ultrasounds, electrocardiograms, and lab tests to be done in the home; and new CPT payments that target complex patients such as those who need chronic care management, remote patient monitoring, and advance care planning.
HBPC's value has been demonstrated through improved outcomes and reduced costs for complex patients. Medicare's Independence at Home house call program improved outcomes and decreased costs by $2,000 per patient per year, and the U.S. Department of Veterans Affairs' HBPC program reduced hospital days by 60%, readmissions by 21%, and nursing home use by an astounding 89%.1 The data generated support for HBPC on Capitol Hill, at the Centers for Medicare & Medicaid Services (CMS), from Medicare Advantage plans, and from investors.
More recently, the COVID-19 public health emergency (PHE) brought virtual care into patients' homes in a remarkable way. But telehealth is beyond the scope of this article. Currently, Congressional action is needed to enable telehealth to continue in the home after the PHE.
Still, family physicians can take advantage of the growing support for HBPC. This article outlines steps for adding house calls to an office-based practice. Reasons to do so include the following:
Continuity of care for patients who have difficulty getting to the office, ensuring they are not lost in the system.
Better quality of care, increased time with patients, and improved doctor-patient-caregiver relationships, resulting in increased patient satisfaction scores, increased referrals from family members, increased physician satisfaction, and decreased burnout.
Improved end-of-life care, fulfilling the wishes of the majority of patients who desire to be at home surrounded by loved ones at the time of death.
Improved value-based care performance from superior risk capture, reducing gaps in care, improving quality, and lowering the total cost of care.
Increased reimbursement for complex patient care.
KEY POINTS
Increased payment, improved technology, and the aging of the population have all contributed to steady growth in physician house calls.
House calls have been shown to improve patient outcomes and decrease costs by $2,000 per patient per year.
When adding house calls to an office-based practice, three ingredients necessary to success are patients, processes, and payments.
THREE INGREDIENTS FOR SUCCESS
A successful house call program requires three ingredients: patients, processes, and payments.
Patients. There is some flexibility in choosing which patients should receive home visits. Medicare has never required house call patients to meet the homebound definition that it requires for receiving skilled nursing and therapy services in the home. But until January 2019, Medicare required additional documentation of medical necessity for every home visit, describing why a house call was needed in “lieu of an office visit.” The 2019 Medicare Physician Fee Schedule Final Rule removed this requirement as of Jan. 1, 2019.
Still, most house call programs focus on complex patients who have difficulty getting to the office. Some practices use data analytics to identify and target high-risk patients. Common candidates for HBPC include the following:
Frail older adults with multiple (often five or more) chronic conditions and deficiencies in activities of daily living (ADL).
Younger homebound patients, usually with one principal neuromuscular condition such as multiple sclerosis, amyotrophic lateral sclerosis, or cervical spine injuries (some on ventilators).
Patients with high-risk diagnoses like congestive heart failure and chronic obstructive pulmonary disease.
Patients with high hospital and emergency department (ED) utilization in the past six to 12 months.
Patients with hierarchical condition category (HCC) scores greater than 2.0.
Another group well-suited for HBPC is post-acute, transitional care management (TCM) patients. During the high-risk transition period, these patients benefit from a short course of HBPC that reduces complications and readmissions. Payments for TCM (CPT codes 99495 and 99496) have increased more than 20% over the past two years. CMS has also unbundled virtually all care management services that previously were not billable within the 30-day TCM period. These include chronic care management, care plan oversight for home health and hospice services, face-to-face and non-face-to-face prolonged services, and more when reasonable and necessary. Numerous hospitals are partnering with HBPC programs to reduce their readmission rates.
Logistical considerations for choosing house call patients include the following:
Geography: A geographic radius should be determined for home visits based on driving time (e.g., no more than 20 minutes from the physician's office or home). Telehealth, at least while it is allowed under the PHE, is an excellent way to provide care for more distant patients.
Established vs. new house call patients: Some practices may decide to limit house calls to established patients. But if you desire to grow a house call practice, the largest referral source tends to be home health agencies, followed by hospital and rehabilitation discharge planners, social services, and word of mouth.
Place of service: Practices may offer house calls to patients at home or in domiciliary settings (e.g., assisted living facilities or group homes). There are economies of scale in domiciliary care because you can see multiple patients in the same location on the same day, and the payments are roughly the same as home visits.
Capacity: A good way to start is with a half day or one full day of house calls per week, and then increase that time as volume demands.
Operational processes. Practices will need to address operational issues such as scheduling, visit preparation, staffing, supply management, and safety.
Efficient scheduling is critical to reduce travel time, and can be achieved through the following steps:
Schedule patients in close proximity. This is facilitated by assigning days to specific geographic areas and using mapping/routing software.
Map and route patients one to two days before the visit, notify patients or caregivers of the approximate visit time (usually providing a two- to four-hour window or simply indicating morning or afternoon), and verify the address (sometimes the address on file is for mailing the bill and is not the patient's physical location).
Use electronic health record flags/alerts for travel notes, communication preferences, and patient preferences. Special visit instructions should be noted on the schedule (e.g., “call daughter ahead,” “go in back door,” or “dogs need to be secured”).
Call when en route to the visit so the patient is ready and has medication out.
Give patients follow-up timeframes (e.g., four to six weeks or two to three months) instead of exact dates to allow the schedule to be fluid, to facilitate scheduling patients within the same geographic area, and to enable last-minute schedule changes based on patient acuity.
Make sure that clerical tasks are done before the visit, including obtaining signed forms and medical records (e.g., HIPAA forms, consent for treatment, or medical history forms) when possible.
Staffing considerations include the following:
Medical assistant (MA) support: Many physicians choose to do house calls solo, mainly because of the cost of including an MA. But having an MA route and drive saves the physician significant time and allows charting and phone calls while in transit. During the house call, the MA can check vitals, do immunizations, draw blood, assist with medication reconciliation and refills, get forms signed, review gaps in care, do assessments (such as PHQ-2/9, Mini-Cog, nutritional, and safety surveys), assist with wound care, help with orders (e.g., durable medical equipment, home health, and hospice), and increase safety. Making one extra house call a day covers the MA's cost, and the time savings more than allow for that one extra call.
Advanced practice provider visits: Nurse practitioner and physician assistant house calls have dramatically increased over the past decade; they are now the largest provider group making house calls. This is a cost-effective model with good outcomes, when provided with physician support.
Supply management involves keeping track of what supplies are used and restocking at the end of the day. Unlike in the office, you cannot walk down the hall to a storage closet if you run out of something during a home visit. Ensure equipment is sanitized and charged. Have a container in the car for standard supplies that are not damaged by temperature extremes (e.g., wound care items). Review schedules in advance to identify any special supply needs (e.g., a cooler for storing and transporting drawn labs).
Safety concerns include higher crime areas and homes with potentially dangerous patients, caregivers, or pets. Safety and emergency plans should include the following:
Handling car accidents and other incidents such as falls with injuries, needle-sticks, etc.
Handling pets in the home. Some HBPC programs require pets be caged during visits. Others leave it to the discretion of the pet owner and the physician.
Sitting on a hard surface chair to avoid unseen soiling, bedbugs, etc.
Washing or sanitizing hands before, during, and after the visit.
Noting safety issues on the schedule, including a history of multi-resistant organisms, bed bugs, or firearms (which should always be locked). During the PHE, conduct COVID-19 screening questions when notifying the patient of the appointment time and again when en route to the patient's home.
Seeing patients in higher crime areas during daylight hours. There is debate among HBPC clinicians about wearing clothing that identifies them as health care workers, such as a lab jacket. Some think it's better to avoid drawing attention to themselves. Others believe it is good for people to know they are there to provide care. Determine which is more comfortable for you.
Turning on smartphone location service apps, which enable the office to know the physician's location and allow the physician to quickly call in an emergency through a simple touch or verbal command.
Planning for inclement weather or natural disasters. Patients may need to be rescheduled.
Exiting the premises if the physician feels unsafe. Consider having a code word to alert staff if you need assistance.
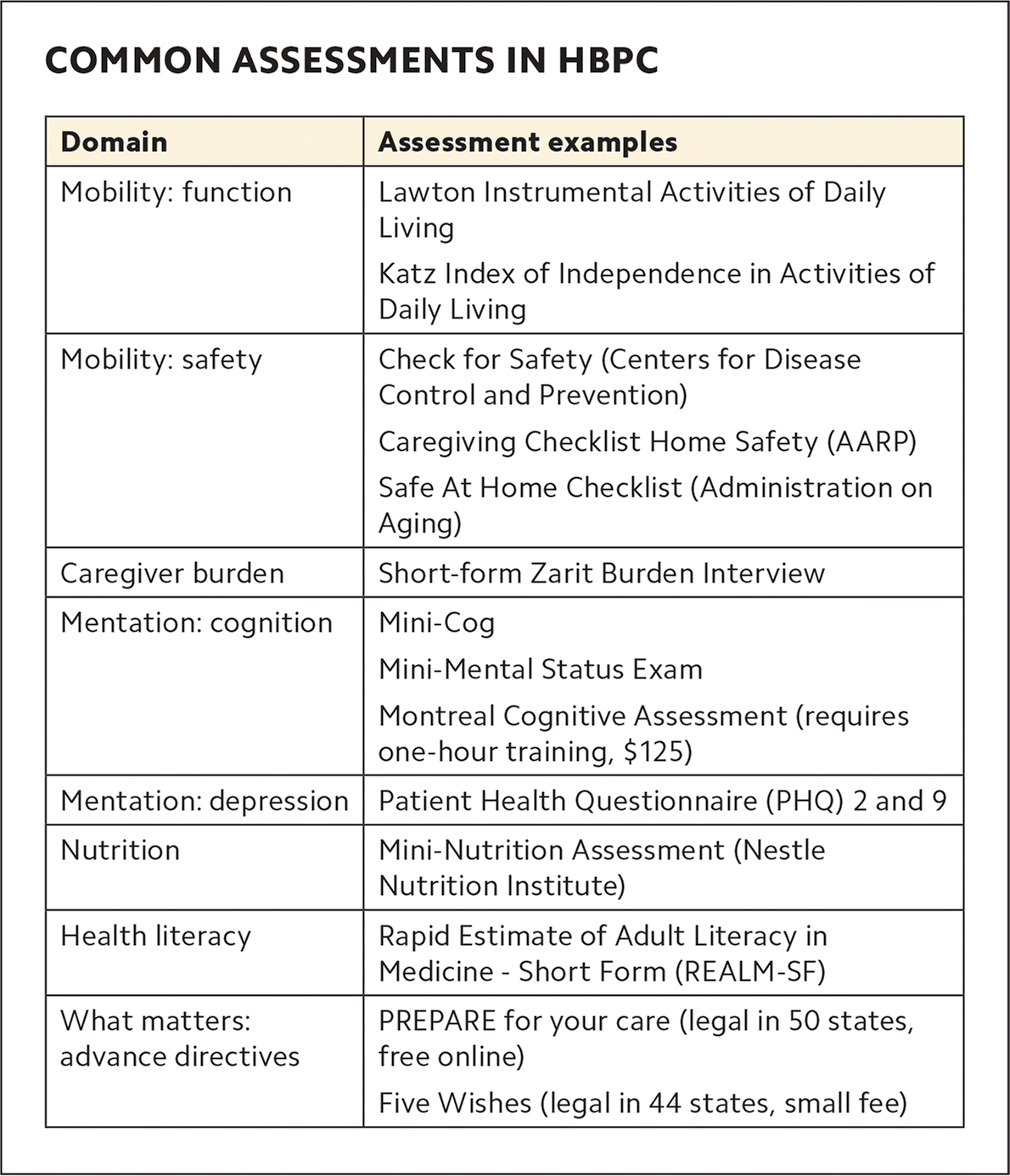
Clinical processes. The Institute for Healthcare Improvement's Age-Friendly Health Systems' "4Ms" framework is an excellent approach to complex house call patients. The 4Ms are what matters, medication, mentation, and mobility. What matters is determined through conversations with patients about their goals of care, leading to advance directives. The home is an ideal setting to have these conversations. It is also the best place to reconcile and optimize medications, which often includes deprescribing in frail older adults. Mentation refers to diagnosing and managing dementia, depression, and delirium. Mobility focuses on ADLs, maintaining function, gait, safety, and independence. (See “Common assessments in HBPC.”)
| Domain | Assessment examples |
|---|---|
| Mobility: function | Lawton Instrumental Activities of Daily Living Katz Index of Independence in Activities of Daily Living |
| Mobility: safety | Check for Safety (Centers for Disease Control and Prevention) Caregiving Checklist Home Safety (AARP) Safe At Home Checklist (Administration on Aging) |
| Caregiver burden | Short-form Zarit Burden Interview |
| Mentation: cognition | Mini-Cog Mini-Mental Status Exam Montreal Cognitive Assessment (requires one-hour training, $125) |
| Mentation: depression | Patient Health Questionnaire (PHQ) 2 and 9 |
| Nutrition | Mini-Nutrition Assessment (Nestle Nutrition Institute) |
| Health literacy | Rapid Estimate of Adult Literacy in Medicine - Short Form (REALM-SF) |
| What matters: advance directives | PREPARE for your care (legal in 50 states, free online) Five Wishes (legal in 44 states, small fee) |
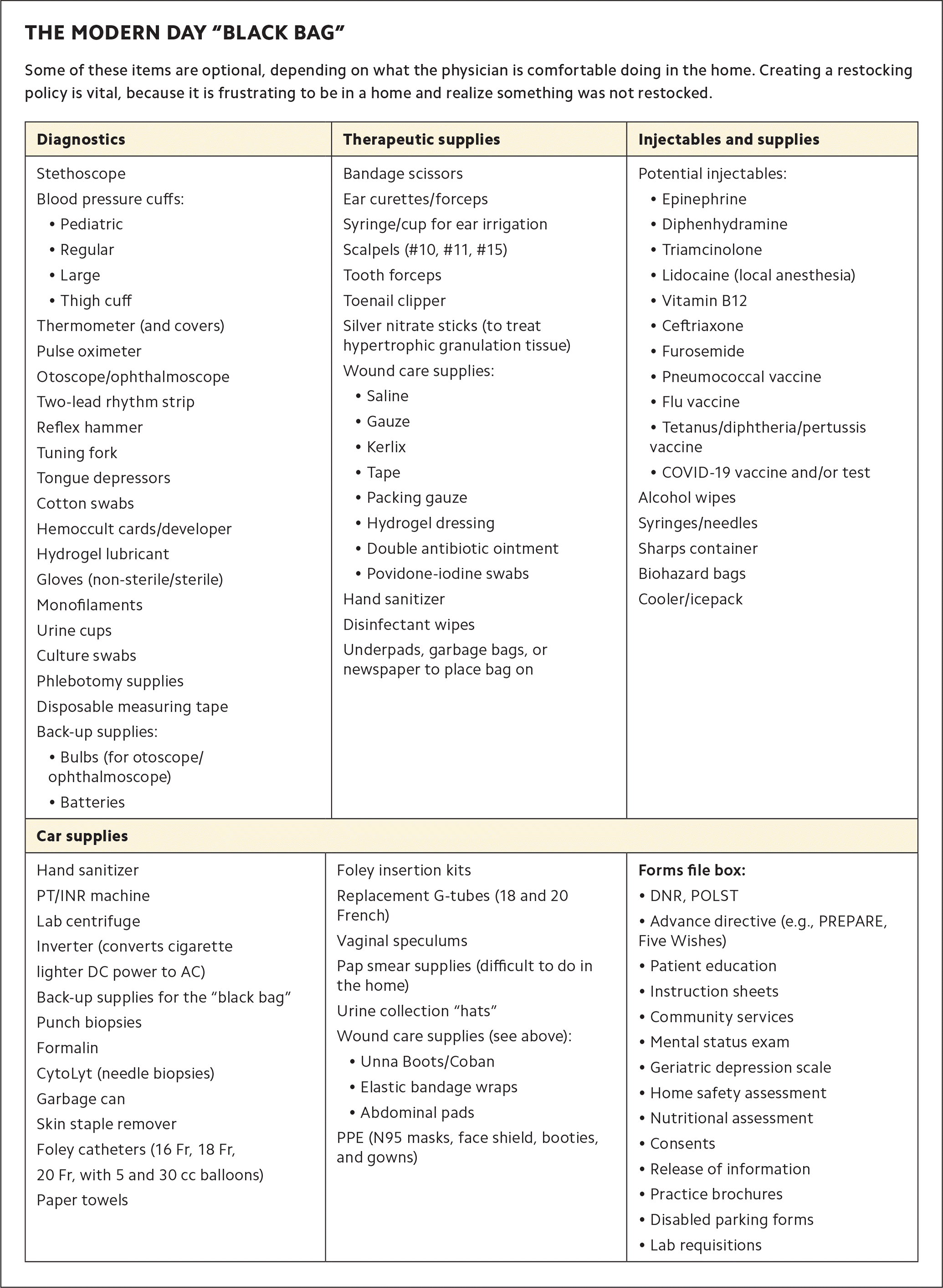
A house call's main clinical difference is that the exam room is in the patient's home. This requires bringing the office to the patient. The table below shows the modern-day “black bag.” The supply list will vary somewhat depending on what the physician is comfortable doing in the home. The home also provides tremendous information about the patient, including diet, safety (are there grab bars, fall hazards, etc.), social determinants of health, and what matters to the patient (pictures, religious objects, etc.). It is important to be culturally sensitive in patients' homes, which is best accomplished by asking about patient and caregiver preferences.
| Diagnostics | Therapeutic supplies | Injectables and supplies |
|---|---|---|
| Stethoscope Blood pressure cuffs:
Thermometer (and covers) Pulse oximeter Otoscope/ophthalmoscope Two-lead rhythm strip Reflex hammer Tuning fork Tongue depressors Cotton swabs Hemoccult cards/developer Hydrogel lubricant Gloves (non-sterile/sterile) Monofilaments Urine cups Culture swabs Phlebotomy supplies Disposable measuring tape Back-up supplies:
| Bandage scissors Ear curettes/forceps Syringe/cup for ear irrigation Scalpels (#10, #11, #15) Tooth forceps Toenail clipper Silver nitrate sticks (to treat hypertrophic granulation tissue) Wound care supplies:
Hand sanitizer Disinfectant wipes Underpads, garbage bags, or newspaper to place bag on | Potential injectables:
Alcohol wipes Syringes/needles Sharps container Biohazard bags Cooler/icepack |
| Car supplies | ||
| Hand sanitizer PT/INR machine Lab centrifuge Inverter (converts cigarette lighter DC power to AC) Back-up supplies for the “black bag” Punch biopsies Formalin CytoLyt (needle biopsies) Garbage can Skin staple remover Foley catheters (16 Fr, 18 Fr, 20 Fr, with 5 and 30 cc balloons) Paper towels | Foley insertion kits Replacement G-tubes (18 and 20 French) Vaginal speculums Pap smear supplies (difficult to do in the home) Urine collection “hats” Wound care supplies (see above):
PPE (N95 masks, face shield, booties, and gowns) | Forms file box:
|
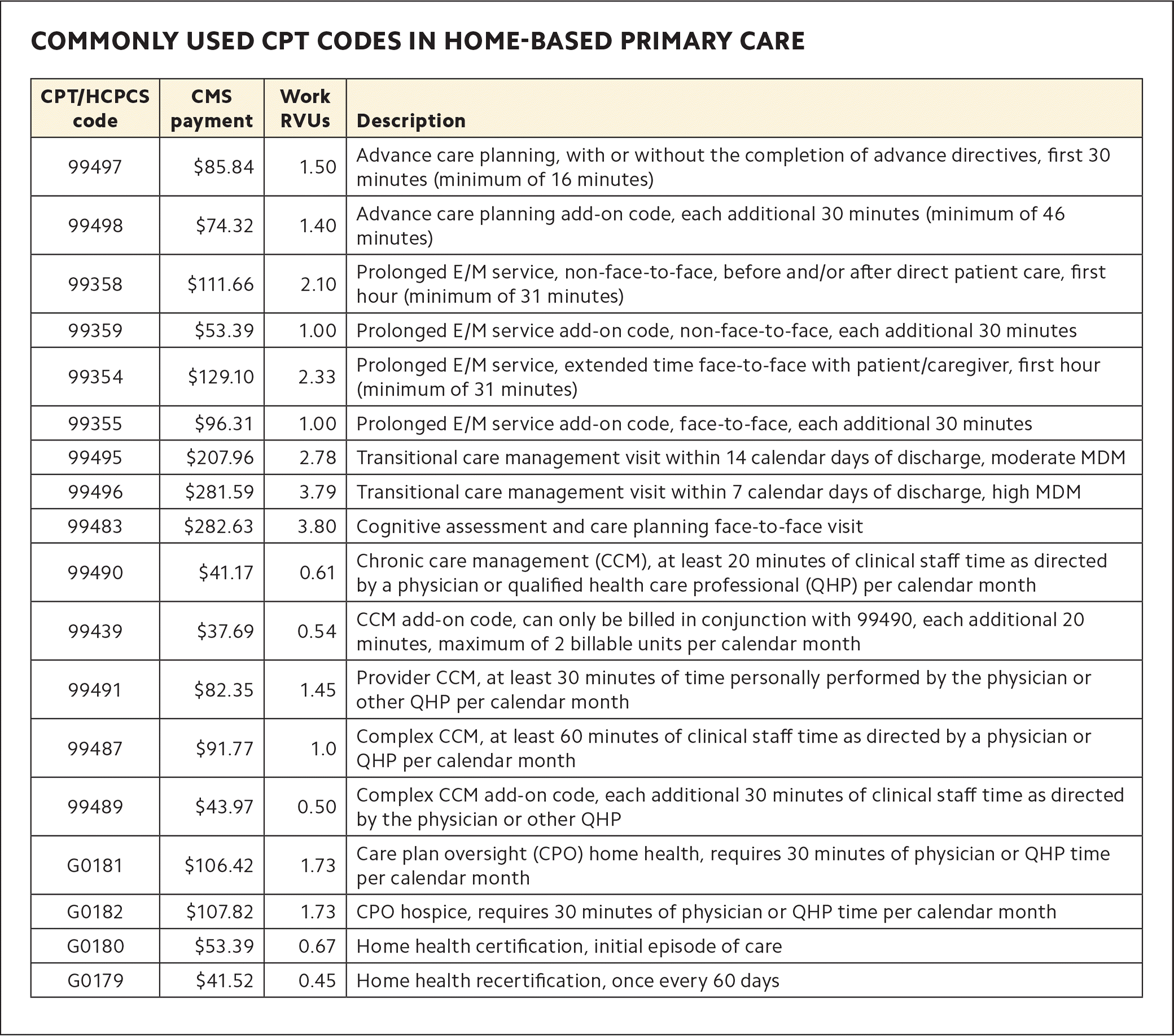
It is wise to review charts the day before the home visit to see if fasting blood work or any unique supplies are needed, such as injections, immunizations, or gastrostomy tubes. It also helps to review charts for complex, new, and TCM patients ahead of the visit and start pre-charting. Extensive prep time (more than 30 minutes) can be billed using CPT codes for prolonged evaluation and management (E/M) services. (See “Commonly used CPT codes in home-based primary care.”)
| CPT/HCPCS code | CMS payment | Work RVUs | Description |
|---|---|---|---|
| 99497 | $85.84 | 1.50 | Advance care planning, with or without the completion of advance directives, first 30 minutes (minimum of 16 minutes) |
| 99498 | $74.32 | 1.40 | Advance care planning add-on code, each additional 30 minutes (minimum of 46 minutes) |
| 99358 | $111.66 | 2.10 | Prolonged E/M service, non-face-to-face, before and/or after direct patient care, first hour (minimum of 31 minutes) |
| 99359 | $53.39 | 1.00 | Prolonged E/M service add-on code, non-face-to-face, each additional 30 minutes |
| 99354 | $129.10 | 2.33 | Prolonged E/M service, extended time face-to-face with patient/caregiver, first hour (minimum of 31 minutes) |
| 99355 | $96.31 | 1.00 | Prolonged E/M service add-on code, face-to-face, each additional 30 minutes |
| 99495 | $207.96 | 2.78 | Transitional care management visit within 14 calendar days of discharge, moderate MDM |
| 99496 | $281.59 | 3.79 | Transitional care management visit within 7 calendar days of discharge, high MDM |
| 99483 | $282.63 | 3.80 | Cognitive assessment and care planning face-to-face visit |
| 99490 | $41.17 | 0.61 | Chronic care management (CCM), at least 20 minutes of clinical staff time as directed by a physician or qualified health care professional (QHP) per calendar month |
| 99439 | $37.69 | 0.54 | CCM add-on code, can only be billed in conjunction with 99490, each additional 20 minutes, maximum of 2 billable units per calendar month |
| 99491 | $82.35 | 1.45 | Provider CCM, at least 30 minutes of time personally performed by the physician or other QHP per calendar month |
| 99487 | $91.77 | 1.0 | Complex CCM, at least 60 minutes of clinical staff time as directed by a physician or QHP per calendar month |
| 99489 | $43.97 | 0.50 | Complex CCM add-on code, each additional 30 minutes of clinical staff time as directed by the physician or other QHP |
| G0181 | $106.42 | 1.73 | Care plan oversight (CPO) home health, requires 30 minutes of physician or QHP time per calendar month |
| G0182 | $107.82 | 1.73 | CPO hospice, requires 30 minutes of physician or QHP time per calendar month |
| G0180 | $53.39 | 0.67 | Home health certification, initial episode of care |
| G0179 | $41.52 | 0.45 | Home health recertification, once every 60 days |
House call practices commonly have 20% to 25% mortality rates, so it is critical to discuss goals of care such as the patient's desired medical decision-maker if needed, level of hospital care, cardiopulmonary resuscitation (CPR), and end-of-life wishes (e.g., desired place of death, hospice services, and funeral arrangements). These advance care planning (ACP) discussions can be billed with CPT code 99497 if a minimum of 16 minutes is spent and the patient consents to the conversation voluntarily (be sure to note this in your documentation). These discussions often take place over several visits, and there is no limit on how often ACP can be billed. Copays are waived for ACP done during annual wellness visits, but co-pays will apply if performed with another service.
House call patients are best served by an interdisciplinary team providing a range of services, often virtually, including the following:
Ancillary service providers (mobile X-ray, ultrasound, and phlebotomy).
Home health and hospice (Medicare pays physicians for the certification and recertification of home health and care plan oversight if they spend 30 minutes in a calendar month overseeing home health or hospice).
Care coordination departments (such as ED or hospital discharge planning).
Durable medical equipment companies.
Community organizations (Area Agencies on Aging can assist with Meals on Wheels, utilities, home maintenance, etc.; other community organizations may provide behavioral health, private duty, or respite care; and websites such as findhelp.org by Aunt Bertha list resources by ZIP code).
Other professionals making house calls (audiologists, dentists, optometrists, podiatrists, etc.).
PAYMENT FOR HOUSE CALLS
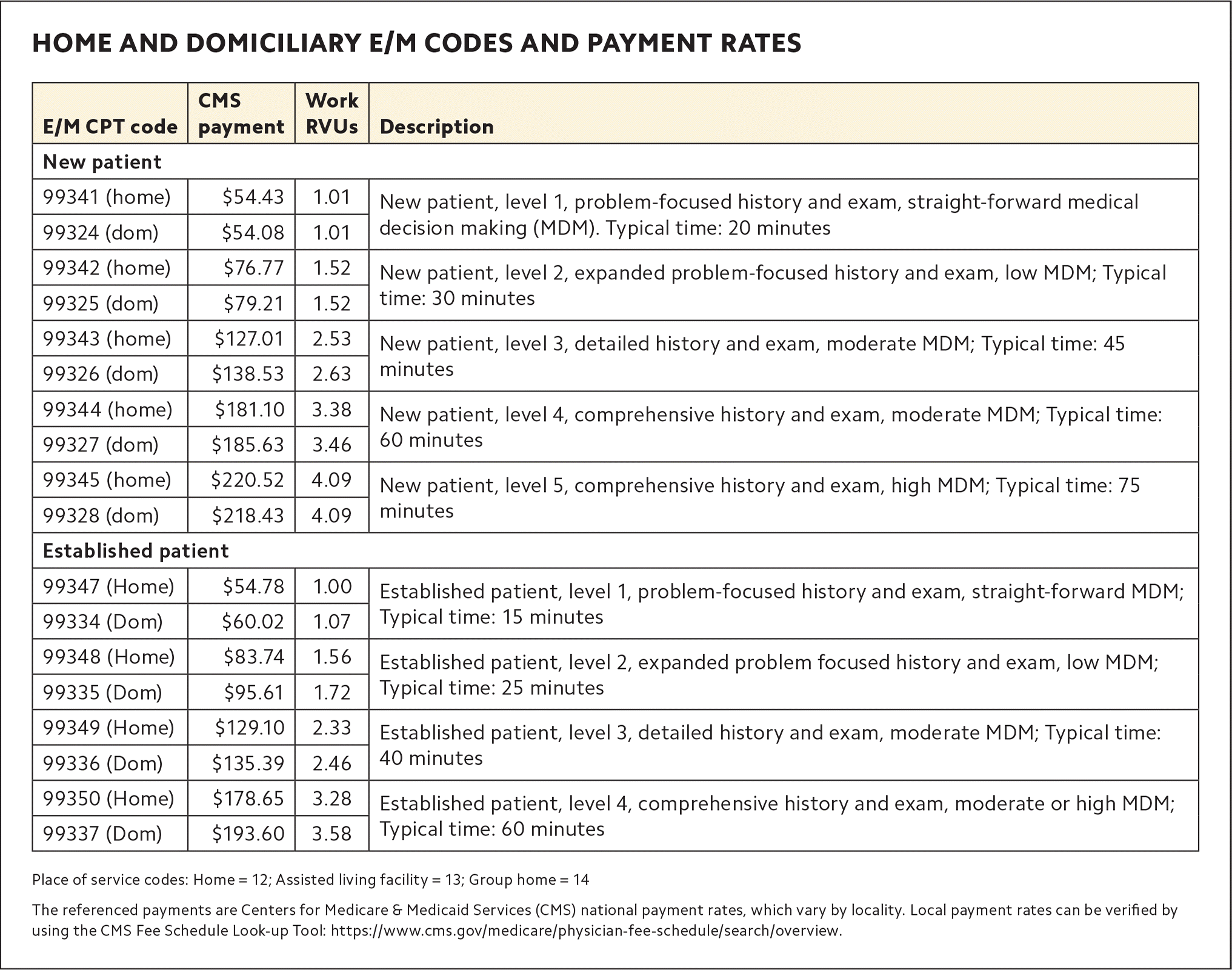
Medicare fee-for-service (FFS) payments fund most house call programs. The 2021 changes in office outpatient E/M documentation requirements do not apply to home or domiciliary visit codes, so you are still required to use the 1995 or 1997 E/M documentation guidelines for these visits. Billing by time still requires that more than 50% of the visit be spent in counseling and/or coordination of care. (See “Home and domiciliary E/M codes and payment rates.”) Other commonly used CPT codes in HBPC and their payment rates are listed in the table above. Most of these CPT codes are new in the past decade.
| E/M CPT code | CMS payment | Work RVUs | Description |
|---|---|---|---|
| New patient | |||
| 99341 (home) | $54.43 | 1.01 | New patient, level 1, problem-focused history and exam, straight-forward medical decision making (MDM). Typical time: 20 minutes |
| 99324 (dom) | $54.08 | 1.01 | |
| 99342 (home) | $76.77 | 1.52 | New patient, level 2, expanded problem-focused history and exam, low MDM; Typical time: 30 minutes |
| 99325 (dom) | $79.21 | 1.52 | |
| 99343 (home) | $127.01 | 2.53 | New patient, level 3, detailed history and exam, moderate MDM; Typical time: 45 minutes |
| 99326 (dom) | $138.53 | 2.63 | |
| 99344 (home) | $181.10 | 3.38 | New patient, level 4, comprehensive history and exam, moderate MDM; Typical time: 60 minutes |
| 99327 (dom) | $185.63 | 3.46 | |
| 99345 (home) | $220.52 | 4.09 | New patient, level 5, comprehensive history and exam, high MDM; Typical time: 75 minutes |
| 99328 (dom) | $218.43 | 4.09 | |
| Established patient | |||
| 99347 (Home) | $54.78 | 1.00 | Established patient, level 1, problem-focused history and exam, straight-forward MDM; Typical time: 15 minutes |
| 99334 (Dom) | $60.02 | 1.07 | |
| 99348 (Home) | $83.74 | 1.56 | Established patient, level 2, expanded problem focused history and exam, low MDM; Typical time: 25 minutes |
| 99335 (Dom) | $95.61 | 1.72 | |
| 99349 (Home) | $129.10 | 2.33 | Established patient, level 3, detailed history and exam, moderate MDM; Typical time: 40 minutes |
| 99336 (Dom) | $135.39 | 2.46 | |
| 99350 (Home) | $178.65 | 3.28 | Established patient, level 4, comprehensive history and exam, moderate or high MDM; Typical time: 60 minutes |
| 99337 (Dom) | $193.60 | 3.58 | |
Value-based care (VBC) payments are fueling the growth of house calls. Payments can vary, from shared savings with only upside potential and no downside risk, to global capitation with full risk for all patient care. Three things are essential for success: 1) capturing risk scores for accurate payment, 2) improving quality and the patient experience and closing gaps in care, and 3) lowering costs principally by reducing acute care utilization. House calls do all three exceedingly well and lower acute-care usage more than any other intervention. For family practices involved in Accountable Care Organizations or other forms of VBC, house calls can significantly contribute to the bottom line.
RESOURCES
American Academy of Family Physicians Home-based Primary Care Member Interest Group (AAFP members only)
Rerucha CM, Salinas R, Shook J, Duane M. House calls. Am Fam Physician. 2020;102(4):211–220.
