Draft Guidelines Issued for Office-based Primary Care Procedures
'If You Don't Find Them Useful, Now Is the Time to Say Something'
It was in this shadow of excessive regulation that a multispecialty effort -- the Project on Facility Guidelines for the Safe Performance of Primary Care and Gynecology Procedures in Offices and Clinics -- was born late in 2016.
According to the project website, the end goal is to "articulate evidence-informed guidelines that will further health care quality, safety, affordability and patient experience without imposing unjustified burdens on patients' access to care or on clinicians' ability to provide care within their scope of practice."
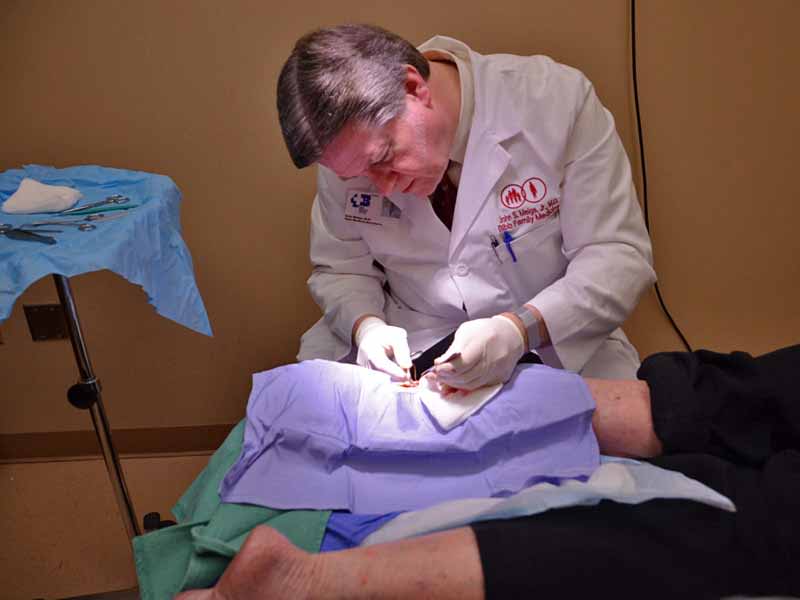
Now, in mid-April 2018, a draft set of guidelines has been posted on the website for public comment. Family physicians and all affected stakeholders are urged to read the guidelines and provide their input before the comment period closes on May 13 at 11:59 EDT.
Breadth of Participation
This multi-specialty effort was initiated by the American College of Obstetricians and Gynecologists and the National Partnership for Women & Families. Those founders then asked the AAFP, the American College of Physicians, the American College of Nurse-Midwives, Nurse Practitioners in Women's Health, and the Society of Family Planning to join the planning committee.
A guideline summit meeting in December 2017 included more than a dozen other organizations as well as patient representatives.
Story Highlights
Impact on Family Medicine
Valerie King, M.D., M.P.H., a professor in the Department of Family Medicine at Oregon Health and Science University (OHSU) in Portland, represents the AAFP on the project's procedures working group that reviewed evidence and current clinical practices in six domains.
She told AAFP News the issue is critical for family medicine.
"Family physicians do an awful lot of primary care-oriented procedures in their offices and clinics, and when local regulations or state legislators try to say what they can do -- or who can do it -- that influences their practices," said King.
For instance, physicians may have had run-ins with regulations on facility standards that have no scientific basis, but nonetheless dictate the width of halls and doorways.
Family physicians who have the competency-based training to do a vasectomy may have been told the procedure can only be performed by a urologist, said King.
Because of those kinds of situations, family physicians would do well to invest some time reading the draft guidelines to ensure they are applicable to their individual practices.
"If people agree to them, this will be a nationally recognized set of guidelines, said King, who also serves as the research director for OHSU's Center for Evidence-based Policy. "These guidelines will probably be used in the state that you're working in. So if you don't find them useful, now is the time to say something."
Keep in mind that even if an individual physician has not yet been affected, a colleague's practice somewhere in the country undoubtedly has been touched by overbearing restrictions.
King said her workgroup has many examples -- for instance with emergency lighting and material disposal -- where local rules, regulations and state laws require action that some policymaker apparently pulled out the air with no evidence to back it up.
"This can happen to you, too," said King. "And policies that are unnecessarily restrictive result in restricted access to care for your patients."
Project Findings
The working group on which King participates researched guidelines for six domains of facility factors:
- emergency preparedness,
- biological material handling,
- physical plant specifications,
- clinician qualifications beyond licensing and competency,
- other policies and procedures, and
- facility accreditation and licensing.
King talked about the level of commitment among those in her group.
"We looked high, low and wide," said King. "We had a really extensive search process, we commissioned several systematic reviews, we went through and looked at expert-based guidelines and did methodological assessments.
"We did everything we could to be robust and evidence-based about what we were doing here," she said. "The bottom line is that we could find no evidence that there was a problem that would necessitate the kind of facility requirements that we were seeing written into law and regulations."
At the end of the day, King and her team decided to articulate what the accepted standards are, and that's what physicians will see when they review the document, said King.
"The draft guidelines are an articulation and a compilation of those standards because we did not find good evidence that said anything else was necessary."
King noted that some of the rules, regulations and laws the working group researched were written to deal with ambulatory surgical centers. "Obviously that's very different from most office-based procedures," she said.
She also pointed out that the guidelines do not address anesthesia or sedation. "We're not trying to supplant what we found to be reasonable and widely accepted guidelines already developed by the American Society of Anesthesiologists."
Once the comment period concludes, experts will read and collate the comments. If a public reviewer points out literature that was missed by the group's research, they'll dive back in before finalizing the guidelines and readying them for dissemination nationwide.
Stay tuned for that release in the future.
