Nearly one half of Americans die of cardiovascular disease. The morbidity and mortality associated with coronary artery disease is strongly related to abnormal lipid levels, oxidation of lipids and intra-arterial clot formation. Nutrition powerfully influences each of these factors. There is growing evidence that patients can improve lipid levels and decrease the rate of cardiovascular events by “adding” specific foods to their diets and switching from saturated and polyunsaturated to monounsaturated fats and n-3 fatty acids. Appropriate dietary changes decrease arteriosclerotic plaque formation, improve endothelial vasomotor dynamics, reduce oxidation of low-density lipoproteins and enhance thrombolytic activity. Brief discussions between physicians and patients can influence patients' food choices. Changes in diet can reduce the premature mortality and morbidity associated with coronary artery disease.
Physicians in the United States diagnose over 500,000 new cases of coronary artery disease each year. Diet is strongly related to the development of this disease. Family physicians can play a critical role in reducing the morbidity and mortality associated with coronary artery disease by influencing their patients' dietary choices.
Brief messages from physicians regarding food choices can be effective in changing their patients' eating habits.1 While physicians often have been skeptical about their ability to influence patients' diets, significant diet changes are achievable and sustainable.2 Current evidence suggests that, given the opportunity and support, 50 percent of people with angina are willing to make dramatic changes in their diet.3,4 For example, the Ornish program is a lifestyle modification plan that promotes daily aerobic exercise, daily stress reduction and a diet with less than 10 percent of calories from fat. Patients with known coronary artery disease who followed the program achieved a 37.4 percent decrease in low-density lipoprotein (LDL) cholesterol levels and a greater than 90 percent decrease in angina frequency within two months.3 Patients in other studies achieved similar success using the Ornish program.4 A five-year clinical trial5 demonstrated excellent adherence to the Ornish program. While the Ornish program is limited by patient willingness and financial resources, it demonstrates that, with adequate support, motivated patients can achieve dramatic, long-term dietary changes.
Therapy Goals
Practitioners need efficient methods of providing practical information to healthy patients; they need to help them interpret their cholesterol and lipid levels, and to give them information to help them improve their dietary choices. Patient handout materials provide details and complement brief physician messages.
We lack controlled randomized clinical trials that clearly establish the ideal LDL cholesterol level or total cholesterol/high-density lipoprotein (TC/HDL) ratio. However, in patients with known coronary artery disease, strong evidence based on clinical outcomes suggests that patients with high LDL cholesterol levels can decrease their risk of mortality and morbidity by reducing their LDL cholesterol level by 30 to 35 percent.6,7
For example, in 1995 the Group Health Cooperative of Puget Sound, a 500,000–member health maintenance organization, used an evidence-based review of the literature6,7 to establish lipid lowering targets for patients with known coronary artery disease. When LDL cholesterol levels exceed 125 mg per dL (3.25 mmol per L), diet and/or medications are used to reduce LDL cholesterol levels by at least 30 percent. If original LDL cholesterol levels are unknown, lipid targets should include LDL cholesterol levels less than 100 mg per dL (2.60 mmol per L), or LDL cholesterol levels less than 130 mg per dL (3.35 mmol per L) and a TC/HDL ratio less than 4.0 mg per dL.
Not all patients are willing or able to reach these lipid targets with lifestyle changes alone. Patients at high risk of coronary artery disease who fail to reach these targets with diet and exercise should be prescribed lipid-lowering medications.
Dietary Methods to Reduce LDL Levels
While clinicians often tell patients what to eliminate from their diets to reach a more favorable lipid profile, they can enhance their advice by also telling them what to add (Table 1).8 Patients might perceive food additions as more palatable than food restrictions.
Increase Soy Products and Legumes
Intake of soy products decreases LDL and total cholesterol levels without decreasing HDL cholesterol levels.9 Legume intake has also been shown in studies to decrease LDL and total cholesterol levels without decreasing HDL levels.10 Soy and bean products can serve as a protein source in a meal and can further reduce LDL cholesterol levels if they are substituted for fatty animal products.
Increase Garlic
Several meta-analyses11,12 have shown that garlic intake reduces LDL cholesterol levels by up to 9 percent and produces a small rise in HDL cholesterol levels; one medium-size garlic clove daily or capsules with 900 to 1,800 mg of dried fresh garlic are sufficient. Garlic has no known side effects except for the presence of odor in some individuals.
So far, no clinical trials have proved that increased intake of garlic decreases cardiac-induced mortality or morbidity, yet its use appears safe and potentially beneficial.
Increase Soluble Fiber
Soluble fiber increases excretion of fecal bile acid and removal of cholesterol. Good sources of soluble fiber include oat products, barley, fruits and vegetables. Several studies have shown that one daily serving of oat bran or oatmeal decreases total cholesterol levels by up to 3 percent.13 Pectin, a soluble fiber found in fruit, also decreases LDL cholesterol levels. Several servings must be eaten daily for substantial reductions. Exchanging soluble fiber for fat intake produces even greater reduction in LDL cholesterol levels.
Increase Monounsaturated Fats
Both monounsaturated and polyunsaturated fatty acids decrease LDL and total cholesterol levels and produce a small increase in triglyceride levels. However, there is growing evidence that increased intake of polyunsaturated fatty acid increases the oxidation of LDL cholesterol, leading to increased LDL uptake by macrophages, foam cell formation within the arterial intima and development of coronary artery obstruction.14 Polyunsaturated fatty acids also increase platelet aggregation, which can increase thrombus formation and the risk of stroke and myocardial infarction.15 These factors make the intake of monounsaturated fats (such as canola oil, monounsaturated-rich safflower oil and olive oil) preferable to polyunsaturated fats (such as corn oil, soybean oil and many margarines).
In contrast to the dominant use of polyunsaturated fat sources in most of the Western world, the Mediterranean diet uses predominantly monounsaturated fatty acids and n-3 fatty acids (omega-3 fats) as fat sources. To test the applicability of the Mediterranean diet in patients with cardiac disease, investigators in France16,17 randomized 605 post-myocardial infarction patients to either a control diet similar to the (NCEP) Step I-II diet (with 30 percent of total calories from fat) or an experimental diet similar to the Cretan Mediterranean diet. The Cretan diet uses olive oil and a special canola-oil margarine as its fat source. In this study, the Cretan diet also included more servings of legumes per day than the NCEP-like diet. Significant reductions in infarction, unstable angina, heart failure, stroke and thromboembolic events were noted in the patients on the experimental diet.
Over five years, total mortality decreased by 70 percent in the patients who followed the Mediterranean diet compared with the patients who followed the control diet (Figure 1). Since the difference in fat intake was minimal (33 percent in the control diet versus 30 percent in the Mediterranean diet) and lipid profiles were analogous, factors other than a reduction in fat intake must account for these striking differences in clinical events. These results are important because they indicate that dietary changes, independent of lipid levels, influence outcomes of patients with coronary heart disease.
FIGURE 1.
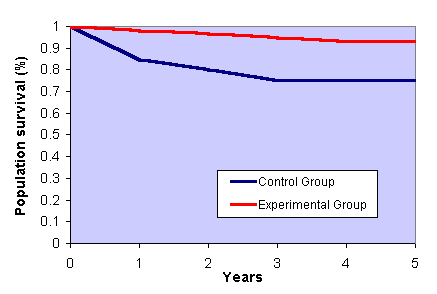
Comparison of survival rates in patients following myocardial infarction. The fat in the control group's diet consisted of standard, predominantly polyunsaturated fat, with 33 percent of total calorie intake from fat. The experimental group followed the Cretan Mediterranean diet for coronary artery disease. Fat intake consisted of mostly monounsaturated fat and increased omega-3 fatty acids, with 30 percent of total calories from fat.
Increase Monounsaturated-Rich Nuts
Nuts are a rich source of n-3 fatty acids, monounsaturated fats and vitamin E. Studies have shown that an increased intake of nuts is associated with improved lipid levels and decreased mortality and myocardial infarction.18–20 Nuts rich in monounsaturated fats and n-3 fats (e.g., hazelnuts, almonds, pecans, cashews, walnuts and macadamia nuts) appear preferable to nuts containing polyunsaturated fats, such as peanuts and pine nuts.
Reduce Saturated Fats and Trans Fatty Acids
It is well established that reducing intake of saturated fat reduces LDL cholesterol levels and that reductions in LDL cholesterol levels decrease the risk of coronary artery disease. European studies21 have shown that the causal relationship between saturated fat intake and coronary artery disease may be stronger than the relationship between coronary artery disease and hypertension, diabetes or tobacco use.
With the increasing popularity of margarine, trans fatty acids are gaining in use and now represent 2 to 3 percent of total calories in the U.S. diet. Trans fatty acids increase LDL cholesterol levels and decrease HDL cholesterol levels.22,23 Studies24 have shown that people can reduce their intake of saturated fat and trans fatty acids by nearly 50 percent by cutting out three dietary sources: butter and margarine, fatty meats and dairy products made from 2 percent or whole milk.
FIGURE 2.
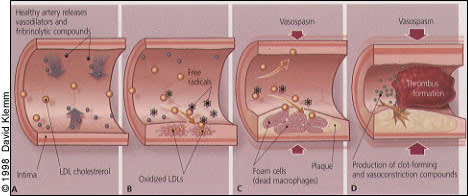
(A) An antioxidant-enriched diet maintains healthy arteries that release vasodilators and fibrinolytic compounds. (B) An antioxidant-inadequate diet results in free radical proliferation and LDL oxidation. Macrophages engulf oxidized LDL, die and form foam cells in the arterial intima. (C) Increased LDL oxidation and foam cell proliferation forms plaque and blocks the formation of fibrinolytic compounds and vasodilators. (D) A clinical event occurs when a 20–30% lumen-obstructing plaque ruptures. The plaque rupture causes immediate release of clot-forming and vasoconstriction compounds. Lumen obstructions lead to myocardial infarction or death. (LDL = low-density lipoprotein)
Methods of Decreasing Oxidation of LDL Cholesterol
A growing body of evidence suggests that the oxidation of cholesterol is an important factor in the development of coronary artery disease.25 First, oxidation of LDL cholesterol plays an essential role in macrophage uptake of LDL and the consequent accumulation of cholesterol plaque. Second, while intake of antioxidants is believed to decrease oxidation of LDL cholesterol, perhaps equally important is the role of antioxidants in improving vasomotion26 (Figure 2). Endothelial wall function is related to inhibition of platelet activity and fibrinolysis, critical factors in the pathophysiology of atherosclerosis.27
Epidemiologic studies have shown that an increased consumption of vegetables and fruits is associated with a decreased rate of coronary artery disease and increased plasma levels of antioxidants.28 The antioxidants in fruits and vegetables appear to decrease the oxidation of LDL cholesterol and decrease arterial plaque formation. Physicians should encourage patients to eat at least five to seven servings of vegetables and fruits daily.
Monounsaturated cooking oils and garlic also decrease the oxidation of LDL cholesterol.14,29,30 In one study,31 olive oil decreased LDL oxidation and also decreased macrophage uptake of LDL cholesterol. As previously noted, the intake of polyunsaturated fat increases oxidation of LDL cholesterol.14
Vitamin E obtained from food sources is inversely associated with the risk of death from coronary heart disease.19 In one epidemiologic study of 34,486 postmenopausal women,19 dietary intake of nuts and seeds, concentrated food sources of vitamin E, was determined to be inversely related to the risk of death from coronary artery disease. In the Mediterranean diet study,16,17 greater serum levels of vitamin E were detected in patients on the Mediterranean diet, despite a lower consumption of dietary vitamin E. From this study, legumes and monounsaturated cooking oils appear to contain other antioxidants that maintain vitamin E levels.
Dietary Methods of Increasing Antithrombin Activity
The medical literature emphasizes plaque formation as the major factor affecting arterial blood flow. However, many acute myocardial infarctions are the result of plaque rupture and subsequent thrombus formation.32 Factors that deter thrombus formation and platelet aggregation may improve the clinical prognosis substantially. Alcohol has been found to decrease platelet aggregation. Garlic and n-3 (omega-3) fatty acids can also decrease platelet aggregation and increase fibrinolytic activity.11,21
Saturated fatty acids and polyunsaturated fatty acids increase platelet aggregation.15,21 A P/S ratio (defined as the ratio of polyunsaturated fatty acids to saturated fatty acids) greater than 0.8 is associated with increased platelet aggregation.15,21 Hence, substituting polyunsaturated fat for saturated fat reduces LDL cholesterol levels but may increase thrombus formation.
N-3 Fatty Acids
At first glance, physicians might avoid technical information about n-3 fatty acids because these compounds fall into complex biochemical pathways, but their actions are fairly straightforward and important. Dietary n-3 fatty acids are derived from plant and seafood sources. Plant sources provide a medium-chain fatty acid of 18:3 n-3 (called alpha-linolenic acid). Seafood provides long-chain fatty acids of 20:5 n-3 (called EPA or eicosapentaenoic acid) and 22:6 n-3 (called DHA or docosahexaenoic acid). Alpha-linolenic acid is converted into long-chain fatty acids. Since linoleic acid and linolenic acid compete for the same delta-6 desaturase enzyme reaction,33 this conversion accelerates greatly, increasing EPA levels 2.5-fold, when linoleic acid (polyunsaturated fat) intake is limited. Polyunsaturated fats (e.g., corn oil, peanut oil) inhibit the beneficial actions of n-3 fatty acids (Figure 3).
FIGURE 3.
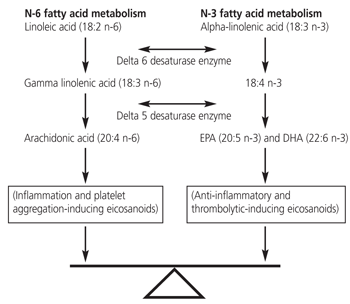
A balanced intake of polyunsaturated fats (n-6 fatty acids) and omega-3 (n-3) fatty acids theoretically produces balanced inflammatory and thrombolytic activity. (EPA = eicosapentaenoic acid; DHA = docosahexaenoic acid)
Plant Sources of n-3 Fatty Acids
Alpha-linolenic acid is an n-3 fatty acid found in green leafy vegetables, canola oil, flax oil, soybean products, walnuts and hazelnuts. Increased intake of foods rich in alpha-linolenic acid decreases LDL cholesterol levels.34 Intake of linolenic acid is strongly associated with a decreased risk of coronary artery disease.35 In one study35 of 43,757 health professionals, the protective cardiac effect achieved with linolenic acid was more significant than a reduction in saturated fat intake. Of particular interest in this study was the finding that plant sources of n-3 fatty acids exhibited a significant protective effect, while seafood sources of n-3 fatty acids did not. Similarly, in the Mediterranean diet study, a threefold increase in alpha-linolenic acid intake was a factor associated with a 70 percent reduction in mortality rates.16,17
Seafood Sources of n-3 Fatty Acids
Fish and fish oils are other common dietary sources of n-3 fatty acids. Fish oils decrease triglycerides36,37 and offer an alternative in the treatment of hypertriglyceridemia to gemfibrozil (Lopid), which may be contraindicated in many patients. Unfortunately, the long-term safety of fish oil as an agent to reduce triglyceride levels remains unknown.
Long-chain n-3 fatty acids also decrease platelet aggregation and improve blood viscosity.36,37 Fish oils, in a dosage of 10 g per day, have almost the same platelet effect as 325 mg of aspirin daily.
Studies evaluating fish consumption and rates of coronary artery disease in healthy adults have provided conflicting results.38,39 There is currently no solid evidence that people without coronary artery disease should eat more seafood. However, studies in patients with coronary artery disease have been more promising, demonstrating significant reductions in mortality and infarction rates.40 The clinical benefits of eating one to two servings of seafood weekly might result from reduced platelet aggregation in people with significant arterial narrowings. Anti-arrhythmic activity associated with increased fish consumption has also been hypothesized as the cause of decreased mortality rates in patients with known coronary artery disease.
Final Comment
Dietary changes can help prevent and treat coronary artery disease. Some diets, like the Mediterranean and Japanese diets, are associated with much lower rates of coronary artery disease than the traditional Western diet. The former diets limit the intake of saturated and polyunsaturated fats and supply an abundance of dietary antioxidants and alphalinolenic acid. Further evidence that a Japanese or Mediterranean diet is in itself beneficial is the finding that Americans have a higher rate of cardiac mortality even when their cholesterol levels are the same as the levels of Japanese or Southern Europeans41 (Figure 4). Nondietary lifestyle factors, such as increased activity, may also influence differences in mortality rates.
Family physicians can sweeten dietary recommendations to their patients by emphasizing the addition of specific beneficial foods, rather than the elimination of foods. Soy products, legumes, garlic, soluble fiber and nuts rich in monounsaturated fat all reduce serum LDL cholesterol levels and should be encouraged as daily staples in the Western diet. Dietary antioxidants hinder arterial plaque formation and improve endothelial vasomotor function. In particular, garlic, red wine, monounsaturated fats, and fruits and vegetables are associated with decreased oxidation of LDL cholesterol.
Intake of saturated fat increases the rates of strokes and heart attacks. Trans fatty acids act like saturated fats and are associated with worsened lipid profiles. Physicians should encourage patients to decrease their use of saturated fat and trans fatty acids (Table 1).8
Moderate use of monounsaturated fats (canola oil and olive oil) decreases LDL cholesterol levels and LDL oxidation and appears preferable to use of highly polyunsaturated fats. In contrast to ultra–low-fat diets, the “take home message” from clinical studies of a Mediterranean diet is that switching from saturated and polyunsaturated fats to monounsaturated and n-3 fats is more important than cutting the total fat intake.
Intake of n-3 fatty acids from plant and fish sources is associated with anti-arrhythmic activity, decreased platelet aggregation and decreased rates of sudden death in patients with known coronary artery disease. In repeated clinical trials, plant sources of alpha-linolenic acid have been associated with decreases in LDL cholesterol levels and decreases in the rate of morbidity and mortality associated with coronary artery disease. One to two servings of seafood a week appears to benefit patients with coronary artery disease. Healthy populations have not shown a consistent benefit from eating more seafood. Studies that assess intake of n-3 fatty acids from fish sources also need to assess the intake of n-3 fatty acids from plant sources.
Except for the Mediterranean diet study, we lack controlled, randomized clinical trials using dietary interventions to assess clinical outcomes. While the Ornish program excels at improving intermediate markers of coronary artery disease (i.e., LDL cholesterol levels and treadmill results), no randomized trials show that the Ornish program decreases cardiac mortality, overall mortality or even nonfatal cardiac events. And, while the Mediterranean diet showed a decrease in cardiac and noncardiac mortality and events in patients with coronary artery disease in France, and might be more easily accommodated by some patients than ultra–low-fat diets, it remains to be proved that the Mediterranean diet is applicable to other countries and cultures.
A modified “antioxidant diet” that includes up to 20 percent of total calories from fat (largely monounsaturated fat and n-3 fatty acids) and generous amounts of dietary antioxidants from plant sources could increase patient compliance and might lead to a decrease in overall mortality and morbidity.
Family physicians can motivate their patients to eat better by providing them with brief but detailed nutritional information. Short, repetitive messages regarding nutrition are effective in changing patients' eating habits.1 In patients with known coronary artery disease, LDL and TC/HDL target levels should be reached within two to six months of diet therapy, or lipid-lowering medications should be considered. Ongoing dietary intervention should continue even after lipid-lowering medications are initiated.

