Smoking rates among persons with a history of alcohol abuse are triple that of the general public. Strong evidence indicates that the risk of cancer and cardiovascular disease is higher in recovering alcoholics than in peers who smoke, but do not drink alcohol. Yet these persons often receive less than optimal tobacco counseling out of fear that attempts at smoking cessation will jeopardize their sobriety. Recent research, however, does not support this belief; rather, it suggests that smoking cessation may actually enhance alcohol abstinence. A model for more effective counseling of smokers in recovery is presented, including an algorithm for assessing stages of readiness to change, with activities tailored for each stage. Specific motivational counseling techniques may be useful in encouraging recovering alcoholics to progress to the point that they are ready to change their smoking behavior.
Smoking remains the chief preventable cause of premature disability and death in the United States. Smoking rates average 25 percent in the general population1 but increase to 80 to 95 percent in chemically dependent persons.2
Epidemiologic studies3–6 suggest that current and former alcoholic adults are at greater risk for some deleterious health effects of smoking, particularly cancer and cardiovascular disease, than are members of the general smoking and nonsmoking populations. A recent study on mortality following inpatient addiction treatment7 found that patients previously treated for alcoholism or other drug dependence had a significantly higher cumulative mortality rate at 20 years (48.1 percent) than persons in the general population (18.5 percent). Since the causes of these deaths were more often related to tobacco (50.9 percent) than to alcohol (34.1 percent), the study concluded that “nicotine-dependence treatment is imperative in such high-risk patients.”7
Until relatively recently, few studies had examined the effects of simultaneous treatment of multiple addictions. Smoking was generally considered more socially acceptable than other forms of substance use. For a long time, in fact, nicotine was not even considered addictive. The use of tobacco products was also perceived as being less disruptive to society than other forms of chemical dependence. Furthermore, most staff members in chemical dependency treatment centers were recovering alcoholics or problem drinkers who still smoked.8,9 Most importantly, traditional recovery folklore emphasized handling “one thing at a time,” based on the rationale that smoking cessation is stressful and likely to endanger sobriety.
As early as 1983, however, a positive relationship was found between smoking cessation during alcohol treatment and the chance of maintaining sobriety.10 The findings of this study suggested an additive or synergistic effect when smoking and alcohol addictions were addressed simultaneously. Other recent research studies and review articles have supported these findings.11–16
A model illustrating smoking cessation activities for use with patients in alcohol recovery is presented in this article. The model consists of an algorithm for determining the patient's stage of readiness to change smoking behavior,17 strategies for interventions appropriate for each stage and a counseling technique that can enhance patient motivation.18 This model follows the clinical practice guidelines of the Agency for Health Care Policy and Research (AHCPR) of the U.S. Department of Health and Human Services.19
Assessing Readiness to Change
In the readiness-to-change model, smoking cessation is viewed as a process of change with five stages: precontemplation, contemplation, preparation, action and maintenance. Research has suggested that the progress patients make following interventions for behavioral change tends to be a function of their pretreatment stage of change.17 When a smoker's stage of readiness to change is known, messages can be tailored to the appropriate goal for that patient's condition.
An algorithm for assessing stage of readiness to change is presented in Figure 1.17 The question “Are you currently using tobacco?” is in accordance with the clinical practice guidelines of the AHCPR. According to these guidelines19 and supporting research,20 every patient's current tobacco-use status should be identified at every office visit, and all smokers should be offered smoking cessation treatment at every visit. It is especially important to use these strategies with recovering alcoholic patients, since these persons have been found to be at increased risk for tobacco-related illnesses. The other questions in the algorithm assess the patient's stage of readiness to change smoking behavior by identifying current intentions and previous actions.
FIGURE 1.
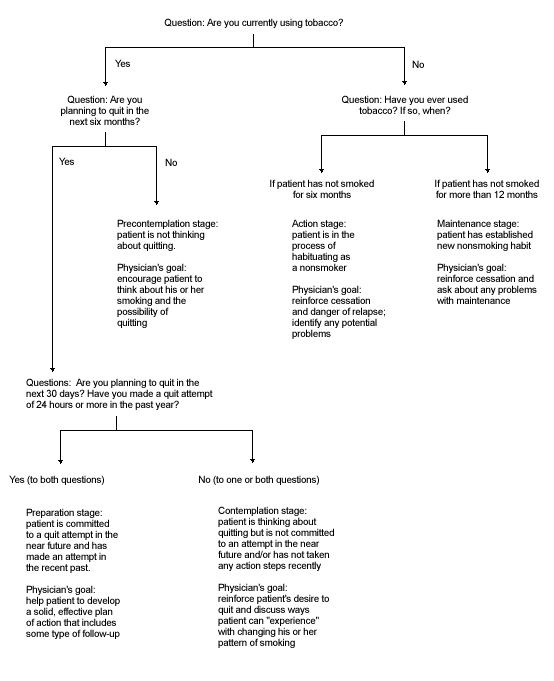
Algorithm for identifying five stages of readiness to change in recovering alcoholic patients who use tobacco.
Counseling Strategies
Realistic Goals
Once the smoker's stage of readiness has been identified, the strategies for that stage can be implemented (Table 1). These activities are designed to facilitate patient movement from his or her current stage to the next stage, with the eventual goal being long-term smoking cessation. The activities themselves are a mix of proven smoking cessation techniques and Alcoholics Anonymous' 12-step activities with which the patient is likely to be familiar. Drawing a parallel between the patient's successful alcohol recovery and his or her tobacco addiction allows smoking cessation to be redefined in a way that is familiar to the patient and may increase the possibility of successful cessation.21
TABLE 1 Stage-Based Counseling Strategies for Smoking Cessation in Recovering Alcoholic Patients
| Precontemplation stage: patient is not considering quitting in the next six months | |
| 1. Take a smoking history (if not previously done) that includes the following: the age at which the patient started smoking; the amount smoked per day; the brand of cigarettes smoked; the length of time after awakening before the patient has the first cigarette; the number of past attempts to quit and the length of time off cigarettes each time; the reasons for relapse; concerns about quitting; changes in smoking behavior since the patient has been in recovery; and potential barriers to quitting (family, friends, co-workers, etc.). | |
| 2. Assess the patient's knowledge by asking an open-ended question: “What do you know about the increased risks to your health from your history of heavy drinking and smoking?” | |
| 3. Assess the patient's cognitive rationale for smoking, using the positive/negative technique: | |
| “What is positive about smoking for you?” | |
| “What would be negative about quitting for you? Are you concerned that trying to quit smoking might make it harder to stay off alcohol?” | |
| “What would be positive about quitting for you?” | |
| “What would be negative about continuing to smoke? Do you think of your smoking as an addiction in the same way that your previous alcohol use was an addiction?” | |
| 4. Give a strong message about the patient's need to stop smoking and your willingness to help when he or she is ready: “I encourage all my patients who smoke to quit. This is especially important for those with a history of heavy drinking. I'd like you to stop smoking. If you're unable to do so today, then I'd like you to think about it and let me know how I can help when you're ready.” Consider giving patient education materials appropriate to the patient's stage of readiness to change. | |
| 5. Update the patient's smoking status and stage of readiness to change at each office visit. Record the patient's smoking status in the chart at each visit. (Label the charts of current smokers so that all staff members can participate in counseling for smoking cessation.) | |
| 6. Document the stage and intervention in the patient's record, including the increased risk because of his or her past alcohol history. | |
| Contemplation stage: patient is considering quitting in the near future but has made no commitment, as indicated by action in the past year | |
| 1. Take a smoking history, if not previously done (see Precontemplation, item 1). | |
| 2. Assess cognitive rationale for smoking, using the positive/negative technique (see Precontemplation, item 2). | |
| 3. Identify reasons for not committing to quit by asking the patient the following questions: | |
| “What is it that keeps you from setting the date and quitting?” | |
| “Do you have any concerns about maintaining your sobriety if you attempt to quit smoking?” | |
| “How did you overcome any similar concerns you had about trying to quit alcohol?” | |
| 4. Give a strong, nonjudgmental message about the patient's need to stop smoking and your willingness to help when he or she is ready: “I'm ready to help you whenever you choose to commit to quit. I consider your smoking to be as serious a threat to your health as your drinking was. You might think about how you were able to successfully lick that problem.” | |
| 5. Encourage the patient to “experiment” with quitting: “As with drinking, you'll eventually need to go ‘cold turkey’ in order to successfully quit smoking. In the meantime, you can learn more about your addiction to cigarettes and how to manage the cravings by experimenting.” Suggested patient strategies might be stopping smoking for 24 hours and keeping a diary of what it feels like, or cutting out, for one to two weeks, the two or three cigarettes that are hardest to give up each day and keeping track of effective coping techniques, or reducing the number of cigarettes smoked each day by one half for one week. Consider giving patient education materials that are appropriate to the patient's stage of readiness to change. | |
| 6. Document stage, intervention and follow-up in the patient's record. | |
| Preparation stage: the patient is planning to quit smoking in the near future and has made a genuine attempt to quit in the past year | |
| 1. Take a smoking history, if not done previously (see Precontemplation, item 1). | |
| 2. Reinforce the patient's desire to quit and offer support. Define the patient's desire to quit in the same positive framework as his or her decision to get into alcohol recovery: “We both know that this won't be easy, but neither was getting sober. It's the best gift you could give yourself and your family. I'll help you all the way.” | |
| 3. Discuss the patient's past quit attempts, if any, including particular strategies that were helpful, along with situations that led to relapse. Ask if alcohol use was involved in previous returns to smoking. | |
| 4. Help the patient develop an explicit plan for quitting, including a quit date, strategies for coping with problem situations and rewards for success. Discuss the patient's experience with getting sober. How did the patient do it? What worked best? How did the patient manage cravings to drink? How does the patient feel about himself or herself for successfully working through the alcohol cessation program? How might the patient apply 12-step concepts to quitting smoking? Consider the possibility of using nicotine replacement therapy (see the guidelines of the Agency for Health Care Policy and Research19). Give patient education materials appropriate to the patient's stage of readiness. | |
| 5. Explain the difference between temporary and permanent relapses, and the need to keep working on the plan regardless of slips. Emphasize “one day at a time.” | |
| 6. Schedule follow-up contact in one to two weeks. The contact does not need to be a clinic visit. In fact, telephone contact may be more acceptable to both the patient and the physician. Use of support staff in this role may be more efficient. Discuss sources of outside support, such as getting a “sponsor” to help with the plan, attending nonsmoking Alcoholics Anonymous meetings, attending a Nicotine Anonymous program (if available) and doing daily meditations on being smoke-free and coping with cravings. | |
| Action stage: the patient successfully implements new behavior | |
| 1. Continue positive reinforcement and support as needed until the patient has been abstinent for one year. | |
| 2. Encourage the patient to call or come to the office as soon as possible if he or she relapses. | |
| Relapse or maintenance stage: patient has either relapsed to smoking or has maintained abstinence from smoking for one year | |
| 1. If the patient has relapsed, assess the reason and discuss how the patient thinks he or she might handle smoking cessation differently the next time. | |
| 2. Following a relapse, assess the patient's current stage of readiness to quit again. Recycle through the process. | |
| 3. If the patient is maintaining abstinence, periodically reinforce behavior. | |
Trying to persuade a patient who is in the precontemplation stage to agree to quit smoking is a frustrating, time-consuming activity that is likely to fail. However, getting the patient to discuss concerns about quitting and presenting information on the risks involved with smoking are accomplishable goals. Thus, setting a quit date is realistically reserved for a patient who is in the preparation stage. In summary, the overall approach of the readiness-to-change model is based on the recognition that smoking is an addictive, complex behavior, and that change takes time.
Motivational Counseling
While many physicians voice concerns about repeatedly “nagging” patients who have indicated no interest in quitting smoking, they also feel obligated to provide good care. As described in one text, “Motivational interviewing is a particular way to help people recognize and do something about their present or potential problems. It is particularly useful with people who are reluctant to change and ambivalent about changing. It is intended to resolve ambivalence and to get a person moving along the path to change.”18
The key components of motivational interviewing, or counseling, are a nonpaternalistic, nonjudgmental attitude on the part of the physician, an orientation that accepts patients as they are, and techniques that encourage and reinforce patient self-responsibility. A complete description of motivational counseling is beyond the scope of this article. In brief, the five basic principles of motivational counseling are as follows:
Express Empathy. In providing smoking cessation counseling for a patient in recovery from alcoholism, the physician needs to express empathy in order to convey acceptance of the patient's current situation. Acceptance does not mean agreement with, or approval of, the patient's behavior. Rather, it is the respectful desire to understand the patient's frame of reference. It acknowledges that changing behavior is difficult and involves feelings of ambivalence.
Respectful listening and reflection of feelings are two key communication skills for this task. For example, the physician might say the following: “So, it seems like you think you should stop smoking at some point, but you're afraid that quitting both smoking and drinking would be too hard. I would like to tell you about some facts that have recently come to light on that subject.”
Develop Discrepancy. This is accomplished by creating and amplifying incongruities between the patient's present behavior and his or her stated personal goals. Using skillful questioning to help the patient clarify goals and explore consequences, the physician can often get the patient to present his or her own reasons for needing to change. This approach can be much more effective than subjecting the patient to another lecture, because it allows the patient to think about his or her behavior without feeling pressured and coerced. The following remarks could accomplish this goal: “I know that you are interested in protecting your health and your family's well-being by the fact that you've worked so hard at attaining sobriety. What do you know about the additional risk that smoking holds for people with a past history of heavy alcohol use?”
Avoid Argumentation. Arguing with a patient tends to evoke resistance. As a result, both the physician and the patient are likely to come away feeling dissatisfied and more entrenched in their own positions. While motivational counseling is confrontational in its goals, it is not confrontational in its style. Resistance by the patient is a signal to the physician to change strategies: “I can see that you're just not ready to try quitting right now. I would ask that you give some thought to what we have talked about, and let me know if and when you're ready. I'd like to help.”
Roll with Resistance. The physician can also “roll with resistance” by using the momentum of the patient's resistance to shift his or her perspective. Turning a question or problem over to the patient is an excellent way to do this. This approach encourages the patient to use his or her own resources to solve the problem. For example, the physician might use the following statements: “Smoking is the main way that you cope with stress, and you're worried about giving it up. That's understandable. Did you learn any methods in your recovery program that could help you when you decide to tackle this addiction?”
Support Self-Efficacy. This is the only possible path to change. The concept of self-efficacy can be difficult, because it requires a shift in perception that often seems at odds with professional ethics and values. Most physicians understand that they cannot force patients to change their behavior. However, physicians often feel inadequate or frustrated when they are unable to persuade patients to do what is best for them. As a result, they often avoid the topic of smoking cessation or nag patients about quitting smoking.
In the physician training program at the University of Nebraska Medical Center, residents are encouraged to respect the patient's right to make decisions about his or her own behavior. At the same time, residents are encouraged to define for themselves what they need to do in order to feel as if they have fulfilled their professional responsibilities. This letting go of the responsibility for change often frees the physician to listen more empathically and to assume a less authoritarian position. Using this approach, the physician can make statements such as the following: “You're not ready to make any plans to quit right now, but I'm glad we've had a chance to talk about it. You've shown good judgment in the past by getting into alcohol recovery, and we both know these things take time.”
The stage of readiness to change should be identified during every office visit for patients who are in alcohol recovery but continue to smoke. Specific stage-based activities and motivational counseling techniques should also be used with these patients. These interventions require only three to five minutes, assuming that the tobacco-use history was obtained in a previous visit.
Final Comment
The evidence that smoking cessation intervention does not endanger sobriety has been accumulating steadily since 1983.10–14,22–26 Tobacco cessation counseling for recovering alcoholic patients is important and efficacious. Smoking cessation does not appear to negatively affect sobriety—and may even enhance sobriety.
While more research is needed to identify the most effective techniques for increasing smoking cessation in recovering alcoholics, physicians can use several tools to enhance their care of these patients. The first tool is patient education. Many patients in alcohol recovery are not aware that they have an increased risk for health problems related to smoking. Furthermore, they probably do not know about the positive effects of smoking cessation on abstinence. Physicians also must address the fears of these patients and dispel the beliefs that derive from traditional treatment folklore.
The model discussed in this article is another important tool for physicians. Using this model, physicians can provide brief, tailored interventions based on concepts that are already familiar to patients in alcohol recovery. Finally, specific counseling techniques can increase the likelihood of a cooperative dialog that may enhance the motivation of both patients and physicians to address the serious problem of tobacco addiction.

