All antidepressants are equally effective in treating depression, and all have approximately equivalent rates of onset of action. Pathare and Paton review the combination of factors that affect the choice and effectiveness of antidepressant medications, including clinical and patient characteristics, side-effect profile and experience of the prescribing physician.
Because certain types of depression respond particularly well to specific medications, obtaining a detailed diagnostic history is important. A previous experience of similar episodes of depression and the response of specific agents can be particularly helpful (see the accompanying figure). Patients with mixed anxiety and depression respond well to selective serotonin reuptake inhibitors. Patients with agitated depression may do best with a sedating tricyclic agent such as amitriptyline; the best choice for a patient with atypical depression may be monoamine oxidase inhibitors, and a stimulating agent such as imipramine may help when social withdrawal is a prominent feature of depression. Patients with depression that is accompanied by delusions and psychotic features often have a poor response to antidepressants when used alone, but the addition of an antipsychotic drug greatly improves the outcome.
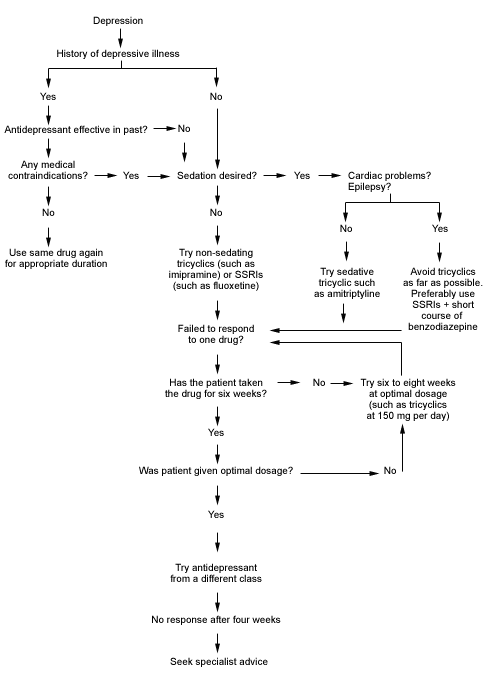
Decision tree for drug treatment of depression. (SSRIs = selective serotonin reuptake inhibitors)
The risk of suicide in patients with depression is difficult to predict and may be minimized by providing adequate dosages of an appropriate antidepressant and regulating the quantity of the medication provided, particularly if tricyclic antidepressants are used. Selective serotonin reuptake inhibitors are safer if the potential for a patient to overdose exists, but these drugs are significantly more expensive than tricyclic antidepressants.
Too small a dosage of antidepressants given for too short a time is the most common problem with the use of antidepressants. Approximately 70 percent of patients respond to the first agent administered if it is given in therapeutic doses (such as amitriptyline at 150 mg daily or fluoxetine at 20 mg daily) for six to eight weeks. Noncompliance is a frequent cause of the patient's apparent failure to respond to therapy. If the patient does not improve following an adequate trial of therapy given at an optimal dosage, options include increasing the dosage if the patient can tolerate it or changing the antidepressant to an agent of a different chemical class. Up to 15 percent of patients respond to a change in medications at this stage.
The risk of relapse following a single episode of depression is approximately 65 percent within the first year in patients who stop taking medication. As only 15 percent of those who continue to take antidepressant medication relapse, the authors conclude that younger patients should continue medication for at least six months following remission of symptoms. Elderly patients and those with recurrent symptoms should be maintained on antidepressant medication for at least two years after symptoms are controlled.

