
Am Fam Physician. 1998;58(6):1292-1296
Dramatic decreases in hypertension-related mortality from strokes and heart attacks have occurred in the 25 years since the National High Blood Pressure Education Program (NHBPEP) began: a 59.0 percent reduction for stroke mortality and a 53.2 percent reduction for coronary heart disease (CHD) mortality. These decreases resulted from a concerted effort to encourage physicians to conduct blood pressure screening in their patients and treat hypertension and to inform the general population about the importance of knowing their own blood pressure values and seeking treatment for hypertension.
Among educational methods used by NHBPEP are periodic guidelines from the Joint National Committee (JNC) on Prevention, Detection, Evaluation and Treatment of High Blood Pressure. The Sixth Report of the JNC (JNC-VI) has recently been published1; it details some unsettling trends, as discussed in the article by Kaplan.2 The first trend can be found in U.S. death rates for strokes and CHD from 1972 to 1994. The stroke curve is practically level, and the rate of decline of the age-adjusted mortality rates from CHD has slowed. Also, the incidence of end-stage renal disease related to hypertension continues to increase (Figure 1), as does the prevalence of CHD (Figure 2).
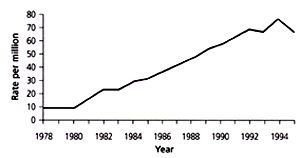
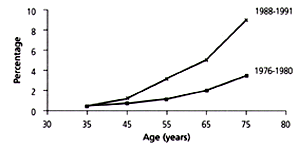
Finally, findings from the recent Third National Health and Nutrition Examination Survey (NHANES III, phase 2)1 show that awareness, treatment rates and control of hypertension are lower than expected from previous trends (Table 1). In addition, recent reports show that blood pressure control had deteriorated in patients in a Minnesota survey3 and in a cohort of elderly persons in Iowa.4 These various trends, although unexplained, suggest that physicians should be more vigilant in controlling hypertension.
The goal for the treatment of hypertension is a blood pressure level of less than 140/90 mm Hg or as low as tolerated.1 The latter goal is important for patients with renal disease and hypertension because a reduction in blood pressure to 130/85 mm Hg or lower (125/75 mm Hg) in those who also have proteinuria (defined as over 1 g per 24 hours) is recommended to slow the progressive decline in the glomerular filtration rate.5 That hypertension itself without preexisting renal disease is a risk factor for end-stage renal disease was found in the long-term follow-up of several thousand men who were screened for the Multiple Risk Factor Intervention Trial6; this was particularly true among African Americans.
Another group deserving heightened attention is elderly persons, because they have a higher incidence of hypertension. For example, NHANES III7 found that the prevalence of hypertension was 60 percent in non-Hispanic whites, 71 percent in African Americans and 61 percent in Mexican Americans 60 years of age or older. Not only is the prevalence of hypertension among elderly persons an important consideration, but the number of elderly persons with hypertension is also important. These numbers have increased greatly, and increases will continue. By 2030, the number of U.S. citizens 65 years of age or older is expected to be 70 million—up from 33 million in 1994.8 Thus, unless hypertension can be prevented, millions of additional people will need treatment for high blood pressure.
Ample evidence now shows that drug therapy for elderly patients with hypertension can reduce the incidence of stroke and heart attack. The NHBPEP recently reviewed data from seven trials9; in all, benefit was achieved with drug therapy for stroke, CHD and cardiac failure. Isolated systolic hypertension was the focus of the Systolic Hypertension in the Elderly Program (SHEP) Trial.10 This trial was randomized and placebo controlled, and enrolled 4,736 participants 60 years of age or older. The patients in the trial first received chlorthalidone, then received atenolol, if necessary. Average pretreatment blood pressure values in the drug- and placebo-treated groups were 171/77 mm Hg and 170/76 mm Hg, respectively. Blood pressure values in the subjects who received treatment averaged 142/68 mm Hg over five years, and blood pressure values in the placebo group averaged 155/74 mm Hg (Figure 3). Strikingly, the difference of 13.6 mm Hg resulted in a reduced stroke rate of 36 percent and a reduced myocardial infarction rate of 27 percent. If such benefits can be achieved with minor decreases in blood pressure, imagine what might be gained by a tolerated reduction to even lower levels.
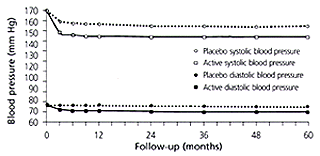
It seems wise, therefore, that all physicians pay close attention to the blood pressure values that they achieve with treatment of their patients—be it with nonpharmacologic modalities or antihypertensive drugs—and aim for strictly normal levels if such are well tolerated.
Current hypertension control is just not good enough. We can do much better.