The exercise stress test is a useful screening tool for the detection of significant coronary artery disease. Documentation of the patient's symptoms, medications, past and current significant illnesses, and usual level of physical activity helps the physician determine if an exercise stress test is appropriate. The physical examination must include consideration of the patient's ability to walk and exercise, along with any signs of acute or serious disease that may affect the test results or the patient's ability to perform the test. The test report contains comments about the maximal heart rate and level of exercise achieved, and symptoms, arrhythmias, electrocardiographic changes and vital signs during exercise. This report allows the clinician to determine if the test was “maximal” or “submaximal.” The quality of the test and its performance add to the validity of the results. The conclusion section of the test report indicates whether the test results were “positive,” “negative,” “equivocal” or “uninterpretable.” Further testing may be indicated to obtain optional information about coronary artery disease and ischemic risk if the test results were equivocal or uninterpretable.
Despite advances in disease prevention, coronary artery disease remains a major cause of illness and death in the United States.1,2 The costs of treating this disease and the indirect costs resulting from lost work and wages are substantial.3 The exercise stress test is a useful tool for detecting coronary artery disease and for evaluating medical therapy and cardiac rehabilitation following myocardial infarction.4,5
In addition to the standard exercise stress test, other methods of cardiovascular stress testing include scintigraphy and echocardiography (Table 1).4–9 Exercise stress scintigraphy uses a radioactive tracer to enhance abnormal areas of myocardial blood flow. Stress scintigraphy can be performed with pharmacologic agents instead of exercise if the patient's condition does not allow sufficient physical activity for performing the study. Echocardiography has recently been used in combination with exercise or pharmacologic stress testing as yet another form of noninvasive cardiac evaluation.
TABLE 1 Suggested Cardiac Stress Testing Based on the Clinical Circumstances
| Test and CPT code* | Indication | Medicare reimbursement | Typical office charge |
|---|---|---|---|
| Standard exercise stress test (treadmill, bicycle, ergometer); 93015 | Typical angina; atypical angina; normal findings on ECG in a patient with risk of coronary artery disease | $ 98.89 | $175 to 250 |
| Exercise stress test scintigraphy (e.g., thallium-201); 93015 and 78461 | Abnormal findings on baseline ECG that limit value of standard exercise stress test; standard test produced equivocal or unexpected results | 298.00 | 350 to 450 |
| Pharmacologic stress scintigraphy; 93015 and 78461 | Typical angina with poor exercise capacity; severe obesity; patient is receiving antianginal agents, which may blunt heart rate; paced rhythm, significant ectopy or left bundle branch block; poor exercise tolerance; severe congestive heart failure; unstable angina with known coronary artery disease | 298.00 | 350 to 450 |
| Echocardiography combined with either pharmacologic or exercise stress test; 93350 and 93015 | Moderate to severe pulmonary disease, especially COPD, and poor exercise tolerance; assessment of wall motion or valvular function with increased heart rate; may help distinguish single-vessel and multiple-vessel disease | 238.71 | 350 to 600 |
CPT = current procedural term; ECG = electrocardiogram; COPD = chronic obstructive pulmonary disease.
*—CPT code includes performance and interpretation.
Competence and Equipment Requirements
The clinical competence to perform exercise stress testing is usually granted by staff privileges in health care institutions. The Joint Commission on Accreditation of Healthcare Organizations requires that institutions assess competence on the basis of criteria established in the medical staff bylaws. A combined specialty task force, composed of members from the American College of Cardiology (ACC), the American College of Physicians and the American Heart Association (AHA), in 1996 issued a statement on clinical competence in exercise testing.10
Equipment requirements for exercise stress testing include a bicycle ergometer or treadmill, a monitor system, a medical crash cart and a defibrillator. Equipment costs can range from $15,000 to $40,000. Personnel requirements include the examiner and one other person trained in basic cardiac life support, although someone with advanced cardiac life support skills is preferred.4,11
Sensitivity and Specificity
Exercise stress testing provides a controlled environment for observing the effects of increases in the myocardial demand for oxygen; significant fixed stenoses from coronary artery disease result in electrocardiographic (ECG) evidence of ischemia.5
Particularly difficult to detect is evidence of fixed stenoses with collateral blood flow, as well as low-grade (less than 50 percent) stenoses. These abnormalities may not produce sufficient impairment of blood flow to affect the ECG. Some studies indicate that low-grade stenoses are often the source of spontaneous thrombosis, leading to the sudden development of significant stenosis, infarction and sudden death because such lesions do not have the benefit of collateral blood flow.12 An exercise stress test would not be helpful in detecting this type of lesion.13
The estimation of the pretest probability of a significant fixed stenosis should be based on the patient's age, gender, symptoms, concurrent medical conditions, medications and physical examination, as well as on the clinician's diagnostic experience with symptoms of myocardial ischemia.5 This information is helpful for determining the potential utility of an exercise stress test for a given patient.5,14
The sensitivity of exercise stress testing ranges from 23 to 100 percent, and the specificity ranges from 17 to 100 percent.5,7,10 For example, in an abnormal exercise stress test in which a man reaches a heart rate of 85 percent of the predicted maximum for his age, the sensitivity and specificity for the diagnosis of significant coronary artery disease is 65 percent and 85 percent, respectively.10,11 A more detailed discussion of sensitivity, specificity, population effect and probability analysis is available in the ACC/AHA Task Force Report on Exercise Stress Testing.7,10
Indications for the Standard Exercise Stress Test
Table 27 summarizes the currently accepted indications for exercise stress testing. Consideration may be given to obtaining this test when patients present with symptoms of coronary artery disease, including the classic anginal symptoms of chest pressure or pain that occurs with or without exertion. Atypical presentations or anginal equivalents, such as shortness of breath or dyspnea on exertion, are also appropriate indications for this study.4,5,7,13
Patients with coronary artery disease who have undergone surgical intervention or are receiving medical therapy can perform an exercise stress test when they are medically stable and symptom-free. The study can be used to assess the effectiveness of treatment. After myocardial infarction, patients may be candidates for exercise stress testing at a low level of exercise to determine functional capacity and identify any ECG changes or symptoms during exercise.15 With this information, the clinician is often able to prescribe an exercise regimen or more aggressive therapy, or to select the appropriate tests for further evaluation.16,17
Asymptomatic healthy persons may be considered as candidates for exercise stress testing if they are in high-risk occupations (e.g., pilots, firefighters, law enforcement officers, mass transit operators).7 In addition, the American College of Sports Medicine (ACSM) recommends an exercise stress test for all women 50 years of age and older and all men 40 years of age and older who plan to engage in vigorous exercise. The ACSM does not recommend exercise stress testing for asymptomatic healthy persons who are not planning vigorous exercise, regardless of the person's age.18
An exercise stress test may also be considered in asymptomatic patients who have two or more risk factors for coronary artery disease or a concurrent chronic disease, such as diabetes, that carries a high risk of coronary disease. Patients with valvular disorders (except those with hemodynamically significant aortic stenosis) may undergo an exercise stress test to evaluate their functional capacity, the effectiveness of treatment, their symptom complex or the need for surgical intervention.
Pretest Evaluation
The history, physical examination and laboratory studies necessary to evaluate the patient's suitability for performing an exercise stress test are summarized in Table 3.
TABLE 3 Summary of Pertinent Data to Obtain Before Exercise Stress Testing
| History | |
| Type, character, duration, radiation of symptoms | |
| Chest pain | |
| Atypical presentation | |
| Associated symptoms | |
| History of other medical conditions | |
| Hypertension | |
| Diabetes | |
| Pulmonary disease | |
| Lipid abnormalities | |
| CNS disease, including cognitive disorders | |
| Coagulation or platelet abnormalities | |
| Physical limitations | |
| Medications | |
| General activity level and exercise expectations, goals or needs | |
| Physical examination | |
| General appearance, including gait and mobility | |
| Cardiac—murmurs, gallop, rhythm, assessment of valvular function | |
| Pulmonary—rales, wheezes | |
| Vascular—bruits, pulses | |
| Musculoskeletal—limb strength and mobility | |
| Laboratory studies | |
| Screening chemistry and hematologic profiles | |
| Resting ECG | |
CNS = central nervous system; ECG = electrocardiogram.
In addition, the patient should receive the proper preparatory instructions for the exercise stress test as required by the hospital or the testing laboratory. Instructions usually include no food intake for six to 12 hours before the study. Patients should be told to wear loose-fitting, comfortable clothing and comfortable walking shoes. In addition, instructions about modifying the doses of any medications should be given.
HISTORY
In addition to the presence and character of chest pain, concurrent medical conditions such as claudication, severe physical disabilities and pulmonary disease should be considered in view of their effects on the patient's ability to exercise. Such conditions may render the patient unable to perform the test. Exercise usually worsens uncontrolled hypertension, and the pretest evaluation may be terminated because of this finding.15
The patient's general activity level and pulmonary reserve and the presence of arthritic disease may influence the type of exercise test protocol selected and the duration and level of activity achieved. Many exercise protocols exist to accommodate patients who need to walk at a slower pace or advance through exercise stages at a slower rate.
The patient's current medications are important. Nitrates may mask the occurrence of chest pain; beta-adrenergic blockers may blunt the heart rate response to exercise, and digoxin (Lanoxin) may produce abnormal ST-segment depression.
PHYSICAL EXAMINATION
A general physical examination with special attention to the systems listed in Table 3 usually is adequate for the pretest evaluation. Cardiac examination should include an assessment for the presence of murmurs and valvular disease. Severe valvular dysfunction, especially aortic stenosis, is an absolute contraindication to exercise stress testing.4,7 Gallop rhythms are noteworthy because the presence of an S3 may indicate significant congestive heart failure, a contraindication if it is clinically severe. While the development of an S4 during exercise may indicate significant cardiac ischemia, detection of it during a physical examination does not signify ischemia and is not grounds for not performing an exercise stress test.7
A thorough pulmonary examination is helpful in detecting signs of severe pulmonary disease or congestive heart failure disorders that may not be obvious from the patient's history. Pulmonary pathology may render the patient unable to walk on a treadmill or use the exercise equipment.
An assessment of the vascular system should include palpation of the carotid and peripheral pulses, as well as evaluation for the presence of bruits over the abdominal aorta and other larger vessels. Because claudication of the lower extremities or transient ischemic attack–type symptoms can occur during exercise, another type of stress testing that does not require exercise should be considered if the physical examination suggests that these problems are clinically significant.7
Assessment of the musculoskeletal system includes evaluation of the patient's ability to walk at a moderate to fast pace without significant gait disturbances. The hips, shoulders, arms and legs should allow relatively full mobility and support during exercise.
LABORATORY STUDIES
Screening laboratory studies are obtained to diagnose subclinical disease that may be present. Exercise stress testing should not be performed in patients with symptoms of anemia or severe hepatic, renal or metabolic disorders.
A resting ECG is an essential part of the pretest evaluation. The patient should have a resting ECG that is free of the abnormalities listed in Table 4. While the presence of any of these ECG changes is not an absolute contraindication to exercise stress testing, they may interfere with the validity of the test by altering the ECG changes that are consistent with ischemia during exercise. Most authorities suggest an imaging study in addition to exercise stress testing as a part of the cardiac evaluation in most patients with these changes on the baseline ECG.19 It should be noted, however, that in these persons, an exercise stress test could potentially be used to evaluate functional capacity, blood pressure response or other clinically determined parameters.
TABLE 4 Baseline ECG Changes That May Obscure Exercise Stress Test Results
| ST-segment changes* (≥ 1 mm) | |
| Depression or elevation | |
| Ventricular strain patterns | |
| Right ventricular hypertrophy | |
| Left ventricular hypertrophy | |
| T-wave changes* | |
| Inversions—secondary to strain or old injury | |
| Conduction abnormalities | |
| Left bundle branch block: ST-segment and T-wave changes | |
| Right bundle branch block: ST-segment and T-wave changes (in V1, V2 and V3 leads only) | |
| Prolonged QT interval | |
ECG = electrocardiogram.
*—In multiple leads, representing one wall or area of the ventricle.
Potential Contraindications to Exercise Stress Testing
ABSOLUTE CONTRAINDICATIONS
Table 5 lists the absolute contraindications to exercise stress testing. Exercise stress testing may worsen the patient's condition or place the patient at increased risk of cardiac instability or injury in the setting of acute myocardial infarction, unstable angina, acute cardiac inflammation, severe congestive heart failure, uncontrolled sustained ventricular arrhythmias, symptomatic supraventricular arrhythmia, high-grade block, hemodynamically significant aortic stenosis or severe hypertension. Patients with such conditions usually require immediate medical or surgical intervention as clinically indicated but may be reassessed as candidates for exercise stress testing when the acute problems are resolved. The remaining contraindications listed in Table 5 render the patient physically unable to perform an exercise stress test.4,7,13
TABLE 5 Absolute Contraindications to Exercise Stress Testing
| Acute myocardial infarction or unstable angina | |
| Acute cardiac inflammation | |
| Pericarditis | |
| Endocarditis | |
| Myocarditis | |
| Severe congestive heart failure | |
| Uncontrolled sustained ventricular arrhythmias, symptomatic supraventricular arrhythmias or high-grade block | |
| Hemodynamically significant aortic stenosis | |
| Severe hypertension (systolic pressure > 200 mm Hg or diastolic pressure >110 mm Hg) | |
| Severe acute medical illness, drug toxicity or electrolyte abnormalities | |
| Active thromboembolic processes | |
| Pulmonary embolism | |
| Deep venous thrombosis | |
| Poor candidate for exercise | |
| Extreme obesity, with weight exceeding the recommendations or the equipment capacity (usually > 159 kg [350 lb]) | |
| Severe mental or physical disabilities | |
RELATIVE CONTRAINDICATIONS
Relative contraindications to exercise stress testing are listed in Table 6. While patients with these conditions may undergo a standard exercise stress test, they require special consideration because the presence of these conditions may invalidate the test results.
TABLE 6 Relative Contraindications to or Conditions Requiring Special Consideration for Exercise Stress Testing
| Current medications | |
| Digoxin | |
| Type I antiarrhythmic agents (e.g., quinidine, procainamide [Pronestyl], disopyramide [Norpace]) | |
| Tricyclic antidepressants | |
| Vasodilators (nitrates, alpha-adrenergic blockers, alcohol, other antihypertensive agents) | |
| Beta-adrenergic blockers | |
| Metabolic abnormalities | |
| Acid-base disorders | |
| Thyroid abnormalities | |
| Abnormal calcium, magnesium or potassium levels | |
| Vasoregulatory disorders | |
| Other cardiac conditions | |
| Mitral valve prolapse syndrome | |
| Wolff-Parkinson-White syndrome | |
| Recurrent paroxysmal supraventricular or atrioventricular nodal tachyarrhythmias | |
In most cases, medications should not be withheld in preparation for an exercise stress test.4,7,11 Patients can be instructed to take their medications before an exercise stress test, with the exception of insulin and oral hypoglycemic agents. Depending on how stable the patient's diabetic condition is, all of the dose of insulin or the hypoglycemic agent or one half of the dose should be withheld before the test.
Digoxin may depress the ST-segments. If ST-segment depression of 1 mm or more is present on the baseline ECG, use of ECG criteria for exercise-induced ischemia during exercise will be difficult. Type I antiarrhythmic agents and tricyclic antidepressants are proarrhythmogenic. For example, if at baseline a patient receiving any one of these medications has significant ectopy, the patient is at increased risk of hemodynamically significant arrhythmias with exercise and should not undergo exercise stress testing.7
The antihypertensive effect of beta blockers, alpha blockers and nitroglycerin may cause significant hypotension during exercise. In general, orthostatic blood pressure assessment and a careful history will identify most patients susceptible to such a response. Beta blockers may also blunt the heart rate during exercise. While patients receiving beta blockers may perform the exercise required for the test, the usual age-adjusted target heart rate may not be a realistic end point for them.
Most electrolyte and endocrinologic abnormalities can affect the heart rate and ST-segment and T-wave changes on a resting ECG, and they may affect the patient's ability to exercise as well.20 Vasoregulatory problems from central and peripheral autonomic neuropathy associated with disorders such as diabetes, Parkinson's disease and Shy-Drager's syndrome may cause profound vasodilation and hypotension during exercise. The pretest evaluation should alert the clinician to the presence of this tendency, and exercise stress testing should not be performed if such a response to exercise seems significant.4
Patients who have a history of tachyarrhythmias may be considered candidates for exercise stress testing, but those with easily reproduced tachycardia during exercise or other heavy physical activity are not candidates for exercise stress testing. Such a problem may be found in patients with mitral valve prolapse syndrome, Wolff-Parkinson-White syndrome and episodic or periodic supraventricular tachycardia. The occurrence of a tachyarrhythmia during exercise stress testing could cause syncope or, at a minimum, produce an inconclusive result.
Understanding the Results
Most exercise stress tests are interpreted in a standard format that includes an interpretation (or comment) section and a conclusion section.21 Table 7 summarizes the currently accepted interpretation and conclusion categories and their subsections. Each section may not be described in every report because some of them may not be relevant or particularly useful in every clinical circumstance.
TABLE 7 Standard Format for Reporting the Results of an Exercise Stress Test
| Items included in interpretation of the results | |
| Basic ECG interpretation | |
| Symptoms reported during stress testing | |
| Reason for ending exercise | |
| Estimate of exercise capacity in METS | |
| Blood pressure response | |
| Presence and frequency of arrhythmias or ectopy | |
| ECG changes (type and location) observed during the test | |
| Conclusions | |
| Positive | |
| Negative | |
| Equivocal | |
| Uninterpretable | |
| Goal achieved | |
| Maximal | |
| Submaximal | |
ECG = electrocardiogram; METS = metabolic equivalents.
INTERPRETATION
An interpretation of the baseline ECG is included in the report, noting any abnormalities and changes that occurred with changes in position (standing, lying or sitting). Symptoms occurring during the exercise stress test are usually reported as well. Most commonly, these comments are described as “fatigue,” “legs tired,” “chest pain/pressure,” “shortness of breath,” etc. If these symptoms were severe, they may have been the reason for discontinuing the test. Other reasons cited for stopping the test may be “target heart rate achieved,” “exercise stopped per patient's request,”“equipment malfunction” or “ECG findings or criteria were met.”
Also usually described are the duration of the exercise period and the workload in METS (metabolic equivalents, or resting oxygen consumption of about 3.5 mL per kg per minute).22 The interpreter may also add subjective comments about the patient's exercise capacity; for example, the report may state “poor exercise tolerance (3 to 4 METS)” or “good exercise tolerance (10 to 11 METS).” The cardiorespiratory fitness levels established by the ACSM can serve as general guidelines.18
Increases or decreases in blood pressure during exercise and rest are also noted. Hypotension, defined as a drop of more than 10 mm Hg in the systolic blood pressure during exercise, may signify severe cardiac ischemia.15 Opinions vary as to the definition of a hypertensive response to exercise, but most authorities accept as a maximal limit a systolic pressure of 230 mm Hg. The diastolic blood pressure during exercise usually varies 10 mm Hg in either direction. A 10 mm Hg decrease in the diastolic blood pressure during the postexercise period is not unusual and is considered physiologic.21,22
While the presence of arrhythmias may or may not carry clinical significance, their frequency, type and appearance or disappearance with exercise and rest are also noted.
The final category of information provided in the report is the ECG response during exercise and recovery. Findings usually include the presence and location of ST-segment changes, P-wave, T-wave and U-wave changes, and the appearance of conduction abnormalities during the exercise and recovery periods.15,23
TEST CONCLUSIONS
Positive Results. Figure 1 shows the ECG findings suggestive of myocardial ischemia; Table 8 lists the clinical findings suggestive of a positive test.
FIGURE 1. Exercise Stress Test
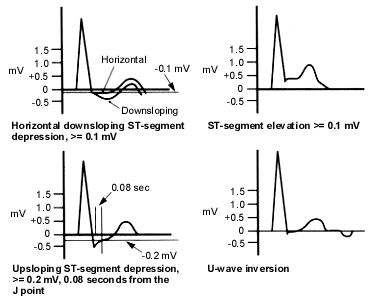
Electrocardiographic (ECG) findings suggestive of a positive exercise stress test. In addition to the ECG findings depicted here, the occurrence of frequent premature ventricular contractions (PVCs), multifocal PVCs or ventricular tachycardia at mild exercise (less than 70 percent of maximal heart rate) is suggestive of an exercise stress test positive for myocardial ischemia.
TABLE 8 Clinical Findings That Suggest an Exercise Stress Test Positive for Ischemia
| Exercise-induced hypotension |
| Exercise-induced angina or anginal equivalents |
| Appearance of an S3, S4 or heart murmur during exercise |
S3 = third heart sound; S4 = fourth heart sound.
An exercise stress test positive for myocardial ischemia may be further qualified with the terms “probably” and “strongly.” For example, hypotension (a drop of more than 10 mm Hg in systolic pressure) or large (more than 2 to 3 mm) ST-segment depressions, either alone or in combination, are strongly positive test results. The presence of these abnormalities leaves little clinical doubt that significant coronary artery disease exists.4 The appearance during exercise of an S3, S4 or murmur indicates cardiac muscle dysfunction and therefore ischemia.4 The interpreter may also comment on the recovery or return to baseline of these findings as well as any interventions needed to bring about this change.
Negative Results. A negative test result is simply the lack of any of the above-mentioned findings. Some normal physiologic and ECG changes may occur during exercise (Table 9).
TABLE 9 Nonsignificant Findings During Exercise Stress Testing
| Fatigue, dyspnea, diaphoresis, flushing | |
| Incremental increase in blood pressure and heart rate | |
| ECG changes | |
| Shortening of QT interval | |
| Functional J point depression ≤ 0.2 mV for < 0.06 seconds in duration | |
| Peaking of T waves and P waves | |
| Shortening of P-R interval | |
ECG = electrocardiogram.
Equivocal, or Inconclusive, Findings. Equivocal exercise stress test results are summarized in Table 10. These ECG changes are not diagnostic of ischemia.21 Alterations in the P-wave and T-wave morphology and changes in atrioventricular conduction with exercise are considered nondiagnostic if the changes revert to baseline in the rest period. The appearance of unifocal, premature atrial contractions or premature ventricular contractions (fewer than five per minute) is not a specific indicator for coronary artery disease.23 The development of intraventricular blocks, such as right bundle branch block, left bundle branch block and hemiblocks, is a nondiagnostic finding. An intraventricular block may also obscure ischemic changes and hinder further interpretation of the ECG. As with all inconclusive results, additional testing is needed. In most cases, an imaging study, exercise scintigraphy or echocardiography is needed to document ischemia.
TABLE 10 Inconclusive, or Nondiagnostic, Findings on Exercise Stress Testing
| Development of clinically insignificant arrhythmias |
| Unifocal premature ventricular contractions |
| Atrial or junctional tachyarrhythmias |
| Development of blocks |
| Primary or secondary type I atrioventricular block |
| Bundle branch blocks |
| Hemiblocks |
| Changing atrioventricular conduction |
| Morphology changes |
| T-wave flattening |
| P-wave changes < 0.01 mV |
| ST depression < 0.10 mV |
Uninterpretable Results. In addition to equipment failure, other causes of uninterpretable test results include the patient's or operator's inability to complete the test before any goals are met. Further diagnostic studies should be planned, and any information that could have contributed to this result should be included in the report. For example, the patient may have appeared on physical examination to be a good exercise candidate but was unable or unwilling to comply with the requirements of the exercise stress test. In this case, the reason for noncompliance can help the clinician choose another examination that would be more appropriate for the patient.
Maximal and Submaximal Exercise Stress Test. A maximal exercise stress test is one that achieves the target heart rate, exercise level or time limit established for the patient. In most cases, the goal is the target heart rate, as calculated with the following formula: (220 − patient's age) × 0.85 beats per minute. An exercise stress test that does not meet the expected goal is called a submaximal study.6,18 If the stress test is submaximal because of decreased exercise capacity or noncardiac symptoms, consideration should be given to obtaining radionuclide scintigraphy or echocardiographic studies that do not include exercise as a component of the evaluation.5,20,24

