Despite widespread support for the concept of advance care planning, few Americans have a living will or a health care proxy. Advance care planning offers the patient the opportunity to have an ongoing dialog with his or her relatives and family physician regarding choices for care at the end of life. Ultimately, advance care planning is designed to clarify the patient's questions, fears and values, and thus improve the patient's well-being by reducing the frequency and magnitude of overtreatment and undertreatment as defined by the patient. An advance directive consists of oral and written instructions about a person's future medical care in the event he or she becomes unable to communicate. There are two types of advance directives: a living will and a health care power of attorney. Family physicians are in an ideal position to discuss advance care plans with their patients. By introducing the subject during a routine office visit, physicians can facilitate a structured discussion of the patient's wishes for end-of-life care. At the next visit, further discussion can include the patient and his or her proxy. A document that clearly delineates the patient's wishes is then developed. The patient should be assured that the directive can be changed at any time according to the patient's wishes. The advance care plan should be reviewed periodically to make sure the specifications continue to be in line with the patient's wishes.
Attention to the issues that surround death and dying is growing. Some people argue that in the quest to cure disease, the age-old intent to alleviate suffering has been lost. Relief of suffering is a central, albeit sometimes neglected, goal of medical care. Evidence suggests that physicians do not adequately address the needs of dying patients and their families.1 Patients frequently suffer from inadequate control of pain and other symptoms, from a lack of communication about their illness and the options for treatment, from poor psychosocial and spiritual support and from haphazard discharge planning.2
Results from the SUPPORT Trial
Data from the SUPPORT trial1 provide a picture of the failure to address the needs of dying patients. This four-year study was conducted at five U.S. teaching hospitals and included 9,105 seriously ill patients. The study was designed to improve the care of patients near the end of life.
In the observational phase of the study, the investigators found that nearly one half (49 percent) of the patients who indicated they wanted cardiopulmonary resuscitation (CPR) withheld did not have do-not-resuscitate (DNR) orders written in their medical charts during that hospitalization. While almost one third of the patients preferred that CPR be withheld, less than one half of the physicians were aware of their patients' preferences.
Among patients who died in the observational phase of the study, almost one half (46 percent) received mechanical ventilation within three days of death, and more than one third (38 percent) spent at least 10 days in an intensive care unit (ICU). Eight days was the median duration these patients spent in an ICU, in a comatose state or on mechanical ventilation. Fifty percent of the conscious patients who died in the hospital were reported to have moderate to severe pain at least one half of the time. Decision-making capacity for many of these patients was clearly compromised. The investigators concluded that their findings “confirmed substantial shortcomings in [the] care [of] seriously ill hospitalized adults.”
Goal of Advance Care Planning
In 1990, a committee of the World Health Organization argued in a report on palliative care for cancer pain that curative care and palliative care are not mutually exclusive.3 Currently, palliative care is generally perceived as a measure limited to the last weeks or days of a patient's life. For cancer care at least, the committee argued that palliative care should be a gradually increasing component of care from diagnosis until death (Figure 1).
FIGURE 1. Allocation of Medical Care Resources
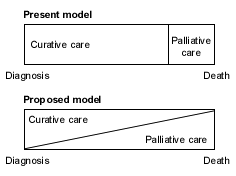
World Health Organization model for allocation of medical care resources.
Despite the enactment of the Patient Self-Determination Act in 1991,4 fewer than 40 percent of hospitalized patients have advance directives.5,6 The goal of advance care planning is to promote high-quality personalized care of patients who, because of serious illness, become unable to communicate their values, concerns and wishes (Table 1). Introducing the subject in the office setting, before the patient becomes seriously ill, is a way family physicians can help patients make their wishes for end-of-life care known.
Content of Advance Care Planning
Advance care planning is an ongoing process that offers the patient the opportunity to have a dialog with his or her family members and physician regarding the choices for care at the end of life. The important issues concerning the patient's questions, fears and values are explored. As the issues are uncovered, the information can be translated into a plan of action, called the advance directive.
Given the continuity of care provided by family physicians and the breadth of the relationships that develop between family physicians and their patients, the family physician is ideally suited to begin this dialog and follow through with this process. Numerous opportunities arise in the outpatient setting to initiate and follow the process of advance care planning.
ADVANCE DIRECTIVES
Descriptions of the different types of advance directives are summarized in Table 2. An advance directive consists of a person's oral and written instructions about his or her future medical care, in the event he or she becomes unable to communicate, becomes incompetent to make health care decisions (during a terminal illness) or is in a persistent vegetative state.
TABLE 2 Terminology Used in Advance Care Planning
| Term | Definition |
|---|---|
| Advance care planning | The process (rather than a single consultation or the signing of a statutory document) of discussing end-of-life care with the patient and developing a valid expression of the patient's wishes regarding future medical care. Advance care planning aims to improve the process of health care decision making and produce a better outcome of care. |
| Advance directive | A person's oral and written instructions about his or her future medical care, in the event he or she becomes unable to communicate. Each state has different regulations for the use of advance directives. There are two types of advance directives: a living will and a health care power of attorney. |
| Health care power of attorney | A document in which the patient appoints someone to make decisions about his or her medical care if he or she cannot make those decisions. This type of advance directive is sometimes called a health care proxy, durable power of attorney for health care decisions or appointment of a health care agent. The person appointed may be called a health care agent, surrogate, attorney-in-fact or proxy. |
| Living will | A written form of advance directive in which a patient's wishes regarding the administration of medical treatment are described if the patient becomes unable to communicate at the end of life. State law may define when the living will goes into effect and may limit the treatments to which the living will applies. The patient's right to accept or refuse treatment is protected by constitutional and common law. Living wills can be general or very specific. |
| Patient Self-Determination Act | The federal law that requires health care facilities receiving Medicaid and Medicare funds to inform patients of their right to execute advance directives. Both federal and state laws govern the use of advance directives. All 50 states and the District of Columbia have laws recognizing the use of advance directives. |
There are two types of advance directives: a health care power of attorney and a living will. The health care power of attorney, or health care proxy, is a document by which the patient appoints a trusted person to make decisions about his or her medical care if he or she cannot make those decisions. A living will is a written form of advance directive in which the patient's wishes regarding the administration of medical treatment are delineated in case the patient becomes unable to communicate his or her wishes.
Advance Care Planning in the Outpatient Setting
Unfortunately, most people do not open a discussion about their end-of-life wishes with their physician. Studies have shown that patients believe physicians should initiate this process.7 Therefore, it is important for the physician to invite patients and their family members to have discussions with each other and with the physician to clarify and document the patient's values, concerns and choices regarding end-of-life treatment and care.
Advance care planning in the hospital setting is often hobbled by the circumstances that led to the admission. The thoughts and decision-making processes of the very sick are often complicated by emotional pressures, physical discomfort and the effects of various medications. Patients may be frightened, confused, depressed or medicated. Evidence suggests that postponing the discussion of these issues until the patient is hospitalized and seriously ill may prove to be too late for any beneficial effect.1
The SUPPORT investigators concluded that “to improve the experience of seriously ill and dying patients, greater individual and societal commitment and more proactive and forceful measures may be needed.”1 A physician-initiated discussion of the advance care plan in the outpatient setting is an important proactive measure.
The outpatient setting is ideal for developing an advance care plan, and the primary care physician is well situated to initiate the discussion.8,9 A survey of 883 patients sheds light on the opinions and preferences of patients and physicians.7 Patients indicated that the discussion should be initiated by the physician early in the physician–patient relationship and early in the course of the patient's disease. They also believed the discussion should be conducted in an outpatient setting and that the closest person in their lives should be included in the discussion.
The survey also showed that the respondents wanted detailed information, with an emphasis on the outcomes of life-sustaining treatment. Flexibility was desired in terms of the amount of time devoted to the discussion. Supplemental information in the form of a videotape or reading material was also desired. The findings of the survey seem to indicate that the issue of death and dying is not as delicate a subject as physicians may believe and that patients do not need, or want, to be protected from this information.10
Procedures that are generally addressed in advance directives are listed in Table 3. The advance care plan is a process interwoven into the ongoing physician–patient relationship. It is an integrated aspect of good, day-to-day medical care, not merely a single clinical encounter or a signature on a document. A discussion of this nature does not need to take up much time.10 It can easily be incorporated into an annual health maintenance examination or a follow-up visit for a progressive illness. A physician-initiated discussion of advance directives has been shown to be welcomed and appreciated by patients.11–14
TABLE 3 Interventions that Might Be Addressed in Advance Directives
| Cardiopulmonary resuscitation |
| Mechanical ventilation |
| Hemodialysis |
| Chemotherapy |
| Artificial nutrition or hydration |
| Transfusion of blood or blood products |
| Intravenous therapy |
| Pacemaker insertion |
| Antibiotic use |
| Surgery |
Implementing and Following the Advance Care Plan
Emanuel and colleagues15 translated the broader concepts of advance care planning, research and clinical experience into a set of practical recommendations for clinicians. The following is a distillation of the most salient features of their work.
The five steps identified in the ideal process of advanced care planning are as follows: (1) raise the topic and give information regarding the advance directive and health care proxy; (2) facilitate a structured discussion; (3) complete a statement, date and record it and have the patient supply copies to the proxy and anyone else deemed appropriate (i.e., clergy); (4) periodically review and update the directive, and initial and date all changes; and (5) implement the plan by following the patient's wishes when the appropriate time comes. These steps are described in Table 4.
TABLE 4 Steps for Incorporating Advance Care Planning into the Outpatient Setting
| Step | Activity |
|---|---|
| 1. Introduce the topic and give information to the patient. | Bring up the subject during an office visit. |
| Provide patient with information from a brochure, videotape, Internet sites, etc. | |
| 2. Facilitate the discussion. | Invite proxy to attend (with patient's permission). |
| Develop a draft of the directive and proxy. | |
| Allow time for reflection and discussion with others. | |
| 3. Complete directive and document in medical record. | Test the patient's resolution by providing clinical examples. |
| Provide a copy of the directive to the patient, proxy and others, as needed. | |
| Put copies of directive and proxy form in patient's chart. | |
| 4. Review and update directive. | Consider the need to review and update at a time of change in the patient's medical condition or life circumstance. |
| 5. Apply directive when patient is unable to communicate. | Avoid rigid application to unpredicted circumstances. |
| Interpret patient's previous statements together with document. | |
| Align with health care proxy to attempt to make decisions the patient would have made. |
Adapted from Emanuel LL, Danis M, Pearlman RA, Singer PA. Advance care planning as a process: structuring the discussions in practice. J Am Geriatr Soc 1995;43:440–6.
INTRODUCING THE SUBJECT OF END-OF-LIFE CARE
The language used to introduce the advance care plan to the patient can diminish any reluctance the physician may feel about broaching the issue. The subject of advance care planning may be introduced as follows: “Mrs. Jones, I'd like to talk with you regarding your health care in the future if you become seriously ill. This is a conversation I have with all of my patients and doesn't reflect on your health in particular. Many experts recommend that we all consider what level of health care we would want in case of a future illness where our ability to communicate may be impaired. In fact, I myself have made plans for the care I want if I become seriously ill. There is even a federal law that helps to ensure that all people are aware that advance planning for their medical care is available to them. I think it's important to discuss these issues. Is this something you have thought about or discussed before?”
This approach frames a difficult topic in a sensitive fashion and allows the patient to express his or her level of understanding and comfort with the issue. By taking the initiative, the physician is demonstrating that his or her respect and concern for the patient transcend immediate clinical demands. It communicates to a patient that he or she will not be abandoned at a vulnerable time.
Providing the patient with supplemental educational material, such as a videotape or brochure, is often helpful in supporting the discussion16 (Table 5). The patient may also be referred to a representative of the clergy or a social worker for further discussion. The introductory discussion may be concluded by giving the patient appropriate forms and offering to continue the discussion at the next visit. The family member or friend to be designated as the proxy should be invited and encouraged to attend the next visit.
TABLE 5 Some Sources of Information on End-of-Life Issues
| Internet sites | |
| http://www.choices.org | |
| Internet site for Choice in Dying. While Choice in Dying does not oppose physician-assisted dying, its principal work involves educating the public about advance directives. A booklet, “ Questions and Answers: Advance Directives and End-of-Life Decisions,” is available. Specific state advance directive and health care proxy forms can be downloaded free of charge from the Web site. 475 Riverside Dr., Room 1852 New York, NY 10115 Telephone: 212-870-2040 or 800-989-9455 E-mail: cid@choices.org | |
| http://www.soros.org:80/death.html | |
| Internet site for the Project on Death in America, which seeks to transform the culture of dying by supporting initiatives in research, scholarship, the humanities and the arts, and by fostering innovation in the provision of care, in public and professional education, and in public policy. | |
| http://www.hcfa.gov:80/Medicare/advdir.htm | |
| Internet site for obtaining information on the advance directive and health care proxy from the Health Care Financing Administration. | |
| Journal articles and books | |
| Doukas DJ, Brody H. Care at the twilight: ethics and end-of-life care. Am Fam Physician 1995;52:1294–6. | |
| Doukas DJ, McCullough LB. The values history. The evaluation of the patient's values and advance directives. J Fam Pract 1991;32:145–53. | |
| Doukas DJ, Reichel W, eds. Planning for uncertainty: a guide to living wills and other advance directives for health care. Baltimore: Johns Hopkins University Press, 1993. | |
| Emanuel LL, Danis M, Pearlman RA, Singer PA. Advance care planning as a process: structuring the discussions in practice. J Am Geriatr Soc 1995;43:440–6. | |
| This is a defining presentation of ways to implement the advance care plan in the outpatient setting. | |
FOLLOWING THROUGH WITH DISCUSSIONS
When the patient returns for the next visit, the physician can begin the discussion by eliciting information about the patient's wishes and concerns. It is important to try to understand the patient's goals in a range of possible scenarios. This may be approached by asking the patient if there are situations that he or she especially fears. The patient's general values and specific wishes can be outlined by developing a mock advance directive form in pencil as the patient discusses his or her wishes. The patient should be assured that the form is a first draft and that he or she will have opportunities to make changes.
Importantly, issues raised during this conversation help to ensure that the patient does not formulate expectations of the physician that run counter to the physician's guiding moral, ethical and professional principles for end-of-life care. It should be noted that if a physician at some point cannot, for reasons of conscience, comply with the advance directive the patient would like to have, the physician must provide continuing care and must help the patient transfer to another physician's care.
This visit may be the first opportunity for the physician and the proxy to meet and take the first step in forming an alliance in support of the patient. The proxy, by virtue of his or her relationship to the patient, may have a degree of difficulty in separating his or her own motives and preferences from those of the patient. These differences can be raised and pointed out as the physician helps the proxy to understand his or her role. The proxy should be encouraged to listen to and help clarify the patient's wishes.
COMPLETING THE ADVANCE CARE PLAN
After the patient has had the opportunity to discuss these important considerations, the next step can be taken. The completed statement, based on the information obtained in the discussions with the patient, can be used to review the patient's preferences. It is important to document the patient's wishes in clear and detailed language to minimize the risk of later confusion between the physician and the patient's family members when the patient may be unable to communicate.
As an indication that the document has been reviewed, the physician should sign and date it. The original is returned to the patient, and copies are placed in the patient's chart and given to the proxy and anyone else the patient deems appropriate, such as family members, the patient's clerical representative and the patient's lawyer. The patient should be reminded that he or she is not permanently committed or “boxed in” at this or any other point in the process.
REVISING THE ADVANCE CARE PLAN
Thereafter, the advance care plan can be revisited and revised at any time. The written document is a “living” document and, as such, is subject to change. Occasions for revision may arise when the patient's medical condition or relationship to the proxy changes. However, because studies have demonstrated that patients' wishes regarding end-of-life decisions tend to remain consistent over time, it is reasonable to explore the reasons for the patient's desire to alter the plan.17 Any change should be documented and dated, and the revised copy should be placed in the patient's chart and given to the patient, the proxy and any other parties deemed appropriate by the patient.
On the other hand, if the patient affirms in a follow-up discussion that the wishes expressed in the document remain the same, a note to this effect should be made in the chart. Such documentation helps to confirm the consistency of the patient's wishes.
IMPLEMENTING THE ADVANCE CARE PLAN
The final step in the process is the application of the directive in an actual situation. Because all possible case scenarios could not have been anticipated during the previous steps, application of the directive will inevitably entail a measure of estimated interpretation. Action aimed at fulfilling the patient's intentions is the goal.18
The physician's role at this stage is to diagnose the condition, convey opinions and, if the patient has lost the ability to communicate, offer judgment to the proxy, just as if the proxy were the patient. The proxy, at this time, should attempt to serve as the voice of the patient. Together, the physician and the proxy collaborate to follow through with the plan of action that is thought to most closely approximate the course the patient would have taken, based on an understanding of the patient's previously stated values and directives.
Final Comment
To maximize the efficacy of an advance care plan, Danis19 reinforces this approach with the following suggestions:
- Make sure that copies of an advance directive are in the possession of all relevant parties and ensure that a copy is also in the patient's medical record.
- Recognize that a written document cannot substitute for an explicit discussion of the patient's wishes.
- Discuss the patient's wishes again when his or her health status changes, because the patient's wishes may have changed.
- Appreciate that all circumstances cannot be anticipated in a specific treatment directive and, thus, a goal-oriented discussion should complement the discussion of specific treatment preferences.
- Recognize that an individual advocate or an institutional commitment to respecting advance directives will increase the likelihood that a plan will be followed.
Finally, physicians are not automatically obliged to comply with patients' requests for treatment when they believe such requests are ill-advised, harmful or futile. Strict adherence to such requests may interfere with the physician's autonomy and ability to provide sound medical care.

