Ludwig's angina is a potentially life-threatening, rapidly expanding, diffuse inflammation of the submandibular and sublingual spaces that occurs most often in young adults with dental infections. However, this disorder can develop in children, in whom it can cause serious airway compromise. Symptoms include severe neck pain and swelling, fever, malaise and dysphagia. Stridor suggests an impending airway crisis. Causative bacteria include many gram-negative and anaerobic organisms, streptococci and staphylococci. Initial treatment consists of high doses of penicillin G given intravenously, sometimes in combination with other drugs. Patients usually recover without complications.
Ludwig's angina was described initially by Wilhelm Frederick von Ludwig in 1836. Five patients had marked swelling of the neck that progressed to involve the tissues covering the muscles between the larynx and the floor of the mouth. Ludwig described indurated edema of the submandibular and sublingual areas with minimal throat inflammation but without lymph node involvement or suppuration. At that time, the condition was almost always fatal.1,2
Illustrative Cases
CASE 1
A 14-month-old girl was admitted to the hospital because of swelling below the chin that had increased during the previous two days. Fever developed on the day of admission, and she had reduced fluid intake and urine output.
On physical examination, a tender, indurated, warm swelling that spread laterally was seen in the submental area (Figure 1). An excoriated oval lesion was present on the chin. The child was uncomfortable and preferred to keep her mouth open. She had no respiratory distress or cyanosis. Her temperature (taken rectally) was 38.8°C (101.8°F); respiratory rate was 34 breaths per minute; and heart rate was 166 beats per minute. The oxygen saturation, in room air, was 95 percent.
FIGURE 1.
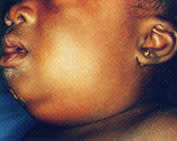
Marked submental swelling in the patient in illustrative case 1; note open mouth.
Neck radiographs revealed marked submandibular soft tissue prominence that was characteristic of Ludwig's angina. No abscess was seen on ultrasonogram.
The white blood cell count was elevated, with a shift to the left. Blood culture was sterile. The illness resolved following initial treatment with intravenous oxacillin followed by oral dicloxacillin.
CASE 2
A boy aged 33 months presented to the emergency department because of progressive enlargement under the chin for one day and inability to swallow. Three weeks earlier, he had fallen and injured his nose.
On examination, the patient had swelling, erythema and tenderness in the submandibular area. Pain prevented him from opening his mouth (Figures 2 and 3). His temperature was 38.8°C (101.8°F); cardiac and respiratory rates were normal; and no respiratory distress was noted.
FIGURE 2.
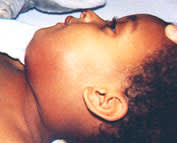
Tender swelling in patient in illustrative case 2. Patient is unable to open mouth.
FIGURE 3.
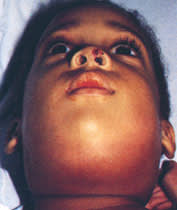
Note spread of swelling laterally and abrasion on nose in same patient as shown in Figure 2.
The white blood cell count was 14,600 cells per mL (14.6 × 109 per L), with elevated band forms. Radiographs of the neck showed marked soft tissue prominence; no foreign body was present. Ludwig's angina was diagnosed clinically, and treatment with intravenous nafcillin was started.
By the third day of treatment, the submental tenderness, erythema and induration began to resolve. Incision and drainage produced approximately 10 mL of purulent material. Culture was sterile, as was the initial blood culture.
Improvement was obvious within 24 hours of the surgical treatment. The boy was discharged after seven days of treatment with intravenous nafcillin and was continued on a course of oral penicillin for an additional 10 days.
Anatomic Considerations
A knowledge of neck spaces and fascial relationships is important in diagnosing and treating neck infections. Spaces created by various fasciae of the neck are potential areas of infection. Invasion by bacteria produces cellulitis or abscess, and spread occurs by continuity along these paths of least resistance, rather than by lymphatic channels.3,4
The submandibular space is composed of two spaces separated anteriorly by the mylohyoid muscle: the sublingual space, which is superior, and the submaxillary space, which is inferior. The spread of infection is halted anteriorly by the mandible and inferiorly by the mylohyoid muscle5 (Figure 4). The infectious process expands superiorly and posteriorly, elevating the floor of the mouth and the tongue. The hyoid bone limits the process inferiorly, and swelling spreads to the anterior aspect of the neck, causing distortion and a “bull neck” appearance5 (Figure 5). This then evolves to an infectious compartment syndrome of the submandibular and sublingual spaces.6
FIGURE 4.
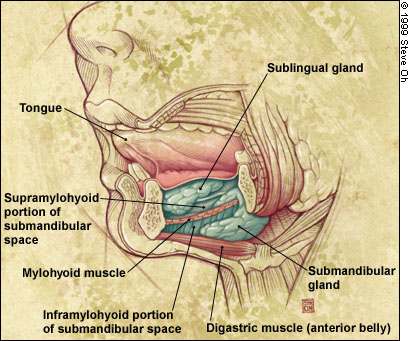
Sublingual space, superior to mylohyoid muscle. The submandibular space is inferior to the mylohyoid muscle.
FIGURE 5.
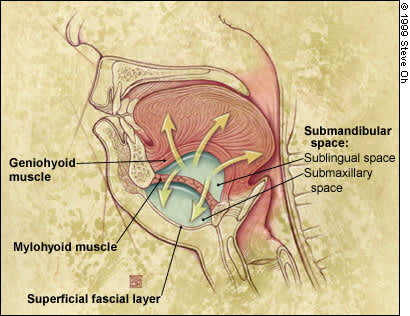
Spread of process superiorly and posteriorly elevates floor of mouth and tongue. In anterior spread, the myoid bone limits spread inferiorly, causing a “bull neck” appearance.
Clinical Features
In a study spanning a 13-year period,7 Ludwig's angina was diagnosed in 41 patients, of whom 10 (24 percent) were children. Another study,8 involving 110 patients who had deep neck abscesses, included 21 children aged 10 years and younger. Ludwig's angina has been reported in infants as young as 12 days.9–12
Predisposing factors include dental caries, recent dental treatment, sickle cell disease, a compromised immune system, trauma and tongue piercing.13 Ludwig's angina in children can occur de novo, without any apparent precipitating cause.7
The signs and symptoms of Ludwig's angina are the result of a rapidly expanding cellulitis. Severe pain and neck swelling occur in virtually all patients.14 Fever, toothache, malaise, dysphagia and fetid breath are common. Trismus also occurs, as experienced by the child in the second illustrative case.15
A child may sit leaning forward to maximize the airway. Examination may reveal carious molar teeth, neck rigidity or drooling. The presence of stridor, dyspnea, decreased air movement or cyanosis requires prompt attention because it may indicate an impending airway crisis.
The bacterial isolates vary and are often mixed. α-Hemolytic streptococci, staphylococci and bacteroides are commonly reported. Other anaerobes such as peptostreptococci, peptococci, Fusobacterium nucleatum, Veillonella species and spirochetes are also seen. A foul breath odor usually indicates the presence of an anaerobe. Gram-negative organisms such as Neisseria catarrhalis, Escherichia coli, Pseudomonas aeruginosa and Haemophilus influenzae have also been reported.6 A β-hemolytic streptococcus was isolated in 18 percent of a large series of patients with deep neck abscesses.8 Antibiotic treatment before hospital admission often results in sterile cultures.
Treatment
Treatment includes assessment and protection of the airway, use of intravenous antibiotics, surgical evaluation and, if necessary, operative decompression. Recommended initial antibiotics are high-dose penicillin G, sometimes used in combination with an anti-staphylococcal drug or metronidazole (Flagyl I.V.). In penicillin-allergic patients, clindamycin hydrochloride (Cleocin HCl) is a good choice.
Alternative choices include cefoxitin sodium (Cefoxil) or combination drugs such as ticarcillin-clavulanate (Timentin), piperacillin-tazobactam (Zosyn) or amoxicillin-clavulanate (Augmentin).8 Intravenous dexamethasone sodium phosphate (Decadron), given for 48 hours, has been beneficial in reducing edema, which helps maintain airway integrity and enhances antibiotic penetration.6
Surgical drainage may be indicated if no clinical improvement is seen within 24 hours. In one series of 41 patients, including 10 children, seven were treated successfully with conservative medical management. Incision and drainage were necessary in three patients. Tracheostomy was necessary in only one child. One of the 10 children died.7 The airway remains the major concern because it can be compromised with little warning.
Final Comment
Ludwig's angina can be fatal. Failure to diagnose deep neck infections promptly may be caused by a clinical picture that is altered by previous antibiotic use. With early diagnosis, aggressive intravenous antibiotic therapy and management in an intensive care unit, the process should resolve without complications.

