
Am Fam Physician. 1999;60(1):245-246
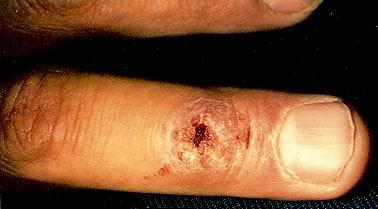
A 35-year-old man who is employed at a pet store presented with a nodule on a finger (see the photograph). For four weeks the nodule increased in size, but it had remained the same size for the past three weeks. The patient also had a small, slightly tender epitrochlear lymph node. The patient had completed 10-day courses of dicloxacillin and then cephalexin without noticeable benefit. Exploration undertaken in the emergency department for a possible foreign body in the nodule only made it more painful.
Question
Discussion
The answer is C: Localized infection with Mycobacterium marinum can follow contamination of a minor abrasion (or a preexisting cut) obtained while cleaning aquariums—hence the name “fish-tank granuloma.” The organism is a free-living fish pathogen that occurs in fresh, salt and brackish water.1 Evidence of local infection usually appears two to six weeks after inoculation and may follow any aquatic activity, from fishing and boating to skin diving. Local infection may occur in immunocompetent persons and can spread in a “sporotrichoid” pattern, characterized by a series of similar nodules extending along local lymphatics. Deeper infections in the musculoskeletal system may occur, rarely, but systemic disease occurs almost exclusively in immunocompromised persons.
Other infections that may present with such a solitary nodule in an otherwise healthy person include sporotrichosis, nocardiosis, leishmaniasis, tuberculosis and actinomycosis. In an immunocompromised person with a solitary nodule, cutaneous coccidioidomycosis, histoplasmosis and aspergillosis should be considered. Neoplasms such as squamous cell carcinoma and keratoacanthoma may resemble the nodule in this photograph. Diagnosis is best made by biopsy, with bacterial, fungal and mycobacterial culture of tissue. Histologic results of all of these infections may reveal pseudoepitheliomatous hyperplasia, which can mimic squamous cell carcinoma. To avoid unwarranted (and unsuccessful) surgery, the receiving pathologist or dermatopathologist should be informed about the diagnostic considerations so that special stains, including that for acid-fast bacilli, may be ordered.
M. marinum is generally resistant to penicillins and cephalosporins and is uniformly resistant to isoniazid (INH). Effective treatment includes tetracycline, doxycycline (Vibramycin), minocycline (Minocin), trimethoprim-sulfamethoxazole (Bactrim), an aminoglycoside such as amikacin (Amikin) or kanamycin (Kantrex), a combination of ethambutol (Myambutol) and rifampin (Rifadin), or the quinolones.2 Duration of treatment ranges from six weeks to 18 months depending on clinical response.
Microsporum canis is a dermatophyte fungus carried by dogs, cats and people, and is a frequent cause of tinea corporis. Young kittens in the household are frequently implicated in widespread cases. Red, scaled rings would be more typical of this condition.
Staphylococcus aureus can cause deep-tissue inflammation in botryomycosis (a chronic soft tissue infection) but should have responded to the medications that this patient had received.
Borrelia burgdorferi is the spirochete responsible for Lyme disease. Erythema chronicum migrans usually presents as a slowly expanding red ring, not as a discrete nodule on a digit.
“Flesh-eating strep” is the appellation given to a particularly aggressive streptococcus serotype that produces necrolytic enzymes and can spread deep and wide within hours. Rapidly advancing induration, dusky discoloration and pain disproportionate to the apparent disease should alert the physician to this diagnosis, especially in a patient who appears very ill.