Dyspepsia, often defined as chronic or recurrent discomfort centered in the upper abdomen, can be caused by a variety of conditions. Common etiologies include peptic ulcers and gastroesophageal reflux. Serious causes, such as gastric and pancreatic cancers, are rare but must also be considered. Symptoms of possible causes often overlap, which can make initial diagnosis difficult. In many patients, a definite cause is never established. The initial evaluation of patients with dyspepsia includes a thorough history and physical examination, with special attention given to elements that suggest the presence of serious disease. Endoscopy should be performed promptly in patients who have “alarm symptoms” such as melena or anorexia. Optimal management remains controversial in young patients who do not have alarm symptoms. Although management should be individualized, a cost-effective initial approach is to test for Helicobacter pylori and treat the infection if the test is positive. If the H. pylori test is negative, empiric therapy with a gastric acid suppressant or prokinetic agent is recommended. If symptoms persist or recur after six to eight weeks of empiric therapy, endoscopy should be performed.
Dyspepsia is upper abdominal pain or discomfort that is episodic or persistent and often associated with belching, bloating, heartburn, nausea or vomiting.1 The condition is reported to occur in approximately 25 percent (range: 13 to 40 percent) of the population each year, but most affected persons do not seek medical care.2,3 Nonetheless, dyspepsia is responsible for substantial health care costs (medications and diagnostic evaluations) and considerable time lost from work. Even though dyspepsia is a highly prevalent condition, no definitive studies have as yet established guidelines for the work-up of dyspeptic patients in the primary care setting.
It is well accepted that patients with peptic ulcer disease associated with Helicobacter pylori infection should be treated with antibiotics to eradicate the organism.4 However, this implies that a diagnosis of ulcer and H. pylori infection has been confirmed.
The approach to previously uninvestigated dyspepsia is more difficult. It includes differentiating the cause of dyspepsia, selecting among the available options for initial management and distinguishing between patients who require endoscopy and those who can safely receive empiric drug therapy. The challenge is further increased by the controversy surrounding the role of H. pylori in nonulcer dyspepsia.5,6
Differential Diagnosis
Because the differential diagnosis of dyspepsia is broad, initial efforts should be focused on the most common etiologies (Table 1).7,8 In about 50 to 60 percent of patients, a specific etiology is not identified (i.e., “functional” or nonulcer dyspepsia).7,9,10 Many of these patients are hypothesized to have an augmented perception of visceral pain.8
TABLE 1 Differential Diagnosis of Dyspepsia
| Diagnostic category | Approximate prevalence* | |
|---|---|---|
| “Functional” dyspepsia† | Up to 60 percent | |
| Dyspepsia caused by structural or biochemical disease | ||
| Peptic ulcer disease | 15 to 25 percent | |
| Reflux esophagitis | 5 to 15 percent | |
| Gastric or esophageal cancer | < 2 percent | |
| Biliary tract disease | Rare | |
| Gastroparesis | Rare | |
| Pancreatitis | Rare | |
| Carbohydrate malabsorption (lactose, sorbitol, fructose, mannitol) | Rare | |
| Medications (see Table 4) | Rare | |
| Infiltrative diseases of the stomach (Crohn's disease, sarcoidosis) | Rare | |
| Metabolic disturbances (hypercalcemia, hyperkalemia) | Rare | |
| Hepatoma | Rare | |
| Ischemic bowel disease | Rare | |
| Systemic disorders (diabetes mellitus, thyroid and parathyroid disorders, connective tissue disease) | Rare | |
| Intestinal parasites (Giardia, Strongyloides) | Rare | |
| Abdominal cancer, especially pancreatic cancer | Rare | |
*—Prevalence figures are based on the occurrence of the disorders in patients with dyspepsia who are investigated with endoscopy.
†—Functional or nonulcer dyspepsia is defined as a history of at least three months of dyspepsia with no definite structural or biochemical explanation.
Information from Talley NJ, Silverstein MD, Agreus L, Nyren O, Sonnenberg A, Holtmann G. AGA technical review: evaluation of dyspepsia. Gastroenterology 1998;114:582–95, and Fisher RS, Parkman HP. Management of nonulcer dyspepsia. N Engl J Med 1998;339:1376–81.
Structural conditions commonly associated with dyspepsia include peptic ulcers and gastroesophageal reflux disease (GERD). Gastric or esophageal cancers are serious causes but account for fewer than 2 percent of cases.7,11
History
A thorough history is important in evaluating the patient with dyspepsia, although symptoms alone may not be very useful in establishing a specific diagnosis. One group of investigators found extensive symptom overlap when they attempted to categorize patients into diagnostic groups, which included ulcer-like, dysmotility-like, reflux-like and unspecified dyspepsia.12 Reflux-like symptoms may be of greater diagnostic value in that symptoms alone can reasonably identify the presence of GERD.6,13 However, symptom identification is only a small part of the full clinical evaluation of dyspepsia. Questions that may be useful in identifying other causes of dyspepsia-like symptoms are presented in Table 2.
TABLE 2 Questions to Ask When Determining Common Causes of Dyspepsia
| Peptic ulcers |
| Does the patient have a personal history of ulcers? |
| Does the patient have a strong family history of ulcers? |
| Does the patient report melena? |
| Is the patient a smoker? |
| Gastroesophageal reflux disease |
| Does the patient complain of heartburn or sour belches? |
| Are symptoms worse when the patient is lying down? |
| Does the patient have a chronic cough or hoarseness? |
| Biliary tract disease |
| Does the patient report any history of jaundice? |
| Does the patient report dark urine? |
| Does pain occur after meals? |
| Is the pain associated with meals or belching? |
| Pancreatitis |
| Is the pain stabbing, and does it radiate to the patient's back? |
| Is the pain abrupt, is it unbearable in severity and does it last for many hours without relief? |
| Does the patient have a history of heavy alcohol use? |
| Cancer |
| Is the patient over 50 years of age? |
| Has the patient had a recent significant weight loss? |
| Does the patient have trouble swallowing? |
| Has the patient had recent protracted vomiting? |
| Does the patient have a history of melena? |
| Is the patient a smoker? |
| Irritable bowel syndrome |
| Is dyspepsia associated with an increase in stool frequency? |
| Is pain relieved by defecation? |
| Metabolic disorders |
| Does the patient have a medical history of diabetes mellitus, hypothyroidism or hyperthyroidism, or hyperparathyroidism? |
| Medications |
| Is the patient currently taking medications commonly associated with dyspepsia? |
PEPTIC ULCER DISEASE
Patients who present with dyspepsia should be asked about risk factors associated with peptic ulcers. If a patient has a history of ulcers, a recurrent lesion is likely.14 Risk factors for ulcers include a family history of ulcers,15 a history of nonsteroidal anti-inflammatory drug (NSAID) use16 and current cigarette smoking.16–18
GASTROESOPHAGEAL REFLUX DISEASE
Reflux-like dyspepsia, or GERD, can be distinguished from other gastrointestinal disorders with reasonable accuracy on the basis of symptoms.6,13 The two symptoms that define this disorder are heartburn and regurgitation.1 The epigastric burning sometimes radiates to the throat and worsens when a patient eats, bends down or lies flat.19 Esophageal spasm from gastroesophageal reflux is characterized by sharp, stabbing substernal pain. Heartburn and esophageal reflux and spasm commonly occur at night or after the consumption of a large meal. If the diagnosis of GERD is uncertain, intraesophageal pH monitoring may help in separating the disease from other causes of dyspepsia.7,13
GASTROPARESIS
Dysmotility-like dyspepsia, or gastroparesis, is associated with symptoms of bloating, abdominal distention, flatulence and prominent nausea.1,19 Patients with this condition tend to feel hungry but have premature satiety with resultant epigastric heaviness or fullness even after the consumption of small meals.19 Gastroparesis should be suspected in a symptomatic patient who has diabetes mellitus, especially when peripheral neuropathy is present.
IRRITABLE BOWEL SYNDROME
The abdominal pain associated with irritable bowel syndrome may frequently be confused with the pain of nonulcer dyspepsia.20 However, the syndrome is generally associated with abnormal bowel habits and can usually be distinguished from nonulcer dyspepsia by the symptoms listed in Table 3.21
BILIARY TRACT DISEASE
Gallstones are common and often asymptomatic. When pain occurs, it is episodic and severe, and may last for hours.9 Unlike the pain associated with peptic ulcers, the pain in gall bladder disease tends to occur after eating, especially after the consumption of a large fatty meal. Patients with dyspepsia should also be asked about the presence of dark urine, jaundice and acholic stools.9
MALIGNANCY AND OTHER SERIOUS DISEASES
Fortunately, malignancies are rare in patients with dyspepsia.11,20,22 The symptoms of gastric cancer are similar to those of other causes of epigastric pain. However, the presence of “alarm symptoms,” such as dysphagia, unexplained weight loss (greater than 3 kg [6 lb, 8 oz]), history of gastrointestinal bleeding or clinical signs of anemia, may help to identify patients with more serious disease.22 Patients with gastric cancer also tend to be older and to have a shorter presenting history; they complain of continuous pain exacerbated by food and usually have associated anorexia.9
MEDICATION-INDUCED DYSPEPSIA
A complete medication history, including prescription and over-the-counter drugs, should always be obtained as part of the evaluation of patients with dyspepsia. Agents that have been associated with dyspepsia are listed in Table 4. Because dosage reduction or discontinuation of the offending agent may relieve a patient's symptoms, questions directed at identifying medication-induced dyspepsia may avoid costly diagnostic studies.
TABLE 4 Agents Commonly Associated with Dyspepsia
| Acarbose (Precose) |
| Alcohol |
| Alendronate (Fosamax) |
| Cisapride (Propulsid) |
| Codeine |
| Iron |
| Metformin (Glucophage) |
| Nonsteroidal anti-inflammatory drugs |
| Oral antibiotics (e.g., erythromycin) |
| Orlistat (Xenical) |
| Potassium |
| Corticosteroids (e.g., prednisone) |
| Theophylline |
The use of herbal products, home remedies and other products (e.g., vitamins, minerals and shark cartilage) sold in health food stores should be specifically addressed. Dietary supplements can be harmful, but patients may not consider their use important enough to mention.23 Herbs are currently considered dietary supplements, but they are not regulated by the U.S. Food and Drug Administration. Thus, purity and quality are difficult to ensure, and a number of products contain contaminants. Although documentation is poor, these products have been reported to cause a number of side effects, including dyspepsia (Table 5).23 Harmful drug-herb interactions are also possible.
TABLE 5 Herbs Noted to Have Side Effects that May Be Confused with Dyspepsia
| Herb | Side effects |
|---|---|
| Garlic | Stomach burning, nausea |
| Gingko | Mild gastrointestinal disturbances |
| Saw palmetto | Upset stomach |
| Feverfew | Gastrointestinal disturbances |
| Chaste tree berry | Gastrointestinal disturbances |
| White willow | Possibly adverse reactions similar to those of salicylates |
Information from Pharmacist's letter continuing education booklet: therapeutic use of herbs #422-000-98-079-Hot. Stockton, Calif.: Therapeutic Research Center, 1988.
NSAID-Induced Ulcers. New data regarding treatment options for NSAID-induced ulcers are discussed in detail elsewhere.24–27 In general, a proton pump inhibitor or a histamine H2- receptor blocker is used to treat an NSAID-induced ulcer; a proton pump inhibitor is the agent of choice when a patient is unable to discontinue use of the NSAID.27 No firm conclusions have been reached on the role of H. pylori infection in patients with NSAID-induced peptic ulcers.28 However, experts agree that H. pylori should be eradicated in patients taking NSAIDs who have an ulcer, as the cause of the ulcer is difficult to determine.27
OTHER DISORDERS
Patients with ischemic heart disease may relate their symptoms to the stomach rather than the heart. Therefore, cardiac etiologies need to be ruled out. Unfortunately, gastrointestinal and cardiac pain may be clinically indistinguishable, posing a difficult diagnostic and therapeutic challenge.
Some historical features may help to distinguish between cardiac and gastrointestinal causes of dyspepsia. Burning pain suggests a gastrointestinal etiology, whereas pressure radiating to the left arm suggests a cardiac origin. Pain lasting for hours tends to be gastrointestinal in origin. Positional pain is also more likely to have a gastrointestinal cause. For example, pain that occurs when a patient is lying down is more typical of GERD than of cardiac disease.
Metabolic disorders are a rare cause of dyspepsia. Other disorders to consider include malabsorption syndrome, collagen vascular disorders, Zollinger-Ellison syndrome and Crohn's disease.
Physical Examination
With the exception of epigastric tenderness, the physical examination is usually normal in patients with uncomplicated dyspepsia. In addition to evaluating the epigastric pain, it is important to assess the patient's hemodynamic status because hypotension or tachycardia may indicate significant blood loss from gastrointestinal bleeding. The stool should also be tested for occult blood.
An association between dental erosions and GERD has been found,29 but its incidence remains unclear. Thus, an oral examination may suggest the presence of GERD in a patient with extensive loss of enamel and exposed dentin.
Jaundice or a positive Murphy's sign suggests gall bladder disease. Signs of hypothyroidism or hyperthyroidism should also be considered in the evaluation of dyspepsia.
Weight loss, a positive fecal occult blood test, a palpable mass, signal nodes (Virchow's nodes) and acanthosis nigricans are signs of possible malignancy. Patients with dyspepsia and any of these signs should undergo endoscopy as soon as possible. Clinical signs of anemia, such as brittle nails, cheilosis and pallor of the palpebral mucosa or nail beds, may also suggest malignancy.
Laboratory Evaluation
The initial evaluation of dyspepsia should include a complete blood count to rule out anemia. If the history and physical examination suggest the presence of gallstones or another hepatobiliary condition, liver function tests and sonographic evaluation should be ordered. Likewise, if pancreatitis is suspected, serum lipase and amylase levels should be obtained. Patients with nausea, vomiting and epigastric fullness may also have generalized electrolyte imbalances. Therefore, electrolyte measurements should be considered.
Historically, upper gastrointestinal radiographs were obtained in patients with dyspepsia. Today, radiographs are considered inferior to upper endoscopic examination for confirming or excluding ulcers, reflux disease and malignancies.4,7 Although endoscopy with biopsy is considered the gold standard for diagnosing H. pylori infection,30,31 the procedure is not always practical and may not be cost-effective.30
H. pylori can also be detected in the serum with antibody titers, in the breath with the urea breath test (UBT) and in the stool with a polymerase chain reaction (PCR) test or an antigen enzyme immunoassay (EIA). With the UBT, if H. pylori is present, the urease produced by the organism breaks down ingested carbon 14–labeled urea into ammonia and labeled carbon dioxide, which can be detected in the patient's breath. The UBT is more sensitive and specific than serologic testing, but it also tends to be more expensive.32 Because serology is considered to have acceptable sensitivity and specificity for H. pylori infection, its cost and availability make it more practical than the UBT.31
A positive serology test only indicates previous exposure to H. pylori, not active infection. Thus, the test is not useful for confirming eradication of the organism. The UBT is the best test for this purpose, because once H. pylori is eradicated, urease is no longer produced.
Noninvasive detection of H. pylori in the feces is of particular importance in young patients. The reported sensitivities of PCR and EIA for H. pylori are 93.7 percent and 88.9 percent, respectively; the respective specificities are 100 percent and 94.6 percent.33
Management
After a thorough clinical evaluation and detailed history, conditions such as GERD, irritable bowel syndrome, biliary pain and medication-induced dyspepsia can most likely be confirmed or excluded.6,34 The remaining patients probably have ulcer-like, dysmotility-like or functional (nonulcer) dyspepsia.6 On investigation, most patients are found to have functional or nonulcer dyspepsia.6 Before any investigation is performed, the physician must decide whether the patient is at high risk for serious disease and should undergo immediate endoscopy or whether the patient can safely receive drug therapy.
In 1996, a consensus statement from the American College of Gastroenterology suggested that three options are available for the management of new-onset dyspepsia not caused by NSAIDs: (1) endoscopy in all patients, (2) a trial of empiric antisecretory drug therapy and (3) noninvasive serologic testing for H. pylori infection followed by antibacterial treatment if the test is positive.4 Other options that have been examined include empiric eradication of H. pylori infection and testing for H. pylori infection with endoscopy reserved for use in patients who have a positive test. Unfortunately, the ranking of management options is controversial, and no definitive recommendations can be made.
A number of decision analyses have been conducted to determine the most reasonable management approach.2,35–37 Factors to consider in selecting a strategy include cost, patient and physician attitudes about having an uncertain diagnosis, ethics, patient satisfaction and prevalence of disease. A model for the evaluation of patients who present with dyspepsia is provided in Figure 1. Strategic options for the initial management of patients with new-onset dyspepsia are compared in Table 6.7
FIGURE 1. Dyspepsia
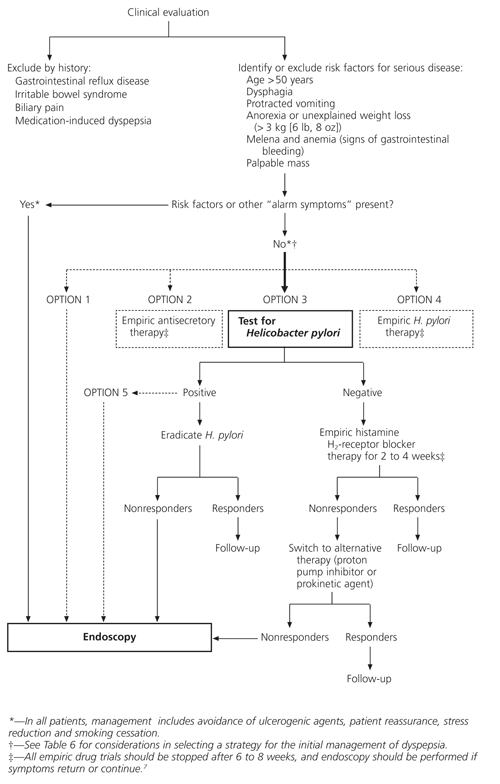
Proposed model for the evaluation and management of dyspepsia in the primary care setting.
TABLE 6 Considerations in Selecting a Strategy for the Initial Management of Dyspepsia
| Strategy | Advantages | Disadvantages |
|---|---|---|
| Option 1: endoscopy | Gold standard test to exclude gastroduodenal ulcers, reflux esophagitis and upper gastrointestinal cancers Beneficial because up to 40 percent of patients have an organic cause of dyspepsia Provides adequate patient reassurance Test of choice for targeting therapy | Expensive Invasive Not cost-effective or practical in young patients without alarm symptoms Rarely, endoscopic complications |
| Option 2: empiric treatment with acid suppression | Least expensive strategy Rapid relief of symptoms High response rate May reduce the number of endoscopies | Cost advantage is lost with symptom recurrence or lack of response. High rate of symptom recurrence May promote inappropriate long-term medication use May delay diagnostic testing May mask the symptoms of malignant ulcers Likely to provide the least patient reassurance Rarely, serious side effects (i.e., gynecomastia or hematologic disorders) |
| Option 3: test for Helicobacter pylori and treat if test is positive | Based on literature review, seems to be an acceptable approach and the least expensive strategy in H. pylori–sensitive patients Recommended by the American Gastroenterological Association May reduce the number of endoscopies | May increase levels of antibiotic resistance Relies on accurate H. pylori testing May result in overtreatment because of false-positive results or undertreatment because of false-negative results Benefits in patients with functional dyspepsia are likely to be small or nonexistent. Cancer and ulcer disease may be missed. Patient inconvenience because of complicated drug regimens May result in serious side effects (i.e., pseudomembranous colitis) Long-term outcome of treating all infected patients is inadequately documented |
| Option 4: empiric eradication of H. pylori | Avoids cost of H. pylori testing and endoscopy (actual cost savings may be modest if patient eventually requires endoscopy) May reduce the number of endoscopies | Most evidence does not favor this approach. |
| May increase levels of antibiotic resistance | ||
| Benefits in patients with functional dyspepsia are likely to be small or nonexistent. | ||
| Cancer and ulcer disease may be missed. | ||
| Patient inconvenience because of complicated drug regimens | ||
| May result in serious side effects (i.e., pseudomembranous colitis) | ||
| Long-term outcome of empirically treating all patients is inadequately documented. | ||
| Option 5: test for H. pylori and perform endoscopy if test is positive | Endoscopy will detect gastroduodenal ulcers, reflux esophagitis and upper gastrointestinal cancers. Minimizes antibiotic resistance | Not cost-effective compared with testing for H. pylori followed by treatment if the test is positive |
| May overuse endoscopies because of false-positive tests | ||
| Invasive |
Information from Talley NJ, Silverstein MD, Agreus L, Nyren O, Sonnenberg A, Holtmann G. AGA technical review: evaluation of dyspepsia. Gastroenterology 1998;114:582–95.
OPTION 1: ENDOSCOPY
Most physicians agree that definitive diagnostic evaluation with endoscopy is indicated in older patients at higher risk for malignancy and in younger patients with alarm symptoms. The guidelines outlined in the Maastricht European Consensus Report recommend endoscopy for patients older than 45 years of age, whereas the American Digestive Health Foundation recommends endoscopy for dyspeptic patients older than 50 years.38
Although clinical judgment is always best, a list of conditions to consider has been developed to serve as a guide in screening patients who may have risk factors for serious disease (Figure 1). If a patient will not accept a probable diagnosis and has concerns about malignancy, early investigation with endoscopy may be appropriate.20
OPTION 2: EMPIRIC ANTISECRETORY DRUG TRIAL
Although empiric drug trials are falling out of favor, acid suppression still remains an option in patients with dyspepsia.4 This approach is usually relatively inexpensive and provides relief of symptoms in many patients. However, the cost advantage can be lost if a patient eventually requires diagnostic evaluation.
When empiric therapy is used, a step-wise approach is suggested, with a medication being tried for two to four weeks. Therapy begins with an H2-receptor blocker; if necessary, a proton pump inhibitor is tried next. Antacids provide little help,8 but some experts suggest that prokinetic agents should be considered as alternatives to antisecretory drugs in an empiric drug trial.7 Uninvestigated new-onset dyspepsia is likely to be a nonulcer condition, although the possibility of ulcers and other disorders still exists.
Regardless of response, all drug trials should be stopped after six to eight weeks. If symptoms persist or recur, endoscopy should be performed.7 If patients have little to no response to drug therapy after seven to 10 days, endoscopy should be considered.7
Empiric drug therapy has also been recommended for patients with persistent symptoms but normal endoscopic findings. If drug therapy is not successful in these previously investigated patients, other approaches of limited value (e.g., antidepressant drug therapy, behavioral therapy or psychotherapy) may be pursued,34 and the diagnosis should be reevaluated.
OPTION 3: HELICOBACTER PYLORI TESTING AND TREATMENT
No consensus exists on how, in whom and when to test for the presence of H. pylori infection.5,6 The treatment of dyspepsia associated with H. pylori in the absence of ulcers is also controversial.5,6 Some investigations have shown that antibiotics are not useful for relieving symptoms in patients with nonulcer dyspepsia; however, these findings are questionable because of serious methodologic weaknesses in the studies.39 On the other hand, a recent analysis2 and a prospective study40 suggest that treating nonulcer dyspepsia with an H. pylori regimen is reasonable and cost-effective.
Investigators in one study suggested that the role of H. pylori infection in nonulcer dyspepsia is uncertain for two reasons.2 First, treatment has not consistently alleviated symptoms. Second, epidemiologic evidence of an association between H. pylori gastritis and nonulcer dyspepsia is equivocal. These investigators concluded that initial anti– H. pylori therapy is the most cost-effective management strategy in H. pylori–seropositive patients with dyspepsia.2
Other investigators have disagreed, stating that, like endoscopy, anti– H. pylori treatment has cost and feasibility issues.41 Most importantly, several investigators have stressed the need to consider potential adverse outcomes associated with the widespread use of antimicrobials, including problems with altering the normal flora and increasing antimicrobial resistance.41
Two recent studies reached opposite conclusions regarding the efficacy of eradicating H. pylori infection in patients with nonulcer dyspepsia.40,42 Thus, more investigation is needed before an evidence-based conclusion can be drawn.
Based on a review of the literature and available decision analyses, the American Gastroenterological Association suggested that the most reasonable strategy for the management of patients who present with dyspepsia is noninvasive testing for H. pylori infection followed by eradication of the organism if the test is positive.7 A cost-utility study in a primary care setting reached the same conclusions.37 Supporting data included the comparative cost-effectiveness of this approach and its lower potential for antibiotic resistance.
OPTION 4: EMPIRIC HELICOBACTER PYLORI ERADICATION
One cost-utility study found that empiric H. pylori eradication was similarly cost-effective to initial H. pylori testing followed by eradication when the test is positive.37 However, most evidence does not favor this strategy because it is more likely to lead to antibiotic resistance, as well as the unnecessary use of antibiotics.7
OPTION 5: NONINVASIVE HELICOBACTER PYLORI TESTING AND ENDOSCOPY
Noninvasive testing for H. pylori followed by endoscopy is another option. However, this strategy is unlikely to be as cost-effective as testing for and treating H. pylori infection.7
NONPHARMACOLOGIC MANAGEMENT
All patients with dyspepsia should be advised to stop smoking and, if their medical condition permits, to discontinue ulcerogenic medications. They should also avoid foods and other factors that precipitate their symptoms.
Because dyspepsia may be aggravated by stress, anxiety or depression, it may be useful to explore these issues. Reassurance is a key step in managing dyspepsia, but advice regarding stress-reducing activities such as exercise and relaxation is also important.
Final Comment
Questions about the evaluation and management of dyspepsia remain unanswered. Unfortunately, little consensus data are available to guide physicians in the diagnosis and management of patients presenting with dyspepsia in the primary care setting. The situation is complicated by the need to have a cost-effective, yet rational approach to dyspepsia.
Dyspepsia has a large number of possible etiologies. Most commonly, it is caused by gastric ulcers or GERD, although malignancies and other serious conditions also need to be considered. In many patients, a definitive investigation reveals no specific etiology. Because symptoms alone are not useful in distinguishing between causes, all aspects of the patient's evaluation, including the medical history, physical examination and laboratory review, are essential in the diagnosis.
Primary care physicians must determine when to treat empirically and when to arrange endoscopy for patients. Patients at high risk for malignancy should have early endoscopy. In young patients without signs or symptoms of a serious underlying disorder, the most evidence-based initial management strategy appears to be H. pylori testing followed by eradication of the organism when the test is positive.8,40 If symptoms resolve, no further treatment is necessary.
A gastric acid suppressant or prokinetic agent can be used in patients with nonulcer dyspepsia who do not have H. pylori infection and in patients with H. pylori infection who do not respond to anti– H. pylori agents (probably a large number of such patients, if not the majority43). If symptoms still do not improve, endoscopy and more specialized testing are indicated.8
If, after endoscopy and all other specialized testing, the diagnosis is functional or nonulcer dyspepsia and the symptoms do not respond to all previous treatments, dietary, environmental and emotional triggers should be evaluated and addressed.43 Additional treatments can include antidepressant drug therapy, stress management, relaxation therapy, hypnotherapy or psychotherapy.44
Future breakthroughs in dyspepsia management are likely to come from the evaluation of visceral sensitivity and brain-gut interactions.43

