
Am Fam Physician. 2000;61(3):789-791
A 41-year-old woman presented complaining of the progressive development of lesions on her lower extremities (see accompanying photos). She had also noted swelling of her right wrist and ankle with associated mild pain. The lesions were located primarily over the shins and medial aspects of both lower extremities, and consisted of erythematous macules, some of which had confluent borders. The lesions were palpable, did not blanch on pressure, and had no overlying warmth or tenderness. Mild swelling of the right ankle was present, although the patient maintained full range of motion. The remainder of the physical examination was unremarkable.
The patient had been recently diagnosed with hypertension for which she had been taking an angiotensin-converting enzyme inhibitor (ramipril) for two weeks. The patient had no other chronic medical illnesses. She had a history of intravenous drug use during adolescence.
On laboratory evaluation, she was noted to have proteinuria (1.2 g per day), with a creatinine clearance of 56 mL per minute (0.93 mL per second). Serum aminotransferase levels were mildly elevated: alanine aminotransferase was 123 U per L; aspartate aminotransferase was 139 U per L. The patient tested positive for hepatitis C virus (HCV) infection, most likely contracted during her years of intravenous drug use.
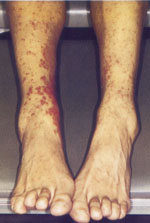
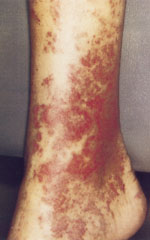
Question
Discussion
The answer is C: mixed cryoglobulinemia. Her rash is a leukocytoclastic vasculitis caused by cutaneous deposition of cryoimmunoglobulins. Several studies1,2 have established a strong link between HCV infection and mixed cryoglobulinemia, a multisystem disorder that is characterized by deposition of circulating immune complexes in small and medium-sized blood vessels resulting in arthralgias, Raynaud's syndrome and purpura. Kidney, nerve and brain involvement is possible.
It is important to obtain a thorough medication history in any patient who presents with a rash, because drug-induced etiologies are among the most common causes of leukocytoclastic vasculitis. Ramipril has been associated with a rash in a small percentage of patients. It often may not be possible to distinguish between a drug-induced vasculitis and a cryoglobulinemic rash by physical examination alone. However, the coincident clinical findings of positive serum HCV antibody, HCV RNA and serum cryoglobulins make the latter much more likely. In this patient, the rash improved on treatment of HCV infection, despite continued treatment with ramipril.
Cellulitis was ruled out by the absence of warmth or tenderness on examination of the leg, as well as absence of systemic manifestations such as a fever or elevated white blood cell count.
Lichen planus, a skin rash that occurs in less than 1 percent of the general population, persists for a long time. It presents as flat-topped, violaceous, pruritic papules in a generalized distribution. There is a high incidence of mucosal involvement, and it can involve the hair and nails. Antibodies to HCV are present in 10 to 38 percent of patients with lichen planus.
Porphyria cutanea tarda presents with photosensitivity, skin fragility, bruising, and vesicles and bullae that can become hemorrhagic. The so-called sporadic variety is the most common type, although rare familial forms exist. There is a high prevalence (62 to 91 percent) of HCV antibody positivity in patients with the sporadic form of porphyria cutanea tarda.3 Antiviral therapy with alpha-interferon for the underlying HCV infection can be effective in treating the associated mixed cryoglobulinemia.4 Patients who have no detectable HCV RNA at the end of a course of treatment have significantly improved purpura and serum cryoglobulin levels; however, a rebound phenomenon of clinical and serologic variables has been noted after discontinuation of this therapy.4
Although cryoglobulins are found in 19 to 54 percent of patients with HCV infection, symptoms occur in only 25 percent of these.5 Duration of HCV infection and severity of histologic hepatic inflammation do not appear to be related.5 In addition to cryoglobulinemia, other important extrahepatic manifestations of HCV infection include membranoproliferative glomerulonephritis, thyroiditis, porphyria cutanea tarda and lichen planus.6
Several types of cryoglobulinemias are recognized. Type I (monoclonal immunoglobulin) is associated primarily with malignant processes of the immune system. Type II (at least one monoclonal immunoglobulin, usually IgM mixed with polyclonal immunoglobulins) and type III (polyclonal only) are also known as mixed cryoglobulinemias. HCV has become one of the most common causes of mixed cryoglobulinemia, although mixed cryoglobulins are also observed with other chronic infections (e.g., hepatitis B, endocarditis) as well as autoimmune and malignant disorders.7
The clinical presentation of mixed cryoglobulinemia is quite variable. Cutaneous leukocytoclastic vasculitis is the most clinically evident manifestation. It usually presents with palpable purpura and petechiae that involve the lower extremities.8 Skin lesions are not always obvious and are sometimes not present. Arthralgias and arthritis may be prominent. The joint involvement is usually a symmetric, nonmigratory polyarthritis involving ankles, wrists, elbows, hands and toes. The most serious manifestation is renal damage due to deposition of the circulating cryoimmunoglobulins. This can present as nephrotic syndrome, glomerulonephritis or acute renal failure. Renal biopsy usually reveals IgM and IgG deposition within subendothelial immune deposits. Treatment of the underlying chronic infection can ameliorate cryoglobulinemia. Corticosteroids and cytotoxic agents are sometimes used in severe cases.