
A more recent article on geriatric assessment is available.
This is a corrected version of the article that appeared in print.
Am Fam Physician. 2000;61(4):1089-1104
The number of persons 65 years of age and older continues to increase dramatically in the United States. Comprehensive health maintenance screening of this population is becoming an important task for primary care physicians. As outlined by the U.S. Preventive Services Task Force, assessment categories unique to elderly patients include sensory perception and injury prevention. Geriatric patients are at higher risk of falling for a number of reasons, including postural hypotension, balance or gait impairment, polypharmacy (more than three prescription medications) and use of sedative-hypnotic medications. Interventional areas that are common to other age groups but have special implications for older patients include immunizations, diet and exercise, and sexuality. Cognitive ability and mental health issues should also be evaluated within the context of the individual patient's social situation—not by screening all patients but by being alert to the occurrence of any change in mental function. Using an organized approach to the varied aspects of geriatric health, primary care physicians can improve the care that they provide for their older patients.
Current predictions suggest that the number of persons 65 years of age and older will more than double in the United States during the next 30 years. As a result, the number of elderly Americans could increase from 34 million in 1998 to approximately 69 million in 2030. This increase, combined with the disproportionate rate at which elderly patients use medical resources, will require that primary care physicians become increasingly knowledgeable about the needs of geriatric patients and increasingly efficient in the evaluation and management of concerns unique to these patients.
The value of performing a comprehensive geriatric assessment appears to be equivocal. Simple screening instruments can be helpful in identifying patients at risk for common health problems and in improving the clinical assessment of a disease course.1 However, these screening tools may not be effective in reducing health care utilization or costs.2
The comprehensive geriatric assessment is often described in the literature as a multidisciplinary, time-intensive evaluation of a patient previously identified as being at significant risk for imminent morbidity or mortality.2,3 An evaluation of this type is impractical in most primary care settings and is seldom used by practicing physicians.4 Yet the ongoing, long-term management component of primary care is a key ingredient in the success of outpatient geriatric evaluation.5
Effective primary care management of geriatric health issues, with its goal of caring for healthy and functional elderly patients, may perhaps be better described as comprehensive health screening. Using simple and easily administered assessment tools, physicians can improve the identification of specific problems that are common in the elderly and also shift their focus from disease-specific intervention to preventive care and proactive medical management.5
In 1996, the U.S. Preventive Services Task Force (USPSTF) published the second edition of its Guide to Clinical Prevention Services.6 In this publication, the USPSTF updated earlier recommendations on preventive services for patients at various stages of life. The recommendations for patients 65 years of age and older include a number of items common to other age groups. The unique assessment categories for older patients are sensory perception (hearing and vision screening) and accident prevention. Assessment areas common to other age groups but with special implications for the elderly include diet and exercise, immunizations and sexuality. Although the USPSTF found little evidence in 1996 to support the value of screening for dementia, recent pharmaceutical advances have resulted in beneficial treatment options that were not available just a few years ago.7
Using the USPSTF recommendations as a guide, this article reviews available standardized assessment tools and techniques that can be used in outpatient settings. The goals are to encourage a systematic assessment of various areas of potential geriatric risk and to develop a database appropriate to the unique concerns of elderly patients. All of the information does not need to be gathered in one office visit. Multiple visits can be used to perform the entire assessment.
Injury Prevention
The USPSTF recommends that primary care physicians ask patients in most age groups about the routine use of safety belts and bike helmets, the availability of smoke detectors, the maintenance of hot water heater temperature at or below 48.8°C (120°F) and the danger of smoking near bedding or upholstery.6 Fall prevention, however, is an assessment category unique to patients 65 years of age and older.
The annual incidence of falls in patients over 65 years of age who live independently is approximately 25 percent but rises to 50 percent in patients over 80 years of age.8 Falls are responsible for a significant number of accidental deaths and traumatic injuries among the elderly. One third of patients with confirmed falls may not recall falling.9
RISK FACTORS
Intrinsic factors that contribute to falls include age-related changes in postural control, gait and visual ability, and the presence of acute and chronic diseases that affect sensory input, the central nervous system and musculoskeletal strength and coordination. Certain medications can also increase the risk of falling (Table 1).10
Osteoporosis is one notable intrinsic factor that leads to falls. In patients with this condition, a pathologic fracture may precede a fall. In the absence of universally accepted criteria for the assessment of bone mineral density, screening should be directed at a risk assessment for osteoporosis (Table 2).
| Increasing age |
| Female gender |
| Early menopause |
| Low body weight |
| Small stature |
| White or Asian race |
| Family history |
| Drug use (e.g., steroids, heparin) |
| Low calcium intake |
| Excessive alcohol intake |
| Smoking |
| Physical inactivity |
| Conditions that impair calcium absorption |
| High caffeine intake |
Extrinsic factors that contribute to falls include poor lighting, obtrusive furniture, slippery floors, loose floor coverings and bathrooms without handrails or grab bars.
MOBILITY AND DEXTERITY
A comprehensive risk assessment for falls incorporates a review of all potential intrinsic and extrinsic factors, as well as a focused physical examination (Table 3).11 The physical examination can be a simple evaluation of one-leg balance (i.e., the ability to stand unassisted on one leg for five seconds)12 or a more structured evaluation such as the “Get Up and Go” test.13 In the “Get Up and Go” test, the patient is observed as he or she rises from a sitting position, walks 10 ft, turns and returns to the chair to sit. The effectiveness of the test for predicting falls can be enhanced by timing the process, with more than 16 seconds suggesting an increased risk of falling.14 Any observed or reported changes in gait, strength or balance may require further evaluation with a more detailed assessment.
Sensory Perception
Changes in vision and hearing occur as patients age. Because these changes can have a great impact on well-being, the USPSTF recommends regular vision and hearing screening for patients 65 years of age and older.6
VISION
One study found that 72 percent of community-based patients more than 64 years of age had impaired vision as tested with a Snellen eye chart.15 Other studies have detected lower percentages of geriatric patients with vision problems, but the prevalence of visual impairment is still quite high. The most common causes of visual impairment in the elderly include presbyopia, cataracts, glaucoma, diabetic retinopathy and age-related macular degeneration. Changes in vision can cause a significant number of problems for elderly patients, including an increased risk for falls.16
The Snellen eye chart is an appropriate tool for visual acuity screening in the elderly. Referral to an ophthalmologist should be considered when visual acuity is worse than 20/40 (with normal corrective lenses, if applicable) and visual impairment is interfering with daily activities.
The USPSTF found insufficient evidence to recommend for or against screening with ophthalmoscopy performed by primary care physicians in asymptomatic elderly patients. However, patients at high risk for glaucoma (i.e., black patients over 40 years of age, white patients over 65 years of age and patients with diabetes mellitus, myopia, ocular hypertension or a family history of glaucoma) should be referred to an eye care specialist for tonometry, funduscopy and visual field examination. The optimal frequency for glaucoma screening in these patients is uncertain.6
HEARING
The prevalence of hearing loss in the geriatric population ranges from 14 to 46 percent,17,18 but only 20 percent of primary care physicians routinely screen elderly patients for hearing loss.18 As a result of psychologic, financial and mechanical impediments, only 32 percent of persons with moderate to marked hearing loss use a hearing aid.17
Presbycusis, a progressive high-frequency hearing loss, is the most common cause of hearing impairment in geriatric patients.19 This type of hearing loss decreases the ability to interpret speech, which can lead to a decreased ability to communicate20 and a subsequent increased risk for social isolation and depression.17 Hearing loss in the elderly can also adversely affect physical, emotional and cognitive well-being.21
Questionnaires such as the Hearing Handicap Inventory for the Elderly–Screening version (HHIE–S) have been shown to accurately identify persons with hearing impairment18 (Figure 1).22 The reference standard for establishing hearing impairment, however, remains pure tone audiometry, which can be performed in the physician's office. Combining the HHIE–S questionnaire with pure tone audiometry has been shown to improve screening effectiveness.20

Appropriate interventions include periodic screening to provide early detection of hearing impairment, cautious use or avoidance of ototoxic drugs, and support for the obtainment and continued use of hearing aids.17 Interventions to be considered, depending on the degree of hearing loss, are provided in Table 4.10
Nutrition
Malnutrition and undernutrition are common yet frequently overlooked problems in the geriatric population. Elderly patients with a compromised nutritional state require longer hospital stays and develop more complications.23
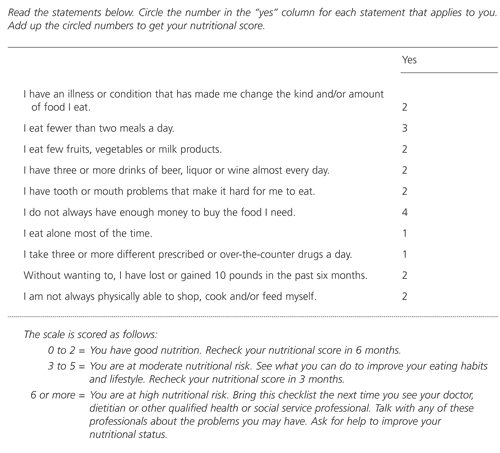
The USPSTF recommendation for encouraging regular tooth brushing, flossing and dental visits gains importance in the elderly.6
Immunizations
A 1990 report24 indicated that fewer than 30 percent of adults had received updated tetanus-diphtheria, influenza and pneumococcal immunizations. The poor compliance rate was determined to be secondary to patients' concerns about adverse reactions to immunizations and physicians' overlooking the need for such immunizations. In recent years, however, immunization rates in adults have improved. Data from the Centers for Disease Control and Prevention indicated that the 1997 rates for influenza and pneumococcal vaccinations were 65.5 percent and 45.5 percent, respectively.25
Primary care physicians must be diligent in assessing the immunization status of geriatric patients and providing the recommended vaccines. As suggested by the USPSTF,6 an annual influenza vaccination in the fall is recommended for all elderly patients. Patients over 65 years of age should also receive at least one pneumococcal vaccination in their lifetime, with high-risk patients receiving a second immunization in six years. The tetanus-diphtheria (Td) toxoid should be given every 10 years. The Td toxoid is given again after five (or more) years if the patient suffers a wound that would be classified as “dirty.”
Sexuality
Although the tempo and intensity of sexual activity may change over time, problems that relate to a person's ability to have and enjoy sexual relations should not be considered part of the normal aging process. Studies show that 74 percent of married men and 56 percent of married women over 60 years of age remain sexually active.26
Common problems affecting sexual functioning include arthritis, diabetes, fatigue, fear of precipitating a heart attack and side effects from alcohol, prescription drugs and over-the-counter medications.27 Older patients state that they would like their physician to initiate discussions about sexuality, ask open and direct questions, and treat them as normal sexual persons.28
Continence
Incontinence is estimated to occur in 11 to 34 percent of elderly men and 17 to 55 percent of elderly women.29 Although incontinence is common, is frequently reversible30 and has significant social and emotional consequences,31 relatively few patients volunteer that they are having problems or request treatment.32
The first step in screening for urinary incontinence is to ask the patient if he or she is experiencing any problems in this area. Two straightforward questions are “Do you ever lose urine when you don't want to?” and “Have you lost urine on at least six separate days?” Affirmative answers to both questions constitute a positive screen. In this situation, further evaluation is necessary. Evidence of stress incontinence is elicited by questions such as “Do you ever lose urine when you cough, exercise, lift, sneeze or laugh?”
The assessment for urinary incontinence should include an evaluation of cognitive function, fluid intake, mobility, medication side effects and previous urologic surgeries.30 The physical examination should focus on the lower genitourinary tract in women and the prostate gland in men. A rectal examination can determine the presence of fecal impaction, and a simple urinalysis can be used to screen for infection or glycosuria.
Mental Status
Changes in mental status can have a profound impact on elderly patients and their families. Two of the more common changes are cognitive decline and depression.
COGNITION
Dementia is chronic and progressive, and it is characterized by the gradual onset of impaired memory and deficits in two or more areas of cognition, such as anomia, agnosia or apraxia. For the diagnosis of dementia to be established, these deficits must be present with no alteration of consciousness and no underlying medical cause that would better explain the deficits.
Two of the more commonly used screening tools for dementia are the Mini-Mental State (Figure 3)33 and the Clock Test.34 An alternative to patient testing is a structured family report using the Informant Questionnaire on Cognitive Decline in the Elderly (IQCDE).35 Although less discriminating than the Mini-Mental State, the IQCDE is not affected by a patient's educational level or premorbid intelligence.36 Combining these tools can increase the sensitivity of the screening process and identify additional patients in the early stages of dementia.37

DEPRESSION
Depression significantly increases morbidity and mortality.38 As opposed to dementia, depression is usually characterized by a relatively rapid onset, intact but possibly retarded cognitive abilities and a generally time-limited duration.
The Geriatric Depression Scale, shown in Figure 4,39 is a good screening tool to use in older patients.40 It avoids issues related to physical symptoms and asks questions requiring only a “yes” or “no” answer. The one-question Yale Depression Screen (“Do you often feel sad or depressed?”) has also been found to be an effective screening tool41 and may be worth considering when clinical time is at a premium.

An assessment for suicide risk is important in geriatric patients who appear depressed. The best way to accomplish this task is to ask direct, yet nonthreatening questions. An effective interview progression might be to begin by asking patients if they are concerned that they are becoming a burden to their family and if they have ever felt that their family might be better off without them. This is followed by questions about active suicidal ideation.42
Social Issues
Because multiple aspects of the social situation can influence functional ability, efficient use of time can be made by asking patients and family members if any recent changes have occurred in living arrangements, finances or activities. Actual or potential care-givers can provide information about a patient's social network and support system, as well as the availability of care.6
Evaluating a caregiver's potential for feeling overwhelmed is important in determining the risk of “burning out.” Referral to agencies such as the Alzheimer's Association or a local senior center can provide functional and emotional support for patients and caregivers.6
Other issues that need to be addressed with patients and caregivers include advance directives, the living will and the durable power of attorney. Finally, the USPSTF recommends that all family members of geriatric patients receive training in cardiopulmonary resuscitation.6
Remaining as independent as possible for a long as possible is a primary concern for most elderly patients. The level of supportive assistance that is needed can quickly be determined by asking the patient and/or caregiver about the patient's ability to perform the Activities of Daily Living (ADLs) and Instrumental Activities of Daily Living (IADLs). An ADL evaluation form is provided in Figure 5,43 and an IADL evaluation form is presented in Figure 6.44 Having the patient complete a structured series of activities, such as the Performance Test of Activities of Daily Living (PADL), provides similar information without reporting bias.45
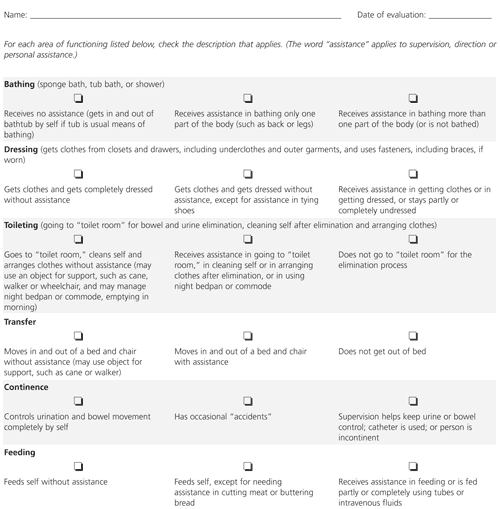

One recent study indicated that short-term memory and orientation are the domains most closely associated with ADL dependence. The study findings suggested that a shortened version of the Mini-Mental State that included only the recall of three words and the orientation to month, year and address could be a valid and time-efficient assessment tool.46
Final Comment
Geriatric patients present multiple challenges to primary care physicians. Using a standard assessment plan, which might include a chart-based checklist of counseling topics (Figure 7),6 as well as a brief screening list (Table 5),47 physicians can prevent or delay some of the major causes of morbidity and mortality in their older patients. The assessment can be performed over time and during multiple visits. By performing comprehensive health screening, physicians can provide appropriate interventions and improve quality of life for their geriatric patients.
