The Omnibus Budget Reconciliation Act (OBRA) of 1987 limited the use of psychotropic medications in residents of long-term care facilities. Updates of OBRA guidelines have liberalized some dosing restrictions, but documentation of necessity and periodic trials of medication withdrawal are still emphasized. Antidepressant drugs are typically underutilized in nursing homes. Tricyclic antidepressants have many side effects and thus are not preferred medications in elderly patients. Anxiety and insomnia are common problems in the institutionalized elderly. If behavioral measures are not successful, antidepressant medications with shorter half-lives may avoid drug accumulation, which can lead to excessive sedation, cognitive impairment and an increased risk for falls. In the elderly, antipsychotic medications can cause serious side effects, such as extrapyramidal symptoms and tardive dyskinesia. Newer antipsychotic drugs are less often associated with these side effects, but they should be used only for specific diagnoses and when behavioral and environmental measures are unsuccessful.
Improving the quality of care for nursing home residents has been a major concern for years. Recently, attention has focused on maximizing the appropriate use of psychotropic medications to manage agitation and other behavioral problems associated with dementia.
Mental disorders are present in a large percentage of the nursing home population. Antipsychotics, benzodiazepines and antidepressants are among the medications most commonly used to manage problem behaviors.1 Historically, antipsychotics and benzodiazepines have been used excessively (and without appropriate diagnosis or monitoring for side effects) in nursing home residents, often solely for the convenience of staff. Studies have found that most residents of long-term care facilities receive at least one psychotropic medication. Meanwhile, antidepressants have been underutilized because depression is often overlooked as a cause of behavioral disturbances in this population.2
The misuse of psychotropic drugs exposes patients to medication side effects and can lead to deterioration of medical and cognitive status. To combat this problem, the federal government passed nursing home reform legislation, the Omnibus Budget Reconciliation Act (OBRA) of 1987.3 This legislation is directed at protecting residents of long-term care facilities from medically unnecessary “physical or chemical restraints imposed for purposes of discipline or convenience.”3
The Health Care Financing Administration (HCFA), an agency responsible for regulating nursing homes participating in the Medicare and Medicaid programs, developed interpretive guidelines for fulfilling OBRA requirements.4 These guidelines were implemented nationally in 1990 and remain in force5 (Figure 1).4 Updated guidelines were implemented in July 1999.6
FIGURE 1. HCFA Guidelines
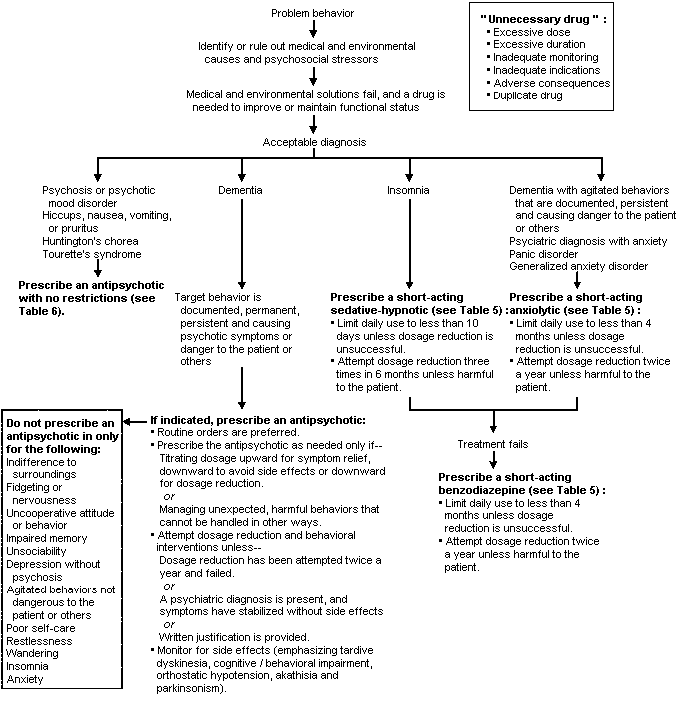
Summary of the Health Care Financing Administration (HCFA) guidelines.
Information from Health Care Financing Administration. Survey procedures and interpretive guidelines for skilled nursing facilities and intermediate care facilities. Baltimore: U.S. Dept. of Health and Human Services, 1990.
Summary of OBRA Interpretive Guidelines
All psychotropic drugs (antidepressants, anxiolytics, sedative-hypnotics and antipsychotics) are subject to the “unnecessary drug” regulation of OBRA. According to the HCFA guidelines,4 “residents must be free of unnecessary drugs,” which are defined as those that are duplicative, excessive in dose or duration, or used in the presence of adverse effects or without adequate monitoring or indication. The remaining regulations apply to anxiolytic, sedative-hypnotic and antipsychotic drugs only.
Medical, environmental and psychosocial causes of behavioral problems must be ruled out, and nonpharmacologic management must be attempted before psychotropic drugs are prescribed to nursing home residents. Because treatment with psychotropic medications is indicated only to maintain or improve functional status, diagnoses and specific target symptoms or behaviors must be documented, and the effectiveness of drug therapy must be monitored. Specific dosage limits must be observed, and periodic dosage reductions or drug discontinuations must be undertaken. Side effects (of antipsychotics, in particular) must be monitored. Barbiturates and certain other older tranquilizers may not be prescribed unless they were being used successfully before a patient was admitted to a long-term care facility (Table 1).4 Phenobarbital can be used solely to control seizures.
TABLE 1. Drugs Not to Be Used in Nursing Homes*
| Barbiturates |
| Amobarbital (Amytal) |
| Amobarbital-secobarbital (Tuinal) |
| Aspirin-butalbital-caffeine (Fiorinal) |
| Butabarbital (Butisol) |
| Pentobarbital (Nembutal) |
| Secobarbital (Seconal) |
| Other tranquilizers |
| Ethclorvynol (Placidyl) |
| Glutethimide (Doriden) |
| Meprobamate (Miltown) |
*—In accordance with regulations relating to the Omnibus Budget Reconciliation Act of 1987, drugs listed in this table are not to be used unless started before admission to a nursing home, given as a single dose for a medical or dental procedure or used for the treatment of seizures (phenobarbital).
Information from Health Care Financing Administration. Survey procedures and interpretive guidelines for skilled nursing facilities and intermediate care facilities. Baltimore: U.S. Dept. of Health and Human Services, 1990.
OBRA restricts the use of antipsychotic drugs only in patients with dementia. None of the OBRA dosage restrictions or monitoring requirements apply in patients with psychotic disorders (e.g., schizophrenia).
Each nursing home is surveyed annually. Because facilities that do not meet HCFA's legislated requirements may be denied Medicare reimbursement,7 physicians who prescribe medications for nursing home residents must document the medical necessity of noncompliance with regulations (e.g., drug prescriptions in excess of OBRA-mandated dosages). As a resource for physicians and facilities, a local consultant pharmacist reviews all charts monthly and assists with compliance.
According to the OBRA strategy, the long-term care facility, rather than the prescribing physician, is accountable for monitoring drug use.8 Some consider that this approach better reflects the realities of nursing home practice, in that the prescribing physician only visits the facility occasionally.8 Regardless of where final responsibility lies, physicians need to be aware of the HCFA interpretive guidelines for the fulfillment of OBRA requirements.
The updated HCFA regulations change some antipsychotic dosing restrictions.6 Medications considered potentially hazardous to the elderly are listed in Tables 2 and 3.9
TABLE 2. Drugs with a High Potential for Severe Outcomes in the Elderly
| Drugs | Comments |
|---|---|
| Psychotropics | |
| Amitriptyline (Elavil) | Strongly anticholinergic and sedating |
| Barbiturates | More side effects than most sedative-hypnotic drugs; should not be used except to control seizures (phenobarbital) |
| Long-acting benzodiazepines | Long half-life and, hence, prolonged sedation; associated with an increased incidence of falls and fractures |
| Doxepin (Sinequan) | Strongly anticholinergic and sedating |
| Meprobamate (Miltown) | Highly addictive and sedating |
| Analgesics | |
| Meperidine (Demerol) | Not effective when administered orally; metabolite has anticholinergic profile |
| Pentazocine (Talwin) | Confusion and hallucinations more common than with other narcotics |
| Miscellaneous | |
| Antispasmodic agents (gastrointestinal) | Highly anticholinergic with associated toxic effects |
| Chlorpropamide (Diabinase) | Serious hypoglycemia possible because of the drug's prolonged half-life |
| Digoxin (Lanoxin) | Decreased renal clearance; doses should rarely exceed 0.125 mg except when treating arrhythmias |
| Methyldopa (Aldomet) | Causes bradycardia and exacerbates depression |
| Ticlopidine (Ticlid) | More toxic than aspirin |
Information from Beers M. Explicit criteria for determining potentially inappropriate medication use by the elderly. An update. Arch Intern Med 1997;157:1531–6.
TABLE 3. Drugs with a High Potential for Less Severe Outcomes in the Elderly
| Drugs | Comments |
|---|---|
| Analgesics | |
| Indomethacin (Indocin) | More central nervous system side effects than any other nonsteroidal anti-inflammatory drug |
| Propoxyphene (Darvon) | Few advantages over acetaminophen and has narcotic side effects |
| Antihypertensives | |
| Beta blockers | Can cause problems in patients with asthma or chronic obstructive pulmonary disease; may precipitate syncope because of negative inotropic and chronotropic effects |
| Reserpine* | Can cause depression, sedation and orthostatic hypotension |
| Miscellaneous | |
| Antihistamines† | Highly anticholinergic |
| Cyclandelate (Cyclospasmol) | Generally ineffective for dementia or any other condition |
| Dipyridamole (Persantine) | Frequently causes orthostatic hypotension; of benefit only in patients with artificial heart valves |
| Ergoloid mesylates (Hydergine) | Generally ineffective for dementia or any other condition |
| Muscle relaxants | Increased cholinergic activity, sedation and weakness |
| Trimethobenzamide (Tigan) | Least effective antiemetic and can cause extrapyramidal symptoms |
*—Reserpine is available alone (in generic form) and is also found in combination drugs such as reserpine-trichlormethiazide (Metatensin).
†—Over-the-counter and prescription first-generation antihistamines.
Information from Beers M. Explicit criteria for determining potentially inappropriate medication use by the elderly. An update. Arch Intern Med 1997;157:1531–6.
Impact of OBRA on the Prescribing of Psychotropic Drugs
Several multiyear, multifacility reviews have examined the impact of OBRA regulations on the prescribing of psychotropic drugs in nursing homes.2,7,8,10,11 Researchers confirm an encouraging trend toward increased awareness of the indications for neuroleptic drugs and the side effects of these medications.2
Since OBRA was enacted, overall use of antipsychotic drugs in nursing home residents has declined by nearly one third,10 and prescriptions for antidepressants have increased8 (by almost 85 percent in one study10). Furthermore, selective serotonin reuptake inhibitors (SSRIs), nortriptyline (Pamelor) and trazodone (Desyrel) are being prescribed significantly more often, and amitriptyline (Elavil) and doxepin (Sinequan) are being used less often.8
The prescribing patterns for anxiolytic and sedative-hypnotic drugs are less consistent. One large study documented a 12 percent increase in prescriptions for anxiolytics but found decreases in the prescribing of particular agents, such as diazepam (Valium) and diphenhydramine (Benadryl).8 Two studies2,7 unequivocally cited the implementation of OBRA regulations, rather than other educational and consultative interventions, as being responsible for decreased use of neuroleptic drugs and lower dosages of these agents when they are used.
A recent review11 found that specific guidelines (on appropriate diagnosis, target symptom documentation and reasonable dosage level) were widely followed, with compliance rates ranging from 70 to 90 percent. Less specific guidelines (on attempts to use nonpharmacologic interventions and the monitoring of drug efficacy and safety) were less well followed, with compliance rates below 55 percent.
Recommendations for the Clinical Use of Psychotropic Drugs
Prescribed judiciously, psychotropic drugs can enhance the physical and psychologic well-being of the elderly. However, altered drug disposition makes this age group particularly sensitive to undesirable side effects, which can lead to a decline in medical and functional status or the use of additional prescriptions and an increased risk of drug interactions. Psychotropic medications, including side effects and recommendations on use in the elderly, are briefly reviewed in the following sections.
ANTIDEPRESSANT DRUGS
OBRA requirements for the prescribing of antidepressant drugs are limited. The legislation mandates only documentation of an appropriate diagnosis, use of a reasonable dosage (Table 4), clinically acceptable duration of use and monitoring for common adverse reactions.
TABLE 4. Antidepressant Drugs and Dosages Preferred for Use in the Elderly
| Drugs | Geriatric dosage (mg per day) | Side effects | ||||
|---|---|---|---|---|---|---|
| Starting dosage | Maintenance dosage | Sedation | Agitation | Anticholinergic effects | Orthostatic hypotension | |
| Tricyclic antidepressants | ||||||
| Desipramine (Norpramin) | 25 | 50 to 150 | Low | Low | Low | Low |
| Nortriptyline (Pamelor) | 10 to 25 | 40 to 75 | Moderate | — | Low | Low |
| Selective serotonin reuptake inhibitors | ||||||
| Citalopram (Celexa) | 20 | 20 to 40 | Low | Low | — | — |
| Fluvoxamine (Luvox) | 50 | 50 to 200 | Low | Low | — | — |
| Paroxetine (Paxil) | 10 | 20 to 30 | Low | Low | — | — |
| Sertraline (Zoloft) | 25 to 50 | 50 to 150 | Low | Low | — | — |
| Miscellaneous | ||||||
| Bupropion (Wellbutrin) | 100 | 100 to 400 | — | Moderate | — | Low |
| Nefazodone (Serzone) | 100 | 100 to 600 | Moderate | — | Low | Low |
| Trazodone (Desyrel) | 25 to 50 | 50 to 300 | High | — | Low | Moderate |
| Venlafaxine (Effexor) | 75 | 75 to 350 | Low | Low | Low | Low |
— = Very low or insignificant effects.
Nevertheless, choosing antidepressants with suitable side effect profiles is important in geriatric patients. The older tricyclic antidepressants, although highly effective, have side effects to which the elderly are especially sensitive. Of particular concern are excessive sedation, anticholinergic effects (dry mouth, constipation, urinary retention, blurred near vision, tachycardia and confusion), orthostatic hypotension and electrocardiographic changes. In elderly patients, it is better to use tricyclic antidepressants that cause less severe anticholinergic effects and orthostatic hypotension, such as nortriptyline and desipramine (Norpramin).
Subtle differences among SSRIs should also be considered. The half-lives reported for fluoxetine (Prozac) and its active metabolite are long (84 and 146 hours, respectively).12 Because of fluoxetine's long half-life and the persistence of side effects (sometimes for weeks after discontinuation), this drug is generally not recommended for use in elderly patients. Sertraline (Zoloft) and its metabolite have considerably shorter half-lives (25 and 66 hours, respectively). Paroxetine (Paxil), which has no active metabolite, also has a considerably shorter half-life (24 hours) than fluoxetine.12,13
Most SSRIs are associated with significant drug interactions. Fluoxetine, paroxetine and, to a lesser extent, sertraline inhibit the metabolism of warfarin (Coumadin), cisapride (Propulsid), benzodiazepines, quinidine, tricyclic antidepressants, theophylline and some statins.12 In patients at risk for these interactions, citalopram (Celexa), a new SSRI now available in the United States, may offer an advantage. Studies have shown that compared with other SSRIs, citalopram has less of an inhibitory effect on the cytochrome P450 system.14 Citalopram is as effective as fluoxetine and sertraline in the treatment of depression.14
Trazodone and nefazodone (Serzone) are also recommended for use in the elderly. Both of these drugs are fairly sedating (trazodone more so than nefazodone) and therefore are useful in elderly patients with depression and agitation or insomnia. Because trazodone is associated with significant orthostatic hypotension, nighttime dosing may be preferable. If trazodone causes excessive sedation or postural hypotension, nefazodone is an alternative. However, nefazodone inhibits the cytochrome P450 3A4 pathway, and it may exhibit dangerous interactions with cisapride.12
Venlafaxine (Effexor) and bupropion (Wellbutrin) are effective, well-tolerated antidepressants that lack significant anticholinergic side effects. Because bupropion is structurally related to stimulants, bedtime administration should be avoided. Bupropion in dosages above 400 mg per day is associated with seizures.12 In dosages exceeding 200 mg per day, venlafaxine causes increased blood pressure in 3 to 13 percent of patients.12 Therefore, higher dosages of these drugs are not recommended.
The tetracyclic drug mirtazapine (Remeron) is another newer antidepressant. This drug is a weak blocker of alpha-adrenergic and muscarinic receptors. Because of these actions, mirtazapine can cause orthostatic hypotension and anticholinergic effects; however, these side effects are less severe than those occurring with tricyclic antidepressants. Somnolence has been reported by more than 50 percent of patients treated with mirtazapine.15 Research on the use of this drug in geriatric patients has been limited.12,15
Most antidepressants have a long enough half-life in the elderly that they may be given as a single dose in the morning or evening, depending on the sedative or activating properties of the particular drug. Dosages need to be titrated carefully: the more gradual the titration, the lower the likelihood of side effects.
Typical antidepressant dosage ranges are one half of those used in younger patients. Occasionally, however, a full dosage is needed to yield a therapeutic effect.
ANXIOLYTIC AND SEDATIVE-HYPNOTIC DRUGS
Benzodiazepines are indicated for the short-term management of anxiety and insomnia, but nonpharmacologic measures should be tried first. Emphasizing good sleep habits is a first step and should include decreasing afternoon caffeine intake, exercising regularly before dinner, avoiding naps, establishing regular sleep hours, treating nighttime pain, addressing nocturia and maintaining a comfortable bedroom environment (temperature, noise level, lighting, etc.).
When benzodiazepine therapy becomes necessary for older patients, it is preferable to use short-acting agents. Elderly patients can better tolerate temazepam (Restoril) and lorazepam (Ativan), which have relatively short half-lives (three to 18 hours and 10 to 16 hours, respectively) and relatively short durations of action.16,17 Long-acting benzodiazepines, which have half-lives that may exceed 100 hours, carry higher risks for elderly patients. Indeed, the continuous administration of a long-acting benzodiazepine can lead to profound confusion, cognitive impairment and falls. For this reason, OBRA guidelines permit the use of long-acting benzodiazepines in residents of long-term care facilities only if a trial of short-acting benzodiazepines fails.
Side effects of all benzodiazepines include excessive sedation, psychomotor slowing, cognitive impairment, confusion, forgetfulness, morning “hangover” effect, ataxia and falls. Occasionally, dysphoria, irritability and agitation develop in elderly patients treated with these drugs.16
Zolpidem (Ambien) is a newer medication with some advantages as a short-term sleep aid for the elderly. Compared with benzodiazepines, zolpidem appears to carry less risk for the development of tolerance, withdrawal phenomenon or rapid-eye-movement rebound. Side effects of zolpidem include drowsiness, dizziness, headache and gastrointestinal upset.17
OBRA regulations permit the use of antihistamines such as diphenhydramine and hydroxyzine (Atarax, Vistaril) for the management of anxiety and insomnia in elderly patients. However, even in low dosages, these drugs are associated with impairment of daytime functioning.17 Furthermore, the anticholinergic effects of antihistamines (delirium, confusion, disorientation, etc.) may exacerbate problem behaviors.17
Sedating antidepressants in low dosages are often used to treat insomnia. Nortriptyline (in a dosage of 10 to 25 mg per day) and particularly trazodone (in a dosage of 25 to 150 mg per day), which exhibits no anticholinergic effects, are well suited for use in geriatric patients.17
OBRA-specified dosages of commonly used anxiolytic and sedative-hypnotic drugs are listed in Table 5.
TABLE 5. Anxiolytic and Sedative-Hypnotic Drugs Commonly Used in the Elderly
| Drugs | Geriatric dosage (mg per day)* | |||
|---|---|---|---|---|
| Anxiety | Insomnia | Onset of action | ||
| Short-acting agents | ||||
| Benzodiazepines | ||||
| Alprazolam (Xanax) | 0.75 | 0.25 | Intermediate | |
| Estazolam (Prosom) | 0.5 | 0.5 | Fast | |
| Lorazepam (Ativan) | 2 | 1 | Intermediate | |
| Oxazepam (Serax) | 30 | 15 | Slow | |
| Temazepam (Restoril) | — | 15 | Intermediate | |
| Triazolam (Halcion) | — | 0.125 | Fast | |
| Antihistamines | ||||
| Diphenhydramine (Benadryl) | 50 | 25 | Fast | |
| Hydroxyzine (Atarax) | 50 | 50 | Fast | |
| Miscellaneous | ||||
| Zolpidem (Ambien) | — | 5 | Fast | |
| Long-acting agents | ||||
| Benzodiazepines | ||||
| Chlordiazepoxide (Librium) | 20 | 20 | Intermediate | |
| Clonazepam (Klonopin) | 1.5 | 1.5 | Intermediate | |
| Clorazepate (Tranxene) | 15 | 15 | Fast | |
| Diazepam (Valium) | 5 | 5 | Very fast | |
| Flurazepam (Dalmane) | 15 | 15 | Very fast | |
| Halazepam (Paxipam) | 40 | 20 | Slow | |
| Prazepam (Centrax) | 15 | 15 | Slow | |
| Quazepam (Doral) | 7.5 | 7.5 | Intermediate | |
— = Not indicated.
*—The dosages given in this table are as established by the Health Care Financing Administration guidelines for fulfilling the requirements of the Omnibus Budget Reconciliation Act (OBRA) of 1987. They are not the maximum dosages. When the OBRA-specified dosage of a drug is exceeded, documentation of necessity is required.
ANTIPSYCHOTIC DRUGS
Because of their many deleterious side effects, antipsychotics should be used only as a last resort in the management of behavioral problems in the elderly (Table 6). The efficacy of these drugs for most problem behaviors is debatable. In several studies,5,8 antipsychotics have been no more effective than placebo. Some investigators believe that antipsychotic drugs should be used only for the management of psychotic features that cause patients “serious distress.”7
TABLE 6. Antipsychotic Drugs Commonly Used in the Elderly
| Drugs | Geriatric dosage (mg per day)* | Side effects | ||||
|---|---|---|---|---|---|---|
| Sedation | Extrapyramidal effects | Anticholinergic effects | Orthostatic hypotension | Tardive dyskinesia | ||
| Phenothiazines | ||||||
| Chlorpromazine (Thorazine) | 75 | High | Moderate | Moderate | High | Yes |
| Fluphenazine (Prolixin) | 4 | Low | High | Low | Low | Yes |
| Mesoridazine (Serentil) | 25 | High | Low | High | Moderate | Yes |
| Prochlorperazine (Compazine) | 10 | Moderate | High | Low | Low | Yes |
| Promazine (Sparine) | 150 | Moderate | Moderate | High | Moderate | Yes |
| Trifluoperazine (Stelazine) | 8 | Low | High | Low | Low | Yes |
| Triflupromazine (Vesprin) | 20 | High | Moderate | High | Moderate | Yes |
| Thioridazine (Mellaril) | 75 | High | Low | High | High | Yes |
| Thioxanthene | ||||||
| Thiothixine (Navane) | 7 | Low | High | Low | Moderate | Yes |
| Butyrophenone | ||||||
| Haloperidol (Haldol) | 4 | Low | Very high | Low | Low | Yes |
| Dibenzoxazepine | ||||||
| Loxapine (Loxitane) | 10 | Low | Moderate | Low | Low | Yes |
| Dihydroindolone | ||||||
| Molindone (Moban) | 10 | Moderate | Moderate | Low | Low | Yes |
| Atypical antipsychotics | ||||||
| Clozapine (Clozaril) | 50 | High | Low | High | Moderate | Low |
| Olanzapine (Zyprexa) | 10 | Moderate to high | Low | Moderate to high | Moderate | Low |
| Quetiapine (Seroquel) | 200 | Moderate | Low | High | Moderate | Low |
| Risperidone (Risperdal) | 2 | Low | Low | Low | Low | Low |
*—The dosages given in this table are as established by the Health Care Financing Administration guidelines for fulfilling the requirements of the Omnibus Budget Reconciliation Act (OBRA) of 1987. They are not the maximum dosages. When the OBRA-specified dosage of a drug is exceeded, documentation of necessity is required.
Common side effects of antipsychotics include sedation, anticholinergic effects, orthostatic hypotension, extrapyramidal symptoms and tardive dyskinesia. Extrapyramidal symptoms include dystonic reactions, pseudoparkinsonism and akathisia. All extrapyramidal symptoms are reversible on discontinuation of antipsychotic drugs.
Dystonic reactions are acute spasms of muscle groups and can result in a fixed upward gaze, neck twisting, facial muscle spasms causing grimacing, a clenched jaw and difficulty with speech. Often painful, dystonic reactions can be quite frightening to patients. These reactions typically occur soon after an antipsychotic drug is initiated.
Pseudoparkinsonism presents with classic parkinsonian symptoms such as rigidity, slowed movements, shuffling gait, slow, monotonous speech and pill-rolling tremor. The symptoms develop over a few weeks of antipsychotic drug therapy.
Akathisia is a form of agitation. Symptoms include inability to sit still, pacing, restlessness, foot tapping, and rocking and shifting of weight while standing. It can be difficult to distinguish akathisia from the agitation that is often present in patients with dementia. Akathisia generally appears days after the initiation of an antipsychotic medication.
Although often considered an extrapyramidal symptom, tardive dyskinesia is a separate, mechanistically distinct phenomenon. It is a long-term side effect that may persist after an antipsychotic drug is discontinued. Typical symptoms are rhythmic involuntary movements of the tongue, lips or jaw, such as protrusion of the tongue or puckering of the lips. Irregular involuntary movements of the extremities or spine are also possible. All traditional antipsychotics may cause tardive dyskinesia.
Older neuroleptic drugs are classified as high, moderate or low potency. Antipsychotic drugs with higher potency have a greater affinity for dopamine receptors and tend to cause more extrapyramidal symptoms. Antipsychotics with lower potency have a greater affinity for histaminic, alpha-adrenergic and muscarinic receptors. These drugs are more likely to cause increased sedation, orthostatic hypotension and anticholinergic effects. Elderly patients are sensitive to all these side effects.
Mounting evidence indicates that newer antipsychotics given in low dosages are much less likely to cause extrapyramidal symptoms.18 These drugs, which include clozapine (Clozaril), olanzapine (Zyprexa), quetiapine (Seroquel) and risperidone (Risperdal), have a greater affinity for dopamine-D2 receptors and are potent antagonists of the serotonin receptor.
Clozapine, olanzapine and, to a lesser extent, quetiapine may cause sedation, anticholinergic effects and orthostatic hypotension. Quetiapine has not been studied in the elderly.18 How this drug compares with other newer antipsychotics remains to be established.19 Risperidone is well tolerated,18 and several studies have demonstrated its efficacy in the management of psychotic and aggressive symptoms in patients with dementia.18,20 Risperidone, in dosages of 0.5 to 1.0 mg per day, has successfully alleviated behavioral disturbances in patients with Alzheimer's disease.21,22 Clozapine is somewhat more difficult to use because of its association with agranulocytosis and the need for periodic monitoring of complete blood counts.
Final Comment
Psychotropic medications are sometimes required to maximize quality of life and functional status in nursing home residents. In tailoring pharmacologic regimens for these patients, physicians need to give careful attention to accurate diagnosis, appropriate dosing, side effects, drug interactions and pertinent drug pharmacokinetics. An ongoing evaluation of effectiveness requires reassessment at regular intervals to rethink medication regimens in light of changes in the health status of geriatric patients.

