Fractures of the humerus, scapula and clavicle usually result from a direct blow or a fall onto an outstretched hand. Most can be treated by immobilization. Dislocation of the humerus, strain or sprain of the acromioclavicular and sternoclavicular joints, and rotator cuff injury often can be managed conservatively. Recurrence is a problem with humerus dislocation, and surgical management may be indicated if conservative treatment fails. Rotator cuff tears are often hard to diagnose because of muscle atrophy that impairs the patient's ability to perform diagnostic maneuvers. Chronic shoulder problems usually fall into one of several categories, which include impingement syndrome, frozen shoulder and biceps tendonitis. Other causes of chronic shoulder pain are labral injury, osteoarthritis of the glenohumeral or acromioclavicular joint and, rarely, osteolysis of the distal clavicle.
Shoulder pain is a common complaint in family practice. Knowledge of the acute and chronic disorders that commonly cause shoulder pain is important because many of them can be managed without referral to a subspecialist.1 This article reviews common causes of shoulder pain and discusses imaging, treatment and indications for referral.
Clavicular Fractures
Clavicular fractures are common, accounting for one of every 20 fractures.2 Most occur in the middle one third of the clavicle. Patients with fracture of the proximal or medial clavicle often have concomitant posterior dislocation of the sternoclavicular joint. Clavicular fractures usually occur during a fall onto an outstretched hand, although some result from a blow to the shoulder. Because the clavicle is directly beneath the skin, these fractures are relatively easy to diagnose: palpation will reveal point tenderness or an obvious deformity. A complete neurovascular examination of the upper extremities should be performed to identify any associated brachial plexus or vascular injuries.
Verification of clinical findings with radiographs is important, particularly to determine whether the patient has a displaced fracture of the proximal or distal clavicle, which may require referral for orthopedic care. A standard anteroposterior (AP) view and an AP view taken with the x-ray beam tilted 45 degrees (cephalic tilt view) are usually adequate. In a patient with substantial trauma, a chest film should be obtained to exclude a concomitant pneumothorax or rib injuries.
Treatment of most clavicular fractures is conservative and consists of a figure-of-eight strap or sling worn for two to four weeks, primarily for comfort. A follow-up radiograph can be obtained four to six weeks after the injury to ensure adequate positioning and healing.
Displaced distal clavicular fractures may result in disruption of the stabilizing ligaments of the acromioclavicular joint. Fractures of this type are more difficult to immobilize properly, and patients with this problem should generally be referred to an orthopedist for further evaluation.
Proximal Humeral Fractures
Humeral fractures are most commonly caused by a direct blow or a fall onto an outstretched hand. Physical examination frequently reveals crepitus at the fracture site. Ecchymosis often occurs within 24 to 48 hours of the injury.
AP and lateral radiographs of the humerus will usually show the fracture. An axillary view should be included if the patient is able to perform the necessary maneuvers (Figure 1). This view is most appropriate for diagnosing dislocations or subtle scapular fractures, particularly those of the coracoid process.3 Because the patient must be able to abduct the arm sufficiently, an axillary view can be difficult to obtain and interpret. The Y view (scapular lateral view) is useful if the patient is unable to abduct the arm (Figure 2).
FIGURE 1.
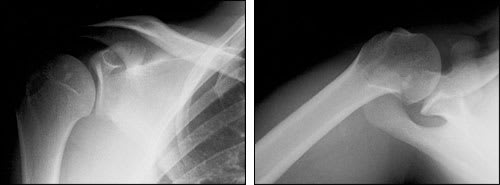
Radiographs of the shoulder. (Left) True anteroposterior view. (Right) Axillary lateral view.
FIGURE 2.
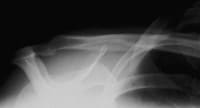
Y view showing the scapula laterally. The humeral head normally overlies the glenoid cavity.
Fractures of the greater tuberosity may be best visualized with an axillary or a Y view. Additional AP views with the humerus in internal and external rotation are sometimes necessary.3
The treatment of stable proximal humeral fractures (those displaced less than 1 cm) consists of a shoulder immobilizer to prevent external rotation and abduction. Referral for surgical treatment may be required for complex fractures (three- and four-part proximal humeral fractures), those involving the anatomic neck, fractures displaced more than 1 cm or those associated with neurovascular injury.4 Follow-up radiographs should be obtained early in treatment to ensure that the fracture fragment has not displaced.
Scapular Fractures
Scapular fractures, which are uncommon,5 result from a direct blow to the scapular area or from extremely high-force impact elsewhere to the thorax. The patient usually has tenderness at the fracture site, and arm abduction is painful. The neck and scapular body are most commonly involved.
Most scapular fractures can be adequately seen with AP and axillary or lateral views of the shoulder. If other injuries are suspected or if the patient was involved in a high-speed or high-force trauma, a chest film and trauma series of the humerus on the affected side should be considered.
Treatment usually consists of a sling for comfort. Range-of-motion exercises are begun as soon as acute pain resolves, usually within two weeks. Early mobilization is important to avoid loss of range of motion, possibly leading to frozen shoulder. Orthopedic referral is indicated for patients with fractures that are unstable or that involve the articular site.
Glenohumeral Dislocation
The glenohumeral joint is normally bathed in a small amount (less than 1 mL) of free synovial fluid. Under normal conditions, the intraarticular pressure is negative, which creates a relative vacuum that resists bony translation.6
The humeral head can dislocate anteriorly, posteriorly or inferiorly in relation to the glenoid fossa. Most shoulder dislocations are anterior. Patients usually hold the affected arm in external rotation and abduction. The humeral head usually is palpable anteriorly, and the diagnosis is often confirmed by locating a dimple in the skin beneath the acromion.
Posterior dislocation is uncommon, and diagnosis is often delayed. Typically, the patient presents with the arm held close to the body in abduction and internal rotation. Usually, external rotation (active and passive) and forward elevation are extremely limited.
Younger athletes and older adults can have a fractured proximal clavicle rather than a dislocation with a similar mechanism of injury.
The diagnosis of glenohumeral dislocation is confirmed with at least two radiographic views of the affected shoulder. A true AP view, with the x-ray beam perpendicular to the plane of the scapula, usually reveals an anterior dislocation but can miss a posterior dislocation. An axillary or a Y view provides a more accurate picture of the anteroposterior position of the humeral head relative to the glenoid fossa3 (Figure 3). If the diagnosis is still unclear after plain films have been obtained, a computed tomographic (CT) scan should be considered. Care should be taken to look for an avulsion fracture of the glenoid (Bankart lesion). This injury usually requires surgical repair (Figure 4).
FIGURE 3.
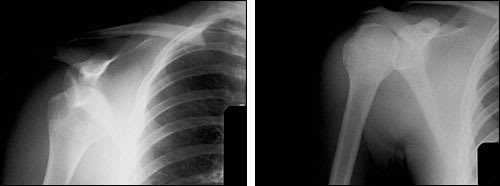
Anteroposterior views of the shoulder, showing anterior dislocation (left) and normal alignment after reduction (right).
FIGURE 4.
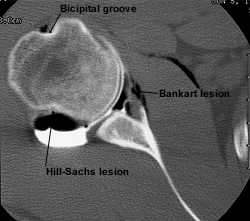
Computed tomographic arthrogram showing a Bankart lesion with a spur extending off the inferior glenoid. The anteroinferior labrum is absent.
A patient with recurrent anterior shoulder dislocation often has subtle clinical findings. Tenderness may be noted over the posterior aspect of the shoulder. The anterior apprehension test usually causes more pain than apprehension. A Hill-Sachs lesion (a bony defect in the posterolateral portion of the humeral head) occurs in more than 50 percent of patients with a primary dislocation.7 This lesion is associated with an increased risk of recurrent dislocation (Table 1). TABLE 1Complications of Anterior Shoulder Dislocation
Complication
Incidence
Recurrent dislocation
Decreased occurrence with age
Bony injury
Hill-Sachs lesion* in > 50% of patients with primary dislocation
Rotator cuff tear
50% in patients < age 40; 80% in those > 60
Vascular injury
Increased occurrence with advanced age
Neurologic injury
Most common in axillary nerve
Arthropathy
20% of patients 10 years after dislocation
*—Bony defect in posterolateral humeral head.
Information from Hovelius L, Augustini BG, Fredin H, Johansson O, Norlin R, Thorling J. Primary anterior dislocation of the shoulder in young patients: a ten-year prospective study. J Bone Joint Surg [Am] 1996;78:1677–84.
Shoulder dislocation is treated with relocation of the humerus (using the method with which the clinician is most familiar) and immobilization, to permit capsular healing. Mobilization of the shoulder and the elbow can usually be resumed within seven to 10 days following injury. Early range-of-motion exercises are important, particularly in older patients, to prevent complications such as frozen shoulder.
A more aggressive rehabilitation program with a shorter course of immobilization has been advocated for elite athletes.8,9 Reported recurrence rates of anterior dislocations, particularly in younger athletes who throw overhead, are as high as 90 percent,10,11 although a recent prospective Swedish study demonstrated lower rates of recurrence.7
The classic treatment of recurrent shoulder dislocations has been open surgery and a Bankart repair (surgical repair of a detachment of the labrum to the glenoid). This approach has a success rate as high as 95 percent.12 In a recent study of young athletes, arthroscopic Bankart repair was compared with three weeks of immobilization for the treatment of an initial anterior shoulder dislocation. The group treated surgically had fewer episodes of recurrent instability than the group managed with immobilization.9 Based on these results, early surgery may have a role in the treatment of high-performance athletes with anterior glenohumeral dislocation.
Acromioclavicular Joint Sprain and Separation
A common injury among athletes and active patients is acromioclavicular (AC) sprain, also referred to as “shoulder separation.” The current classification system recognizes six grades of AC ligamentous injuries (Table 2).13 A direct blow to the superior aspect of the shoulder or a lateral blow to the deltoid area often produces this injury. Occasionally, an AC sprain results from falling onto an outstretched hand. TABLE 2Classification of Acromioclavicular (AC) Joint Injuries
Ligaments or joint
Grade 1
Grade 2
Grade 3
Grade 4
Grade 5
Grade 6
Acromioclavicular ligaments
Sprained
Disrupted
Disrupted
Disrupted
Disrupted
Disrupted
Acromioclavicular joint
Intact
Disrupted or slight vertical separation
Disrupted
Disrupted
Separated
Ruptured
Coracoclavicular ligaments
Intact
Sprained
Disrupted or slight vertical separation
Disrupted
Disrupted
Disrupted
Adapted with permission from Rockwood CA Jr. In: Rockwood CA Jr, Green DP, Bucholz RW. Rockwood and Green's Fractures in adults. 4th ed. Philadelphia, Pa.: Lippincott-Raven, 1996;1341–407.
On examination, the patient has well-localized swelling and tenderness over the AC joint. When an AC joint injury is suspected, the patient should be examined in the sitting position because the weight of the arm in the standing position stresses the AC joint and may exaggerate an existing problem. A palpable “stepped” deformity between the acromion and the clavicle indicates a more severe injury, possibly a complete dislocation. An AP view of the shoulder usually confirms the diagnosis. An axillary view should be obtained if a grade 4 to grade 6 injury is suspected.
Most patients with grades 1 and 2 injuries can be treated without surgery. In some patients, however, a grade 2 lesion can be difficult to differentiate from a grade 3 injury on routine radiographs if the patient supports the injured side. Patients with grade 3 and higher injuries should generally be referred to an orthopedist for possible operative repair. Grades 2 and 3 injuries are often associated with chronic AC joint pain.
Sternoclavicular Joint Sprain and Separation
Anterior sternoclavicular (SC) joint separation occurs when the medial end of the clavicle is displaced anteriorly or anterosuperiorly with respect to the anterior border of the sternum. This injury is most commonly the result of a motor vehicle crash.14 The patient with an SC joint injury will complain of pain, particularly with shoulder adduction. Localized tenderness and deformity are often noted. The head may be tilted toward the side of the dislocation. When the patient is supine, the discomfort is often exacerbated, and the patient cannot place the affected shoulder flat on the examining table. A posterior dislocation can be life-threatening because of compression of the trachea and great vessels of the neck.
The SC joint and proximal physis of the clavicle can be difficult to see on plain films. A modified radiographic view, such as a 40-degree cephalic tilt view, is often helpful. A CT scan can provide more detail about the extent of injury. Mild SC sprains are usually treated conservatively with a sling or figure-of-eight appliance and progressive range-of-motion exercise. Acute SC dislocations can be managed with closed reduction by experienced physicians, but surgical reduction for definitive management is often required.
Rotator Cuff Tear
Tears of the rotator cuff are most common in persons older than 40 years.15 In younger patients, these injuries typically result from trauma. In middle-aged or older patients, a more common presentation is chronic impingement syndrome, often resulting in rupture of the cuff. When a rotator cuff ruptures, the resulting muscular atrophy often limits the patient's ability to perform the necessary diagnostic maneuvers. In these patients, a rotator cuff tear can be difficult to diagnose clinically. An AP view of the glenohumeral joint may show calcific tendonitis of the cuff and superior migration of the humeral head, which should prompt further imaging studies if the clinician suspects a tear15,16 (Table 3). TABLE 3Imaging Studies of the Shoulder
Imaging modality
Advantages
Disadvantages
MRI
95% sensitivity and specificity in detecting complete rotator cuff tears, cuff degeneration, chronic tendonitis and partial cuff tears
Often identifies an apparent “abnormality” in an asymptomatic patient
No ionizing radiation
Arthrography
Good at identifying complete rotator cuff tear or adhesive capsulitis (frozen shoulder)
Invasive
Relatively poor at diagnosing a partial rotator cuff tear
Ultrasonography
Accurately diagnoses complete rotator cuff tears
Less useful in identifying partial cuff tears
Operator-dependent interpretation
MRI arthrography
Reliably identifies full-thickness rotator cuff tears and labral tears
Invasive
CT scanning
May be useful in diagnosis of subtle dislocation
Ionizing radiation
MRI = magnetic resonance imaging; CT = computed tomographic.
Treatment consists of surgical repair in younger and selected older patients or rehabilitation in patients who are not good candidates for surgery. Early identification of a rotator cuff tear is important so that consultation for possible surgical repair can be considered. Repair within three weeks of injury is recommended to avoid tendon retraction, reinjury, tendon degeneration and muscle atrophy.
Impingement Syndrome
The rotator cuff occupies the space between the coracoacromial arch and the humerus. With abduction of the arm, the tendons of the rotator cuff can be impinged between the bony structures of the arch and the humerus. The impingement syndrome was described by Neer17,18 as a series of pathologic changes in the supraspinatus tendon: stage I causes hemorrhage and edema; stage II, tendonitis and fibrosis; and stage III, tendon degeneration of the rotator cuff and biceps, bony changes and tendon rupture.
Pain related to impingement usually occurs over the anterolateral aspect of the shoulder, often with some radiation to, but not usually beyond, the elbow. Typically, the pain is aggravated by overhead activity and is worse at night. Patients often report a clicking or popping sensation in the affected shoulder. In young throwing athletes with these symptoms, however, the examiner should be concerned about the possibility of a labral disorder. Biceps tendonitis frequently occurs in the later stages of impingement, and rehabilitation can help correct this problem.19
The examiner should distinguish between primary and secondary impingement. Initial treatment of both conditions is conservative, but when conservative treatment fails, the surgical approach to the two problems differs markedly. Symptoms in older patients usually reflect chronic overuse and degeneration of the supraspinatus tendon. This process is referred to as primary impingement. For instance, a 65-year-old patient with anterior shoulder pain probably has primary outlet impingement. In contrast, a 17-year-old baseball pitcher is more likely to have secondary impingement, with an underlying problem of instability. This patient will often complain of arm heaviness and numbness (“dead arm” syndrome) rather than shoulder pain.20
Therefore, the primary diagnosis in younger throwing athletes is typically subtle glenohumeral instability with secondary impingement and subacromial bursitis noted on examination. Weakness in the scapular stabilizers can play an important role in the development of shoulder problems, particularly in athletes.21 Repeated stresses from overhead motions like throwing can lead to fatigue of the muscles that stabilize the humeral head and prevent anterior subluxation. Secondary impingement, therefore, can occur when the fatigue and dysfunction of the rotator cuff cause the humeral head to migrate superiorly within the glenohumeral joint, impinging the rotator cuff tendon under the coracoacromial arch.
Other causes of impingement include a curved or hooked acromion, AC spurring and a thickened coracoacromial ligament.22 Radiographs should be considered if a patient shows no improvement after two to three months of conservative therapy for presumed impingement syndrome (Table 4).23 Degenerative changes at the AC joint, sclerosis, osteophyte formation at the inferior aspect of the acromion and sclerosis or cyst formation at the site of supraspinatus tendon insertion into the greater tuberosity should increase the clinician's suspicion of impingement and chronic rotator cuff tears. In some cases, magnetic resonance imaging (MRI) or other imaging studies (Table 3) may be necessary. T2-weighted MRI has a reported accuracy of 84 to 100 percent in the diagnosis of rotator cuff tears.15,16 TABLE 4Suggested Radiographs for Anterior Shoulder Pain
Radiograph
Abnormality best visualized
AP view of glenohumeral joint
Degenerative glenohumeral changes
AC joint
AC degenerative changes
AC joint separation
Distal clavicle fracture
Axillary lateral view of shoulder
Glenohumeral dislocation
Bony Bankart lesion*
Supraspinatus outlet (arch)
Abnormality of acromion process
Degenerative changes of anterior acromion
AP = anteroposterior; AC = acromioclavicular.
*—Avulsion fracture of the glenoid.
Adapted with permission from Lyons PM, Orwin JF. Rotator cuff tendinopathy and subacromial impingement syndrome. Med Sci Sports Exerc 1998;30(4 suppl):S12–7.
Initial treatment of most patients with impingement syndrome (primary and secondary) is conservative, especially in the acute phase of pain: rest, nonsteroidal anti-inflammatory drugs (NSAIDs), icing and avoiding aggravating activities. It may be necessary to modify the patient's work activities, particularly overhead lifting. After most of the pain has resolved, a rotator cuff strengthening program should be instituted. In some patients, particularly athletes with secondary impingement, scapular rotator cuff strengthening also should be incorporated into the physical therapy program. Athletes with secondary impingement and underlying instability who fail to show improvement with conservative therapy should be referred for consideration of a stabilization procedure. In contrast, an older patient with primary impingement would probably undergo open or arthroscopic subacromial decompression.
A corticosteroid injection can be therapeutic and diagnostic in patients with impingement syndrome. If the diagnosis of impingement is uncertain, lidocaine (Xylocaine) and/or bupivacaine (Marcaine) can be injected into the subacromial space. After the drug has dispersed for several minutes, impingement tests can be repeated. A decrease in pain increases the certainty that impingement is the primary process. Corticosteroids are often combined with anesthetics in this procedure. A recent randomized, double-blind study24 noted significant short-term relief of subacromial impingement symptoms with corticosteroid injections.
Frozen Shoulder
Adhesive capsulitis, or frozen shoulder, results from thickening and contraction of the capsule around the glenohumeral joint and causes loss of motion and pain. Frozen shoulder classically consists of shoulder pain that is slow in onset and presents without any radiographic abnormalities. Usually, the discomfort is localized near the deltoid insertion, the patient is unable to sleep on the affected side and glenohumeral elevation and external rotation are restricted.
Frozen shoulder most often occurs as a result of immobility following a shoulder injury. An autoimmune cause of frozen shoulder has been proposed.25,26 The diagnosis is usually made clinically, and physicians should always be concerned about a possible underlying rotator cuff tear. Radiographs often appear normal, although osteopenia of the humeral head may be noted as a result of disuse. Arthrography demonstrates generalized constriction of the joint capsule, with loss of the normal axillary and subscapularis spaces (Table 3). The capsule can be dilated during arthrography, converting the procedure from a diagnostic to a therapeutic one.
A carefully designed treatment plan for patients with frozen shoulder may include physical therapy, pain medication such as NSAIDs and, occasionally, intra-articular corticosteroid injection. Surgical referral may be indicated after conservative treatment has failed, although the exact timing of surgery should be decided on an individual basis.
Biceps Tendonitis
Biceps tendonitis results from inflammation of the sheath around the long head of the biceps and is usually manifested by discrete pain and tenderness in the area of the bicipital groove, often occurring concomitantly with impingement syndrome or rotator cuff tear. Management is usually conservative; rest, icing, NSAIDs and corticosteroid injections may all be helpful. When conservative management fails, surgical transfer of the tendon may be necessary.
Labral Injury
The SLAP lesion (superior labrum anterior and posterior) and other glenoid labral tears are common in throwing athletes who present with a painful shoulder that clicks or pops with motion. Patients often have a positive “clunk” test,27 especially in the overhead position. They may have tenderness to deep palpation over the anterior glenohumeral joint and signs of laxity or instability. Plain films are often normal, and MRI arthrography may be needed to view the torn labrum (Table 3). For patients who do not respond to rest, NSAIDs and physical therapy, arthroscopic or open surgical repair may be indicated.
Glenohumeral Arthritis
Arthritis of the glenohumeral joint generally causes pain with activity, loss of passive motion and stiffness. Some patients may complain of nighttime pain. Causes of arthritis include previous trauma, rheumatoid arthritis, rotator cuff tear and Lyme disease. Multiple joint involvement is suggestive of rheumatoid arthritis.
An AP view of the glenohumeral joint will usually reveal degenerative changes and loss of joint space (Table 2). Treatment is initially conservative, using heat and ice, NSAIDs, range-of-motion exercises and corticosteroid injections. Patients for whom conservative therapy fails can be referred for further evaluation and treatment.
Osteolysis of the Distal Clavicle
Atraumatic osteolysis of the distal clavicle is an unusual injury that occurs most often in weight lifters.28 Although its cause remains obscure, the problem most likely begins as a stress fracture. Subsequent bone resorption causes cystic and erosive changes, and bone remodeling cannot occur because of the continual stress imposed on the joint. Patients typically have dull pain over the AC joint, which is often worst at the beginning of an exercise period. Any movement requiring abduction of the arm more than 90 degrees is painful.
Plain films of the AC joint and clavicle usually confirm the diagnosis. Key findings include osteopenia and lucency in the distal clavicle (Figure 5). Treatment consists of discontinuing load-bearing activity. Conservative management should be used for as long as the patient will comply. Consideration for resection of the distal clavicle should be individualized according to each patient's functional demands and symptoms.
FIGURE 5.
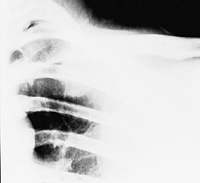
Osteopenia and lucency in a patient with osteolysis of the distal clavicle.

