Lichen planus is an inflammatory mucocutaneous condition with characteristic violaceous polygonal flat-topped papules and plaques. Pruritus is often severe. Skin lesions may be disfiguring, and involvement of the oral mucosa or genital mucosa in severe cases may be debilitating. Oral lichen planus may predispose to the development of squamous cell carcinoma within lesions. Involvement of the scalp and the nails may also occur. While most cases of lichen planus are idiopathic, some may be caused by the ingestion of certain medications (e.g., gold, antimalarial agents, penicillamine, thiazide diuretics, beta blockers, nonsteroidal anti-inflammatory drugs, quinidine and angiotensin-converting enzyme inhibitors) or linked to hepatitis C virus infection. Patients with localized lichen planus are usually treated with potent topical steroids, while systemic steroids are used to treat patients with generalized lichen planus.
Lichen planus is an inflammatory mucocutaneous condition that usually exhibits a distinctive morphology. The prevalence of lichen planus is unknown, but it is estimated to occur in less than 1 percent of the population. Estimates of the prevalence vary among different populations, but the condition does not appear to exhibit a racial predilection. It most commonly affects middle-aged adults of both sexes, with a slight predominance in women.1
Clinical Presentation
The classic appearance of skin lesions includes violaceous polygonal flat-topped papules and plaques (Figure 1). Close examination reveals a reticulated pattern of white scale known as Wickham's striae (Figure 2). Early cutaneous lesions may be difficult to diagnose, often appearing as scattered erythematous papules (Figure 3). More developed and extensive lesions may mimic discoid lupus, psoriasis or secondary syphilis. The flexor surfaces of the extremities, particularly the wrists, are common locations for lichen planus.
FIGURE 1.
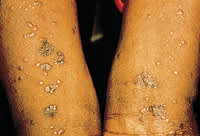
Cutaneous lesions of classic lichen planus.
FIGURE 2.
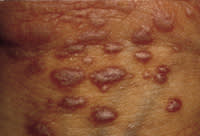
Close-up reveals Wickham's striae.
FIGURE 3.
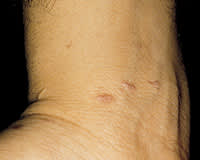
Early, scattered lesions of lichen planus.
Another clue to the diagnosis is that lesions may occur in areas exposed to trauma, such as lacerations. This tendency is known as an isomorphic response, or Koebner's phenomenon. Lesions often resolve with intense hyperpigmentation. Some physicians describe lichen planus with the six “Ps”: pruritic, polygonal, planar (flat-topped), purple papules and plaques. While some patients may be asymptomatic, most experience intense pruritus, a hallmark of lichen planus.
While this “classic” form of cutaneous lichen planus is the most common, other variants do exist and exhibit various morphologies. Patients with hypertrophic lichen planus present with thick hyperkeratotic plaques, commonly found on the anterior surface of the legs (Figure 4). In vesiculobullous lichen planus, patients exhibit blisters within the plaques, while the actinic type of lichen planus occurs on sun-exposed areas of skin.
FIGURE 4.
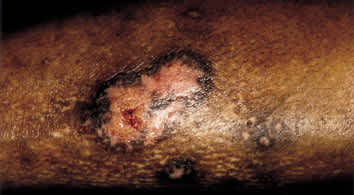
Hypertrophic lichen planus on the anterior surface of the leg.
While lichen planus often occurs only on cutaneous surfaces, it may also involve the oral mucosa, the genital mucosa, the nails and the scalp. Moreover, these areas may be exclusively involved. Oral lichen planus classically presents on the buccal mucosa as a white, lacy, reticular pattern (Figure 5). Papular, atrophic or erosive lesions may also occur. Erosive lesions, in particular, may be quite painful and lead to multiple complications such as secondary infections (particularly candida), and poor nutrition and dehydration secondary to pain. Patients with long-term oral mucosal lesions have an increased risk of developing squamous cell carcinoma within the lesions.2 Patients with these lesions should undergo regular oral follow-up, and a biopsy of any suspicious lesions should be performed.
FIGURE 5.
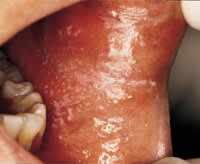
Reticular oral lichen planus of the buccal mucosa.
Genital lichen planus may also exhibit various morphologies. In men, the classic lesion is visible as violaceous papules on the glans penis. In women, violaceous papules, hypertrophic lesions or erosions may occur, typically on the vulva. Erosive lichen planus may be very painful, and in longstanding cases, may lead to alterations of the genital architecture.3 Squamous cell carcinoma has been reported in patients with genital lichen planus; therefore, follow-up and biopsy of any suspicious lesions are necessary.
Lichen planus may also involve the nails and the scalp. Multiple types of nail changes may occur that include ridging, distal splitting, thinning, subungual hyperkeratosis, pterygium formation and even loss of the nail.1,4 However, none of these findings are specific to lichen planus. Additionally, lichen planus of the nails is often resistant to treatment. Lichen planus lesions that appear on the scalp are known as lichen planopilaris. Patients usually present with the initial clinical sign of areas of hair loss with keratotic follicular papules (Figure 6). If left untreated, these areas progress to scarring alopecia. The hair follicles are destroyed and regrowth of hair will not occur.
FIGURE 6.
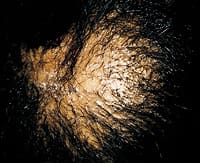
Lichen planus of the scalp.
Diagnosis
A diagnosis of lichen planus is reached on the basis of the typical clinical appearance and a punch biopsy of the lesion. Histopathology reveals characteristic findings of a band-like infiltrate of lymphocytes at the epidermal-dermal junction and damage to the basal cell layer. Epidermal changes include wedge-shaped hypergranulosis and irregular acanthosis leading to a saw-toothed appearance.5
Etiology
The etiology of lichen planus is unknown, although many studies have investigated and support an immunologic pathogenesis. Lymphocytes, particularly T-cells, play a major role.1,4,6 Other factors include antigen-presenting cells, adhesion molecules and inflammatory cytokines. While most cases of lichen planus are idiopathic, some are linked to medication use or hepatitis C virus (HCV) infection.
Lichenoid drug eruptions are reactions that may occur after exposure to various medications. These eruptions may exhibit a cutaneous and histologic appearance identical to that of idiopathic lichen planus and, thus, must be considered in every patient with lichen planus. While an exhaustive list of possible offending agents is quite long, the most common include gold, antimalarial agents, penicillamine, thiazide diuretics, beta blockers,7 nonsteroidal anti-inflammatory drugs, quinidine and angiotensin-converting enzyme inhibitors.8
The interval between administration of the offending medication and the development of the lichenoid drug eruptions is usually a few months, although it may range from 10 days to several years.8 While the eruptions spontaneously clear anywhere from weeks to months after discontinuation of the medication in many patients, some patients require systemic therapy. Unfortunately, no test is available to confirm the causality of a particular medication. If the patient is taking a potentially offending medication, it should be discontinued whenever possible.
In the past few years, lichen planus has been linked to HCV infection, with studies demonstrating a higher prevalence of anti-HCV antibody titers in patients with cutaneous and oral lichen planus, compared with control subjects.9–14 The reported rates of association have differed widely, probably because of varying study design, oral versus cutaneous lichen planus and geography.
One study12 reported that, in Indianapolis, a region with a low endemic prevalence of HCV, tests for HCV antibody were positive in 3.5 percent of patients with lichen planus. However, only patients with abnormal liver function tests were screened. Two studies of patients with lichen planus that did not exclude patients with normal liver function reported a positive HCV antibody in 23 percent of patients tested in Miami13 and 60 percent of patients tested in a region of Japan with a high endemic HCV prevalence.14
Although the manner in which HCV infection predisposes patients to the development of lichen planus is unknown, some speculate that long-term infection may lead to an aberrant immunologic response.9 Considering the current evidence, it is appropriate to screen all patients with lichen planus for HCV infection.
Treatment
The treatment of patients with lichen planus must be individualized (Table 1).1,4,15–17 Patients vary greatly in severity of symptoms, extent of lesion involvement and response to treatment. Many treatment options are discussed in the literature, each with its own risk profile. Unfortunately, larger randomized trials to support the effectiveness of most of these treatments are lacking, and many treatments are recommended based on anecdotal evidence. Another factor to consider when treating patients with cutaneous lichen planus is that spontaneous remissions occur in the majority of patients after one year.18 TABLE 1Treatment of Lichen Planus
Treatment
Indication
Instructions
Efficacy
Advantages
Disadvantages
Potent topical corticosteroid creams or ointments: clobetasol (Temovate), halobetasol (Ultravate), augmented betamethasone diproprionate (Diprolene), diflorasone (Psorcon)1,15
Localized cutaneous
Apply a thin layer to involved areas twice daily, for an initial trial of 2 to 3 weeks; occlusion may be used to enhance effects*
Widely used, although no controlled study has proved efficacy
When used appropriately, no systemic side effects
Use of topical corticosteroids may be cumbersome for some patients; use of lesser potency steroids is required (hydrocortisone, 2.5%) on the face, axillae, groin or genitals; higher potency steroids may rarely be used (with caution) in these locations for severe disease*
Systemic corticosteroids1,4,15,16
Generalized cutaneous
Oral prednisone, 30 to 60 mg, once daily for 4 to 6 weeks, then taper over next 4- to 6- week period; lower doses and other types of corticosteroids have been used
Widely used and alleviates symptoms in most patients, but unclear if total duration of disease is affected
Quick and often dramatic relief of symptoms
Many possible side effects that include effects on blood pressure, blood glucose and bone density
Acitretin (Soriatane)15
Generalized cutaneous; resistant to corticosteroids
30 mg taken orally once daily for 8 weeks
Efficacy demonstrated by controlled trial
Effective oral therapy of relatively brief duration
Physician must be experienced in prescribing retinoids; severe risk of teratogenicity and other possible systemic side effects (e.g., hepatotoxicity, increase in triglycerides); regular laboratory monitoring necessary
PUVA (psoralen plus UVA phototherapy)15
Generalized cutaneous; resistant to corticosteroids
Administered 3 times weekly; duration of treatment based on response; good results reported with 8 weeks of treatment
Efficacy not demonstrated by controlled trial, but open studies report good results
Limited systemic side effects
Oral psoralens may induce nausea; PUVA therapy increases risk of skin cancer; patient must travel to phototherapy center for each treatment
Topical corticosteroids in alternative vehicle (i.e., fluocinonide [Lidex] ointment, 0.05% in Orabase)4,17
Oral
Apply to dried oral mucosa 6 times daily; taper use as patient improves
Efficacy demonstrated in controlled trial of 9 weeks' duration
When used appropriately, no systemic side effects
Use of topical corticosteroids may be cumbersome for some patients
Intralesional triamcinolone acetonide (Kenalog)1,15
Hyperkeratotic or resistant localized plaques
Intralesional injection of 5 to 10 mg per mL into plaque
Anecdotal evidence
When used appropriately, no systemic side effects
Local atrophy, useful only for localized lesions
*—Use of any potent topical corticosteroid on extensive surface areas for more than two weeks or under occlusion increases risk of atrophy, striae, and systemic absorption.
Potent topical corticosteroids are used to treat the early or localized lesions of patients with cutaneous lichen planus. These ointments or creams are applied to the affected areas twice daily, with an initial trial treatment period of two to three weeks to monitor efficacy. Occlusion may be used to enhance the effect of the topical medication. For resistant or hyperkeratotic plaques, intralesional injections of triamcinolone acetonide (Kenalog) may be used.1,15
Oral corticosteroids are the most common treatment for patients with generalized cutaneous lichen planus,15,16 although recommendations concerning dosage and duration of therapy vary. The recommended prednisone dosage is 30 to 60 mg once daily for four to six weeks, with the dosage then tapered over the following four- to six-week period.4 Other studies suggest treating patients at lower doses of prednisone or with other forms of corticosteroids, including short courses of oral prednisolone16 or intravenous methylprednisolone.15 While systemic corticosteroids alleviate symptoms in most patients, it is unclear whether this therapy affects the total duration of the disease.4,15
[ corrected] If corticosteroid resistance occurs, other treatment options are available. One controlled trial15 demonstrated efficacy of treatment with a dosage of 30 mg daily of acitretin (Soriatane) once daily for eight weeks. When prescribing any retinoid, however, physicians must be familiar with the risk profile because of the severe teratogenicity associated with this class of drugs. Phototherapy using psoralens (PUVA) has also been reported to be effective in corticosteroid resistance. Although the duration of treatment is determined by patient response, good results have been reported after eight weeks of treatment. Multiple other therapies, such as griseofulvin (Grisactin), cyclosporine (Sandimmune), dapsone and hydroxychloroquine (Plaquenil), have been anecdotally reported as effective for the treatment of patients whose lichen planus is corticosteroid-resistant.4,15
A topical corticosteroid is considered first-line therapy for patients with oral lichen planus.15 One controlled trial17 demonstrated the effectiveness of fluocinonide (Lidex) ointment applied to dried oral mucosa six times daily for nine weeks. The steroid, in an adhesive base, was prepared by the pharmacy, although Orabase has also been recommended as an occlusive vehicle.4 Other topical medications and systemic therapies have been used to treat patients with oral lichen planus15 that is corticosteroid-resistant. These therapies include topical cyclosporine, systemic corticosteroids, topical and systemic retinoids and oral PUVA.

