Aphthous ulcers are a common and painful problem. Benign aphthae tend to be small (less than 1 cm in diameter) and shallow. Aphthous ulcers that occur in conjunction with symptoms of uveitis, genital ulcerations, conjunctivitis, arthritis, fever or adenopathy should prompt a search for a serious etiology. The lack of clarity regarding the etiology of aphthous ulcers has resulted in treatments that are largely empiric. These treatments include antibiotics, antiinflammatories, immune modulators, anesthetics and alternative (herbal) remedies.
Aphthous ulcers can be classified into three different types: minor, major and herpetiform.1,2 Minor aphthae are generally located on labial or buccal mucosa, the soft palate and the floor of the mouth. They can be singular or multiple, and tend to be small (less than 1 cm in diameter) and shallow3 (Figure 1). Major aphthae are larger and involve deeper ulceration. Major aphthae may also be more likely to scar with healing2 (Figure 2). Herpetiform aphthae frequently are more numerous and vesicular in morphology. Patients with benign aphthous ulcers should have no other findings such as fever, adenopathy, gastrointestinal symptoms or other skin or mucous-membrane symptoms.
FIGURE 1.
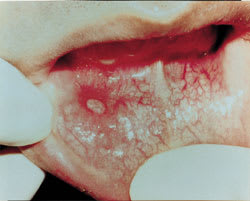
Minor aphthous ulcer.
FIGURE 2.
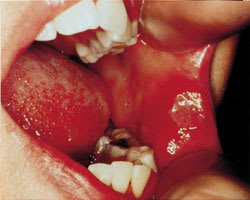
Major aphthous ulcer.
Pathophysiology
The pathophysiology of aphthous ulcers is poorly understood. Histologically, aphthae contain a mononuclear infiltrate with a fibrin coating.3 Patients with recurrent aphthae may have alteration of local cell–mediated immunity. Systemic T- and B-cell responses have also been reported as altered in patients with recurrent aphthae.2
Etiology
Aphthae more commonly affect young adults, and a familial tendency may exist.3 Paradoxically, smoking offers a somewhat protective effect against recurrent aphthae.2 Other etiologic factors such as stress, physical or chemical trauma, food sensitivity and infection have been proposed. Infectious agents such as Helicobacter pylori and herpes simplex virus have been investigated but have not been consistently found in aphthous ulcers.4 The lack of clarity regarding etiology has resulted in treatments that are largely empiric and aimed at symptom reduction.
Differential Diagnosis
Several conditions should be considered in the differential diagnosis when evaluating patients with recurrent aphthae. A primary consideration is that benign aphthae tend to be smaller and are more often self-limited when compared to more serious conditions. Major aphthae can be associated with human immunodeficiency virus (HIV) infection; clinicians should consider HIV testing when aphthae are large and slow to heal. Table 1 outlines the differential diagnosis of aphthous ulcers, with distinguishing features.
TABLE 1 Differential Diagnosis of Aphthous Ulcers
| Diagnosis | Potential differentiating features | |
|---|---|---|
| Infection | ||
| Viral | ||
| Herpesvirus | Vesicular lesions, Tzank stain positive for inclusion-bearing giant cells | |
| Cytomegalovirus | Immunocompromised patient, biopsy positive for multinucleated giant cells | |
| Varicella | Characteristic skin lesions | |
| Coxsackievirus | Hand/foot/buttock lesions, typically in children | |
| Treponemal | ||
| Syphilis | Risk factors, other skin lesions, RPR/FTA test is positive | |
| Fungal | ||
| Cryptosporidium, mucormycosis, histoplasma | Immunocompromised patient, chronicity, biopsy and culture positive | |
| Autoimmune | ||
| Behçet's syndrome | Genital ulceration, uveitis, retinitis | |
| Reiter's syndrome | Uveitis, conjunctivitis, HLA B27 arthritis | |
| Inflammatory bowel disease | Recurrent bloody or mucous diarrhea, other GI ulcerations | |
| Lupus erythematosus | Malar rash, ANA-positive | |
| Bullous pemphigoid | Diffuse skin involvement | |
| Pemphigus vulgaris | Diffuse skin involvement | |
| Hematologic | ||
| Cyclic neutropenia | Periodic fever, neutropenia | |
| Neoplasm | ||
| Squamous cell carcinoma | Chronicity, head/neck adenopathy, biopsy positive | |
RPR/FTA = rapid plasma reagin/fluorescein treponema antibody test; GI = gastrointestinal; ANA = antinuclear antibody.
Infection-causing ulceration in the mouth should be considered when evaluating patients with oral symptoms. A common infection, particularly in patients with HIV infection and aphthae, is herpes5 (Figure 3). When Tzank staining is available, a sample from a herpetic lesion will reveal inclusion-bearing giant cells. Other viral, bacterial, treponemal and fungal agents have the potential to cause mouth ulcers. Biopsy alone or in conjunction with a culture of lesions or blood testing may aid in distinguishing the causative agent.
FIGURE 3.
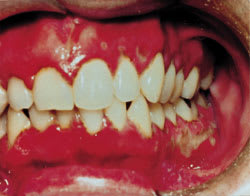
Herpes stomatitis, found primarily on the alveolar mucosa. Tzank stain of a lesion scraping revealed inclusion-bearing giant cells.
AUTOIMMUNE DISEASES
Several autoimmune diseases may mimic benign aphthous ulcers. Behçet's syndrome is an autoimmune vasculitis that causes recurrent oral and genital ulcerations, uveitis and retinitis. Severe aphthae and Behçet's syndrome may be two points on a disease continuum. Non-oral symptoms of Behçet's syndrome may be present in 43 to 100 percent of patients with recurrent aphthous ulcers, depending on severity.6 Reiter's syndrome is associated with oral ulcers, uveitis, conjunctivitis and HLA B27-positive arthritis following nongonococcal urethritis or bacillary dysentery.3 Patients with inflammatory bowel disease, in particular Crohn's disease, may present with associated mouth ulcerations. Lupus erythematosus, bullous pemphigoid and pemphigus vulgaris are other diseases that may involve ulceration of the mouth. In all of these conditions, the associated symptoms should be elicited to make a differentiation from benign recurrent aphthae.
HEMATOLOGIC/ONCOLOGIC DISEASES
Hematologic etiologies should be considered when evaluating recurrent or slow-healing mouth ulcers. Cyclic neutropenia is associated with mouth ulcers during neutropenic periods.2 Fever may also be a presenting symptom during these periods. Consideration may be given to blood count measurement if fever and mouth ulcers regularly occur together. Finally, a neoplasm such as squamous cell carcinoma must be ruled out when evaluating patients with persistent, nonhealing mouth ulceration. Office punch biopsy or surgical biopsy may help make this distinction. Evaluation of the head and neck for adenopathy is particularly important in this situation.
Treatment
Treatment for oral aphthae can be divided into five categories: antibiotic, anti-inflammatory, immune modulatory, symptomatic and alternative (Table 2). The lack of predictability of the efficacy of a particular treatment mirrors the mystery surrounding the etiology of the condition.
TABLE 2 Common Treatments for Aphthous Ulcers
| Agent | Dosage | Evidence for use |
|---|---|---|
| Tetracycline capsule, 250 mg | 1 capsule dissolved in 180 mL of water; rinse with this suspension four times daily for 4 to 5 days | Randomized, controlled studies1 support use |
| Tetracycline syrup, 250 mg per 5 mL | 5 mL “swish and spit” four times daily for 4 to 5 days | As above |
| Minocycline tablet, 100 mg | 1 tablet dissolved in 180 mL of water; rinse with this suspension twice daily for 4 to 5 days | As above |
| Triamcinolone 0.1% in Orabase (Kenalog in Orabase) | Apply to dried ulcer two to four times daily until healed | Randomized, controlled studies1 show decreased pain |
| Dexamethasone elixir, 0.5 mg per 5 mL | Swish and spit with 5 mL every 12 hours | As above |
| Thalidomide | 200 mg, one to two times daily for 3 to 8 weeks Warning: contraindicated in pregnancy | Studies in HIV-infected patients only7 |
| Amlexanox 5% paste | Apply to dried ulcer two to four times daily | Randomized, controlled studies9,10 show decreased symptoms and faster healing |
| Viscous lidocaine, 2% | Apply to ulcer as needed | For brief local pain relief only |
| Zinc lozenges | Suck one lozenge four to six times daily | No studies |
| Vitamin C, 500 mg | One tablet, four times daily | No studies |
| Vitamin B complex | One tablet, four times daily | No studies |
| l-Lysine, 500 mg | One tablet, one to three times daily | Studies in herpes only |
ANTIBIOTIC THERAPY
Topical and systemic antibiotic treatments are empiric and are used because of a belief that some as-yet-undiscovered infectious agent is causing the aphthous ulcer. Tetracycline and minocycline are the agents most commonly used. A 250-mg antibiotic capsule of tetracycline can be dissolved in 180 mL water and used as a “swish and swallow” or “swish and spit” treatment four times per day for several days in adult patients. Reduction of pain and duration of ulcerations may result. Tetracycline suspension, 250 mg per 5 mL, can also be used in a similar fashion, with 5 mL swished four times per day. (In children and in women who may be pregnant, tetracycline should be avoided because of its tendency to discolor teeth.) Minocycline can also be used this way, with a 100-mg tablet dissolved in 180 mL water and swished twice per day.1 The same precautions for children and women apply. In addition, minocycline use can cause fetal harm. Therefore, women who are pregnant or who become pregnant while taking the antibiotic should be informed of the potential for harm to the fetus.
ANTI-INFLAMMATORY AGENTS
Local anti-inflammatory agents may be the most helpful way to speed healing and relieve symptoms in the management of recurrent minor aphthous ulcers. Triamcinolone 0.1 percent (Kenalog in Orabase) can be applied to ulcers two to four times a day.1 This preparation also provides a protective local coating for the ulcer. Early initiation of this treatment may result in a more rapid response. The paste can be applied until the ulcer is healed. For more extensive oral ulceration, dexamethasone elixir, 0.5 mg per 5 mL, may be used as a rinse and expectorated.1 Patients should be warned of the potential for secondary fungal infection when using a steroid rinse. Systemic steroids are generally not recommended in the management of aphthous ulcers, although they may be helpful in the management of conditions that mimic aphthous ulcers.
IMMUNE MODULATORS
Immune modulators used for the management of aphthous ulcers have been investigated most thoroughly in patients infected with HIV. Aphthous ulcers in HIV-infected patients may have extremely protracted healing times, up to months. Thalidomide (Thalomid) is the agent most frequently used for management of aphthous ulcers that cause severe pain with eating. Thalidomide in a dosage of 200 mg once to twice daily for three to eight weeks yields a faster healing rate than placebo.7,8 Thalidomide is contraindicated in non-HIV–infected patients because of its potential for significant side effects and teratogenicity.
Amlexanox 5 percent paste (Aphthasol) has been examined in several studies of the treatment of aphthous ulcers. The paste was applied to ulcers two to four times a day.9 Healing time was improved with this agent. In one large study, 21 percent of patients achieved complete healing at three days compared with 8 percent of untreated patients.10
OTHER AGENTS
Other strategies exist for local and systemic symptom relief in patients with aphthous ulcers. Pain relief may be achieved with 2 percent viscous lidocaine applied with a cotton swab several times daily, as needed.1,11 Over-the-counter benzocaine preparations (e.g., Anbesol and Oragel) may also be used. Over-the-counter agents such as Orabase or Zilactin-B coat aphthous ulcers and provide local protection.11 Brief anesthesia may be obtained with the application of a silver nitrate stick, although the application itself is quite painful. Silver nitrate may cause more local necrosis and, ultimately, delayed healing. Finally, the combination of over-the-counter magnesium hydroxide antacid and diphenhydramine hydrochloride (5 mg per mL), mixed half and half, will bring about some symptom relief.1 A 5-mL dose of the mixture can be swished and swallowed four to six times a day. Systemic nonsteroidal anti-inflammatory agents or acetaminophen may provide some analgesia when ulcers are very painful.
ALTERNATIVE AGENTS
Sucking on zinc gluconate lozenges is anecdotally reported to provide local relief and speeding of healing time for aphthous ulcers. Vitamin C, vitamin B complex and lysine may speed healing when taken orally at the onset of lesions. Sage and chamomile mouthwash, created by infusing equal amounts of the two herbs in water, may be helpful when used four to six times a day. Echinacea is reported to speed healing, perhaps through its immune modulatory effect. Carrot, celery and cantaloupe juices also have been reported as helpful complementary agents.12 None of these agents has been studied in randomized controlled trials.
Final Comment
Aphthous ulcers are a poorly understood clinical entity that cause significant pain in otherwise healthy patients. Several agents are helpful in the management of aphthous ulcers, including antibiotics, antiinflammatories, immune modulators, anesthetics and alternative products. When ulcers are slow to heal or if associated systemic symptoms are present (e.g., uveitis, arthritis, fever, adenopathy), other, more serious conditions should be ruled out.

