A history and physical examination, focusing on risk factors for cardiac, pulmonary and infectious complications, and a determination of a patient's functional capacity, are essential to any preoperative evaluation. In addition, the type of surgery influences the overall perioperative risk and the need for further cardiac evaluation. Routine laboratory studies are rarely helpful except to monitor known disease states. Patients with good functional capacity do not require preoperative cardiac stress testing in most surgical cases. Unstable angina, myocardial infarction within six weeks and aortic or peripheral vascular surgery place a patient into a high-risk category for perioperative cardiac complications. Patients with respiratory disease may benefit from perioperative use of bronchodilators or steroids. Patients at increased risk of pulmonary complications should receive instruction in deep-breathing exercises or incentive spirometry. Assessment of nutritional status should be performed. An albumin level of less than 3.2 mg per dL (32 g per L) suggests an increased risk of complications. Patients deemed at risk because of compromised nutritional status may benefit from pre- and postoperative nutritional supplementation.
The purpose of a preoperative evaluation is not to “clear” patients for elective surgery, but rather to evaluate and, if necessary, implement measures to prepare higher risk patients for surgery. Pre-operative outpatient medical evaluation can decrease the length of hospital stay as well as minimize postponed or cancelled surgeries.1 To effectively provide this consultative service, the physician should understand the risk associated with the particular type of surgery planned and relate this risk to the patient's underlying acute and chronic medical problems. The complete consultation should include recommendations for evaluation and treatment, including prophylactic therapies to minimize the perioperative risk.
Surgical complications occur frequently. One large study2 documented at least one complication in 17 percent of surgical patients. Surgical morbidity and mortality generally fall into one of three categories: cardiac, respiratory and infectious complications (Table 1).2
TABLE 1 Frequency of Postoperative Complications
| Complication | Incidence (%) |
|---|---|
| Infection | 14.3 |
| Wound | 5.1 |
| Pneumonia | 3.6 |
| Urinary tract | 3.5 |
| Systemic sepsis | 2.1 |
| Respiratory | 9.5 |
| Pneumonia | 3.6 |
| Failure to wean from respirator in 48 hours | 3.2 |
| Unplanned intubation | 2.4 |
| Pulmonary embolus | 0.3 |
| Cardiac | 4.5 |
| Pulmonary edema | 2.3 |
| Cardiac arrest | 1.5 |
| Myocardial infarction | 0.7 |
Information from reference 2.
The overall risk for surgical complications depends on individual factors and the type of surgical procedure. For example, advanced age places a patient at increased risk for surgical morbidity and mortality.3,4 The reason for an age-related increase in surgical complications appears to correlate with an increased likelihood of underlying disease states in older persons, because studies have found that healthy elderly patients have surgical complication rates comparable to those of healthy younger patients.5,6 Diseases associated with an increased risk for surgical complications include respiratory and cardiac disease, malnutrition and diabetes mellitus.7 With respect to the type of surgery, urgent and emergency procedures constitute higher risk situations than elective, nonurgent surgery and present a limited opportunity for preoperative evaluation and treatment.
Preoperative History and Physical Examination
The patient should ideally be evaluated several weeks before the operation. The history should include information about the condition for which the surgery is planned, any past surgical procedures and the patient's experience with anesthesia. In children, the history should also include birth history, focusing on risk factors such as prematurity at birth, perinatal complications and congenital chromosomal or anatomic malformations, and history of recent infections, particularly upper respiratory infections or pneumonia.
The physician should inquire about any chronic medical conditions, particularly of the heart and lungs. Medications (including over-the-counter medications) should be noted. Drug dosages may need to be adjusted in the perioperative period. Aspirin and non-steroidal anti-inflammatory drugs should be discontinued one week before surgery to avoid excessive bleeding.
Immunization status can be documented, and vaccines can be updated if necessary. The patient should be asked about smoking history and alcohol and drug use. Ideally, the patient should quit smoking eight or more weeks before surgery to minimize the surgical risk associated with smoking.8
A functional assessment should be performed, and the physician should review the patient's social support and need for assistance after hospital discharge. For example, a patient who is scheduled for hip replacement surgery and has limited assistance available at home may require home services or temporary placement in a rehabilitation facility. Plans for such assistance can be made before hospitalization.
Table 2 summarizes the findings on the history and physical examination that suggest the need for further evaluation. Cardiopulmonary assessment may reveal key features that warrant preoperative intervention or further evaluation, including elevated blood pressure, heart murmurs, signs of congestive heart failure and pulmonary disease, most commonly obstructive pulmonary disease. Additionally, the physician should note any signs of malnutrition. In selected patients, a baseline mental status examination, using a standardized format, is required.
TABLE 2 Summary of Recommended Preoperative Laboratory Tests Depending on the History and Physical Findings
| Condition | Indicated testing and other measures* | |
|---|---|---|
| Healthy patient12 | ||
| ≤ 40 years | Hemoglobin, urine screening for pregnancy in women of childbearing potential | |
| > 40 years | Add ECG and blood glucose (age ≥ 45 years) | |
| Cardiovascular disease12,18 | ECG, chest radiographs, hemoglobin, electrolytes, BUN, creatinine, glucose (age ≥ 45 years or history of diabetes) | |
| Recent MI (≤6 weeks), unstable angina, decompensated CHF, significant arrhythmias, severe valvular disease | Cardiology consultation | |
| Previous MI (> 6 weeks ago), mild stable angina, compensated CHF, diabetes mellitus | Stress test if high-risk procedure or patient has low functional capacity; consider assessment of left ventricular function (i.e., echocardiography) | |
| Rhythm other than normal sinus rhythm, abnormal ECG, history of stroke, advanced age, low functional capacity | Stress test if high-risk procedure and patient has low functional capacity | |
| Pulmonary disease12,23,24,31–33 | Chest radiographs, hemoglobin, glucose (age ≥ 45 years), ECG (age > 40 years); provide patient with instructions for incentive spirometry or deep-breathing exercises | |
| Asthma | Pulmonary function testing or peak flow rate to assess disease status | |
| COPD | Consider pulmonary function testing and arterial blood gas analysis for assessment of disease severity | |
| Cough | Evaluate for etiology | |
| Dyspnea | Evaluate for etiology | |
| Smoking | Counsel patient to stop smoking 4 to 8 weeks before surgery | |
| Obesity | Provide patient with instructions for incentive spirometry or deep-breathing exercises | |
| Abdominal or thoracic surgery | Provide patient with instructions for incentive spirometry or deep-breathing exercises | |
| Malnutrition34–36,38–40 | Laboratory tests based on primary disease, plus albumin and lymphocyte count; if malnutrition is severe, consider postponing surgery and providing preoperative supplementation | |
ECG = electrocardiogram; BUN = blood urea nitrogen; MI = myocardial infarction; CHF = congestive heart failure; COPD = chronic obstructive pulmonary disease.
*—Other testing may be warranted based on the patient's surgical condition or other concomitant diseases.
Patients with cardiopulmonary disease may warrant a second examination just before hospitalization. In a child with an upper respiratory tract infection, a second visit to assess the current status of the infection can allow consultation with the surgeon regarding the need to postpone the procedure because of persistent fever, wheezing or significant nasal discharge.
At the time of the preoperative evaluation, the patient can be told, in general terms, what to expect during hospitalization and in the perioperative period. Patients who have pulmonary disease or who will undergo abdominal or thoracic surgery can be given instructions for performing incentive spirometry. The patient should also be provided with information about the expected postoperative course and possible complications. Inquiry regarding health care power of attorney and the patient's wishes regarding resuscitation if life-threatening complications arise can also be discussed.
Laboratory Assessment
Preoperative laboratory studies once routinely included a complete blood count, extensive blood chemistry profile, urinalysis, prothrombin time, partial thromboplastin time, electrocardiogram (ECG) and chest radiographs. Numerous studies have subsequently shown that most of these tests were ordered without a clear indication, and that only a very small percentage of the results were unexpectedly abnormal. Even among the small percentage of patients with unexpected abnormal results, management was unaffected.9–11 Current recommendations call for fewer routine tests and for selective ordering of laboratory tests based on the specific indications in a given patient.12,13 In addition, the availability of previous laboratory testing can obviate the need for additional preoperative tests.14
A hemoglobin measurement is useful in detecting unsuspected anemia and providing a baseline level, which can be helpful information postoperatively, particularly for surgeries with potential hemorrhagic complications. Renal and liver function studies are not routinely needed but may be indicated for patients who have a medical condition or medication use that would serve as indications for these tests.
Preoperative glucose determination should be obtained in patients 45 years or older, as there are currently recommendations to screen everyone more than 45 years of age for diabetes mellitus15 and the presence of diabetes increases perioperative risks.
A urine pregnancy test should be considered for women of childbearing age.
Coagulation times are not routinely indicated, as studies have shown that the yield is very low and that abnormal results are expected or do not significantly affect management.10 Coagulation studies would be indicated if the patient is receiving anticoagulant therapy, has a family or personal history that suggests a bleeding disorder or has evidence of liver disease.
An ECG is also not routinely indicated in patients 40 years or younger, but it should be obtained in patients older than 40 years or in patients with cardiac indications based on the past medical history.12
Chest radiographs should be obtained on the basis of findings from the medical history or physical examination.
Cardiac Evaluation
With the increasing size of the middle-aged and elderly population, more surgical procedures will be performed in patients who have or potentially have coronary artery disease. Cardiovascular disease affects 25 percent of the U.S. population, and cardiovascular disease is the leading cause of death in the United States, with more than 60 percent of cardiovascular-related deaths due to coronary artery disease.4 Cardiac complications are the most common type of complication that can threaten the surgical patient's life or prolong the patient's hospital stay.
RISK FACTOR ASSESSMENT
Risk factors for cardiac complications have been long recognized. Goldman's cardiac risk index16 was one of the first attempts to systematically evaluate a patient's risk of cardiac complications with surgery. This index compiled the risk factors into a point scale that correlated with a patient's risk for perioperative cardiac morbidity and mortality. Subsequent validation studies have shown, however, that some surgical procedures carry minimal risk while others carry excessive risk for which this index does not account, decreasing its correlation with actual outcomes.17
The American College of Cardiology (ACC) and the American Heart Association (AHA) recommendations for the assessment of cardiac risk in patients undergoing noncardiac surgery18 incorporate many of Goldman's risk factors but expand the assessment to include the risk associated with the particular surgical procedure (Table 3), as well as additional patient characteristics that influence perioperative cardiac risk (Table 4). Figure 1 depicts a scheme for preoperative cardiac evaluation based on the level of risk as determined by the features described in Table 4.
TABLE 3 Surgery-Related Predictors for Risk of Perioperative Cardiac Complications
| High risk |
| Emergency surgery |
| Anticipated increased blood loss |
| Aortic or peripheral vascular surgery |
| Intermediate risk |
| Abdominal or thoracic surgery |
| Head and neck surgery |
| Carotid endarterectomy |
| Orthopedic surgery |
| Prostate surgery |
| Low risk |
| Breast surgery |
| Cataract surgery |
| Superficial surgery |
| Endoscopy |
Information from reference 11.
TABLE 4 Patient-Related Predictors for Risk of Perioperative Cardiac Complications
| Major clinical predictors |
| Myocardial infarction ≤6 weeks previously |
| Unstable angina |
| Decompensated congestive heart failure |
| Significant arrhythmias (e.g., causing hemodynamic instability) |
| Severe valvular disease (e.g., aortic or mitral stenosis with valve area < 1.0 cm2) |
| Intermediate clinical predictors |
| Mild angina pectoris |
| Myocardial infarction > 6 weeks previously |
| Compensated congestive heart failure |
| Diabetes mellitus |
| Minor clinical predictors |
| Advanced age |
| Abnormal electrocardiogram |
| Cardiac rhythm other than sinus |
| Low functional capacity, history of stroke, uncontrolled hypertension |
Information from reference 11.
FIGURE 1. Preoperative Cardiac Testing
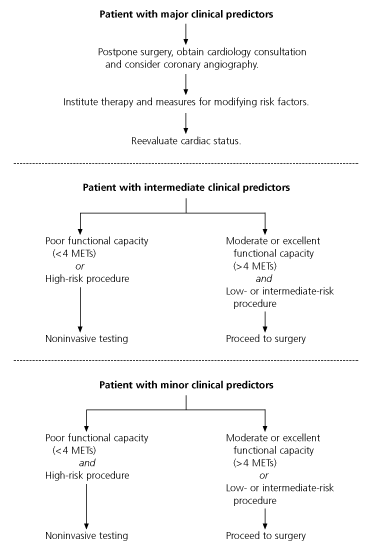
Schematic for determining the need for preoperative cardiac testing on the basis of the patient's clinical predictors and functional status and the risk of the operative procedure. (METs = metabolic equivalents of oxygen consumption)
Adapted with permission from the American College of Cardiology and the American Heart Association. Guidelines for perioperative cardiovascular evaluation for noncardiac surgery. Circulation 1996;93:1280–1317.
The starting point in assessing a patient's cardiac risk often involves a previous history of diagnosed coronary artery disease, any previous cardiovascular procedural interventions or testing, current therapies and any current symptoms suggestive of angina or congestive heart failure. Patients in whom cardiac stress testing was normal within the past two years or who have had coronary bypass surgery within the past five years, and are without symptoms, require no further assessment.18 Similarly, clinically stable patients who have undergone angioplasty between six months and five years previously require no further assessment. In contrast, patients who have had angioplasty within the previous six months may require cardiac reevaluation and/or consultation with a cardiologist before surgery.
Emergency surgery calls for expedited pre-operative cardiac assessment and management. Patients undergoing elective or semi-elective procedures can proceed with preoperative cardiac testing, as outlined in Figure 1. Patients at high risk for complications usually warrant cardiology consultation and possibly angiography. Cardiac stress testing should be performed in patients at intermediate risk and with poor functional capacity (Table 5)19 or who are undergoing high-risk procedures, such as vascular surgery. For patients with minor clinical predictors, only patients who have poor functional capacity and are undergoing a high-risk procedure require stress testing. Patients with positive stress test results warrant cardiology consultation before proceeding with surgery.
TABLE 5 Examples of a Functional Capacity of More Than 4 METs
| Climbing one flight of stairs |
| Mowing the lawn |
| Gardening |
| Golfing without a cart |
| Doubles tennis |
| Swimming |
| Riding a bike |
| Square dancing |
| Jogging |
METs = metabolic equivalents of oxygen consumption. Information from reference 19.
Although cardiac arrhythmias have historically been correlated with increased perioperative risk and are specifically cited in several risk assessment tools, recent data suggest that arrhythmias are not usually the proximate cause of a perioperative complication.20 Rather they serve as markers for possible underlying cardiopulmonary disease and should prompt an evaluation for the cause of the arrhythmia.
ASSESSMENT OF LEFT VENTRICULAR FUNCTION
Assessment of left ventricular function is not routinely indicated for preoperative evaluation whether or not the patient has cardiac disease. If decreased left ventricular function is suspected on the basis of the clinical examination or radiographic evidence of cardiac enlargement, radionuclide imaging or echocardiography may help define left ventricular function and may suggest the need for further evaluation or therapeutic changes. On the other hand, the preoperative assessment guideline from the American College of Physicians18 notes that radionuclide or echocardiographic assessment of left ventricular function does not appear to improve the risk prediction provided by the clinical examination alone.
ASSESSING THE NEED FOR CARDIAC INTERVENTIONS
In summary, recommendations do not call for preoperative cardiac testing in all patients. The need for further cardiac evaluation before surgery is determined by the clinical risk predictors identified from the patient's history, physical examination, ECG and functional status, along with the risk associated with the operation itself. Cardiac interventions are recommended only for patients who would benefit regardless of any planned non-cardiac surgery.18
It should also be emphasized that almost half of perioperative cardiac complications are due to postoperative ischemia or congestive heart failure.21 The incidence of postoperative complications is the highest in the first 48 hours after surgery, and ischemia is clinically silent in up to 90 percent of cases.22 While pre-operative risk assessment and interventions are important, attention to possible complications in the postoperative period is also crucial.
Pulmonary Assessment
The major pulmonary complications in the perioperative period are atelectasis, pneumonia and bronchitis. Predisposing risk factors include cough, dyspnea, smoking, a history of lung disease, obesity and abdominal or thoracic surgery (Table 6).23,24 The most significant of these risk factors is the site of surgery, with abdominal and thoracic surgery having pulmonary complication rates ranging from 30 to 40 percent.24 As a rule, the closer the surgery is to the diaphragm, the higher the risk of pulmonary complications.
TABLE 6 Indicators of Increased Surgical Risk for Pulmonary Complications
| Cough |
| Dyspnea |
| Pulmonary disease |
| Smoking |
| Obesity |
| Abdominal or thoracic surgery |
| FEV1 < 2 L |
| MV V < 50 percent of predicted value |
| PEF < 100 L or 50 percent of predicted value |
| Pco2 ≥ 45 mm Hg |
| Po2 ≤ 50 mm Hg |
FEV1= forced expiratory volume in one second; MV V = maximum voluntary ventilation; PEF = peak expiratory flow rate; Pco2= partial pressure of carbon dioxide; Po2= partial pressure of oxygen.
Baseline chest radiographs may be helpful in at-risk patients.24 Guidelines for ordering pulmonary function tests have been published.25,26 Although the results of pulmonary function testing have not been shown to be predictive of postoperative complications, 40 percent of preoperative pulmonary function tests are ordered without an indication as outlined in the guidelines.27
Pulmonary function testing may be helpful in diagnosing and assessing disease severity. Preoperative guidelines do not define the degree of pulmonary function impairment that would prohibit surgery other than that for lung resection.23,24 With lung resection surgery, patients with a forced expiratory volume in one second (FEV1) of less than 2 L require preoperative ventilation/perfusion studies to determine the predicted postoperative FEV1. An estimated postoperative FEV1 of 800 mL or more is required before lung resection is performed.
PRECAUTIONARY MEASURES FOR AT-RISK PATIENTS
Patients with cough or dyspnea should be evaluated to identify the underlying cause of the symptoms.
Patients who smoke cigarettes should be advised to quit smoking for eight weeks before surgery. This interval will allow the mucociliary transport mechanism to recover, the secretions to decrease and the carbon monoxide levels in the blood to drop.8 Reduction or cessation of smoking for less than four to eight weeks before surgery is of questionable benefit, and has actually been shown in some studies to result in higher complication rates.8,28 Asthma should be under control before surgery, if possible. Steroid therapy for asthma can be continued throughout the perioperative period without excess surgical morbidity.29,30 Patients with asthma or chronic obstructive pulmonary disease can be given pre- and postoperative bronchodilators to increase pulmonary function.
Any pulmonary infection should be treated preoperatively. Pulmonary complications may be prevented by providing patients with instructions on how to perform incentive spirometry and deep-breathing exercises. Deep-breathing exercises and incentive spirometry in the postoperative period may be particularly beneficial in obese patients, in patients with lung disease and in patients undergoing abdominal or thoracic procedures.31–33
Nutritional Assessment
Malnourished patients experience increased surgical morbidity and mortality.34 A preoperative history and physical examination should include an assessment of risk factors for malnutrition, especially in the elderly. Social isolation, limited financial resources, poor dentition, weight loss and chronic disorders such as pulmonary disease, congestive heart failure, depression, diarrhea and constipation are commonly associated with malnutrition. In addition, patients often cannot eat for varying periods before and after surgery, further compromising nutritional status.
The most optimal means of defining a patient's nutritional status has not been established.35 However, if there are nutritional concerns, additional factors can be considered. A weight loss of more than 5 percent in one month or of 10 percent or more over six months, a serum albumin of less than 3.2 g per dL (32 g per L), and a total lymphocyte count of less than 3,000 per μL3 (3.0 × 109 per L) can signify an increased risk of postoperative complications.35,36
Preoperative nutritional supplementation can be provided orally, with enteral tube feeding or with parenteral nutrition. Enteral tube feeding is widely underused, much less expensive than parenteral nutrition and may carry less risk for electrolyte abnormalities and infection.37 Although criteria for the administration of perioperative parenteral nutritional supplementation are not well established, general recommendations are summarized in Table 7.38 The exact duration of supplementation needed is uncertain, but it has been suggested that a minimum of seven to 15 days of oral or intravenous supplementation is required to provide benefit in patients who are malnourished.39,40
TABLE 7 Indicators for Perioperative Nutritional Supplementation
| Preoperative supplementation |
| Severely malnourished patients |
| Patients who have been NPO for three to five days preoperatively |
| Postoperative supplementation |
| Severely malnourished patients during any duration of NPO |
| Malnourished or critically ill patients who have been NPO for five days or more |
| Well-nourished patients who have been NPO for five to 10 days postoperatively |
NPO = no oral intake.
Information from reference 38.
Future Research
Further research will help physicians discern which testing and management interventions have evidence-based proof of their utility. One area of more recent interest is the use of perioperative beta-blocker therapy in patients with coronary artery disease or its risk factors. Initial studies have shown a decrease in perioperative cardiac mortality, with few side effects.41 Revisions in current guidelines are inevitable and may include a recommendation for beta blockers in patients with coronary artery disease.

