A 36-year-old woman with no significant medical history presented with an asymptomatic eruption on her left arm. She noted that the first lesion appeared about a week after her cat had scratched her left arm. Over the next several weeks, more lesions developed proximally (Figure 1).
FIGURE 1.
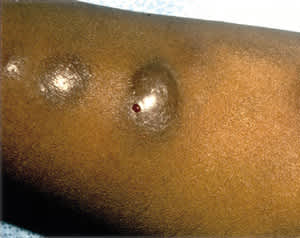
Linear array of nodules on a patient's arm. Largest lesion shows blood clot on site of punch biopsy.
Question
Given the patient's history and skin examination, which one of the following is the best diagnosis?
A. Cat-scratch disease.
B. Mycobacterium marinum infection.
C. Sporotrichosis.
D. Tinea corporis.
E. Toxoplasmosis.
Discussion
The answer is C: sporotrichosis. Sporotrichosis is a fungal infection caused by Sporothrix schenckii, a fungus that is commonly found on decaying vegetation and in the soil. The fungus is found worldwide but is more prevalent in temperate and tropical climates. Infection of human or animal hosts (particularly cats) is often the result of traumatic inoculation of the fungus from thorns, barbs, splinters, moss or hay contaminated with S. schenckii. Moreover, as demonstrated by this case, an infected animal can transmit the fungus to humans. Rarely, direct inhalation into the lungs may be the mode of acquisition.
The differential diagnosis includes other granulomatous diseases or diseases with lymphangitic spread, including atypical mycobacterioses (i.e., Mycobacterium marinum infection), cat-scratch disease and toxoplasmosis.
M. marinum infection (fish tank granuloma) may closely resemble lymphangitic sporotrichosis. Acid-fast bacilli should be seen in the skin biopsy specimen.
Although cat-scratch disease is also associated with cats, it presents with regional lymphadenopathy rather than the linear pattern of skin nodules seen in sporotrichosis.
Toxoplasmosis is associated with the handling of cat feces, but skin lesions are uncommon and do not usually show a linear distribution.
Although tinea corporis is also caused by a fungus, its typical lesion is an annular scaly plaque.
Lymphocutaneous infection is the classic presentation of sporotrichosis (up to 80 percent of cases)1 and is the one presented here. It usually involves the dominant upper extremity and begins as an infective granuloma at the site of inoculation. This painless, indurated nodule may break down into a small ulcer (sporotrichotic chancre) followed by the development of erythematous nodules along the line of lymphatic drainage, leading to the characteristic linear pattern. Regional adenopathy may follow as well.
The diagnosis of sporotrichosis will often be suggested by the clinical presentation and history, because the primary chancre with its associated chain of adenopathy is pathognomonic. Histologic examination of a skin biopsy shows a granulomatous reaction with some foci of necrosis.
Sporothrix is dimorphic. In tissue, the yeast form is cigar-shaped with single, and occasional multiple, buds. These small bodies can be surrounded by a thick eosinophilic substance and are known as the distinctive asteroid bodies. In culture, the fungus is in its hyphal form, as shown in Figure 2. The patient's culture showed multiple conidia on conidiophores.
FIGURE 2.
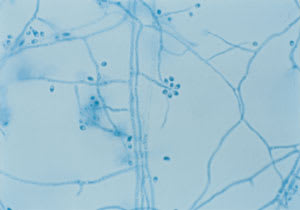
Sporothrix schenckii at room temperature.
Treatment of cutaneous lesions typically involves treatment with up to 16 weeks of oral itraconazole, 200 mg per day.2

