A 72-year-old Guyanese man who had lived in New York City for six years presented with a history of weakness, dizziness, decreased appetite and weight loss of 10 to 15 lb in two weeks. The patient had an unremarkable past medical history, was afebrile on admission and denied any abdominal symptoms. On the second day of hospitalization he developed a fever up to 39.4°C (103.0°F) with chills and rigor. Physical examination was remarkable only for submandibular and inguinal lymphadenopathy. Rectal examination was negative for fecal occult blood. The patient's human immunodeficiency virus (HIV) status was unknown.
Laboratory results showed decreased levels of hemoglobin (7 g per dL [70 g per L]), serum iron (6 μg per dL [2 μmol per L]) and albumin level (2.3 g per dL [23 g per L]). Diffuse bilateral reticulonodular infiltration was apparent on chest radiography. A computed tomographic (CT) scan of the chest showed a 2 × 2 cm nodule at the thoracic inlet with retroperitoneal and paraaortic lymphadenopathy. Abdominal ultrasonography showed periportal lymphadenopathy. A CT scan of the abdomen and pelvis showed diffuse lymphadenopathy with a normal liver, pancreas and spleen. Colonoscopic examination showed malignant-appearing ulcers at the junction of the cecum and ascending colon (Figures 1, 2 and 3) and a large lesion in the descending colon (Figure 4).
FIGURE 1
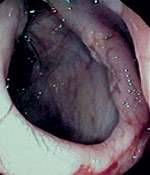
FIGURE 2
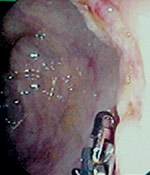
FIGURE 3
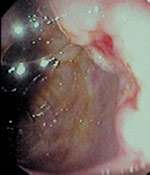
FIGURE 4
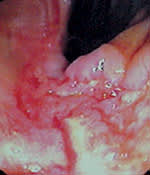
Question
Given the patient's history, laboratory results, imaging studies and colonoscopic findings, which one of the following conditions is represented by the figures above?
- A. Colon cancer.
- B. Tuberculosis of the colon.
- C. Ulcerative colitis.
- D. Crohn's disease.
- E. Colonic histoplasmosis.
Discussion
The answer is E: colonic histoplasmosis. Colonic histoplasmosis was confirmed by biopsy of the colon. This patient had disseminated histoplasmosis and later tested positive for HIV with a CD4 count of less than 20 and a viral load of 240,000 copies per mL.
Colon cancer can present with large ulcerated lesions such as those seen here in the descending colon, but few cases would present with multiple synchronous lesions like those present in this patient.
The diffuse nodular densities seen on chest radiograph, generalized lymphadenopathy and colonic lesions could be consistent with miliary (or disseminated) tuberculosis, and appropriate isolation of the patient would be prudent until results from acid fast bacillus smears and culture of infected tissues were available.
Ulcerative colitis would not present with scattered lesions in the colon, but Crohn's disease can lead to multiple “skip” lesions in different sites. Transmural inflammation and granuloma formation are the classic findings on biopsy of Crohn's lesions.
Disseminated histoplasmosis occurs in 2 to 5 percent of patients with acquired immunodeficiency syndrome (AIDS).1 With the advent of better medications against HIV virus, patients are surviving longer, and more cases of histoplasmosis are being reported. Histoplasmosis has been an AIDS-defining illness since 1987.1
The causative organism, Histoplasma capsulatum, is a fungus that grows both as mycelium in the soil and as a yeast from within infected cells. It is the most common fungus in the United States and is endemic in the Mississippi and Ohio river valleys. In the United States, the incidence of infection is highest in hyperendemic areas and among those who work in the poultry industry.
Disseminated histoplasmosis is seen almost exclusively in patients with AIDS whose CD4 counts are 75 per mL or less. Patients usually present with nonspecific symptoms such as weight loss, fatigue and fever lasting for one to three months. Respiratory symptoms occur in 50 percent, lymphadenopathy in 20 percent and gastrointestinal symptoms (abdominal pain, bleeding, diarrhea and obstruction) in 10 percent.2 The part of the gastrointestinal system most commonly involved is the ileum.3 The gold standard for diagnosis is culture of H. capsulatum from blood or other appropriate body fluid. Histologic evaluation of infected tissue is the most rapid diagnostic technique, but can be falsely negative in many cases. Diffuse nodular or linear densities in the chest radiographs of AIDS patients with a history of residence in endemic areas suggests the possibility of disseminated histoplasmosis.
Disseminated histoplasmosis is usually fatal if not diagnosed early and treated rapidly.4 The recommended treatment is intravenous amphotericin B as induction therapy with a total dose of 1 to 2 g. Relapse is common after successful remission. Lifelong suppressive therapy with itraconazole is recommended.


