Despite exhaustive efforts to better manage patients with type 2 diabetes mellitus (formerly known as non-insulin-dependent diabetes mellitus), attempts at maintaining near normal blood glucose levels in these patients remains unsatisfactory. This continues to pose a real challenge to physicians as the prevalence of this disease in the United States continues to rise. Type 2 diabetes is defined as a syndrome characterized by insulin deficiency, insulin resistance and increased hepatic glucose output. Medications used to treat type 2 diabetes are designed to correct one or more of these metabolic abnormalities. Currently, there are five distinct classes of hypoglycemic agents available, each class displaying unique pharmacologic properties. These classes are the sulfonylureas, meglitinides, biguanides, thiazolidinediones and alpha-glucosidase inhibitors. In patients for whom diet and exercise do not provide adequate glucose control, therapy with a single oral agent can be tried. When choosing an agent, it is prudent to consider both patient- and drug-specific characteristics. If adequate blood glucose control is not attained using a single oral agent, a combination of agents with different mechanisms of action may have additive therapeutic effects and result in better glycemic control.
The prevalence of type 2 diabetes mellitus (formerly known as non-insulin-dependent diabetes mellitus) in the United States has increased dramatically over the past two decades and continues to rise.1Despite the introduction of new agents to the armamentarium of hypoglycemic agents, efforts for better management of this disease have been disappointing and the control of blood glucose levels remains unsatisfactory.2Recently, the results of the United Kingdom Prospective Diabetes Study (UKPDS) were released.3This study, the largest and longest study of patients with type 2 diabetes, has reinforced the belief that improved control of blood glucose levels can substantially lower the overall morbidity associated with this disease, underscoring the urgency to obtain better glucose control in these patients. The focus of this review will be the management of patients with type 2 diabetes using one or more of the five available classes of oral hypoglycemic agents: sulfonylureas, meglitinides, biguanides, thiazolidinediones and alphaglucosidase inhibitors (Table 1). Options for monotherapy and combination therapy, efficacy of specific agents, adverse effects and special populations are some issues addressed in this review.
TABLE 1 Classes of Oral Hypoglycemic Agents
| Drug class | Agent | |
|---|---|---|
| Sulfonylureas | First generation | |
| Acetohexamide (Dymelor) | ||
| Chlorpropamide (Diabinese) | ||
| Tolazamide (Tolinase) | ||
| Tolbutamide (Orinase) | ||
| Second generation | ||
| Glyburide (Micronase) | ||
| Glipizide (Glucotrol) | ||
| Glimepiride (Amaryl) | ||
| Meglitinides | Repaglinide (Prandin) | |
| Nateglinide (Starlix) | ||
| Biguanides | Metformin (Glucophage) | |
| Thiazolidinediones | Pioglitazone (Actos) | |
| Rosiglitazone (Avandia) | ||
| Alpha-glucosidase inhibitors | Acarbose (Precose) | |
| Miglitol (Glycet) | ||
Type 2 diabetes can be described as a syndrome characterized by insulin deficiency, insulin resistance and increased hepatic glucose output.4,5With this in mind, therapies used to treat patients with this disease are aimed at correcting one or more of these physiologic abnormalities. Current recommendations of the American Diabetes Association include a trial of diet and exercise as first-line therapy for the treatment of patients with type 2 diabetes.6If the desired level of glycemic control is not achieved with diet and exercise within a three-month period, pharmacologic intervention is required.
Criteria for initiation of therapy with an oral agent versus insulin are debated among diabetologists, but the decision should be made jointly by the physician and patient to obtain the best results.7(Because of the apparently progressive nature of the beta cell defect in type 2 diabetes, current oral therapies may not prevent an eventual decline in glycemic control, and it is likely that many patients will ultimately require insulin therapy.) Once the decision is made to initiate therapy with an oral agent, it is prudent to consider patient-specific (age, weight, level of glycemic control) and agent-specific characteristics (relative potencies, duration of action, side-effect profiles, cost) to make the most appropriate choice (Tables 2 and 38). Figure 1 illustrates a reasonable stepwise approach for initiating oral therapy in patients with type 2 diabetes and is consistent with the recommendations put forth by several expert committees and diabetes subspecialists.4–6,9
TABLE 2 Clinical Efficacy of Oral Hypoglycemic Agents
| Class of hypoglycemic agents | Reduction in HbA1c(%) | Reduction in FPG (mg per dL [mmol per L]) |
|---|---|---|
| Sulfonylureas | 0.8 to 2.0 | 60 to 70 [3.3 to 3.9] |
| Meglitinides | 0.5 to 2.0 | 65 to 75 [3.6 to 4.2] |
| Biguanides | 1.5 to 2.0 | 50 to 70 [2.8 to 3.9] |
| Thiazolidinediones | 0.5 to 1.5 | 25 to 50 [1.4 to 2.8] |
| Alpha-glucosidase inhibitors | 0.7 to 1.0 | 35 to 40 [1.9 to 2.2] |
HbA1c= glycosylated hemoglobin A1c; FPG = fasting plasma glucose.
TABLE 3 Average Dose and Cost Comparison of Hypoglycemic Agents
| Drug class | Brand name | Generic | Available strengths | Brand name dose range (mg/day) and cost*† | Generic name dose range (mg/day) and cost*† |
|---|---|---|---|---|---|
| Sulfonylureas | DiaBeta | Glyburide | 1.25, 2.5, 5.0 | 5 ($21.24) to 20 ($84.96) | 5 ($16.06 to 20.40) to 20 ($64.26 to $81.73) |
| Micronase | Glyburide | 1.25, 2.5, 5.0 | 5 ($26.49) to 20 ($105.96) | 5 ($16.06 to 20.40) to 20 ($64.26 to $81.73) | |
| Glynase | Glyburide (micronized) | 1.5, 3.0, 4.5, 6.0 | 0.75 ($13.73) to 12 ($73.18) | 1.5 ($8.86 to 11.33) to 12 ($50.45 to $60.96) | |
| Glucotrol | Glipizide | 5.0, 10 | 10 ($24.63) to 40 ($90.46) | 10 ($18.21 to 20.82) to 40 ($66.84 to $76.62) | |
| Glucotrol XL | Glipizide | 5.0, 10 | 5 ($10.65) to 20 ($42.17) | ‡ | |
| Amaryl | Glimepiride | 1.0, 2.0, 4.0 | 1 ($7.34) to 8 ($44.86) | ‡ | |
| Meglitinides | Prandin | Repaglinide | 0.5, 1.0, 2.0 | 1.5 ($51.61) to 16 ($199.20) | ‡ |
| Starlix | Nateglinide | 60, 120 | 180 ($83.00) to 360 ($86.50) | ||
| Biguanides | Glucophage | Metformin | 500, 850, 1,000 | 1,500 ($58.16) to 2,550 ($98.87) | ‡ |
| Glucophage XR | Metformin | 500 | 1,000 ($39.24) to 2,000 ($74.48) | ‡ | |
| Thiazolidinedione | Actos | Pioglitazone | 15, 30, 45 | 15 ($85.50) to 45 ($148.50) | ‡ |
| Avandia | Rosiglitazone | 2.0, 4.0, 8.0 | 4 ($75.00) to 8 ($136.90) | ‡ | |
| Alpha-glucosidase inhibitor | Precose | Acarbose 100 | 25, 50, to 300 ($60.01) | 150 ($46.54) ‡ | |
| Glyset | Miglitol | 25, 50, 100 | 150 ($51.75) to 300 ($59.26) | ‡ | |
| Combination | Glucovance | Glyburide/Metformin | 1.25/250 2.5/500 5.0/500 | 2.5/500 ($23.50) to 20/2,000 ($94.00) | ‡ |
*—Estimated cost to the pharmacist based on average wholesale prices in Red book, Montvale, NJ; Medical Economics Data, 2000. Cost to the patient will be higher based on prescription filling fee.
†— Prices are for a 30-day supply.
‡—Generic formulation not available.
Information from Luna B, Hughes AT, Feinglos MN. The use of insulin secretagogues in the treatment of type 2 diabetes. Prim Care 1999;26:895–915.
FIGURE 1. Management of Type 2 Diabetes
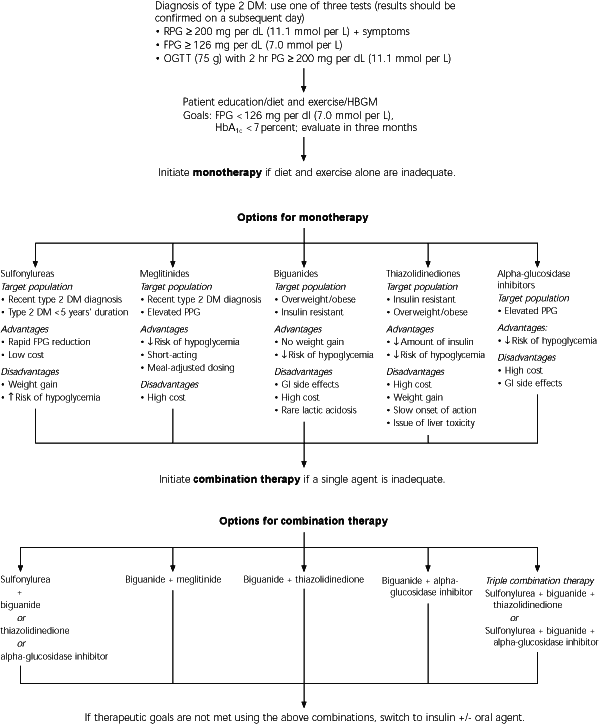
Stepwise approach for the management of type 2 diabetes in patients inadequately controlled with diet and exercise. (RPG = random plasma glucose; FPG = fasting plasma glucose; OGTT = oral glucose tolerance test; PG = plasma glucose; HbA1c = glycosylated hemoglobin A1c; HBGM = home blood glucose monitoring; DM = diabetes mellitus; GI = gastrointestinal; PPG = postprandial glucose)
Sulfonylureas
Sulfonylureas have remained the mainstay of antidiabetic therapy since the early 1950s. Following the release of the University Group Diabetes Program (UGDP) study,10which implicated tolbutamide in increased mortality secondary to cardiovascular events, the use of the first generation sulfonylureas (acetohexamide, chlorpropamide, tolbutamide and tolazamide) quickly fell out of favor.11Recent data, as summarized in an earlier review, supporting the benefits of the sulfonylureas as well as the availability of newer generation sulfonylureas with more favorable side-effect profiles (glyburide [Micronase], glipizide [Glucotrol] and glimepiride [Amaryl]), have contributed to their renewed popularity.3,8
Sulfonylureas work by stimulating insulin release from the beta cells of the pancreas and may slightly improve insulin resistance in peripheral target tissues (muscle, fat). On average, this class reduces glycosylated hemoglobin A1c(HbA1c) levels by 0.8 to 2.0 percent and fasting plasma glucose (FPG) concentrations by 60 to 70 mg per dL (3.3 to 3.9 mmol per L), with the greatest reductions observed in patients with the highest FPG concentrations at the initiation of therapy.4,5,8Hypoglycemia is the most worrisome side effect of the sulfonylureas. It is of particular concern with agents that are metabolized to an active metabolite with significant renal excretion. These agents include chlorpropamide (Diabinese) and glyburide, both of which should be avoided in the setting of impaired renal function and used with caution in elderly patients. Glipizide and glimepiride are associated with a lower incidence of hypoglycemia. All sulfonylureas have been associated with weight gain and thus, may not be the optimal first choice for obese patients.
Unfortunately, not all patients treated with a sulfonylurea will have an adequate response. Treatment failure with sulfonylurea therapy can be divided into two categories: primary and secondary. Primary failure results when a patient exhibits an initial poor response to sulfonylurea therapy (a decrease in FPG levels of less than 20 mg per dL [1.1 mmol per L]). Approximately 20 to 25 percent of patients with type 2 diabetes will demonstrate primary failure to sulfonylurea therapy.12Secondary failure results when the patient responds well to treatment initially (a decrease in FPG of greater than 30 mg per dL [1.7 mmol per L]), but eventually the treatment fails to maintain adequate control. This phenomenon is reported to occur in approximately 5 to 10 percent of patients per year.12Despite these drawbacks, sulfonylureas have been shown to be potent and cost-effective glucose-lowering agents.
When initiating sulfonylurea therapy, the lowest effective dose should be used and titrated to the desired effect at one- to two-week intervals. Most of the hypoglycemic effects of the sulfonylureas will be observed at one half of the maximum dose recommended for a specific agent. In patients who are not responding at one half the maximum dose, an alternative agent or combination therapy should be considered.
Meglitinides
Repaglinide (Prandin) is a new non-sulfonylurea insulin secretagogue agent, the first available from the meglitinide class. Nateglinide (Starlix), the newest member of the class, has recently become available. The mechanism of action of the meglitinides closely resembles that of the sulfonylureas. The meglitinides stimulate the release of insulin from the pancreatic beta cells. However, this action is mediated through a different binding site on the “sulfonylurea receptor” of the beta cell, and the drug has somewhat different characteristics when compared with the sulfonylureas. Unlike the commonly used sulfonylureas, the meglitinides have a very short onset of action and a short half-life. Repaglinide has shown similar effects on HbA1cand FPG levels when compared with glyburide, 0.5 to 2 percent and 65 to 75 mg per dL (3.6 to 4.2 mmol per L), respectively.8Some potential advantages of this class of agents include a greater decrease in postprandial glucose and a decreased risk of hypoglycemia.
Because of the short onset of action of the meglitinides (15 to 30 minutes), patients should be instructed to administer a dose immediately before a meal. If a meal is omitted throughout the day, patients should be instructed to skip the corresponding dose to prevent hypoglycemia. Likewise, if an extra meal is added throughout the day, the patient should add a dose to cover that meal. Repaglinide can be titrated to a dosage of 4 mg before each meal (maximum dosage of 16 mg per day). Nateglinide can be titrated to a dosage of 120 mg before each meal. At least one week should be allowed between dosage adjustments to adequately assess blood glucose response. This unique dosing regimen may allow greater flexibility for patients who have difficulty maintaining a regular meal schedule.
Biguanides
Although biguanides have been in use for many years outside the United States, their reintroduction in this country has been relatively recent. Metformin (Glucophage) is currently the only agent in this antidiabetic class available in this country. Metformin works by reducing hepatic glucose output and, to a lesser extent, enhancing insulin sensitivity in hepatic and peripheral tissues. Metformin has been shown to reduce HbA1clevels by approximately 1.5 to 2.0 percent and FPG levels by 50 to 70 mg per dL (2.8 to 3.9 mmol per L).4,5,13Other effects include a reduction in plasma triglyceride levels and low-density lipoprotein (LDL) cholesterol levels.
On the whole, metformin has a favorable side effect profile. Most of the related side effects (including metallic taste, gastrointestinal discomfort and nausea) are transient and commonly reported only during initiation of therapy. Slow-dosage titration is recommended to lessen these effects. Taking the drug with meals may also lessen the severity of the gastrointestinal side effects. Because metformin does not affect insulin secretion, it is not associated with hypoglycemia when used as monotherapy, but can potentiate hypoglycemia when used in combination with a sulfonylurea or insulin. A rare, but more worrisome potential adverse effect is that of lactic acidosis. As opposed to phenformin, which was withdrawn from the U.S. market during the 1970s, this event is almost unknown with metformin in the absence of other underlying diseases, particularly renal insufficiency. The reported frequency of lactic acidosis in all patients is three cases per 100,000 patient-years.14
Metformin should not be used in patients with elevated serum creatinine levels, specifically, 1.4 mg per dL (120 μmol per L) or more in women and 1.5 mg per dL (130 μmol per L) or more in men. In patients undergoing contrast studies, metformin therapy should be withheld for approximately 48 hours following the procedure or until it has been determined that renal function has returned to baseline. Other situations in which metformin therapy should be avoided include cardiogenic or septic shock, congestive heart failure that requires pharmacologic therapy, severe liver disease, pulmonary insufficiency with hypoxemia or severe tissue hypoperfusion.13–15
Metformin is unusual among the oral antidiabetic drugs in that therapy has been associated with a lack of weight gain and even weight loss in some overweight patients.16–18Although these observed effects make it an ideal first-line agent in overweight patients, results from studies have shown that metformin also improves glycemic control in patients who are not overweight.16–18Recent reports from the UKPDS group indicate that metformin used as monotherapy in obese patients may significantly reduce the risk of macrovascular complications, although the validity of this finding has been questioned.19
Metformin therapy should be initiated at 500 mg twice daily with meals and can be increased by 500 mg (maximum dosage of 2,000 mg daily) at two-week intervals to minimize gastrointestinal side effects. A new extended release formulation of metformin was recently introduced to the market (Glucophage XR), allowing a more convenient once-daily dosing regimen.
Thiazolidinediones
Until recently, the agents in this drug class approved by the U.S. Food and Drug Administration (FDA) included troglitazone (Rezulin), rosiglitazone (Avandia) and pioglitazone (Actos). Subsequently, in March 2000, the FDA asked the manufacturer (Parke-Davis, Warner-Lambert) of troglitazone, the first agent in this class to receive labeling approval, to remove the product from the market. This request occurred following more than 60 reports of severe liver toxicity in patients taking this agent.
A majority of the data reporting the efficacy of this class comes from studies with troglitazone, although results from more recent studies with the newer agents (rosiglitazone and pioglitazone) demonstrate similar properties.20–23The thiazolidinediones work by enhancing insulin sensitivity in both muscle and adipose tissue and to a lesser extent by inhibiting hepatic glucose production. These agents have a notable effect on improving insulin resistance, particularly when used in combination with other antidiabetic drugs, but have no effect on insulin secretion.
Monotherapy with these agents has been associated with a 0.5 to 1.5 percent reduction in HbA1clevels and 25 to 50 mg per dL (1.4 to 2.8 mmol per L) reduction in FPG levels.4,5As a class, the thiazolidinediones have also been shown to alter lipid profiles in patients with type 2 diabetes. Results from studies with troglitazone consistently show a decrease in triglyceride levels—in some cases by as much as 33 percent.24,25The effects on high density lipoprotein (HDL) cholesterol levels have been either favorable or neutral, while some studies report an increase in total and LDL cholesterol levels.24,25Newer data reveal that as monotherapy, rosiglitazone is associated with increases in total, LDL and HDL cholesterol levels and either no change or increases in triglyceride levels. Patients treated with pioglitazone have displayed mean decreases in triglyceride levels, mean increases in HDL cholesterol levels, and no consistent mean changes in LDL and total cholesterol levels.20,21
Because these agents do not increase insulin secretion, hypoglycemia does not pose a risk when thiazolidinediones are taken as monotherapy. Significant weight gain has been reported with all three agents. The thiazolidinediones are relatively safe in patients with impaired renal function because they are highly metabolized by the liver and excreted in the feces; however, caution should be used in patients with hepatic dysfunction because troglitazone and its metabolites have been shown to accumulate in this setting.
The manufacturers recommend that these agents not be prescribed for patients with serum transaminase levels that exceed 2.5 times the upper limit of normal. Mild to moderate edema has been reported in 5 to 7 percent of patients treated with rosiglitazone and pioglitazone.20,21The increase in plasma volume is of concern in patients with congestive heart failure—particularly those with New York Heart Association class III or IV functional status. The use of thiazolidinediones should be avoided in these patients.
As referred to earlier, of greatest concern are the reports of an idiosyncratic drug reaction with troglitazone. This reaction is initially characterized by increased serum transaminase levels, which in some cases progressed to hepatitis, hepatic failure and death. Preliminary attempts (before troglitazone was withdrawn from the market in March 2000) to prevent such incidents included a request by the FDA that Parke-Davis strengthen the drug's labeling and require stringent monitoring of transaminase levels in patients taking this agent. In March 1999, the FDA's Endocrine and Metabolic Drugs Advisory Committee reviewed the status of troglitazone and the potential toxicities and recommended continued availability in a select group of patients: those who are not well controlled with other antidiabetic agents. Since then, it has been determined that patients requiring the use of an insulin sensitizer should be treated with one of the alternative agents. Although results from pre-marketing trials revealed no evidence of hepatotoxicity with the newer agents (rosiglitazone and pioglitazone), two recent case reports demonstrated that rosiglitazone may be associated with hepatic failure following just 14 days of therapy, although a true cause-and-effect relationship has not been established.26,27
The FDA recommends that serum transaminase levels be monitored every other month for the first year in all patients receiving a thiazolidinedione. Following one year of therapy with the newer agents, the incidence of serum transaminase elevations has been reported to be similar to placebo.
The time to achieve a desired effect with the thiazolidinediones is somewhat longer than the other classes of hypoglycemic agents discussed thus far. Intervals of at least three to four weeks should be allowed before increasing the dosage of these agents. Smaller dosages can be initiated if used as part of a combination regimen with a sulfonylurea or a sulfonylurea plus metformin. In patients receiving insulin therapy, the addition of a thiazolidinedione has resulted in significant reductions in daily insulin requirements.28,29
Alpha-glucosidase inhibitors
Acarbose (Precose) and miglitol (Glycet) are the two agents available in this class. Alpha-glucosidase inhibitors act by inhibiting the enzyme alpha-glucosidase found in the brush border cells that line the small intestine, which cleaves more complex carbohydrates into sugars. Because they inhibit the breakdown and subsequent absorption of carbohydrates (dextrins, maltose, sucrose and starch; no effect on glucose) from the gut following meals, the largest impact of these drugs is on postprandial hyperglycemia. Their effect on FPG levels is modest. They have been associated with a reduction in HbA1cby 0.7 to 1.0 percent and FPG levels by 35 to 40 mg per dL (1.9 to 2.2 mmol per L).4,5,30,31Thus, these agents are most useful in patients who have mild FPG elevations or in patients with predominant postprandial hyperglycemia.
The most bothersome side effects observed with these agents are gastrointestinal, including abdominal discomfort, bloating, flatulence and diarrhea but are reversible with discontinuation. Therapy with acarbose has been linked to elevations in serum transaminase levels and the use of this agent is contraindicated in patients with liver cirrhosis. Likewise, concentrations of the alpha-glucosidase inhibitors have been shown to increase proportionally to the degree of renal dysfunction and their use in patients with a serum creatinine level more than 2.0 mg per dL (180 μmol per L) is not recommended. Other contraindications include patients with inflammatory bowel disease or a history of bowel obstruction.32
Therapy should be initiated with the lowest effective dose and titrated slowly over intervals of two to four weeks. Patients should be instructed to take this medication with food. For maximum efficacy, the dietary carbohydrate intake should exceed 50 percent. Although hypoglycemia is not typically associated with monotherapy with the alpha-glucosidase inhibitors, it can occur in combination with other drugs. It is important, therefore, to inform patients that the traditional treatment for hypoglycemia may be blocked while using this therapy and to consume only glucose.
Combination Therapy
If adequate control is not obtained with the use of a single agent, combination therapy is an option (Figure 1).Several of the available oral agents have been studied in combination and have been shown to further improve glycemic control when compared to monotherapy.33As with monotherapy, the choice of a second agent should be based on individual characteristics. Reasonable combinations of agents include a sulfonylurea plus metformin, a sulfonylurea plus an alpha-glucosidase inhibitor, a sulfonylurea plus a thiazolidinedione, metformin plus repaglinide, biguanide plus alpha-glucosidase inhibitor, and metformin plus a thiazolidinedione. A newer formulation (Glucovance) combines glyburide and metformin in one tablet, allowing a more convenient dosing schedule.
Some physicians advocate therapy combining three oral agents, (sulfonylurea, metformin, thiazolidinedione or sulfonylurea, metformin, alpha-glucosidase inhibitor), although this approach has not been extensively studied.34Significant data support the combination of bedtime insulin with daytime sulfonylurea therapy.35,36Although beyond the scope of this review, this combination can be quite effective in reducing FPG. Several other combinations have recently been reviewed.37

