Physicians assess the decision-making capacity of their patients at every clinical encounter. Patients with an abrupt change in mental status, who refuse recommended treatment, who consent too hastily to treatment or who have a known risk factor for impaired decision-making should be evaluated more carefully. In addition to performing a mental status examination (along with a physical examination and laboratory evaluation, if needed), four specific abilities should be assessed: the ability to understand information about treatment; the ability to appreciate how that information applies to their situation; the ability to reason with that information; and the ability to make a choice and express it. By using a directed clinical interview or a formal capacity assessment tool, primary care physicians are able to perform these evaluations in most cases.
Assessing a patient's medical decision-making capacity is part of every medical encounter. The process is generally spontaneous and straightforward: during the performance of routine inpatient and outpatient visits, physicians confirm the ability of their adult patients to understand their medical condition and options for care. For some patients, however, the assessment may not be straightforward. Consider the cases presented below.
Illustrative Cases
CASE 1
A 54-year-old woman with diabetes and schizophrenia has been hospitalized with unstable angina, bilateral heel ulcers, urinary retention caused by an acute urinary tract infection and anemia caused by a combination of gastritis and chronic renal failure. One year ago, she was hospitalized with diabetic ketoacidosis after reporting that “voices” told her to stop taking her insulin. Currently, she is improving but requires a urinary catheter and must keep her legs elevated at rest. She says she is now able to take care of herself and wants to return home. Does this patient have the capacity to make this decision?
CASE 2
A 78-year-old man has a recent diagnosis of metastatic cancer of unknown primary. He returned to the office today after having a computed tomography (CT) scan showing a pancreatic lesion that may be the primary cancer and is the only lesion accessible for biopsy. He requires large doses of narcotics for pain control and his level of consciousness fluctuates greatly. It is not clear if he understands his prognosis or that a tissue diagnosis will probably not affect treatment or outcome. When he is more lucid, he wants “the test”—a CT-guided pancreas biopsy. Does this patient have the capacity to consent to this procedure?
When to Assess Capacity
Four clinical scenarios are described1 that should alert physicians to assess a patient's decision-making capacity more carefully than usual. The first occurs when patients have an abrupt change in mental status. This change may be caused by hypoxia, infection, medication, metabolic disturbances, an acute neurologic or psychiatric process, or other medical problem. The second occurs when patients refuse recommended treatment, especially when they are not willing to discuss the refusal, when the reasons for the refusal are not clear or when the refusal is based on misinformation or irrational biases. The third occurs when patients consent to particularly risky or invasive treatment too hastily and without careful consideration of the risks and benefits. The last scenario occurs when patients have a known risk factor for impaired decision-making, such as a chronic neurologic or psychiatric condition, a significant cultural or language barrier, an education level concern, an acknowledged fear or discomfort with institutional health care settings or who are at an age at either end of the adult spectrum (adolescents younger than 18 years or adults older than 85 years).
Patients exemplifying one of these scenarios require careful assessment but may still be able to make their own decisions. Some abrupt mental status changes, for instance, are only temporary. Some patients refuse treatment for reasons that may be unusual or idiosyncratic but are not irrational when examined in more detail. Other patients consent to treatment without apparent consideration of risks and benefits because they have already decided to follow the recommendations of their physician. Many patients with neurologic or psychiatric conditions,2,3 or those who are younger than 18 or older than 85 years, are able to make decisions about some aspects of their medical care.
Decision-making capacity, medical or otherwise, is always specific to the task requiring the decision.1,4 Certain patients may be able to decide some aspects of their care, but not others. For example, a patient with mild-tomoderate Alzheimer's disease who experiences chest pain may be able to understand the need for antibiotics to fight pneumonia but not the indications for, or the risks and benefits of, cardiac catheterization and angioplasty for coronary artery disease.
How to Assess Capacity
Once a patient has been identified as requiring a more careful assessment of capacity, the evaluation should proceed in a clear and organized manner.1,4–6 Physicians may use a directed clinical interview or a formal capacity assessment tool.
DIRECTED CLINICAL INTERVIEW
Ancillary tests may be needed, depending on the individual circumstances, including history from therapists or other caregivers, physical assessment, laboratory evaluation and possibly even neuroimaging studies. These tests may all help clarify whether the current level of functioning and, possibly capacity, is likely to improve. Table 11,4–6 outlines specific patient abilities to be assessed along with suggested questions to assess each ability during a directed clinical interview. After these abilities are assessed, a general mental status examination also must be performed to determine whether any serious psychopathologic factors may be unduly influencing patient thinking. The clinician's final assessment of whether a patient has medical decision-making capacity depends on whether the clinician believes that the patient is free of significant psychopathologic-impaired thinking and possesses sufficient abilities to make the specific decision in question.
The lack of any one ability does not mean that a patient lacks the overall ability to make a decision.1,4 For example, patients with limited education, with diverse cultural backgrounds or with minimal prior experience in a medical setting may not completely understand all the alternatives to, or all the major risks of, a proposed treatment. However, they may still have enough understanding overall to make their own decisions.
A judgment about capacity is precisely what clinicians are expected to render.7 Legally, such judgments are not made by physicians but are made by the courts according to the laws of the state in which the patient resides. Local authorities should be consulted for specific legal definitions and procedures.8 Practically, most cases never reach the courts and, when they do, the court's legal “determination of competency” usually agrees with the physician's overall “assessment of capacity.” However, a legal determination of incapacity is generally limited to specified rights, whereas incompetency is (legally) associated with a loss of legal rights.9
Both legally and ethically, Western culture favors patient autonomy—an individual patient's right to self determination—over the beneficent protection offered by others.10 Adults are believed to be “good enough” to make their own decisions—for better or worse—even though someone else might be a better decision-maker for them from a purely objective, academic or analytic point of view. Restricting autonomy requires a clear and convincing assessment that a patient's decision regarding care will result in unintended, irreparable harm. Unfortunately, harm is difficult to define because it varies from one person and circumstance to another. Therefore, many experts1,4,11 in capacity believe in a sliding-scale threshold, or variable level of certainty, for capacity that depends on the patient's decision and the specific risks and benefits of the proposed treatment as shown in Figure 1.1,4,11
TABLE 1 Patient Abilities to be Assessed in the Evaluation of Medical Decision-Making Capacity
| 1. | Questions to determine the ability of the patient to understand about treatment and the proposed options for care |
| • What is your understanding of your condition? | |
| • What are the options for your situation? | |
| • What is your understanding of the benefits of treatment and what are the odds that the treatment will work for you? | |
| • What are the risks of treatment and what are the odds that you may have a side effect or bad outcome? | |
| • What is your understanding of what will happen if nothing is done? | |
| 2. | Questions to determine the ability of the patient to appreciate how that information applies to their own situation: |
| • Tell me what you really believe about your medical condition. | |
| • Why do you think your doctor has recommended (name of specific treatment or test) for you? | |
| • Do you think it (specific treatment/test) is the best treatment/test for you? Why or why not? | |
| • What do you think will actually happen to you if you accept this treatment? If you don't accept it? | |
| 3. | Questions to determine the ability of the patient to reason with that information in a manner that is supported by the facts and the patient's own values |
| • What factors/issues are most important to you in deciding about your treatment? What are you thinking about as you consider your decision? | |
| • How are you balancing the pluses and minuses of the treatments? | |
| • Do you trust your doctor? Why or why not? | |
| • What do you think will happen to you now? | |
| 4. | Questions to determine the ability of the patient to communicate and express a choice clearly: |
| • You have been given a lot of information about your condition. Have you decided what medical option is best for you right now? | |
| • We have discussed several choices; what do you want to do? |
FORMAL ASSESSMENT TOOLS
In addition to or instead of a directed clinical interview, a formal, structured assessment tool can be used to evaluate capacity. Two such tools are the Aid to Capacity Evaluation (ACE)3,12 and the MacArthur Competence Assessment Tool (MacCAT).1 Both use standardized questions and scoring systems to achieve a more objective assessment of capacity than an interview. The abilities assessed, however, are the same as those assessed in a clinical interview and the scores still require interpretation by an evaluator. The MacCAT is a lengthy, comprehensive tool designed for patients with complex psychiatric or neurologic conditions whose capacity determination is especially difficult. The assessment can be administered and scored in approximately 30 minutes. The ACE (Figure 2) is a short, more clinically oriented tool that can be administered and scored in five to 10 minutes. The ACE can also be found on the Web site of the University of Toronto Joint Centre for Bioethics:http://www.utoronto.ca/jcb/_ace. General instructions are simple: clinicians are directed to address communication barriers, discuss treatment information and answer patient questions before administering the assessment.
FIGURE 1. Capacity Thresholds
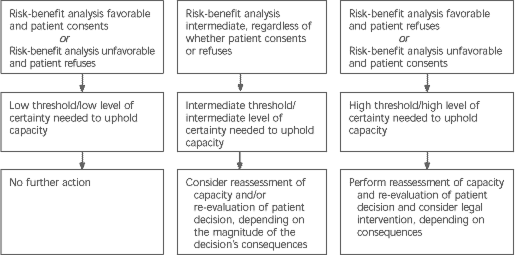
Capacity thresholds according to patient decision and risk-benefit analysis of care options.
Information from references 1, 4 and 11.
Regardless of whether a directed clinical interview or a formal tool is used, the physician must clearly document the assessment and the final judgment about capacity in the patient record. If an interview is used, a brief summary of the questions asked and the answers provided should be documented; if a formal assessment tool is used, it should be included in the patient's record. In either case, the physician must also document the reasoning used to reach the final judgment.
Who Should Assess Capacity
Primary care physicians are qualified to perform capacity assessments. There are several reasons why a patient's primary care physician may be the best professional to assess capacity1,7: (1) the primary physician already knows the patient's medical circumstances and the question to be decided; (2) the primary physician may have the best opportunity to know the patient's and their family's personal values and cultural and religious views; (3) the primary physician has the benefit of history, so that the assessment is not a one-visit snapshot of a patient but is a longitudinal and more thorough assessment based on multiple interactions; and (4) the primary physician, because of an ongoing medical relationship with the patient, is in the best position to reevaluate capacity in the future.
Psychiatrists are more expert in evaluating patients with severe mental illness and may be legally required, in some locales, to assess patients referred to the courts. However, research comparing their judgments to those of other physicians shows that they are no better at assessing capacity in practice.13At the same time, however, because psychiatrists perform capacity evaluations frequently, primary care physicians should feel comfortable consulting them in difficult cases. A bioethics panel may also help clarify or delineate the issues that need to be addressed with a specific patient.
Follow-up of Illustrative Cases
CASE 1
The 54-year-old woman with schizophrenia and multiple medical problems reported that she was not now hearing voices nor was she exhibiting any other psychotic symptoms. She had been very stable on her psychiatric medications for several months. The patient understood her medical situation, appreciated the consequences of care options, analyzed logically the information she was given and was able to express a clear choice. She was judged to have capacity. After learning selfcatheterization, demonstrating knowledge of her medication regimen and agreeing to home health nursing care, she returned home and returned for follow-up visits as directed.
CASE 2
The 78-year-old man with metastatic cancer of unknown primary understood his medical condition and was able to express his choice, but he could not appreciate the fact that the biopsy would probably not affect treatment or outcome and he could not analyze the information given him. Even when he was lucid, he was convinced “the test” would cure him, despite repeated explanations. He was judged not to have capacity. He had a durable power-of-attorney for health care naming his wife as his agent, and, after further discussion, she declined the biopsy. He died several weeks later without a tissue diagnosis but with full palliative care.
Final Comment
Physicians assess the decision-making capacity of their patients at every clinical encounter. Patients requiring careful assessment can be easily identified using standardized evaluations performed by means of a directed clinical interview or the use of a formal assessment tool such as the ACE3,12 or the MacCAT.1
If the patient lacks the capacity for decisionmaking, a determination of surrogacy will be necessary. In the best-case scenario, the patient may have previously appointed an agent; in the worst-case scenario, the court may need to become involved. (The discussion of surrogacy is too broad for this article, but it has been well-covered elsewhere.)4,14 If the patient does not have an advance directive or health care proxy, the surrogate will need to make decisions based on principles of “substituted judgment”(what the patient would have decided) or “best interest” (what the surrogate judges to be best for the patient).

