Clinical Scenario
A 30-month-old infant presents with three days of upper respiratory symptoms, including tugging on the left ear. Examination reveals a red, bulging, immobile left tympanic membrane. The patient is afebrile and in no apparent distress. All immunizations are up to date.
Clinical Question
Should clinicians treat children who have acute otitis media with antibiotics?
Evidence-Based Answer
Based on this review1 and the systematic reviews of Rosenfeld2 and Kozyrskyj,3 antibiotics appear to play a small but potentially useful role in the treatment of acute otitis media in children. Antibiotics produce a reduction in pain at two to seven days but have no effect on tympanometry, audiometry, contralateral otitis media or rate of recurrence. Further randomized trials comparing delayed treatment for 48 to 72 hours with immediate antibiotic therapy appear to be warranted in low-risk populations.
Cochrane Critique
This overview addressed a focused clinical question—whether antibiotics are helpful in the treatment of acute otitis media in children. The Cochrane collaborators reviewed randomized clinical trials in which antibiotics were compared with placebo medication. Standard Cochrane methodology was used to ensure comparable, high-quality studies using blinded, reproducible extraction methods. While unpublished results were not directly addressed, it is unlikely that relevant published, randomized, controlled trials were missed because unpublished trials relating to this particular disease are unlikely to exist. For the most part, patients in the trials were selected from primary care practices in the United States and Europe. The treatments are available to most physicians, and the direct costs are modest.
Practice Pointers
In these studies,1–3 antibiotics reduced pain by 28 percent at two to seven days but had no effect on tympanometry, audiometry, contralateral otitis media or rate of recurrence (Figure 1). However, about 80 percent of children in the placebo group improved in two to seven days, and few adverse outcomes occurred in the control group. Because serious adverse effects such as mastoiditis and meningitis were rare in these pooled analyses, it is not possible to determine whether protocols of delayed treatment or no treatment might be harmful.
Cochrane Abstract
Background. Acute otitis media is one of the most common diseases in early infancy and childhood. Antibiotic use for acute otitis media varies from 31 percent in the Netherlands to 98 percent in the United States and Australia.
Objectives. The objective of this review was to assess the effects of antibiotics in children with acute otitis media.
Search Strategy. The authors searched the Cochrane Controlled Trials Register, MEDLINE, Index Medicus (pre-1965), Current Contents and reference lists of articles from 1958 to January 2000.
Selection Criteria. Randomized trials comparing antimicrobial drugs with placebo in children with acute otitis media were selected.
Data Collection and Analysis. Three reviewers independently assessed trial quality and extracted data.
Primary Results. Ten trials were eligible, but only seven trials, with a total of 2,202 children, included patient-relevant outcomes. The methodologic quality of the included trials was generally high. All trials were from developed countries. The trials showed no reduction in pain at 24 hours, but a 28 percent relative reduction (95 percent confidence interval [CI], 15 to 38 percent) in pain at two to seven days. Since approximately 80 percent of cases will have resolved spontaneously in this time, this means an absolute reduction of about 5 percent, or that about 17 children must be treated with antibiotics to prevent one child from having some pain after two days. There was no effect of antibiotics on hearing problems of acute otitis media, as measured by subsequent tympanometry. However, audiometry was performed in only two studies and incompletely reported. Nor did antibiotics influence other complications or recurrence. There were few serious complications seen in these trials: only one case of mastoiditis occurred (in a penicillin-treated group).
Reviewers' Conclusions. Antibiotics provide a small benefit for acute otitis media in children. As most cases will resolve spontaneously, this benefit must be weighed against the possible adverse reactions. Antibiotic treatment may play an important role in reducing the risk of mastoiditis in populations where it is more common.
These summaries have been derived from Cochrane reviews published in the Cochrane Database of Systematic Reviews in the Cochrane Library. Their content has, as far as possible, been checked with the authors of the original reviews, but the summaries should not be regarded as an official product of the Cochrane Collaboration; minor editing changes have been made to the text (http://www.cochrane.org)
FIGURE 1. Review: Antibiotics for acute otitis media in children
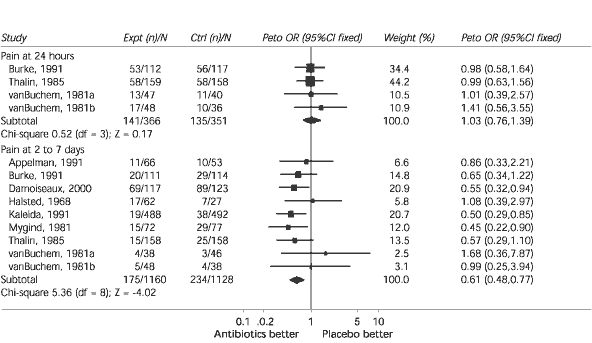
Comparison: Antibiotic vs. placebo
Outcome: Pain
Outcome in terms of pain in a comparison of antibiotics versus placebo in the treatment of acute otitis media in children, (expt = experiment; n = number; N = study population; ctrl = control; Peto OR = Peto odds ratio; CI = confidence interval; df = degrees of freedom; Z = standard deviation)
Adapted with permission from Glaziou PP, Del Mar CB, Sanders SL. Antibiotics for acute otitis media in children. (Cochrane Review). In: The Cochrane Library, Issue 2, 2001. Oxford: Update Software.
Children younger than two years of age and those with bilateral otitis media appear to be at greatest risk for treatment failure, but no validated prediction rules exist to target high-risk groups with antibiotics. Further randomized trials comparing delayed treatment for 48 to 72 hours with immediate antibiotic therapy appear to be warranted in children older than two years, given the present low risk of meningitis and mastoiditis in populations vaccinated against Haemophilus influenzae.
Reading the Numbers
| Relative risk/absolute risk reduction |
| The most valid method of providing results of clinical trials or meta-analysis of clinical trials is to provide the rates of occurrence of important clinical outcomes for both the treated (Pe) and the untreated (Pc) groups, calculating the relative risk reduction, (Pe-Pc)/Pc, and the absolute reduction, Pe-Pc. Some authors express the reciprocal of the absolute risk reduction (1/Pe-Pc) or the number needed to treat (NNT) as a measure of the benefits of treatment. |
| Appropriately applying the NNT and absolute benefits of treatment from a clinical trial or systematic review to an individual patient requires comparable risk of disease in that patient compared with the study population, whereas the relative risk reduction should be robust even when the risk of disease is much different in that individual patient compared to the study population analyzed. For example, the rate of persistent ear pain at two to seven days in children younger than age two with bilateral disease may be greater than the 14 percent found in this meta-analysis in the untreated group—perhaps 28 percent. We will still expect a 34 percent reduction relative to this baseline level with the use of antibiotics if a causal relationship exists between pain and antibiotic use. However, the NNT for one patient to have benefit would be 10.5, not 20 as in the present Cochrane review. |

