There are studies estimating that between 13.8 and 80 percent of all primary care patients will have at least one episode of low back pain during his or her lifetime. Diagnostic testing for low back pain is performed to exclude serious etiologies (i.e., malignancy, infection, inflammatory disease). The best evaluation would be one that minimizes unnecessary testing but is still able to detect serious etiologies. Joines and associates conducted a decision analysis to compare diagnostic strategies for evaluating low back pain in light of the need to rule out spinal malignancy.
FIGURE. Spinal Cancer and Back Pain
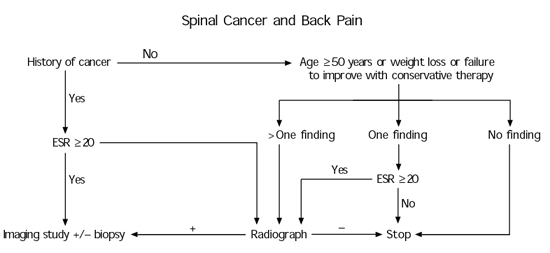
Selective testing for spinal cancer in patients with low back pain. (ESR = erythrocyte sedimentation rate)
Adapted with permission from Deyo RA, Diehl AK. Cancer as a cause of back pain: frequency, clinical presentation, and diagnostic strategies. J Gen Intern Med 1988;3:230–8.
Eleven diagnostic strategies were examined in this study. The elements in a diagnostic work-up included clinical findings, erythrocyte sedimentation rate (ESR) and plain radiographs, all of which were obtained before other imaging studies (bone scan and magnetic resonance imaging [MRI]) or percutaneous vertebral biopsy. Four clinical findings have been shown to be predictors of cancer in patients with low back pain. These are a previous history of cancer, age of at least 50 years, failure of conservative therapy and unexplained weight loss. Cost was also analyzed.
The most effective, but also the most expensive, method of detecting spinal malignancy in a patient with low back pain is to obtain an imaging study for each patient. The cost per case found was determined to be $49,814, with an incremental cost per additional case found of $624,781. The second most effective strategy would be to image everyone if they have a history of cancer, a positive plain film or an elevated ESR. Costs to implement this strategy would be $23,703 and $91,428, respectively. If imaging is done only when there is a history of cancer or if the plain film is positive, the cost per case found is reduced to $10,706, with incremental costs of $50,020. One other dominant strategy (with low sensitivity but high specificity) is to obtain an imaging study if the plain film and the ESR are positive. The cost per case found is $5,283. The cost effectiveness was, of course, dependent on the prevalence of spinal malignancy, which is usually around 1 percent.
Using cost effectiveness to analyze the problem demands a trade-off between sensitivity, specificity and cost. The authors judge the strategy that provides for imaging when the plain film and ESR are positive to be too insensitive; less than 50 percent of cancers are found when using this strategy.
An algorithm proposed by Deyo and Diehl (see accompanying figure) is advocated by the authors if higher sensitivity is desired, but the authors note that although the costs are low, only slightly more than one half of cancers are found with this strategy. For the best balance, they recommend imaging if the plain film or the ESR is positive, or if there is at least one clinical finding. The ESR cutoff in this case should be 50 mm per hour. If an initial biopsy is negative, sensitivity can be improved by repeating the biopsy. Fewer unnecessary biopsies will be performed if serial imaging (bone scans followed by MRI) is performed.
editor's note: The authors do not discuss the use of computed tomographic (CT) scanning as an advanced imaging method since they are specifically looking for spinal malignancy, which will, in general, be well detected with MRI. However, CT may be more appropriate in certain patients—specifically, those in whom MRI is not possible (i.e., those who are severely claustrophobic or who have a metallic foreign body in place). Efficacy and cost effectiveness of CT in these patients would need further study.—g.b.h.

