Diarrheal illness is a common cause of morbidity and even mortality. Most cases are self-limited. Depending on the severity and type of diarrhea, however, specific testing and management strategies are indicated. The Infectious Diseases Society of America (IDSA) presents a clinical guideline for the management of infectious diarrhea.
An increasingly wide variety of agents are recognized as causes of serious diarrheal illness, such as Escherichia coli O157:H7, Campylobacter jejuni, Clostridium difficile, Salmonella, Shigella and Giardia. Cost-effective testing strategies and avoidance of indiscriminate antibiotic use are important components of the rational management of diarrheal illness.
Results of studies document substantial variation in the use of stool testing that is not accounted for by the clinical characteristics of the affected patients. The IDSA suggests use of a specific algorithm for stool testing in patients with diarrhea (see accompanying figure). Persons with diarrhea should be considered for testing if they are febrile or have bloody stool. Standard stool cultures in cases of diarrhea developing in hospitalized patients are common but of very low yield. The guideline suggests testing in this circumstance only for C. difficile toxin unless specific factors suggest a different pathogen (e.g., local outbreak of Salmonella infection). Testing for ova and parasites is of very low yield in most cases, and the guideline reserves it for use in diarrheal illness of more than seven days.
A hospital survey of more than 30,000 stool specimens sent for testing revealed a specific pathogen in only 5.6 percent of cases. In descending order, the most commonly identified pathogens were C. jejuni, Salmonella, Shigella and E. coli O157:H7. When visible blood was present in the stool, more than one third of cases were caused by Shiga toxin-producing E. coli O157:H7. Selective antibiotic treatment was recommended for traveler's diarrhea, Shigellosis and Campylobacter infection. The role of antibiotic therapy in Salmonellosis and E. coli O157:H7 infection remains unclear. Avoidance of antimotility agents in bloody diarrhea is emphasized, especially when illness is caused by E. coli O157:H7, which could increase the risk of subsequent hemolyticuremic syndrome. In selected at-risk populations, wider use of vaccines, including oral typhoid vaccine and oral cholera vaccine (available only outside the United States), is recommended.
FIGURE. Diarrheal Illnesses
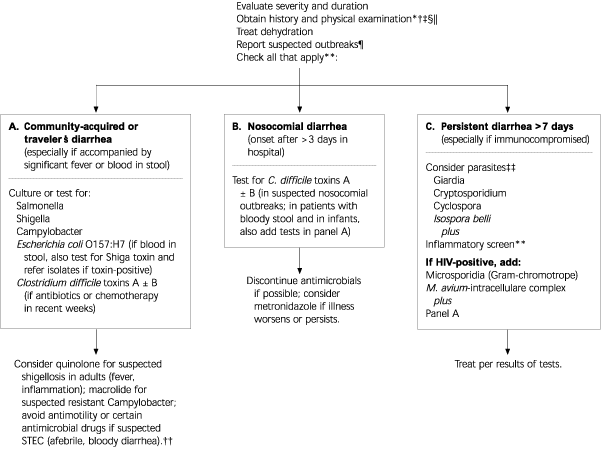
Recommendations for the diagnosis and management of diarrheal illness. (STEC = Shiga toxin-producing Escherichiacoli; HUS = hemolytic uremic syndrome; HIV = human immunodeficiency virus)
Adapted with permission from Guerrant RL, Van Gilder T, Steiner TS, Theilman NM, Slutsker L, Tauxe RV, et al. Practice guidelines for the management of infectious diarrhea. Clin Infect Dis 2001;32:334.

