Am Fam Physician. 2001;64(8):1420-1426
The incidence of ectopic pregnancy increased sixfold in the United States between 1970 and 1992, with more than 100,000 cases occurring in 1992. Although the mortality rate for ectopic pregnancy has fallen, this condition still accounts for 9 percent of deaths during the first trimester of pregnancy. Delay in diagnosis increases the risk of rupture, intra-abdominal hemorrhage, blood transfusion, need for operative intervention and death. The only clinical signs and symptoms of ectopic pregnancy—abdominal pain or vaginal bleeding in the first trimester—are not sensitive or specific enough for diagnosis. Diagnosis of ectopic pregnancy must be timely and accurate to allow appropriate intervention if pathology is detected while not endangering a viable pregnancy. Several diagnostic modalities have been used for ectopic pregnancy, either alone or in combination, but none has been established as superior to others. Gracia and Barnhart performed a decision analysis to determine the optimal strategy for diagnosing ectopic pregnancy and compared it with diagnosis by clinical examination alone.
After reviewing the literature, the authors compared six diagnostic algorithms: ultrasonography followed by quantitative human chorionic gonadotropin (hCG); quantitative hCG followed by ultrasonography; serum progesterone measurement followed by ultrasonography and quantitative hCG for those with nondiagnostic results; serum progesterone followed by quantitative hCG and ultrasonography; ultrasonography with repeated ultrasonography after 24 hours if nondiagnostic; and clinical examination. For each strategy, probabilities were calculated from published studies augmented by data from the authors' teaching hospitals. The results were extrapolated to a hypothetic group of 10,000 women with spontaneous pregnancies presenting with pain or bleeding in early pregnancy. The most important outcome was the number of missed ectopic pregnancies per 10,000 women.
No ectopic pregnancies were missed with the two strategies involving only ultrasonography and hCG measurement. Using transvaginal ultrasonography before determining hCG resulted in fewer interrupted intrauterine pregnancies (70 compared with 122), but the order of testing did not significantly change the time to diagnosis (1.46 and 1.66 days) or the number of laparoscopies or dilatation/ curettage procedures performed. The total estimated charges to patients for these two strategies ($1,958 and $1,842, respectively) were also not statistically different. When the serum progesterone level was used as the initial diagnostic test, an estimated 24 ectopic pregnancies were missed per 10,000 patients, regardless of the order of the subsequent tests. Women with low progesterone levels were presumed to have nonviable pregnancies, and those with levels of at least 25 ng per mL to have viable intrauterine pregnancies. Women with levels between 5 and 25 ng per mL were further investigated with ultrasonography and quantitative hCG. The time to diagnosis was marginally shorter with this strategy than with the first two strategies and resulted in interruption of fewer intrauterine pregnancies when serum progesterone was inserted as an initial test (see accompanying table). The strategy using repeated ultrasonography after 24 hours of observation missed no ectopic pregnancies and had a short time to diagnosis (1.2 days) but interrupted 121 intrauterine pregnancies and had the highest financial charge. Clinical examination missed all ectopic pregnancies.
| Strategy | Missed EP/10,000 | Interrupted IUP/10,000 | LS/10,000 | D&C/10,000 | US/10,000 | H/10,000 | Days to diagnosis/patient | Blood draws/10,000 | *Total charge/ patient |
|---|---|---|---|---|---|---|---|---|---|
| US→hCG | 0 | 70 | 940 | 2,581 | 10,250 | 0 | 1.46 | 5,227 | $1,958 |
| hCG→US | 0 | 122 | 940 | 2,463 | 8,276 | 0 | 1.66 | 14,375 | 1,842 |
| P→US→hCG | 24 | 25 | 916 | 3,547 | 3,272 | 0 | 1.25 | 12,108 | 1,692 |
| P→hCG→US | 24 | 39 | 916 | 3,191 | 2,555 | 0 | 1.26 | 15,003 | 1,569 |
| US→US | 0 | 121 | 940 | 3,319 | 11,760 | 1,760 | 1.21 | 0 | 2,486 |
| CE | 940 | 0 | 0 | 0 | 0 | 0 | 1.0 | 0 | 0 |
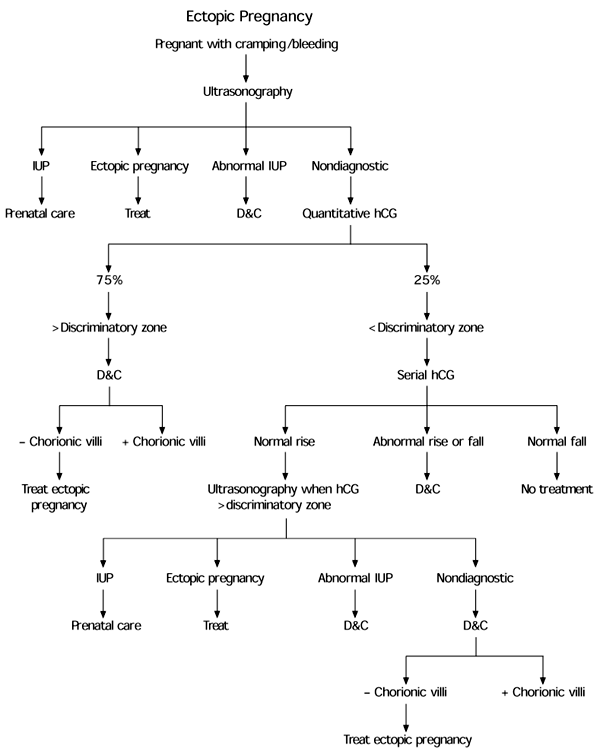
The authors conclude that a strategy using ultrasonography first but also involving quantitative hCG provided the most accurate and efficient approach to diagnosing ectopic pregnancy (see accompanying figure).