Am Fam Physician. 2001;64(9):1498
Family physicians, nurse practitioners and physician assistants are distinctly different in their clinical training, yet they function interdependently. Together, they represent a significant portion of the primary care work force. Training capacity for these professions has increased rapidly over the physician assistant decade, but almost no collaborative work force planning has occurred.
Family physicians, nurse practitioners and physician assistants have complementary and interdependent functions that are important to primary care. However, physician assistants always work with physicians and nurse practitioners almost always do. Despite this functional interdependence, since 1990 there has been tremendous growth in the production capacity of all three professions without joint work force planning.
Family practice residency training capacity has expanded significantly in the past decade. The number of positions offered in family practice residency programs has increased 34 percent, from 2,393 in 1990 to 3,206 in 2000.
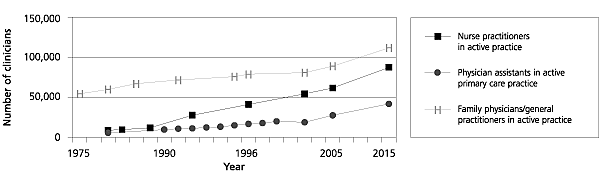
National data about nurse practitioners are of poor quality. We do know that the number of masters-level programs increased 210 percent between 1993 and 1999 and that the number of nurse practitioner students increased fourfold between 1992 and 1997. Between 1990 and 1996, the number of trained nurse practitioners working in nursing doubled to 71,000. Given the current training trends, this number is expected to grow to 106,500 by 2005 and to as many as 151,000 by 2015. While the total number of nurse practitioners may already be larger than the number of family physicians, only two thirds of formally trained nurse practitioners were involved in direct patient care in 1996.
National data about physician assistants are quite good. Between 1991 and 2000, the annual number of annual physician assistant graduates increased by nearly 250 percent and the number of accredited training programs increased from 53 to 126 (138 percent). The Bureau of Labor Statistics lists physician assistants in the top 10 fastest growing professions. An estimated 83 percent of all graduates are in active practice and about 53 percent of these are in primary care. Based on current trends, the number of physician assistants in active practice is projected to reach 79,000 by 2015 and those in primary care about 42,000.
These trends suggest significant, uncoordinated growth for all three professions. Even this work force comparison is incomplete for primary care, as it excludes general internal medicine and general pediatrics. As efforts to improve the quality and safety of health care look to new, integrated models, there is an imperative for these professions to look collaboratively at work force needs.